Introduction
Little is known about the frequency and aetiology of functional gastrointestinal (GI) disorders in the general population. The two most common functional gastrointestinal disorders in the population are functional dyspepsia and irritable colon. Non-ulcer dyspepsia, or the more recent term functional dyspepsia (FD), is used for persistent upper GI symptoms in the absence of a known organic disease. Irritable bowel syndrome (IBS) is characterised by persistent or recurrent abdominal pain related to defecation or to chronic disturbance of bowel habits in the absence of demonstrable organic disease. IBS tends to be a chronic recurring disorder with variable illness episodes that may continue for many years1. Despite the fact that this gastrointestinal condition is quite commonly diagnosed in primary care and by gastrointestinal specialists, there is limited data on the rates of healthcare utilization by patients with IBS2.
Although this subject has received much attention during the past few years in European literature3,4, it is still neglected in Southern Europe, where research in this area is scarce5. For this reason, the current study of the burden of functional gastrointestinal disorders (FD and IBS) and gastroenteritis in the primary care setting on rural Crete was undertaken. In addition, an aim was to explore whether the disorders' diagnoses are consistent with those reported in other European and international studies. The aim of this article was to report on frequencies of FD, IBS and gastroenteritis within the primary-care setting, and to provide some information on the extent to which the recorded diagnoses in physicians' notes fulfil the existing diagnostic criteria.
Method
Setting and study design
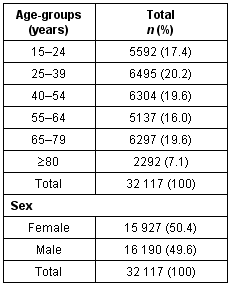
A retrospective study was designed by identifying new cases of functional gastrointestinal disorders. Our study was carried out in rural Crete (which is served by 15 primary health care [PHC] centres and two small community hospitals) based on a patient-records system (Fig 1). Five of these PHC were selected, three located in remote rural areas: Spili (8962 population), Anogia (8204 population) and Perama (11 453 population); and two in semi-rural areas: Neapoli (7183 population) and Archanes (4279 population). These PHC centres covered a total population of 40 081, of which 32 117 persons were aged 15 years and over (Table 1).
Figure 1: Map of the study area, Crete.
Table 1: Descriptive epidemiology of the reference population
Data collection
All available electronic or paper medical records in the studied locations from the period March 1996 to February 2000 (in total 280 000 visits) were reviewed retrospectively for all diagnoses, medical complaints and symptoms related to the GI tract, as noted by the local physician. All records were reviewed by one medical doctor from the research team and validated against pre-defined criteria for gastroenteritis, FD and IBS. The review was completed within 10 months. Information on demographics, co-morbidity and medication was retrieved from the medical records by means of a standardised registration form, and subsequently stored in a research database.
Gastroenteritis was defined as acute diarrhoea, mild to severe with or without vomiting and with or without fever. Information relevant to the findings of recent history (overseas travel, hiking or camping, shellfish consumption, childcare etc) and faecal and blood examination findings consistent with viral or infectious gastroenteritis (blood and/or leukocytes in stools or isolation of bacteria in stools culture was supportive of this diagnosis). We also included all cases with the diagnoses 'diarrhoea and fever,' 'diarrhoeic syndrome,' and 'acute diarrhoea.' all cases that met the criteria defined by Talley (any persistent or recurrent pain or discomfort centred in the upper abdomen, where evidence of organic disease likely to explain the symptoms is absent, including an upper endoscopy)6 for FD, together with those diagnosed as 'epigastralgia,' 'pain in the upper abdomen' or 'dyspeptic disorders' were included in the dyspepsia group. Similarly, cases that met the Rome II criteria for IBS (abdominal pain or discomfort relieved by defecation or associated with change in frequency of stool or in the form of stool)7, or were diagnosed by the local physician as 'spastic colon' or 'spastic colitis', were included in the IBS group. Where the physician recorded a diagnosis of gastroenteritis, dyspepsia and IBS, it was included in the study, irrespective of whether all defined diagnostic criteria were met or not.
In total, 280 000 consecutive visit notes were reviewed. During the 4 year study period, patients with a prior diagnosis of cancer, alcoholism, pancreatitis, peptic ulcer, gastro-oesophageal disease, inflammatory bowel disease and colecystitis, in addition to patients with a previously known use of antacids, antispasmolytics and acid suppressing drugs were excluded, together with pregnant women. Patients who were not inhabitants of the areas of responsibility of the 5 PHC centres were also excluded from the study. In total, 1400 cases fulfilled one or more of the exclusion criteria and were excluded. Information regarding age was lacking for 7.5% (n = 123) of the patients identified (88 patients with gastroenteritis, 29 patients with dyspepsia and 6 patients with IBS).
The study was approved by the Ethical Committee at the University Hospital of Heraklion, Crete.
Statistical analysis
The total number of person-years (aged 15 years and over) in the 4 year study period was 128 468. Relative risks were calculated on the crude data. In the calculation of occurrence rates, cases with missing information regarding age were distributed proportionally into the age-groups (15-24, 25-39, 40-54, 55-64, 65-79, 80 years and over) according to the age-distribution for each disease.
Rates for the cases in the study were calculated as occurrence rates per 1000 person-years. Odds ratios (OR) and 95% confidence intervals (CI) between men and women were also calculated.
Results
The total number of the identified GI cases was 1670 with 25 out of these having more than one of the three diagnoses registered during the study period. The number aged more than 14 years old was 1389. The most common diagnosis in all GI cases was gastroenteritis, accounting for 1130 cases (68.7%), followed by dyspepsia with 394 cases (23.9%), and IBS with 146 cases (8.9%). Among the total number of IBS cases, there were 12 cases that also had a diagnosis of gastroenteritis, which constitute 8.2% of the total IBS diagnosis group. However, four of these 12 IBS cases had a documented history of IBS before they received the gastroenteritis diagnosis.
No case of celiac disease was observed in this population. There was a slight upward trend over time for gastroenteritis cases, while the annual occurrence rates of dyspepsia and IBS cases was relatively stable during the 4 year study period (Figure 2).
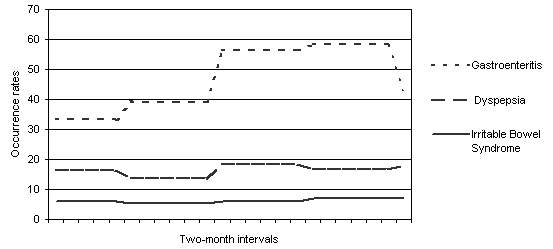
Figure 2: Number of new cases over the study period divided into 2 month periods.
The vast majority of all the GI cases found were seen and confirmed by the GP of the PHC centre. Two percent of the gastroenteritis and dyspepsia cases, and none of the IBS cases were confirmed by a GP and also referred to a specialist. Four percent of the IBS cases and none of the dyspepsia or gastroenteritis cases were confirmed solely by a gastroenterologist.
Four hundred and eighty two (42.6%) of all the gastroenteritis cases were diagnosed by a local physician. The remaining 649 cases (57.4%) were diagnosed by the research team physician on the basis of symptoms noted in the medical record (eg acute, mild or severe diarrhoea, with or without vomiting, and with or without fever). In 1008 (89.2%) of the defined cases, one or several symptoms of gastroenteritis were recorded in the medical records. Results from stool culture were only available for less than 3% of the cases. Dyspepsia was diagnosed by the local physician in 70 (17.8%) of the total study cases and 324 (82.2%) were diagnosed by the research physician on the basis of relevant symptoms recorded in the medical record. The most common symptoms of dyspepsia (persistent or recurrent pain or discomfort centred in the upper abdomen) were present in 352 (89.3%) of the cases. Of all the IBS cases, 119 (81.5%) were labelled by the local physician and 27 (18.5%) were diagnosed by the research team. The discrepancy between 'note recorded diagnosis' and 'retrospective researcher diagnosis' is illustrated (Table 2).
Table 2: Note-recorded diagnosis versus retrospective researcher diagnosis on functional gastrointestinal disorders in rural Crete

The distribution of the three selected diagnoses was quite similar among all the centres. However, for one of the centres (Anogia) the proportion of patients with an IBS diagnosis was lower (p = 0.05) than among the others.
The occurrence rates of gastrointestinal disorders for those over the age of 15 years and odds ratio between men and women are presented (Tables 3-5). The observed total occurrence rate for gastroenteritis was 7.1 per 1000 person-years in the studied population. Gastroenteritis tended to be somewhat higher among the younger age groups and among those over the age of 65 years. There was no sex difference seen for gastroenteritis (p = 0.39).
Table 3: Occurrence rates of gastroenteritis per 1000 person-years by gender and for those over the age of 14 years
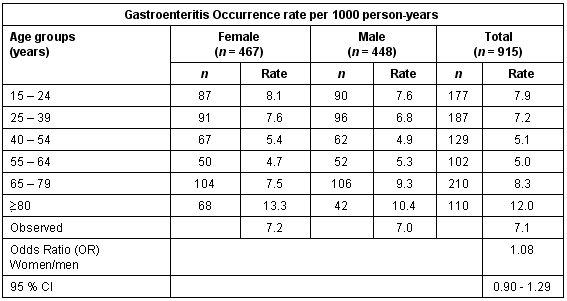
Table 4: Occurrence rates of dyspepsia per 1000 person-years by gender and for those over the age of 14 years
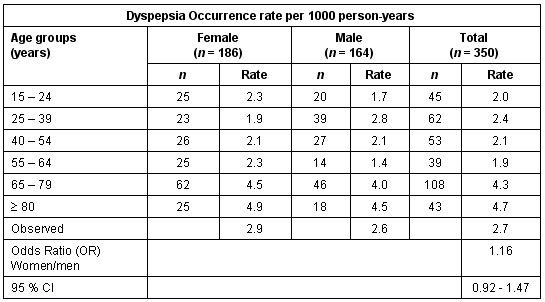
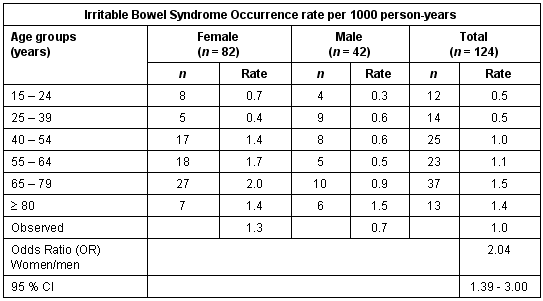
Table 5: Occurrence rates of irritable bowel syndrome per 1000 person-years by gender and for those over the age of 14 years
The observed total occurrence rate for dyspepsia was 2.7 per 1000 person-years in the studied population. An increased rate of dyspepsia was seen among those over the age of 65 years. Men in the age group of 25-39 years had a higher rate of dyspepsia compared with women in the same age-group. A similar but opposite trend was seen among women in the age-group of 55-64 years. In this population, women tended to have a slightly higher, but not statistically significant higher, rate of dyspepsia than men (p = 0.20).
In this population, the observed total occurrence rate of IBS was 1.0 per 1000 person-years. IBS increased with advancing age. Approximately 40% of all the IBS cases occurred among those over the age of 65 years. Women had a higher occurrence rate of IBS with OR = 2.04 (CI 1.39-3.00; p = 0.0002).
Discussion
This study resulted in a database for the rural Cretan setting where a computerized medical system is still in progress. All consultations during the 4 year period, hard copy or computerized, were registered in the database. Available sources of information were searched, including health cards and handwritten records that were still in use in most health centres.
Several methodological flaws obstructed a correct estimate of occurrence rates of FD, IBS and gastroenteritis. The diagnoses of these GI diseases were made retrospectively on the basis of clinical records obtained by physicians. There was a great variation in diagnoses used by the local physicians and scant information on the patients' symptoms and type of treatment. Although this variety of diagnoses and scant information available in medical records could be explained by the high number of non-specialized young physicians, they have grossly limited the outcome of the study and raised some doubts about the validity of the data source. We can also speculate that the lack of use of specific diagnostic criteria by the local physicians could explain the variety of labels used for functional gastrointestinal disorders, although such a statement is not validated by the findings of this study. However, this is not unique for Cretan physicians. In a questionnaire study from the UK it was found that only 12% of GPs had heard of the Rome Criteria II for diagnosis of functional gastrointestinal disorders and only 3% used them8. Despite the GPs unfamiliarity with diagnostic criteria for IBS, their diagnoses of the condition was in close agreement with that of a specialist9,10. A Norwegian study among GPs also revealed poor use of the Rome Criteria II in the diagnosis of IBS11.
Our study was also based on available medical records; a population-based survey may have provided different figures. The term FD might have been misleading because no endoscopy investigations were performed. For that reason, the patients identified with upper abdominal problems were classified as dyspepsia cases, taking into account that ulcer and gastroesophageal reflux cases could be included. It was uncertain to what extent endoscopy was used in diagnosing of FD and IBS but the impression was that it played a minor role.
Although we made a 4 year retrospective review of all the medical records of the PHC centres in the defined areas, it was difficult to classify the cases as prevalent or incidental. This problem has also been found in other studies throughout the primary care setting12. Therefore, we chose to classify the cases in this report as occurrence rates. The cases documented are regarded as new cases, but some might have had a previous history of the disease.
One of the main findings of this study is the high occurrence of gastroenteritis cases and the relatively low occurrence of dyspepsia and IBS in comparison with other studies. Prevalence studies of functional gastrointestinal disorders in Western societies have shown that between 8%-23% of adults have IBS or other functional gastrointestinal symptoms, and that approximately 60%-70% of these are women4,13. The number of IBS patients in our study was small (5.5%). Some studies have reported that only 25%-60% of individuals suffering from IBS symptoms see a physician for their illness2. Studies of prevalence rates of these diseases in the general population based on postal questionnaires and surveys are available in several countries4,13, while studies of incidence rates are quite rare3,14.
Several factors other than the limitations mentioned may explain the low rates of IBS and dyspepsia found on Crete. It is important to note that in the Greek healthcare system, patients may contact a specialist without a referral from the primary care physician, and severe cases could be lost. In rural areas of Greece, patients who are experiencing only minor symptoms are more likely to consult the local non-specialized physician, who visits their village weekly, instead of travelling to healthcare centres or to distant urban specialized doctors. Therefore, the primary-care physicians working at the healthcare centres can only diagnose IBS when a patient, with unexplained symptoms, becomes poly-symptomatic, has experienced symptoms for a long time or has been referred by the local doctor for further investigation. This could mean that FD and IBS in the Cretan rural environment have a minor symptomatology and are, therefore, not as troublesome for the wellbeing of patients as elsewhere. Other possible explanations for the relatively low rates of dyspepsia and IBS may be found in the socio-cultural environment and the Mediterranean diet. The traditional lifestyle and the concept of stress on rural Crete differ from what is common in Northern and Western Europe today. Also, nutritional factors could be of importance, with the Mediterranean diet favourable. These aspects and their positive impact on GI problems need further investigation in future studies.
In this study, IBS was found to be more common among people aged 65 years and older. This differs from epidemiological studies reporting that the prevalence of IBS declines with age15,16. However, one study suggests that IBS may remain a common GI illness even in the aged17. Our findings require further discussion of and analysis of the prevalence and diagnosis pattern of IBS among the elderly. In the present study the occurrence of IBS was significantly higher among women than men, which is in accord with previous studies3,18.
There is also some evidence in the literature that there is an increased risk of IBS after an episode of infective gastroenteritis19,20. In a study of 386 patients with a bacterial-confirmed gastroenteritis who were surveyed by a questionnaire 6 months after the infective episode, it was found that 7% had developed IBS20. In another study from the UK, it was shown that culture-positive gastroenteritis was an independent risk factor for IBS21. Our study did not contribute to this hypothesis, providing only indirect evidence.
Apart from the contribution of this article to the assessment of the prevalence rate of known GI disorders in rural areas of Crete, the present study has also several implications on quality improvement and its implementation in rural primary care in Crete. The heterogenity of the medical records and the lack of information on diagnostic criteria on common GI disorders call for urgent action. Some measures towards quality improvement have been recently reported22, but improvement must be made in the diagnostic skills of the primary-care physicians who serve the rural areas of Crete.
In conclusion, although the limitations of the study do not permit valid judgements and comparisons to be made, this study carries two key messages. The first is that gastroenteritis is still a frequent health problem that prompts many visits to primary care; and the second is that primary care physicians in rural Crete appear to fail to diagnose adequately FD and IBS, and need further training.
Acknowledgements
The authors express their gratitude for support of the study to the directors and staff at the participating PHC centres on Crete. Specific thanks are extended to Dr N Antonakis, GP at the Anogia Health Centre; Dr M Bathianaki, GP at the Archanes Primary Health Care Unit; Dr M Chatziarsenis, Medical Director at the Neapolis Health Centre-General Hospital; Dr A Batikas, GP at the Perama Health Centre; and Mrs A Romanidou, midwife at the Spili Health Centre, for their contribution to the data collection. This study was supported by a grant from the AstraZeneca R&D, Mölndal, Sweden.
References
1. Luscombe FA. Health-related quality of life and associated psychosocial factors in irritable bowel syndrome, a review. Quality of Life Research 2000; 9: 161-176.
2. Gralnek IM. Health care utilisation and economic issues in irritable bowel syndrome. European Journal of Surgery 1998; 583: S73-S76.
3. Garcia Rodriguez LA, Ruigomez A, Wallander MA, Johansson S, Olbe L. Detection of colorectal tumour and inflammatory bowel disease during follow-up of patients with initial diagnosis of irritable bowel syndrome. Scandinavian Gastroenterologist 2000; 35: 306-311.
4. Thompson WG, Heaton KW, Smyth GT, Smyth C. Irritable bowel syndrome in general practice: prevalence, characteristics, and referral. Gut 2000; 46: 78-82.
5. Hungin APS, Whorwell P, Tack J, Mearin F. The prevalence, patterns and impact of irritable bowel syndrome: an international survey of 40 000 subjects. Aliment Pharmacology and Therapeutics 2003; 17: 643-650.
6. Talley NJ, Stanghellini V, Heading RC, Koch KL, Malagelada JR, Tytgat GN. Functional gastroduodenal disorders. Gut 1999; 45(Suppl II): S37-S42.
7. Thompson GW, Longstreth GF, Drossman DA, Heaton KW, Irvine EJ, Muller-Lissner SA. Functional bowel disorders and functional abdominal pain. Gut 1999; 45(Suppl II): S1143-S1147.
8. Gladman LM, Gorard DA. General practitioner and hospital specialist attitudes to functional gastrointestinal disorders. Alimentary Pharmacology and Therapeutics 2003; 17: 651-654.
9. Yawn B, Lydick E, Locke R, Wollan P, Bertram S, Kurland M. Do published guidelines for evaluation of Irritable Bowel Syndrome reflect practice? BMC Gastroenterology 2001; 1: 11.
10. Thompson WG, Heaton KW, Smyth GT et al. Irritable bowel syndrome: the view from general practice. European Journal of Gastroenterology and Hepatology 1997; 9: 689-692.
11. Vandvik PO, Aabakken L, Farup PG. Diagnosing irritable bowel syndrome: poor agreement between general practitioners and the Rome II criteria. Scandinavian Journal of Gastroenterology 2004; 39: 448-453.
12. Jones R. IBS: Prime problem in primary care. Gut 2000; 46: 7-8.
13. Agreus L, Svardsudd K, Nyrén 0, Tibblin G. Irritable Bowel Syndrome and Dyspepsia in the general population: overlap and lack of stability over time. Gastroenterology 1995; 109: 671-680.
14. Jones R, Lydeard S. Dyspepsia in the community: a follow-up study. British Journal of Clinical Pharmacology 1992; 46: 95-97.
15. Jones R, Lydeard S. Irritable bowel syndrome in the general population. BMJ 1992; 304: 87-90.
16. Talley NJ, Zinsmeister AR, van Dyke C, Melton III LJ. Epidemiology of colonic symptoms and the irritable bowel syndrome. Gastroenterology 1991; 101: 927-934.
17. Bennett G, Talley NJ. Irritable bowel syndrome in the elderly. Best Practice in Research. Clinical Gastroenterology 2002; 1: 63-76.
18. Thompson GW. Gender differences in irritable bowel symptoms. European Journal of Gastroenterology and Hepatology. 1997; 9: 299-302.
19. McKendrick MW, Read NW. Irritable bowel syndrome-post salmonella infection. Journal of Infection 1994; 29: 1-3.
20. Neal KR, Hebden J, Spiller R. Prevalence of gastrointestinal symptoms six months after bacterial gastroenteritis and risk factors for development of the irritable bowel syndrome: postal survey of patients. BMJ 1997; 314: 779-782.
21. Garcia Rodriguez LA, Ruigómez A. Increased risk of irritable bowel syndrome after bacterial gastroenteritis: cohort study. BMJ 1999; 318: 565-566.
22. Lionis C, Tziraki M, Bardis V, Philalithis A. Seeking quality improvement in primary care in Crete, Greece: the first actions. Croatian Medical Journal 2004; 45: 509-603.
Abstract
Introduction: Studies of the frequency and aetiology of functional gastrointestinal disorders in the general population have received increasing interest over the past few years; the field seems to be neglected in Southern Europe. The aim of this study was to report on the frequency of functional dyspepsia (FD), irritable bowel syndrome (IBS) and gastroenteritis within the primary care setting, to provide some information on the extent to which the recorded diagnoses in the physicians' notes fulfil existing diagnostic criteria.
Method: A retrospective study was used, where all new cases of these diseases at five primary health care centres in three rural and two semi-rural areas of Crete were identified by scrutinising medical records from 280 000 consecutive visits during a 4 year period. The occurrence rate per 1000 person-years were calculated for the three conditions. We also checked the extent to which the Talley's criteria for FD and Rome II diagnostic criteria for IBS were followed.
Results: Gastroenteritis was revealed to be a quite frequent health problem among the rural population on Crete, while the occurrence rates for other problems, such as dyspepsia and IBS, were found to be lower than expected. IBS was over-represented among women compared with men, OR 2.04 (CI 1.39-3.00). In many cases a diagnosis of FD, IBS or gastroenteritis was evident to the research team on the basis of findings recorded in the notes, but the diagnosis was not recorded by the clinician at the time of consultation.
Conclusions: This study yielded two key messages: the first that gastroenteritis is still a frequent health problem, and the second that primary care physicians in rural Crete seem to fail in adequately diagnosing FD and IBS and need further training.
Key words: Crete, gastrointestinal disorders, medical records, primary care.
You might also be interested in:
2012 - Determinants of under-five mortality in rural and urban Kenya
2011 - Post-crisis: earthquake, tsunami, radiation leak and rural health crisis in Japan





