Participation in competitive sports at the youth level has seen a large number of participants recently, specifically in secondary school athletics. In 2013 the National Federation of High School Associations estimated that 7.8 million student athletes were participating in interscholastic sports1. Due to the significant number of individuals participating in sports, many organizations have adopted and provided recommendations to provide appropriate health care for this specific population of athletes. The National Athletic Trainers Association (NATA), the American Academy of Family Physicians, and the American Medical Association have all advocated for the employment of athletic trainers to provide appropriate medical coverage at high school athletic events2,3.
The recommendation for the provision of a healthcare system in high school sports is grounded in the epidemiological data present in the literature, which details a wide variety of sports-related injuries and conditions affecting high school athletics. Orthopedic injury rates in high school sports vary by gender and activity; however, the consistent theme present in the literature is that high school athletes are sustaining orthopedic injuries that require medical attention4,5. In addition to orthopedic conditions requiring medical care, special attention should be given to the incidence of general medical conditions relating to cardiovascular disease, with an estimated 100 deaths per year6, and heat-related illness, with an estimated 9000 cases treated by medical providers each year7 in high school athletes alone. In the absence of a certified athletic trainer or other healthcare provider, there is an increased reliance on coaches to provide the emergency care required to treat these conditions.
The emergence of sudden cardiac death as a pressing healthcare concern amongst athletic participants cannot be overlooked. While there is debate over the exact number of sudden cardiac emergencies that occur in high school sports, the most significant associated issue is its typical occurrence in an athlete who would otherwise be considered healthy and symptom free6. Recent literature has indicated that the incidence of sudden death appears to be eight times higher when compared to non-athletes8, while specifically the number of deaths in high school sports from indirect causes is significantly higher than for direct traumatic causes9. Numerous predisposing factors have been presented in the literature in an effort to specifically decrease sudden deaths in athletics relating to structural and functional abnormalities of the heart10.
Previously, authors have recommended the use of more advanced medical imaging including electrocardiograms, to identify the various cardiovascular conditions that may lead to sudden cardiac death. However, this is currently only recommended for those individuals who meet the American Heart Association's risk factors for a cardiovascular incidents11,12. The high number of false positive tests13 along with the increasing cost of medical screening, US$2 billion annually14, has made the use of advanced screening tools for all athletes a non-practical method for identifying abnormalities.
Assessing the level of medical services provided to secondary schools in a more rural area is of vital concern due to the fact that rural areas in the USA have disproportionate health disparities and fewer healthcare resources available when compared to more urbanized cities10. It is documented that individuals from rural communities do not seek the same preventative services as their urban counterparts15 and have higher rates of obesity and sedentary lifestyles, which can lead to cardiac disease16,17. With only 29 people per square kilometer, West Virginia is the second most rural state in the nation18. West Virginia has elevated rates of health risk behavior and chronic disease and an above-average number of families and individuals living below the poverty line19,20.
The risk factors of rural healthcare availability and access, coupled with the increased time between cardiac events and advanced medical care in rural areas, are substantial barriers to providing the appropriate level of health care to student athletes in rural areas. Additionally, a number of previous studies have shown inconsistent medical coverage of high school sports, specifically football21,22.
Numerous recommendations have been made to provide a more cost-effective and efficient level of health care to secondary school athletics. These recommendations include providing access to automated external defibrillators (AEDs), implementing emergency action plans (EAPs) and providing medical coverage to all sporting events3,23,24.. The purpose of this study was to determine the level of implementation of emergency preparedness and administrative procedures to provide appropriate medical coverage to high school athletics in the predominantly rural state of West Virginia. Particular attention was given to determine the extent to which the schools provided the recommendations for best practice in the NATA consensus statement outlining appropriate medical coverage for high school athletics3.
Procedures
A listing of all public schools participating in the state high school athletic association with at least one team participating in interscholastic competition was obtained from the West Virginia Department of Education office. Out of the 125 secondary schools in the state, 62 schools were represented in this study, yielding a response rate of approximately 50%. The respondents classified the enrollment of their school as 1A (43.5%), 2A (19.4%), and 3A (35%). The majority of schools (66%) reported a rural zip code at the school level based on Rural Urban Community Area Codes (RUCAs). Each school administrator received an email letter describing the overall purpose of this study, the estimated time for completion of the questionnaire and an electronic link to access the survey instrument. The email also provided contact information for the investigators if the participants had questions or regarding the instrument or results of the study. An administrator from each school was asked to complete a survey specifically assessing policies, procedures and equipment in place at their respective school corresponding the consensus statement points. They were instructed to complete this survey honestly and were given the opportunity to provide feedback regarding the perceived barriers to health care provided. A total of 62 respondents completed the survey (49.6% response rate). The majority of the respondents were principals (92%), followed by athletic administrators (8%).
Instrumentation
An online, cross-sectional, survey utilizing SurveyMonkey was used to gather demographic information along with responses on emergency preparedness. The electronic survey was designed to reduce mailing costs and encourage participation. The survey was organized and constructed to determine compliance with the NATA consensus statement on Appropriate Medical Coverage for Secondary Schools3. The areas specifically examined were aligned with consensus statement 2, 'Development and implementation of a comprehensive athletic healthcare administrative system', and statement 5, 'Development and implementation of a comprehensive EAP'. The questions were a component of the Self-Appraisal Checklist for Health Supervision in Scholastic Athletic Programs25 originally utilized assessing medical care to secondary schools in Arkansas26. Open-ended questions assessed barriers and facilitators to successful sports medicine programs. All questions were drafted using a Likert-type scale with five choices reflecting the level of preparedness and availability of services ('never', 'seldom', 'sometimes', 'always', 'do not know'). School demographics were also measured and school zip codes were collected to determine rurality based on RUCAs. This is a subcounty classification commonly used to classify rural/non-rural areas based on population density and population commuting patterns27.
Data analysis
When responses were received, the statistical information was compiled and analyzed to determine completion of all questions. The Statistical Package for the Social Sciences for Windows v21.0 (SPSS; http://www.spss.com) was used to complete the statistical analysis. Descriptive statistics were gathered and analyzed for each of the individual questions in the instrument and were classified categorically into the recommendations provided in the NATA statement. In addition, all participants were given an opportunity to provide qualitative responses to open-ended questions, which were analyzed independently by three researchers for recurring themes. Only themes with 100% agreement among researchers were reported and discussed. Each respondent self-classified the school according to the class size of the West Virginia Secondary School Activities Commission classifications. Class 3A is identified as having 778 or more students, Class 2A is classified as 429-777 students, and Class 1A is classified as having 0-428 students.
Ethics approval
This study was approved by the Concord University Human Subjects Review Board (project number S13-18).
Consensus statement point 1: 'Develop and implement a comprehensive athletic healthcare administrative system'
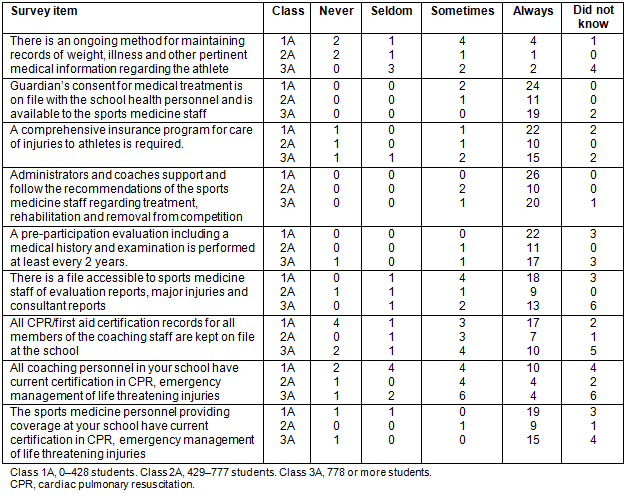
The majority of respondents reported that there was always a consent form on file for student athletes (91%) and comprehensive insurance was required for participation in athletics (80%). However, when questioned if there was an ongoing method for maintaining records of weight and illnesses, 16% of schools responded 'never' and 8% of schools responded 'seldom'.
Over half (56%) reported that CPR and first aid certification records of all members of the coaching staff were always kept on file. Thirty-three percent of respondents reported that all members of the coaching staff were certified in CPR and first aid and 31% responded 'never' when asked if all coaches were certified in CPR and first aid (Table 1).
Table 1: Assessment of development of the implementation of a comprehensive athletic healthcare system
Consensus statement point 5: 'Develop and implement a comprehensive emergency action plan'
When asked if there was a written EAP that outlines procedures to follow in emergency situations during athletic participation, 36% responded 'never' and 38% responded 'always'. The majority (66%) reported that there was an adequate and readily available communication system between the athletic participation area and paramedical assistance. When asked if there was a written plan for the transportation of injured athletes in practice and in contests in an emergency situation only 38% responded 'always'. When asked if there was a written plan for the transportation of injured athletes in practice and competitions for contests in non-emergency situations an equal number of respondents (36%) responded 'never' and 'always' (Table 2).
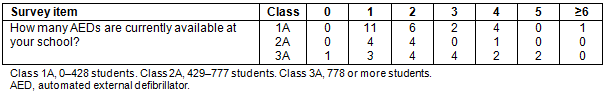
The majority (76%) reported that there was an AED readily available and one school reported there was no AED present on site. A majority of the participants stated their school had more than one AED on site (62%; Tables 3,4).
Table 2: Assessment of development and implementation of a comprehensive emergency action plan
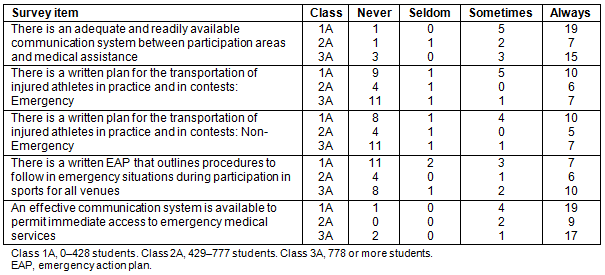
Table 3: Availability of automated external defibrillators at practice and competition
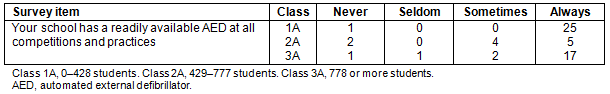
Table 4: Number of automated external defibrillators at respondent schools
Open-ended question 1: 'What limitations does your school have in providing health care to athletes?'
Three themes were present within the responses to the first open-ended question, including lack of funding, lack of certified medical personnel, and an inability to find certified personnel in a rural area (Table 5).
Open-ended question 2: 'What would make it easier to provide health care to athletes at your school?'
Four themes were present within the responses to the second open-ended question, including providing more funding, more certified staff, appropriate treatment space/facilities, and continuing education (Table 5).
Table 5: Sample responses to open-ended questions (chosen responses based on recurring themes)

Discussion
The survey examined the recommendations set forth in the Appropriate Medical Care for the Secondary School-Aged Athlete summary statement published by NATA3. This study specifically reviews information related to statements 1 and 5.
Consensus statement point 1: 'Develop and implement a comprehensive athletic healthcare administrative system'
The development of proper administrative procedures should be a critical component of all public facilities operations. One of the primary components of the administrative system should be proper education and oversight of the athletics program. When no qualified medical personnel, such as an athletic trainer, is present at athletic events, coaches and other athletic staff are often relied upon to provide first aid and manage injuries to the participants. Ensuring that the athletic staff has proper knowledge in the areas of first aid, CPR and management of injuries is essential to the long-term health and safety of all those participating.
Through this study, the authors were able to assess the overall athletic staff's certification rates. One-third (33%) of the schools reported that they always required the coaching staff to maintain certification. Similarly, 31% reported that they never mandated all coaches remain certified in CPR and first aid. These numbers are consistent with a previous study that found less than 50% of coaches in rural South Dakota were currently certified in CPR and first aid28. According to the state athletic association, all coaches must achieve certification initially in CPR and first aid, but there is currently no requirement to maintain certification.
The academic preparation of high school coaches across the USA is typically in the form of an undergraduate physical education curriculum. Compared to an athletic trainer or other allied health professional, the level of preparation and coursework in this field committed to first aid and injury management and prevention is significantly lower. Unfortunately, in the absence of an athletic trainer at the high school, the coach is forced to assume the role of the medical provider and manage and treat injuries that have the potential to become life threatening.
Numerous studies have demonstrated the relatively low knowledge of high school coaches in regards to a variety of health-related issues associated with athletic participation, specifically in the management and recognition of concussion symptoms29,30, as well as alarmingly low passing scores on a first aid31, and knowledge of fluid replacement and hydration strategies32. The present study did not assess the coaches' knowledge in this area; however, the implementation of a healthcare administrative system with individuals possessing knowledge in these areas or at minimum enhancing education in the coaches is essential in reducing the risk of serious injury. It has been documented that knowledge has increased after completion of educational workshops instructing coaches on management of sports related injuries33. This should be an important consideration when assessing the needs and planning of every interscholastic athletic program.
Consensus statement point 5: 'Develop and implement a comprehensive emergency action plan'
The implementation of a comprehensive EAP is another method designed to decrease the risk of death in athletes24,34,35. This emergency plan should encompass all aspects of medical care including implementation of care to be provided, equipment available to be used in case of an emergency, communication methods to access emergency medical services and activate the emergency response, and transportation methods to and from the facility for injured and non-injured individuals24.
It has been previously reported that 79% of individuals suffering from sudden cardiac arrest survived in locations where an EAP was published compared to a 44% survival rate in locations where there was no EAP36. The results of the present study showed that only 38% of the schools in the state had a published EAP for all of the athletic venues and 36% reported that they did not. Currently, not all states have mandated that employment of athletic trainers or EAPs be present. Legislation requiring increased levels of health care and emergency planning in high schools has proven effective in Hawaii, which requires athletic trainers to be employed at every high school37, and in Tennessee, which saw an increase in EAPs and AEDs in the high schools after legislation was passed38.
Recently, there has been a major public effort to get AEDs and EAPs in all places where the public gathers, in order to decrease the risk of out-of-hospital mortality. AEDs are a widely accepted out-of-hospital method to provide care to an individual experiencing a cardiac event. Schools that possess written EAPs also tend to have an AED program in place to deal with sudden cardiac arrests39. This illustrates the need for every school to have a written EAP and associated cardiac care plan to increase the survival rates of individuals with a sudden cardiac condition. This 'chain of survival' concept has been widely recommended by the American Red Cross as well in the literature40.
The results of the present study showed that the majority (76%) of schools in the state always had an AED present. This is consistent with results in other rural communities showing 81% of schools in the state of Vermont having at least one AED present34,41. While the present study did not look at the mortality rates associated with sudden cardiac arrests at the high schools, previous studies have shown survival rates of up to 71% when defibrillation was performed on site by an AED36. This is an increase of survival from previous studies that showed there was a 21% survival rate of sudden cardiac deaths from the years 2000 to 200642.
Participants in the present study consistently expressed the desire to provide more medical services to the athletes, yet the major barrier prohibiting the provision of services was consistently cited as a lack of funding. This lack of financial support is commonly cited as the major mitigating factor in provision of health care43. Due to the economic hardship experienced by many in West Virginia, this barrier is not surprising.
Increasing funding along with increased legislation could very well prove to be an essential component to decrease the risk associated with athletic participation, specifically in underserviced rural communities.
With only 20 out of the 56 schools responding stating that they currently had a Board of Certification certified athletic trainer on staff, along with a majority of the respondents stating that the healthcare provider was only present for football, identifying methods to provide improved care to high school athletics is essential to reduce the rate of sudden death amongst this population. Because advanced cardiac screening on every athlete is neither cost-effective nor practical, alternative methods should be examined and when possible implemented. While it is recommended that high school sports employ an athletic trainer, proper funding and facilities for these positions is often lacking. Developing an EAP and requiring coaches to maintain first aid and CPR certifications are very easy and very low cost steps to enhance the health care of athletes. This is an essential component of all school athletic programs without a qualified medical professional present at practices and games. These two simple steps may help reduce the risk of a sudden cardiac event or other life-threatening injury and reduce the legal liability of the school district and employees.
Limitations in this study include problems associated with survey data including social desirability bias. Additionally, while every effort was made to ensure the confidentiality of their responses, school personnel might be hesitant to report information that would show non-compliance with state or national policies. While RUCA codes were used to measure rurality, the zip codes were at the school, not individual, level. Thus, the rural/non-rural designations might not be appropriate when considering some school locations may be placed outside of more densely populated areas to accommodate traffic and school facilities. Further, since the sample was collected from West Virginia, a largely rural state, the non-rural areas are unlikely to be considered urban. Additionally, with a 50% response rate, selection bias could influence results and thus the data might not be representative of the state or all rural areas.
Preparing for a life-threatening emergency in secondary school athletics is vital to reducing the number of sudden cardiac deaths among young athletes. Alternative funding sources to provide AEDs and improve health care in rural communities should be a priority, especially in high-risk areas. Without proper funding, schools will continue to find it difficult to provide the appropriate level of health care recommended by numerous organizations, which may result in dangerous amounts of time waiting for advanced medical support to arrive. While the barriers in West Virginia are significant, inexpensive and achievable steps could be taken to increase the safety of athletics for students in this rural state. Where appropriate healthcare providers are lacking at secondary school events, coaches should be required to maintain training and certifications in first aid, CPR and emergency care to ensure increased survival rates in the event of a catastrophic injury or event. Thus, increasing legislation or requiring all secondary schools to possess EAPs and AEDs as well as have qualified medical personnel at all events should be a priority for all individuals involved in secondary school athletics, in both rural and non-rural locations.
References
1. National Federation of State High School Associations. 2012-2013 high school athletics participation survey. (Internet). Available: http://www.nfhs.org/ParticipationStatics/ParticipationStatics.aspx/. (Accessed 5 September 2014).
2. Courson R, Goldenberg M, Adams, KG, Anderson SA, Cooper L, Dewald L, et al. Inter-association consensus statement on best practices for sports medicine management for secondary schools and colleges. Journal of Athletic Training 2014; 49(1):128-137. https://doi.org/10.4085/1062-6050-49.1.06
3. Almquist J, Valovich Mcleod TC, Cavanna A, Jenkinson D, Lincoln AE, Loud K, et al. Summary statement: appropriate medical care for the secondary school-aged athlete. Journal of Athletic Training 2008; 43(4): 416. https://doi.org/10.4085/1062-6050-43.4.416
4. Swenson DM, Collins CL, Fields SK, Comstock RD. Epidemiology of US high school sports-related ligamentous ankle injuries, 2005/6-2010/11. Clinical Journal of Sports Medicine 2013; 23(3): 190-196. https://doi.org/10.1097/JSM.0b013e31827d21fe
5. Swenson DM, Henke NM, Collins CL, Fields SK, Comstock RD. Epidemiology of United States high school sports-related fractures, 2008-09 to 2010-11. American Journal of Sports Medicine 2012; 40(9). https://doi.org/10.1177/0363546512453304
6. Maron BJ, Doerer JJ, Haas TS, Tierney DM, Mueller FO. Sudden deaths in young competitive athletes: analysis of the 1866 deaths in the United States, 1980-2006. Circulation 2009; 119(8): 1085-1092. https://doi.org/10.1161/CIRCULATIONAHA.108.804617
7. Kerr ZY, Casa DJ, Marshall SW, Comstock RD. Epidemiology of exertional heat illness among U.S. high school athletes. American Journal of Preventative Medicine 2013; 44(1): 8-14. https://doi.org/10.1016/j.amepre.2012.09.058
8. Maron BJ, Haas TS, Duncanson ER, Garberich RF, Baker AM, Mackey-Bojack S. Comparison of the frequency of sudden cardiovascular deaths in young competitive athletes versus nonathletes: should we really screen only athletes? American Journal of Cardiology 2016; 117(8): 1339-1341. https://doi.org/10.1016/j.amjcard.2016.01.026
9. Boden BP, Breit I, Beachler JA, Williams A, Mueller FO. Fatalities in high school and college football players. The American Journal of Sports Medicine 2013; 41(5): 1108-1116. https://doi.org/10.1177/0363546513478572
10. Batra AS, Hohn AR. Consultation with the specialist palpitations, syncope and sudden cardiac death in children: who's at risk? Pediatrics in Review 2003; 24(8): 269-275. https://doi.org/10.1542/pir.24-8-269
11. Aisf IM, Drezener JA. Sudden cardiac death and preparticipation screening: the debate continues - in support of electrocardiogram-inclusive preparticipation screening. Progress in Cardiovascular Diseases 2012; 54(5): 445-450. https://doi.org/10.1016/j.pcad.2012.01.001
12. Corrado D, Drezner J, Basso C, Pelliccia A, Thiene G. Strategies for the prevention of sudden cardiac death during sports. European Journal of Cardiovascular Prevention and Rehabilitation 2011; 18(2): 197-208. https://doi.org/10.1177/1741826710389924
13. Lawless CE, Best TM. Electrocardiograms in athletes: interpretation and diagnostic accuracy. Medicine and Science in Sports and Exercise 2008; 40(5): 787-798. https://doi.org/10.1249/MSS.0b013e318164dd18
14. Wheeler MT, Heidenreich PA, Froelicher VF, Hlatky MA, Ashley EA. Cost-effectiveness of preparticipation screening for prevention of sudden cardiac death in young athletes. Annals of Internal Medicine 2010; 152(5): 276-286. https://doi.org/10.7326/0003-4819-152-5-201003020-00005
15. Skinner AC, Slifkin RT. Rural/urban differences in barriers to and burden of care for children with special health care needs. Journal of Rural Health 2007; 23(2): 150-157. https://doi.org/10.1111/j.1748-0361.2007.00082.x
16. Perez AP, Munoz JY, Cortes VB, de Pablos Velasco P. Obesity and cardiovascular disease. Public Health Nutrition 2007; 10(10): 1156-1163.
17. Patterson PD, Moore CG, Probst JC, Shinogle JA. Obesity and physical inactivity in rural America. The Journal of Rural Health 2004; 20: 151-159. https://doi.org/10.1111/j.1748-0361.2004.tb00022.x
18. US Census Bureau. State and county quickfacts: West Virginia 2010. (Internet). Available: http://quickfacts.census.gov/qfd/states/54000.html (Accessed 21 January 2012).
19. Centers for Disease Control. West Virginia: burden of chronic diseases. (Internet) 2008. Available: http://www.cdc.gov/chronicdisease/states/pdf/west_virginia.pdf (Accessed 10 June 2011).
20. Census. West Virginia fact sheet. (Internet) 2010. Available: http://www.census.gov/ (Accessed 10 June 2011).
21. Konin JG, Morris BJ, Liller K, Carey A, Coris E, Pescasio M. Status of medical coverage for high school football games in Florida. Athletic Training and Sports Health Care 2011; 3(5): 226-229. https://doi.org/10.3928/19425864-20110228-01
22. Tonino PM, Bollier MJ. Medical superivsion of high school football in Chicago: does inadequate staffing compromise healthcare? The Physician and Sportsmedicine 2004; 33(2): 37-40. https://doi.org/10.3810/psm.2004.02.123
23. Casa DJ, Almquist J, Anderson SA, Baker L, Bergeron MF, Biagioli B, et al. The inter-association task force for preventing sudden death in secondary school athletics programs: best practices recommendations. Journal of Athletic Training 2013; 48(4): 546-553. https://doi.org/10.4085/1062-6050-48.4.12
24. Anderson JC, Courson RW, Kleiner DM, Douglas M, McLoda TA. National Athletic Trainers Association position statement: emergency planning in athletics. Journal of Athletic Training 2002; 37(1): 99-104.
25. American Academy of Pediatrics, Committee on Sports Medicine. A self-appraisal checklist for health supervision in scholastic athletic programs. Elk Gove Village, IL: American Academy of Pediatrics, 1993.
26. Dewitt TL, Unruh SA, Seshardri, S. The level of medical services and secondary-school aged athletes. Journal of Athletic Training 2012; 47(1): 91-95.
27. Washington, Wyoming, Alaska, Montana, and Idaho Rural Health Research Center. Rural-Urban Community Area Codes (RUCAs). (Internet). Available: http://depts.washington.edu/uwruca/index.php (Accessed 25 March 2015).
28. Cross PS, Karges JR, Adamson AJ, Arnold MR, Meier CM, Hood JE, et al. Assessing the knowledge on injury management among high school athletic coaches in South Dakota. South Dakota Medicine 2010; 63(7): 241-245.
29. McLeod TC, Schwartz C, Bay RC. Sport-related concussion misunderstandings among youth coaches. Clinical Journal of Sports Medicine 2007; 17(2): 140-142. https://doi.org/10.1097/JSM.0b013e31803212ae
30. Guilmette TJ, Malia LA, McQuiggan MD. Concussion understanding and management among New England High School football coaches. Brain Injury 2007; 21(10): 1039-1047. https://doi.org/10.1080/02699050701633080
31. Ransone J, Dunn-Bennett LR. Assessment of first aid knowledge and decision making of high school athletic coaches. Journal of Athletic Training 1999; 34(3): 267-271.
32. Geijer JR, Pitney WA, Bradenburg J. Fluid replacement knowledge and sources of hydration information among Illinois high school athletic coaches. The Internet Journal of Allied Health Sciences and Practice 2009; 7(3): 1-6.
33. O'Donoghue EM, Onate, JA, Van Lunen, Peterson CL. Assessment of high school coaches' knowledge of sports-related concussion. Athletic Training and Sports Health Care 2009; 1(3): 120-132. https://doi.org/10.3928/19425864-20090427-07
34. Wasilko SM, Lisle DK. Automated external defibrillators and emergency planning for sudden cardiac arrest in Vermont high schools: a rural state's perspective. Sports Health: A Multidisciplinary Approach 2013; 5(6): 548-552. https://doi.org/10.1177/1941738113484250
35. Drezner JA, Courson RW, Roberts WO, Mosesso VN, Link MS, Maron BJ. Inter-association task force recommendations on emergency preparedness and management of sudden cardiac arrest in high school and college athletic programs: a consensus statement. Heart Rhythm 2007; 4(4): 549-565. https://doi.org/10.1016/j.hrthm.2007.02.019
36. Drezner JA, Toreshadl BG, Rao AL, Huszti E, Harmon KG. Outcomes from sudden cardiac arrest in US high schools: a 2 year prospective study from the national registry for AED use in sports. British Journal of Sports Medicine 2013; 47(18): 1179-1183. https://doi.org/10.1136/bjsports-2013-092786
37. Buxton BP, Okasaki EM, McCarthy MR, Ho KW. Legislative funding of athletic training positions in public secondary schools. Journal of Athletic Training 1995; 30(2): 115-120.
38. Watson AM, Kannankeril PJ, Meredith M. Emergency response planning and sudden cardiac arrests in high schools after automated external defibrillator legislation. The Journal of Pediatrics 2013; 163(6): 1624-1627. https://doi.org/10.1016/j.jpeds.2013.07.024
39. Monroe A, Rosenbaum DA, Davis S. Emergency planning for sudden cardiac events in North Carolina high schools. North Carolina Medical Journal 2009; 70(3): 198.
40. Cummins RO, Ornato JP, Theis WH, Pepe PE. Improving survival from sudden cardiac arrest: The 'Chain of survival' concept. Circulation 1991; 83(5): 1832-1847.
41. Mercer CW, Rhodes LA, Phillips JR. Automated external defibrillators in West Virginia schools. The West Virginia Medical Journal 2012; 108(4): 8.
42. Drezner JA, Chun JS, Harmon KG, Derminer L. Survival trends in the United States following exercise related sudden cardiac arrest in youth: 200-2006. Heart Rhythm 2008; 5(6): 794-799. https://doi.org/10.1016/j.hrthm.2008.03.001
43. Cronin O, Jordan J, Quigley F, Molloy MB. Prepared for sudden cardiac arrest? A cross-sectional study of automated external defibrillators in amateur sport. British Journal of Sports Medicine 2013; 47(8): 1179-1183. https://doi.org/10.1136/bjsports-2013-092919
