Deployment and retention of a sufficient number of skilled and motivated human resources for health (HRH) at the right place and at the right time are critical to ensure people's right to access a universal quality of health care. However, an insufficient number and categories of HRH and their maldistribution have been common problems among countries off track of the Millennium Development Goals. These phenomena are particularly prominent in lower income countries where there is disparity between urban and rural areas in terms of socioeconomic status, including infrastructures1. This impedes the universal health coverage that is critically important to achieve Sustainable Development Goals, especially goal 3 health targets2. A comprehensive approach is necessary from the perspectives of production, recruitment, deployment and retention through regulation, as well as information and financial approaches by intersectoral stakeholders to achieve more equitable distribution of HRH3.
Many countries have attempted to address the disparities in HRH, and there are many academic papers describing what has worked4. There is, however, a dearth of information from Francophone African countries that has been published in English5-7. In 2012, the innovative activities started in nine Francophone African countries as Vision Tokyo 2010 Network8-10, an international network of HRH managers at the Ministry of Health (MoH) level (Box 1). The network identified maldistribution of a limited number of healthcare personnel such as medical doctors, nurses and midwives and their retention in rural areas as overarching problems in the member countries11. This study was planned, conducted and analyzed under the strong leadership of the network. Senegal was chosen as the study area because it is one of the most politically stable countries in the network.
The first objective of this study was to identify the determining factors for the retention of qualified HRH in rural areas by listening to healthcare personnel currently working in rural areas or those who left rural areas to work in urban areas. The second objective was to explore the effective and feasible retention policies for the MoH to implement based on those identified determining factors.
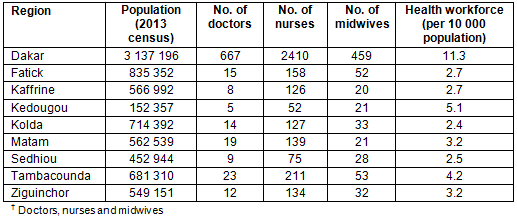
Senegal is located in Sub-Saharan West Africa, which became independent from France in 1960 (Fig1). The demographics of Senegal are shown in Table 1. The official language is French, but Wolof is also widely spoken. Approximately 96.1% of the population practices Islam. Polygamy is known to be more common in rural areas12. There is at least one health center for each health district that supervises health posts. Each health post is located in communes or a rural community and headed by a nurse or midwife. Access to health services in rural areas is a challenge due to long distances via unpaved road from households to health facilities or from health posts to health centers, with limited means of transport13. The concentration of HRH in the capital city of Dakar is striking, with 60% of medical doctors, 41% of nurses and 45% of midwives living in Dakar, while 80% of the population live in places other than Dakar14. Table 2 shows the distribution of healthcare personnel in Dakar and eight rural regions. There was no codified HRH law or policy to address the rural-urban imbalance in Senegal when this study was conducted. The main issues of HRH in Senegal have been the transformation from quantity to quality, the absorption capacity in public health facilities, and maldistribution. The dual practice of civil servants, including healthcare personnel, is prohibited in Senegal. There are 4 private hospitals, 24 private clinics, 414 private medical offices and 700 private pharmacies in the whole country14. Most of them are located in urban areas. Those located in rural areas are mostly run by non-profit organizations.
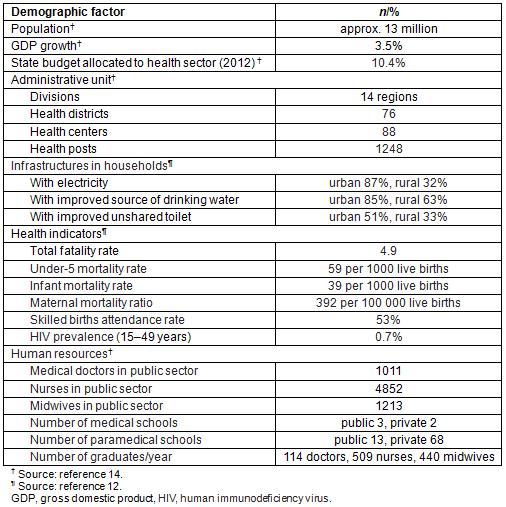
Table 2: Distribution of healthcare workers in Senegal in capital region (Dakar) and eight regions in rural area14
Box 1: The Vision Tokyo 2010 Network

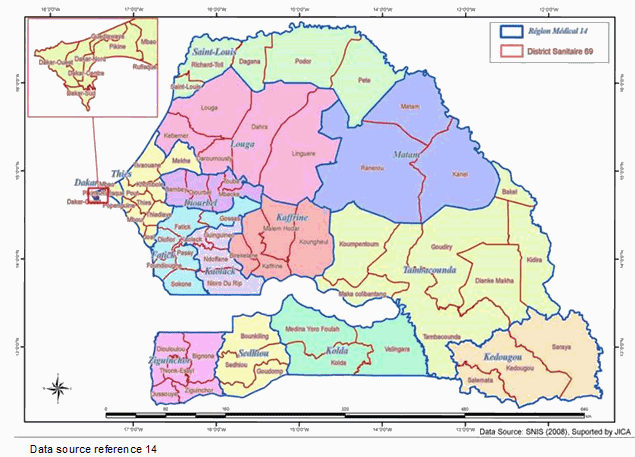
Figure 1: Regions and health districts of Senegal14.
Methods
Sample
The participants in this study constituted three groups of healthcare workers and policy makers in the MoH: (1) those currently working in a rural area for more than two years, (2) those currently working in Dakar with experience of working in a rural area and (3) those currently working in Dakar without any prior experience working in a rural area.
Open-ended questionnaires were administered to the participants in the three groups, asking about their willingness and reasons for accepting to work or continue working in a rural area, and their suggested policies for deployment and retention of healthcare workers in rural areas. Participants included medical doctors, nurses, midwives, and superior technicians in anesthesiology (STA). The MoH attempted to increase the number of these technicians in anesthesiology to expand the availability of surgery at rural hospitals. Among 14 regions, eight contained health districts tentatively identified as a rural area by the Department of Human Resources in the MoH. To select group 1 interviewees, the authors randomly selected healthcare workers from the human resource database in the MoH to be representatives of each category in different types of health facilities from health districts located in rural areas. During the data collection, if a pre-determined health professional was unavailable or had been transferred, a health worker of the same professional type at the same health facility was substituted. Interviewees in group 2 were identified based on the information from the regional health department located in rural health districts. Convenience sampling was applied to selected group 3 interviewees.
For policy makers in the MoH, in-depth interviews were conducted, asking about their definition of a rural area, their perceptions of the management of HRH, and their suggested policies for deployment and retention of healthcare workers in rural areas.
Data collection
The questionnaire and interview guide were developed in French. Four teams, composed of two interviewers and one supervisor, who are all native Senegalese fluent both in French and Wolof, conducted the interviews with the three groups of healthcare workers. Each interview was conducted and recorded in Wolof when the interviewee preferred. The first author and the supervisor conducted the in-depth interviews with policy makers in French.
Interviews were conducted between January and March 2014 in a private room in the health facilities where the interviewee worked. To maintain confidentiality, only the interview team and the interviewee were in the room during the interview. Each interview took 30-90 minutes. All interviews were recorded using both audio and video recorders.
Data analysis
Interviewers transcribed audiotaped interviews to Microsoft Word files. Interviews in Wolof were translated into French. Transcripts were analyzed manually by reading and re-reading them to become familiar with the data. In accordance with the qualitative descriptive method, phrases from the informants' perspectives were coded and reviewed repeatedly. The codes were further analyzed in order to distinguish similarities and differences to form categories reflecting the manifest content of the text. Categories and subcategories were developed until saturation occurred, as determined by the investigators. The regional health director and governor's opinion and documentary reviews5,13-16 were used in the triangulation of interviewees' views.
Ethics approval
The authors obtained ethics approval from the ethics committees of the Ministry of Health and Social Action in Senegal (606 MSAS/DPRS/DR) and the National Center for Global Health and Medicine in Japan (1487). All participants provided written informed consent. Participants were informed of their right to refuse participation in the study and were assured of the confidentiality of the collected information. The respondents did not receive any incentives for participation.
Results
A total of 176 healthcare workers and eight policy makers were interviewed. The demographic characteristics of the healthcare workers are shown in Table 3.
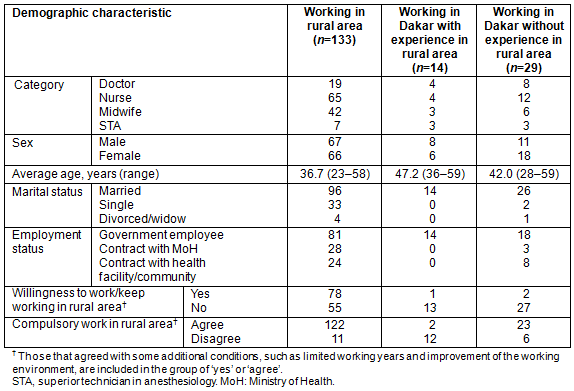
Perception of healthcare workers currently working in rural areas
Three main reasons for accepting the current post were identified:
- willingness to face challenges in a new place
- more medical cases including rare symptoms
- greater responsibility in the health facility
- encouragement by family members
- place of origin.
In large cities, it is medical doctors who make diagnoses and treat patients. Here, I can make the decisions. I am proud of my role. (nurse 1)Encouragement by family members or members of their home town in the rural area also plays a positive role.
Five factors affecting the motivation to keep working in the current post were identified:
- interpersonal relationship in the workplace
- adaptation to the local environment
- distance from family
- career plan
- sense of vocation.
The head of this health facility is a very experienced person. I can learn many things from him. It is good for my future. (nurse 2)Second, motivated healthcare workers found that they assimilated with local languages and culture more successfully.
When I first arrived here, I wanted to leave as soon as possible because I didn't understand the local languages and was not familiar with the food. It was as if I came to a foreign country. But the local people accepted me and helped me to adapt. Now I feel at home. (midwife 1)Third, a female healthcare worker (nurse 3) was one of several who mentioned that living with her husband gives her strong motivation to work and makes her 'feel happy to be here'. She expressed that when her husband is transferred to another area, she will be discouraged and 'want to quit my current post to follow him.'
Fourth, individual career plans also play an important role. Some young healthcare workers wanted to continue their stay to gain clinical experience. On the other hand, those (such as doctor 1) who felt they already had sufficient experience in their current post 'wish another doctor can replace me because I want to continue my study as a specialist, which is impossible here.'
Fifth, a sense of vocation was often mentioned.
I feel confident of my daily responsibilities. During the Tabasuki festival, people invite me to show their appreciation. I can stay here some more years. There are so many things to do to in this poor area. (midwife 2)Suggested deployment policies are classified as:
- production
- Recruit students from rural areas.
- Include rural health in the school curriculum.
- management of health personnel reallocation by MoH
- Have clear terms of reference and duration of assignment.
- family bonding
- Consider spouse's workplace.
- Assign husband and wife to the same place if both of them are healthcare workers.
- information service for cultural differences in rural area prior to deployment.
Most students born in Dakar have never been to a rural area in their life. For them, Senegal is Dakar. At school, they should learn that most Senegalese don't live in Dakar, and that healthcare professionals have a responsibility to serve all Senegalese. (nurse 4)Many healthcare workers mentioned a strong concern regarding the unclear duration of the work at their current post and requested an improvement in human resource management by the MoH.
If I could have known how many years I needed to work here and what kind of career opportunities would be offered afterward, when MoH issued the deployment order, it would have been much easier for me to make a decision to come. (doctor 2)Being close to their family was again a crucial factor influencing their motivation. Any means that avoids separating a healthcare worker and their spouse was considered an important policy.
If a husband and wife are public employees, the government should issue a deployment order that includes both of them. Then they would not refuse it. (doctor 3)Local information was useful for reducing anxiety about being dispatched to an unknown rural area.
When I received the deployment order, I had no idea about the location of this town, its culture, language, food, what I would be able to find at the local market ... I was full of anxiety. You don't want to go to a place you know nothing about, you see. (midwife 3)Midwife 3 recommended publishing a brochure, 'like a tourist guidebook', of each region to reduce the hesitation for departure.
Healthcare workers regard retention policies as 'something effective to increase, or at least maintain my working motivation here'. Their suggestions are classified as:
- fair, transparent, and predictable human resource management by the MoH
- opportunity for continuous education
- working environment with minimum requirements
- family bonding
- incentive schemes
- employment status and promotion
- compulsory work.
When somebody is deployed to a place where he/she does not want to go, reallocation is possible through lobbying of and support from higher-ups if he/she has good connections. I am working in a rural area because I do not have such political connections. This is really unfair. (nurse 5)An equal opportunity to receive continuous education was also mentioned.
The fewer opportunities to learn new things in this place, such as post graduate courses, seminars and national examinations for career advancement, makes me hesitate to stay longer here. (nurse 6)Online training courses were suggested, for example by midwife 4, because 'there is nobody to provide health services in this health facility while I am attending training in the capital city' and 'to maintain a good balance between training and service provisions.'
Acceptable minimum requirements, such as water and electricity, sufficient medical equipment and medicine, were requested, for example by nurse 7, as 'environmental factors that can be improved by MoH' while 'humans cannot change the harsh climate or geographic distance.'
A simplified administrative procedure was recognized as being important to reduce the workload at the health facility.
The administrative paper work really takes up a lot of our time. Very often we need to travel to Dakar to expedite the process. (STA 1)Family bonding was again mentioned, including the accommodations and school for children.
I convinced my wife to come here with me. But when we arrived, we found only a local hut. I could not keep my wife in such a hut for years. I sent her back to the city. Since then I have a double life between here and the city. I am getting tired. (STA 2)Healthcare workers suggested incentive schemes that include both non-financial and financial incentives. Non-financial incentives included priority recruitment of official pilgrimage groups to Mecca or the Vatican, public commendation of services rendered by healthcare workers in rural areas, frequent supportive supervision, and special holidays to spend time with separated family members. Some interviewees suggested making the working experience in rural areas an essential requirement for promotion to the higher management posts or scholarships for postgraduate education.
Financial incentives include hardship allowance and reimbursement for any long-distance commute from the workplace to a regional capital or Dakar for administrative work. The healthcare workers justify a hardship allowance because:
the workload is higher due to lack of human resources, the price of daily necessities in the local market is more expensive because they come all the way from Dakar, and we cannot work privately during off-hours because the population is too poor to pay for a private clinic. (doctor 4)A fair and transparent administration system was seen as a prerequisite for the financial incentive scheme.
Criteria and targets should be carefully defined before implementing the financial incentive scheme. Otherwise it will create further jealousy and confusion in the field. (midwife 5)Healthcare workers also insisted that financial incentives are not a magic bullet and should be considered as a part of comprehensive policy implementations.
I would prefer a better working environment, such as sufficient medical equipment and drugs. Such a good environment would increase my motivation, because I would be able to provide better health service. The financial incentive comes after that. (nurse 8)Some were even concerned about the negative consequence of financial incentives in terms of sustainability.
People always want to get more money once they get some, and the country will not be able to satisfy everyone. Honestly, I think the development partners have also destroyed our system, because people now always request money or per diem. One day the development partners will leave. What will happen in this country then? (STA 3)Priority recruitment of public employees from current contract workers in rural areas was often mentioned as an example of positive discrimination. The recruitment of public employees in Senegal depends on the allocation settled by the Ministry of Public Function and Ministry of Finance, which is not mandated by the MoH. Instead, the MoH can decide who they recruit.
Priority recruitment from workers in rural areas can increase the motivation of healthcare workers. It also informs the public about the seriousness of the MoH to tackle this maldistribution issue. (doctor 5)Similar to the financial incentive scheme, nobody simply agreed with compulsory work in rural areas. Some were concerned:
if a person without personal engagement or who doesn't see the value of working here joins our team, the outcome of our work would not be good. (midwife 6)While many said the best timing for compulsory work in rural areas would be relatively soon after graduation, some, such as midwife 7, expressed a different opinion, saying 'the population in rural areas needs experienced staff, too.'
Perception of healthcare workers currently working in Dakar with experience working in rural areas
Reasons for accepting a post in a rural area were rather passive compared to those currently working in rural areas, who tended to insist on their sense of vocation. The opportunity of being employed by the government played a role. The reasons why they left the rural area also varied: disease or death of family in Dakar, scholarship for their children in Dakar, their own health problems, or other personal issues. All of them returned to Dakar officially, retaining their government employee status. Only one out of 14 interviewees (nurse 9) said he would accept work in a rural area again, 'if I were offered director level.' The reasons for refusing to go back to a rural area are almost the same as the factors affecting the motivation to keep working in rural areas.
When I was alone in the rural area, I lost ambition to improve myself because things were routine. It was not good for myself. In Dakar, I have more opportunity to learn new techniques. (nurse 10)The suggested policies for deployment and retention were quite similar to those suggested by healthcare workers currently working in rural areas. However, this group did not mention anything about having fair, transparent, and predictable human resource management by the MoH.
Perception of healthcare workers in Dakar without experience of working in rural areas
The suggested policies of this group tended to be a wish list.
without a good school for children, my house, infrastructure, good working environment like here in Dakar, I cannot work in a rural area. (midwife 8)Some healthcare workers regarded employment status as more important than the actual workplace.
If I am recruited by the government and am told to go to a rural area, I will accept. (STA 5)Nobody mentioned the issue of human resource management by the MoH.
Perception of policy makers in MoH
Policy makers defined rural areas in a more comprehensive way, basing it:
on several elements in comparison with other areas, for example, the condition of daily life, distance from family, working conditions, financial conditions, and career plan' (policy maker 1).This covers most obstacles suggested by healthcare workers in rural areas. One policy maker admitted there is a gap between original ideas and the present situation of:
regional paramedical schools recruiting students from those rural provinces. We expected them to work in their home provinces after graduation. However, it did not work because we could not deploy enough teachers to serve in those schools. (policy maker 2)The issue of fair, transparent and predictable human resource management in the MoH is well recognized.
People visit me for petition. They ask me to convince government authorities to return their friends or relatives from rural areas to urban areas. (policy maker 3)Policy makers admitted that the management issue negatively affects the motivation of healthcare workers in rural areas.
Healthcare workers in rural areas can be totally forgotten because there is no agreement on the working period in advance. Or, if they work harder and adapt better in a rural area, authorities could decide to keep them there longer because they are doing OK. This situation discourages the healthcare workers a lot. (policy maker 4)Although government employees have an obligation to serve in rural areas, as explained by policy maker 2: 'it is understandable to refuse to stay there because there is neither equity nor justice in the current deployment system.'
The suggested policies for deployment and retention in rural areas by policy makers in the MoH cover all categories listed in the earlier points. To provide better information about cultural differences in rural areas prior to deployment, policy maker 3 proposed to 'develop an orientation module for newly recruited healthcare workers so that they can understand beforehand what to anticipate at their newly assigned post.'
Concrete interventions were suggested to make human resource management transparent, predictable and fair, such as introducing computerized human resource management systems, setting up clear terms of reference and duration of assignment or rotation system, and decentralizing HRH management with budget allocation.
Many healthcare workers go to rural areas because they were simply assigned there, not because they have a firm belief or strong desire to serve the rural population. For them, a transparent deployment order with a clear job description and duration of assignment should be crucial. With those documents, they will be able to make a life plan with less frustration. (policy maker 1)After a certain number of years, said policy maker 5 'that person should be replaced by another healthcare worker instead of being forgotten.'
The human resource management in the Ministry of Education is mentioned as an 'objective competition system' that the MoH can follow.
The school teachers' posts under recruitment are open on the website. The level of the position, its responsibilities, job description, and selection criteria are all there. Anybody interested in a post can apply through the website. School teachers working in rural areas know how many years they need to serve there before they can ask to be transferred. (policy maker 1)Placing more value on the working experience in rural areas in the career track in a systematic way was mentioned as an effective retention tactic because, said policy maker 1, 'a person with an ambitious spirit will not stay in the same position to repeat routine work, when it does not lead to career development.'
Although most authorities were positive about implementing a financial incentive scheme in rural areas, all of them mentioned it should be part of a more comprehensive package including, said policy maker 3, the 'provision of necessary medical equipment and non-financial incentives, such as commendation for a service, giving priority to study abroad, to receive scholarship or continuous education'), as most of the healthcare workers in rural areas mentioned.
Discussion
This study identified factors related to the retention of rural healthcare workers, and explored feasible retention policies in Senegal based on the suggestions of healthcare workers and policy makers. The identified factors to motivate or demotivate healthcare workers to keep working in rural areas were related to pre-service and in-service education, regulatory systems, financial and non-financial incentive schemes, and environmental support. Although some factors were relatively consistent with findings from other studies17-20, several factors specifically insisted upon in this study could be effective policy options for retention of healthcare workers not only in Senegal but also in other African countries or internationally.
First, the value of a permanent contract was highlighted. For the contract healthcare workers, the recruitment for government employment can be an attractive offer even if the workplace is in a rural area. This policy option is not included in the global policy recommendations to improve retention by WHO17. There are three main types of employment for healthcare workers in Senegal: lifetime employment by the government, contract employment with the MoH, and contract employment with a health facility or local community. Only around half of the healthcare workers in the public sector are government employees, with the remainder being short-term contract workers14. The number of healthcare staff to be recruited by the government per year is unpredictable, which is common in Francophone African countries. In the case of Senegal, when there is no government recruitment, or if the allotment for the MoH is insufficient, the MoH directly hires contract healthcare workers using its own budget and allocates them to the health facilities in need. Moreover, a health facility or local community can directly hire contract healthcare staff. The duration of the contract is usually 1 year, with the remuneration and social security system not as good as those for the lifetime government employee because of the budget constraints of the MoH, health facility or the health committee. The findings of the present study show that the countries using a short-term contract employment system like that of Senegal can consider the priority recruitment for lifetime government employees from healthcare workers currently working in rural areas under a short-term contract as a potentially effective retention policy. A study in Lebanon revealed that the possibility of attaining full-time employment status reduced the likelihood of a worker quitting21.
Second, the most prominent values expressed by healthcare workers in rural areas were fairness, transparency, and predictability of human resource management by the MoH. These aspects are again not included in the global policy recommendations by WHO, but should be considered critical cross-cutting issues not only in Senegal but all countries struggling to retain healthcare workers in rural areas. Considering most healthcare workers' motivation to work in rural areas lasts only a limited number of years, setting up a clear duration of the assignment in rural areas and introducing a rotation system could be one policy option to improve the transparency. Many countries already implement a rotation system, but effectiveness seems to vary22-24. Thus, a rotation system with non-adherence to a transparent policy would further demotivate healthcare workers in rural areas 19.
To improve human resource management and keep it transparent, having a regularly updated healthcare personnel database is crucial. It can ease the feeling of inequity among healthcare workers in rural areas, especially to prevent healthcare workers from 'feeling forgotten'25,26. Knowing what type of healthcare workers are currently working where, with which skill, and for how long, the MoH can develop, implement or monitor the appropriate human resource strategy for production, recruitment, deployment, and retention to meet the healthcare needs in the country. However, many countries struggle with accurate and timely data collection, data entry and regular updates. As a part of collaborative work with the Network, the Senegal MoH introduced human resource management software in 2012 after extensive work to modify it based on country context9. This database will be used to monitor and evaluate human resource policies14-16 and strategies and assure their transparency.
Compared with non-financial incentive schemes, financial incentive schemes were less commonly suggested or concerns about their sustainability were expressed. This is unique in this study considering that financial incentives are one of the popular strategies in many countries19,27,28. Almost all interviewees who mentioned financial incentives insisted that they should not be used in isolation, but rather as part of a comprehensive retention policy, with transparency being a prerequisite. This again shows how highly transparency in human resource management is valued by the healthcare workers in rural areas, which could be applicable to other African countries or internationally to ensure the success of any policy implementation that includes financial incentives.
Several specific factors in Senegal were also identified, such as family bonding and religious-related non-financial incentives. Separation from family to work in rural areas has a large, negative impact on the motivation of healthcare workers, despite the fact that being a couple does not necessarily imply living together in the same place. The Senegalese traditional family model incorporates economic strategies to scatter their members in order to diversify sources of income and risk29. Being selected as an official member of a pilgrimage to Mecca can be a great motivation. The 'spirit of Islam' is well integrated into the public life of the Senegalese, while maintaining a good relationship with the Christians30. The government of Senegal organizes an inter-Ministerial official pilgrimage to Mecca every year. Government employees who are selected for this pilgrimage can visit Mecca officially for several months, which is a very important life event for devout Muslims. This non-financial incentive can be effective in other countries where religions play an important role in the healthcare workers' lives.
This study provides the first concrete step toward the implementation of feasible retention policies among the Senegal healthcare workforce. The identified factors and suggested policies seem to be crucial. However, it is impossible for the MoH to implement all suggested policies at once. Their prioritization, including feasibility, acceptability and financial constraints, should be explored. Thus the Department of Human Resources in the Senegal MoH, and the network plan to conduct a quantitative survey to evaluate if the results of this qualitative survey could be generalized, and to identify prioritization (i.e which suggested policy in the qualitative survey might be most effective) and which combination of policies might be most effective. It is anticipated that the real world data obtained in these studies under the strong engagement of Senegal MoH and the network can help inform healthcare workforce policy to improve the retention of qualified healthcare workers in rural Senegal as well as other Francophone African countries through the network.
Conclusions
Determining factors for the retention of qualified HRH in rural Senegal were identified, and are applicable to other countries in Africa and globally. Transparency in human resource management is recognized as an indispensable requirement to ensure the success of any policy implementation. A permanent contract can be an effective and feasible policy option. Family bonding and religious-related non-financial incentives are specific factors in Senegal. The research team, MoH and the network plan to conduct a quantitative survey to confirm the generalizability of these qualitative survey results and identify the most effective combination of policies.
References
You might also be interested in:
2010 - Health worker effectiveness and retention in rural Cambodia



