In rural towns you know most everyone's history, their family, their sorrows and joys. They are neighbors, friends, family, or family/friends of someone you know. As a nurse you have a greater degree of responsibility and accountability. Having worked in both urban and rural environments, I found it was much easier to just 'do the job' in the urban setting. I didn't know anyone. There was no connection. I didn't go home at night and worry about the patients. In the rural setting as a nurse you are compelled to find the answers, to leave no stone unturned for the patients you care for . . .follow-up on every possibility . . . go home at night and worry about those you care for as a nurse. The rural nurse must have commitment and a connection to the people he or she cares for . . . that transcends the experience of nursing in an urban setting. [Anonymous survey respondent]
Background and rationale
The professional literature, as well as the popular media, report a shortage of nurses in the USA, Canada, and internationally. More nurses currently are employed in the workforce, yet nursing shortages continue and are especially critical in many rural communities1-7. Attracting nurses to work in less populated and more remote settings presents challenges that differ from those in more highly populated areas8-10. In light of the serious shortages, what can be done to attract nurses to work in rural areas in roles as described by the quote that introduces this article? What are the characteristics and interests of nursing students who choose to work in the rural environment? How can nursing education programs better prepare students for rural practice? The purpose of this exploratory study was to examine self-identified factors of nursing students who expressed an interest in rural practice. The sample for this study included students from the USA and Canada who were enrolled in graduate and undergraduate programs of nursing, attending an international rural nursing conference held in a north eastern state in the USA. A few words of explanation are offered here regarding nursing education programs in North America, specifically Canada and the USA. Nursing students enrolled in 'undergraduate' programs are completing the basic educational requirements for the baccalaureate degree to become a registered (licensed) nurse. 'Graduate' programs focus on developing a clinical specialty at the master's degree level. The majority of graduate level students attending this conference were enrolled in advanced clinical practice programs, specifically nurse practitioners, midwives and clinical specialists.
There is wide diversity in how rural is defined with conflicting definitions in official definitions of rural and urban and this can hinder precisely discussing rural nursing issues. Still information exists about rural environments that can be useful to begin examining general concerns relative to nursing and health care. Based on census data, in the USA rural residents make up approximately one-fifth (20%) of the total population and are distributed across four-fifths (80%) of the land mass; thus, approximately 54 million people live in areas defined as 'rural'8. In Canada, approximately 95% of the country's land mass is rural and remote, and approximately nine million residents (30%) live in these rural and remote regions11-17. A comprehensive discussion of the particular health-care systems of the USA and Canada is not possible in this short article; however, challenges confronting rural communities in these two nations in many ways are similar. For instance, in the USA, areas designated as Health Personnel Shortage Areas (HPSA) are characterized by insufficient numbers of health professionals, in particular primary care providers. Counties that are designated as HPSA generally have even greater nursing shortages than other rural regions. Even though there is no such federal designation in Canada, similar recruitment and retention challenges exist for nurses, physicians, and other health-care providers in rural and remote regions of that nation12,17. Recruiting and retaining qualified health professionals, nurses in particular, can be especially problematic for rural communities for a number of reasons.
Historically, in both Canada and the USA, the total nursing work force along with the social mandates for nursing are impacted by national legislation and health-care policy. Even though the two nations have different health-care systems, changes in the organization of health-care delivery, third-party reimbursement policies, and fiscal constraints impact nursing practice. Although recent studies indicate that the nursing work force is at its highest, shortages still exist and are projected to continue for several decades2-7. Shortages are attributable to an aging workforce, declining enrollments in programs of nursing, wider career opportunities for women, along with higher salaries in other disciplines. Additionally, intense workloads and higher patient acuity levels contribute to workforce attrition and, ultimately, nursing shortages. Negative images of nurses may be another deterrent to someone choosing nursing as a profession. The popular media, in particular, has a tendency to portray female nurses as frivolous and subservient to male physicians, or employed for long hours in unpleasant work at a low salary; hence, the profession of nursing appears less appealing to someone making a career decision.
Rural health-care facilities face some additional challenges in recruiting and retaining nurses. Fiscal constraints in particular can limit small facilities from aggressively competing with urban-based counterparts which are offering higher salaries and flexible work hours. Small, oftentimes financially strapped hospitals are not able to offer educational benefits, nor do most have opportunities for nurses to practice in a preferred specialty area8-10. In fact, nursing shortages have contributed to the closure of some small hospitals and sometimes force a small hospital to merge with a large urban-based health-care system. Both of these outcomes further restrict access to health care for rural people who live in a remote or medically under served community. As a result they may need to travel greater distances with higher out-of-pocket costs to obtain essential health care.
Limited access to nursing care is of particular concern for rural women and children. In Canada, women have poorer outcomes if they must travel long distances to give birth. In Saskatchewan, a largely rural province, the 1993 closure of 53 rural hospitals with the subsequent loss of nursing care was followed by an increase in its perinatal mortality rate12. In other words, rural consumers are at risk for poorer health outcomes and increased medical errors associated with nursing shortages14-17. It is important to note, too, that the presence of an adequate number of nurses is an important factor in whether or not a rural community is able to recruit and retain physicians to the region.
Debate continues as to whether there is anything unique about rural nursing practice. Some people believe that rural nursing practice is not unique8,9,18-20. Proponents of this belief assume that nursing care needs of individuals are similar regardless of the setting. In their view, nursing care is no different for rural clients than for individuals in other settings. Others suggest that rural nursing should be classified as a specialty practice. They believe this type of nursing practice requires additional skills associated with the rural context and the modifications that must be made to provide appropriate care for rural patients and communities. Rural contextual features, such as a sparser population, greater distance between services and providers, fewer resources, and less formal social structures require that rural nurses be an 'expert generalist'. It was not the intent of this pilot study to settle the debate of whether or not rural nursing should be a specialty practice or to examine the roles and practice patterns of nurses in these settings. Rather, the investigators speculated that knowledge about rural life and familiarity with nursing practice in rural settings are important considerations when a student decides where to work after graduation.
Methods
This small study elicited demographic and qualitative information from volunteers who were attending an international rural nursing conference in the USA in 2002. Based on their combined extensive experience in nursing education and rural practice, the investigators developed a pencil and paper questionnaire survey. Copies of the one page survey were placed on a table near the registration desk. Next to the stack of surveys there was an informational poster inviting students with an interest in rural practice to participate in the study. Informed consent was assumed when a participant took a copy of the tool and responded to the questions. The survey required approximately 5-10 min for an individual to complete and there were no identified benefits or risks for participants.
Of the 14 items on the survey, 11 elicited demographic data related to the respondent's place of residence and education. The remaining items consisted of open-ended questions that elicited short answer responses regarding major factors that contribute to choosing a rural practice setting after graduation, challenges a nurses might expect to encounter in rural practice, and how nursing educators can best prepare nursing students for rural practice after graduation. The last section asked for 'other comments' which allowed for longer narratives if respondents desired to include additional anecdotal information. Surprisingly, more than half the respondents included their name and address for investigators to follow up with additional questions at a future time.
Results
Analysis of the demographic items consisted of frequencies and central tendencies. Short answer responses were analyzed using content analysis processes to identify common themes. Two investigators independently organized the written comments, then compared and contrasted their findings according to themes and subcategories to establish interrater reliability. Table 1 highlights the demographic makeup of the sample in this pilot study.
Table 1: Participants' demographic data
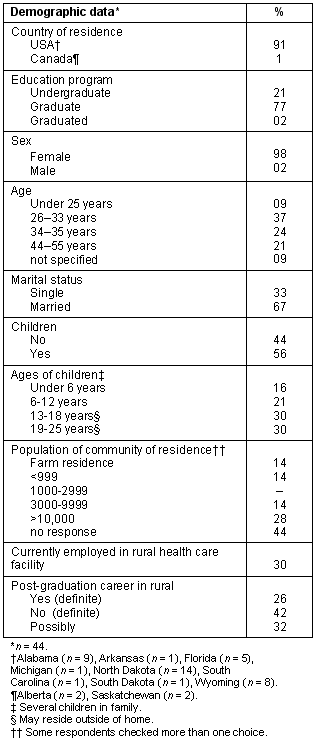
Demographically, the convenience sample (n = 44) included graduate students (63%) and undergraduate students (37%) from the USA (91%) and Canada (9%) who self-reported their interest in rural nursing practice. One participant indicated she/he was a 'recent graduate' but did not elaborate on when she/he graduated. All but one respondent in the sample were female, ranging from under 25 years of age to 55 years. The proportion of Canadian responses was notably low; however, this number reflected the demographic makeup of conference attendees.
Regarding place of residence, 14% indicated they lived on a 'farm', 14% resided in towns having fewer than 1000 residents, 14% resided in communities ranging from 3000 to 9999, and 28% lived in communities that included over10 000 residents. (In some cases, respondents checked more than one option.) Most were married (67%) and had children, ranging in age from under six to 25 years. Of the sample, 30% were employed in a rural health-care facility while attending school and the majority of them planned to continue working in those facilities after completing their education. As for post-graduation plans, 26% definitely planned to continue working in rural places while 42% indicated that definitely was not in their plans; 32% were uncertain about their post graduation employment setting. Of those who indicated they were not planning to work in rural sites, the investigators assumed they were familiar with that kind of practice by their comments and because they were attending an international conference specifically focusing on rural nursing. For that reason their comments were included in the data analyses.
Figure 1 (Part A) highlights thematic findings from the survey in which respondents identified personal, professional, and financial factors that influenced their career choice. Figure 1 (Part B) also highlights major themes of the anticipated challenges in rural nursing practice; specifically, contextual features of rural environments, professional realities of rural nursing, and patient related considerations. Figure 2 summarizes suggested strategies that could be useful to nurse educators in an effort to better prepare nurses for rural practice. The information presented in Figs 1 and 2 will be discussed in subsequent paragraphs. For Fig 1 a general description of the common themes will be presented, interspersed with relevant quotes as submitted by the respondents on the completed surveys.

Figure 1: Analyses of qualitative data: themes

Figure 2: Strategies to prepare nurses for rural practice
Influencing factors to choosing rural practice
Personal factors were revealed by comments indicating that a respondent grew up or at some time lived in a rural setting. The following comments articulate personal factors influencing a preference for rural practice:
I want to go home to my rural [home] town . . . I believe in the rural way of life to raise families.
Quality of life in small towns . . . I like the feel of community there.
I enjoy knowing my neighbors and community . . . Access to outdoor entertainment. . . love of nature . . .quiet setting.
In other words, those who had personal experiences and connections and who enjoyed the lifestyle seemed more interested in returning to practice in a rural setting as a nurse upon completion of their educational program.
Professional factors were associated with respondents' familiarity with the health-care delivery system in less populated areas. Interestingly, consistent with the introductory quote of this paper, these students repeatedly expressed a commitment to help address perceived inequities in the rural health-care system. The following comments reflect the theme of familiarity with and commitment to provide care to rural residents:
[Rural residents have an] Intense need of quality health care, limited access to care ... morbidity and mortality rates that result in health disparities.
[I have the] Ability to provide a needed service to the community.
[I have an] Interest in meeting the health care needs of people in underserved areas; I want to serve the community I live with.
Other dimensions of the professionalism theme centered on using knowledge obtained in respondents' academic programs and their anticipated satisfaction with rural practice, as exemplified by the following comments:
Smaller hospital and the position I will be working in utilizes nurse practitioners (NPs) very well.
[a rural practice provides] Opportunities for my professional advancement. The position is appropriate for my educational preparation. Rural nurses have a connection with community members and an opportunity to 'give back' to the community.
I am treated well. I get more respect there [rural hospital] as a nurse . . . more meaningful and wide range of experiences . . . opportunities for independence in my practice.
The health history of the patient is more accessible to the provider. Constant adaptability is needed [on the part of the provider] because of the diversity of patients and their health conditions.
Financial factors also influenced a few to choose rural practice. Financial support for nursing education and higher nursing salaries in rural settings, especially for those in advanced practice, encouraged some respondents to select a rural practice setting. This theme is best illustrated by the following comments:
I received a bursary to come back to a remote area and pay back that loan.
The pay is highly competitive for an NP and I need the health insurance benefit for my family.
Obviously, respondents who planned to work in a rural setting were more familiar with the rural political and social structures. Likewise, they espoused a commitment to improve health care in the communities where they planned to work after their graduation. Questions that remain unanswered are: How familiar with the rural environment are students who make a rural career decision primarily for financial reasons? What is their level of personal commitment, especially long term, to an underserved community? These questions need closer examination to determine the most effective models that use financial incentives to recruit and retain nurses to remote, rural and medically underserved areas.
Anticipated challenges for nurses in a rural setting
Along with the benefits, respondents in this small study seemed to have a good grasp of real and potential challenges associated with rural nursing practice. Their responses were categorized into three interrelated themes: contextual features of rural environments, professional realities of practice in a more remote setting, and client/patient-related considerations. For all three themes, a crosscutting consideration related to sparse resources associated with low population density.
Contextual features of the rural environment included frequent use of the terms 'isolation' in reference to geographical distances and sparse populations, and 'local politics' in reference to informal social structures in small towns. In turn, these contextual features were associated with professional conflicts and challenges for a nurse in a rural practice. This theme is exemplified by the following remarks:
Isolation and the great distance to access the next level of care or a specialist is a concern for both providers and patients. For example, the Operating Room (OR) schedule book says, 'labor induction due to distance' [which may not be the best reason for delivering a baby].
The previous remarks infer a combined threat of severe weather with great distance relative to the family's situation. Transportation challenges coupled with the great distances to a specialist may require that rural-based providers make decisions about a patient's care that are less likely to present in an urban setting with an array of more accessible health-care resources. Another aspect of the rural context is the need for a nurse to be sensitive to the 'politics' that are inherent in the social structures of small towns, as evidenced by the following comments:
Insiders versus outsiders. The nurse must know whom the community views as insiders versus those who are outsiders. Small town residents have a preference for interacting with long established local residents (insider) versus a newcomer (outsider) to their community.
Familiarity and threats to privacy. In a small-town practice setting you must be very mindful of your demeanor and speech. The community grapevine is always very active. Maintaining confidentiality can be very difficult where everyone knows everyone else . . . when everyone has a vested interest in learning about what is happening in town . . . especially when someone is ill or has some kind of misfortune.
The theme of professional realities of rural nursing practice included the need to be comfortable with the generalist role, aware of limited opportunities to work in a specialty service, and sensitive to threats of maintaining anonymity when the nurse knows most of the patients and their families. Another concern centered on the need for rural nurses to be able to develop professionally in spite of less accessible continuing education opportunities. Respondents enrolled in nurse practitioner programs thought it probably was more difficult to educate rural consumers about the role and scope of practice of NPs, especially in a community that historically had been dominated by physician practices. Another professional reality related to the ability to provide a continuum of care in spite of the lack of resources, specifically shortages of health personnel, equipment, and time. Comments reflecting this theme are exemplified by the following remarks:
Difficulty recruiting qualified professional staff can lead to increased individual burnout. Limited access to state-of-the-art technology and educational conferences [can make it difficult], to maintain professional competence.
Another professional reality identified by respondents centered on isolation associated with great distances and not having face-to-face access to other health professionals, especially nursing colleagues, as reflected in the following comment:
In under-served regions nurses have increased responsibility and doctors rely heavily on their observations and skills. . . I sometimes feel diluted in a rural community . . . professionally isolated. Going back to school has brought me back in touch with nursing and the values and goals of the nursing profession.
The theme of patient-related considerations alluded to the nurse's need to understand rural social, cultural and economic factors, specifically the importance of health insurance, as reflected in the following statements:
Rural patients have diverse needs, are more likely to be uninsured and of lower socioeconomic status . . . and often do not understand the value of health promotion.
A family's cultural preferences may interfere with one of its members (ie, patient) receiving appropriate health care. Many people in the region where I work do not have health insurance. This [situation] presents significant challenges to providers of care who believe more should be done for a patient.
Obviously, based on the responses, a nurse who chooses rural practice must be creative and flexible in order to successfully plan and implement health care in light of rural cultural preferences, environmental contexts, and professional constraints.
Discussion
Overall, the findings in this pilot study revealed that students having an interest in rural practice post-graduation were more likely to be familiar with life in a rural community, as evidenced by the demographic information. As rural practitioners, these nurses need a wide range of nursing skills to care for individuals with diverse conditions across the life span; that is, familiarity with the role of 'expert-generalist'8,13,15. For example, a nurse in a rural hospital may care for an obstetrical patient (mother and baby), someone who had surgery for an acute condition, and an elderly person with an exacerbation of a chronic health problem - all on the same shift. While the generalist role seems overwhelming to many nurses, respondents in this study indicated familiarity with and even acceptance of that expectation.
Respondents who were familiar with the rural environment identified confidentiality issues as both a challenge and an opportunity for professional fulfillment. Maintaining anonymity is a concern for many rural people, even those who say they enjoy being personally acquainted with most others in their community. Nurses in particular tend to be viewed with high esteem by rural consumers, and this can make it difficult to have a life outside work. Some nurses find that recognition is a positive aspect of rural life, while others see it as an invasion of personal privacy13-15. In other words, maintaining confidentiality can present challenges to health professionals who live and work in a small town. Assumptions and leaks in confidentiality that result from chance encounters can quickly become 'facts' and public knowledge via an active community 'rumor mill'. Innovative approaches are required on the part of nurses in rural practice to assure patient confidentiality while at the same time treating others in the community with respect.
Isolation, both geographic and professional, was another salient theme that emerged in respondents' comments. Professional isolation requires an outstanding ability for a nurse who is practising alone to evaluate and prioritize needs and the types of services that can be provided to the local population. The lack of physical access to other providers, education, and technology can potentially cause considerable role strain. Individuals who are uncomfortable when working alone or who lack the confidence to make independent nursing decisions probably would not fare well in a remote rural area13,18-20.
Preparing nurses for rural practice
Even though respondents sought out learning opportunities to prepare them for the rural generalist role, they questioned whether or not their educational program adequately prepared them for this type of practice. Successful nurses in rural practice must be able to assess a community's health needs, have a good understanding of morbidity and mortality rates, and develop appropriate nursing care for individuals, groups, and communities with diverse needs and resources. Along with this content, nursing educators should expose students to rural theory and practice, help them learn about threats to anonymity and confidentiality where informal social structures predominate, and creatively plan a continuum of care within the constraints of less accessible resources8-10. In addition, students need to know about the importance of and strategies for self-care in isolated sparsely populated rural settings. Students having these skills will be more confident to apply for nursing positions in rural settings, and more likely to remain there long term18-20.
Respondents in this study suggested strategies based on personal insights that educators should consider to help address rural nursing shortages:
- Include rural theory and practice perspectives in all nursing courses; invite students and faculty from nursing with a rural background to share their insights; include case studies that have a rural perspective.
- Invite nurses from rural settings as guest lecturers to speak to students individually and in groups about rural practice in order to dispel myths and provide accurate information.
- Invite guest lecturers from other disciplines to talk about their experiences with rural practice and working with nurses in small communities. Examples of disciplines relevant to rural practice might include social work, medicine, dentistry, psychology, pastoral care, nutrition, geography, women's studies, education and law.
- Expose all students to the rural context, the rural health-care delivery system, and clients who live in rural areas.
- Arrange in-depth clinical experiences with rural providers for students having an expressed interest in this kind of practice to facilitate familiarity and comfort with rural practice.
- Promote mentoring arrangements in the form of short term internships and more extensive preceptorships between nurses in rural practice and students who have a rural interest as a way to foster networking that can continue post-graduation.
- Survey nurses in rural areas to learn about their particular education needs. Then, provide accessible continuing education programs (using technology when feasible) to help these nurses maintain clinical expertise and pursue advanced degrees.
- Foster academic-clinical research collaborative arrangements; then, encourage publication of the findings to expand the knowledge base for rural practice.
- Support federal, provincial/state and local entities that offer educational loans with a work pay-back option targeting remote, rural and underserved regions.
It is important to stress that the strategies listed above are based on individual experiences with a number of nursing education programs. Nurse researchers should investigate the most effective ways of implementing the strategies relative to rural practice and include perspectives from rural nursing administrators as well as those of nursing educators.
Limitations, implications and conclusion
This pilot study included a small self-selected sample, comprised of participants attending an international rural nursing conference; thus, generalizability of the findings is limited. Even so, the findings offer preliminary insights regarding factors that influence nursing students' post-graduation choosing of rural employment settings. Another limitation associated with the small sample size is that respondents were from only two nations (Canada and USA) but this reflected the demographic makeup of students who attended this international conference. While other students from Canada and other international destinations may have been interested in attending the conference, costs for travel may have prohibited them from doing so. Because this was a self-selected convenience sample, the findings may not reflect perspectives of other nursing students in those two nations or internationally. Moreover, open-ended pencil-and-paper surveys that elicit short answers limit response options and, consequently, affect the nature, completeness and interpretation of data. In order to learn more about rural nursing shortages and what motivates nursing students to work in rural settings, additional perspectives are needed from nursing students in Canada and the USA, as well from other nations. Additionally, data retrieved from focus groups comprised of students and nurses who practice in rural settings would provide a more complete picture of the phenomenon under investigation. Nursing educators and nursing administrators could use that kind of information to implement more effective education models to enhance the recruitment and retention of nurses in under served rural and remote areas.
The intrinsic value of having an adequate number of appropriately prepared nurses in rural communities cannot be overstated. For those considering this setting, it is advisable to learn about the scope of nursing practice in rural and remote settings by carefully reviewing the nurse practice Acts of a state or province. Likewise, personal knowledge of community norms and behaviors is extremely useful to help one make nursing decisions that are ethically sound and culturally appropriate. While there are challenges in rural practice, the rewards can be great. In the end, highly skilled and creative nurses are prepared to 'leave no stone unturned' when caring for patients in rural and remote communities.
References
1. American Hospital Association. Special workforce survey: Washington, DC. American Hospital Association, 2001.
2. Canadian Institute for Health Information. Nursing workforce getting older: One in three Canadian nurses is 50 or older. (Online) 2004. Available: http://www.cihi.ca/cihiweb/dispPage.jsp?cw_page=media_14dec2004_e (Accessed 24 December 2004.)
3. Canadian Nurses Association. Nursing statistics tell us Canada not prepared for next public health crisis. (Online) 2004. Available: http://www.cna-nurses.ca/_frames/search/searchframe.htm (Accessed 24 December 2004.)
4. Buerhaus P, Staiger D, Auerbach D. Trends: new signs of a strengthening U.S. nurse labor market? Health Affairs-web exclusive. (Online) 2004. Available: http://content.healthaffairs.org/cgi/content/full/hlthaff.w4.526/DC1 (Accessed 15 December 2004).
5. Buerhaus P, Staiger D, Auerbach D. Implications of an aging registered nursing workforce. JAMA 2000; 283: 2948-2954.
6. Hall H. Researchers at Vanderbilt School of Nursing report largest increase in RN employment nationwide in decades, yet crisis still looms. (Online) 2004. Available: http://sitemason.vanderbilt.edu/newspub/crmQtG%3Fid%3D15616 (Accessed 15 December 2004).
7. Sprateley E, Johnson A, Sochalski J, Spencer FM. The registered nurse population: Findings from the national sample survey. Bureau of Health Professions, HRSA, National Center for Health Workforce Analysis. (Online) 2002. Available: http://www.nurseweek.com/nursingshortage/rnsurvey.asp (Accessed 15 December 2004).
8. Bushy A. Orientation to nursing in the rural community. Thousand Oaks, CA: Sage, 2000.
9. Hegney D, McCarthy A. Job satisfaction and nurses in rural Australia. Journal of Nursing Administration 2000; 30: 347-350.
10. Nugent P, Ogle K, Bethune E, Walker E, Wellman D. Undergraduate pre-registration nursing education in Australia: A longitudinal examination of enrollment and completion numbers with a focus on students from rural and remote campus locations. Rural and Remote Health 4: 313. (Online) 2004. Available: http://rrh.org.au/ (Accessed on 15 December 2004).
11. Kerr J, MacPhail J. Concepts in Canadian Nursing. Toronto: Mosby, 1996.
12. Kirby M, LeBreton M. The health of Canadians - the Federal role. Ottawa: The Standing Senate Committee on Social Affairs, Science and Technology, Parliament of Canada, 2002.
13. Leipert B. Women's health and the practice of public health nurses in northern British Columbia. Public Health Nursing 1999; 16: 280-289.
14. Leipert B, Reutter L. Women's health and community health nursing practice in geographically isolated settings: A Canadian perspective. Health Care for Women International 1998; 19: 575-588.
15. Leipert B, Reutter L. Developing resilience: how women maintain their health in northern geographically isolated settings. Qualitative Health Research 2005; 15: 49-65.
16. Palosky C, Peacock C & Holland H. Five years after IOM report on medical errors nearly half all consumers worry about the safety of their health care. Menlo Park, CA: Kaiser Family Foundations. (Online) 2004. Available: http://www.kff.org/kaiserpolls/pomr111704nr.cfm (Accessed 15 December 2004).
17. Romanow R. Building on values: The future of health care in Canada. Ottawa: The Romanow Commission Report. (Online) 2002. Available: http://publications.gc.ca/control/publicationInformation?searchAction=2&publicationId=237274 (Accessed 12 April 2005).
18. Congdon J, Magilvy J. The changing spirit of rural community nursing: documentation burden. Public Health Nurse 2000; 12: 18-24.
19. Long K, Scharff J, Weinert C. Advanced education for the role of rural nursing generalist. Journal of Nursing Education 1997; 36: 91-94.
20. Long K, Weinert C. Rural nursing: Developing the theory base. Scholarly Inquiry for Nursing Practice 1989; 3: 113-127.

