A world view of rural health care
Ensuring equity and cost-effectiveness in rural health services is a challenge in all countries. It is less easy to achieve economies of scale, there are usually greater difficulties in attracting staff, transport costs are higher, and communities tend to be less wealthy and have poorer health. Problems of these types have been reported in recent literature from the USA1,2, Canada3-5, New Zealand6, Australia7 and the United Kingdom8.
There may be additional challenges for many poorer countries. For example, many of them were pressed by international agencies to adopt various forms of privatization9 in spite of the evidence that this would lead to increased inequity for the rural poor10. Related trends that may harm the rural poor include increased user fees9,11,12, decentralization of health sector management13 and multiple health insurance schemes14.
Some of the transition economies have experienced an increased gap in the health status of rural relative to urban populations since 1990 as a consequence of a decline in the number and quality of rural health workers, rural clinics and hospitals15-18. They had formerly benefited from social policies that promoted equity.
Proposed solutions to the problems of transition economies are much the same as in developed countries. Emphasis has been given to the need to find additional finance through hypothecated payroll taxes, voluntary insurance, and increased self-pay19. The roles of purchasing agencies are seen to be important. Aspects requiring attention include methods of rationing20, the specification of a 'basic' or 'essential' package of health services21, and improved coordination between purchasing agencies22.
Changes in methods of payment of care providers are frequently mentioned. Some authors encourage a mix of per case payments for larger hospitals using casemix classifications, and global budgets for smaller district hospitals23. Others propose various forms of needs-based funding or capitation.
Improved management is frequently mentioned. Common themes include better business planning23, closer linking of clinical and non-clinical decisions24, mathematical modeling of options25, better methods of implementation of change26, and more management training27.
Various ideas are raised regarding the methods of care provision. The reduction of hospital services and a corresponding increase in ambulatory services are commonly mentioned24,25, as are improvements in referral processes including gatekeeping28. A few authors argue for more and better management information29,19. The evidence of the effects of these kinds of interventions is sparse and of questionable validity due to the lack of experimental designs.
An overview of the Mongolian health sector
Mongolia is a large country (5 million km2; Fig 1) with a small population (2.6 million). Sixty-five percent of the population lives in urban areas, and rural population densities are extremely low.
Figure 1: Map of Mongolia.
Mongolia has always been a poor country, and the situation deteriorated after 1990 when it lost the support of the Soviet Bloc. By 1993, a slow improvement began with support from rich countries and international organizations. Its per capita gross domestic product was US$1900 in 2001.
The health status of Mongolians has been higher than might be expected from its low level of wealth. The successes are mostly attributable to the establishment of a comprehensive network of government-financed and operated basic services during the communist era30.
This network was put at risk both by the financial crisis after 1990, and the policy advice provided by some international donors. Some advice was sensible: services were usually inefficient under the Soviet-style economy, too many people were guaranteed jobs, consumers' views were ignored, and there were few rewards for innovation. However, the advice made little sense in the health sector, and the government ignored most of it. For example, it chose to retain control over health financing, but compromised this by creating a government-owned health insurance scheme that draws about half its revenue from compulsory employment-based contributions. Most of the Fund's remaining revenue consists of contributions paid by the government on behalf of disadvantaged groups31. The government also makes direct contributions to the operating costs of its health-care facilities through what are termed 'government budgets'.
The government continues to own and operate the large majority of public health, primary care, and hospital services. There is one major exception: in 1999, the previously salaried family doctors were privatized32. They were assisted in establishing themselves in family group practices (FGP) that must compete for members. Each enrolled member leads to payment of a risk-adjusted capitation fee from the government.
Most primary care services are provided free of charge. The most important exception concerns medications, where there are significant co-payments.
Hospital inpatient services are heavily subsidized through the Fund (which is intended to reimburse variable costs) and government budgets (for fixed costs). However, there are small co-payments for most patients. Hospital outpatient services are largely provided on a user-pay basis. However, insurance benefits were extended to a few outpatient services in 2003.
Experiences with various forms of privatization have been mixed. The FGP have been successful in terms of increasing equity of access and quality of care33. However, private hospital services appear to have delivered only marginal improvements in quality of care at significantly higher cost.
Rural health services
Rural health services are provided in three main ways. First, there are district health centers (DHC). These typically have two or three doctors, four or five nurses, and 10 to 20 beds, and provide ambulatory and simple inpatient care for a population of approximately 5000 to 15 000 people. Second, there are services provided by health workers called 'feldshers', who are considered to be part of the DHC but spend most of their working time visiting rural communities. Feldshers have basic training in maternal and child health and simple treatments. Third, there are various traditional health workers who provide a mix of simple treatments.
Patients needing more sophisticated care can be referred to provincial or national specialized hospitals. They may also seek primary medical care from FGP, but these are available only in the major urban areas.
There has been increasing concern for the performance of the DHCs in recent years. Many buildings and much equipment are in a poor state of repair, basic services such as electricity and running water are deficient, and consumables are often not available. Some staff lack training, and the skill mix is seldom optimal. The quality of care is largely unknown, but small-scale studies suggest it is often inadequate.
The deficiencies are partly a consequence of underfunding. In 2001, for example, 32% of patient contacts with health-care services were with DHC, and yet they accounted for only 21% of expenditures.
DHC obtain revenue from two main sources. In 2002, the DHC received about 40% of their revenue from the Fund and 60% from government budgets. Payments by the Fund are on a per case basis and restricted to inpatient services. Government budgets are based on the number of staff and inpatient beds, and are transmitted through local authorities, which have the right to divert a significant proportion of funds intended for health care to other sectors.
The available funding seems to be unfairly distributed among the DHC. We found large differences in per capita funding across the DHC that could not be explained by such factors as population density, population distribution, age and sex distributions, and family incomes.
There are obvious weaknesses. For example, the two main purchasers of services provide conflicting financial incentives. The Fund encourages DHC to admit patients but not to provide health promotion and other types of primary care. The government budget is conditional on DHC undertaking health promotion and illness prevention, but it encourages DHC to recruit staff and open and use beds. Other problems include unnecessary administrative complexity, encouragement of conflict regarding payment responsibilities and associated efforts to cost-shift, and difficulties in making changes that might improve performance (because the two main funders have competing views).
Government policies on rural health services
In 2002, the government announced a DHC development program with three main strategies: (i) further training of feldshers; (ii) renovation of assets; and (iii) improvement of payment methods that would '... largely be based on capitation'.
A model was developed in 2003 that would have affected only the government budget. Per case payments for inpatient care would continue to be made by the Health Insurance Fund.
In outline, a 'package of essential health services' was defined that comprised five categories of public health services and six categories of personal health services. The idea was to allocated funds on the basis of the number of people who would require such services, and the costs per year, per person.
This model was judged to have some weaknesses. For example, it requires data that would be difficult to obtain. It does not take account of the differences in costs associated with distance, age, and poverty. It focuses on services rather than people and, therefore, creates risks of segmenting care along program lines. Finally, there was the problem, common in all countries, of defining the essential services themselves. One difficulty is that a service that is essential to some people in some circumstances is less so for others, and vice versa. Another is that a binary split into 'essential' and 'non-essential' is a simplification that carries practical risks.
In the event, it was decided that much of the responsibility for rationing should be devolved to the service providers themselves - albeit with guidance and periodic audit from outside. The focus should be on creating the incentives and opportunities for DHC staff so that they are continually involved in improving equity and cost-effectiveness, and on ensuring they are more accountable than before for the provision of integrated primary health care.
The aims of the study
In early 2004, the Government of Mongolia directed the concerned ministries (health, finance, and social welfare) to renew their efforts to develop a satisfactory method of funding of rural health services. It should satisfy the requirements as specified in the policy statement of 2002, and overcome the weaknesses of the model proposed in 2003. In particular, it should be directed at the allocation of funding from all sources, it should use data that were easily compiled, and should make each district health authority responsible and accountable for determining the service mix.
The remainder of this article describes how the model was developed, explains its main features, and notes some implications for the funding of rural health services in other countries.
Design of the new method of payment
The model was developed over a period of 2 months in mid-2004. Four main sources of information were used. First, we examined experiences in Mongolia and in other countries with regard to payment methods that might be relevant to DHC. Second, we held informal consultations with interested parties including government officials at the central and district levels, DHC clinical and managerial staff, and managers of the Health Insurance Fund. We involved them from the start, on the grounds that their ideas and commitment were judged to be crucial to success. Third, we analyzed the relatively large quantities of routine statistics that are available for DHC. Finally, we conducted surveys of the opinions of health-care workers as well as insurance and other government officials. Their answers were used not only to assist the process of model design, but also in parameterization of the model.
These processes led to an early decision that payments should be distributed primarily on the basis of estimated needs for care - in other words, by use of risk-adjusted capitation. There were four main reasons. First, it was government policy. Second, the use of risk-adjusted capitation for family doctor services had proven to be relatively successful. Third, output-based payments from the health insurance scheme had proved to be unfair for several reasons, including poor data for use in categorization. Fourth, largely expenditure-based payments have served to prolong demonstrable inequities.
However, it was widely agreed that three other factors should be taken into account. First, the DHCs differ considerably in terms of the populations and areas that they serve, and one important consequence is that travel costs (both for health workers and patients) are highly variable.
Second, there was concern about the variations in capital assets between the DHC, which were at least partly a result of historical factors that were no longer relevant. If this factor was not taken into account, any DHC with capital assets that were too large or otherwise unsuited to the current and future needs for care would have to bear an unfair burden of costs of maintenance or significant reconstruction.
Third, there were concerns about the lack of incentives and rewards for improvement in quality of care. In the case of family doctors, these concerns had been addressed in part by allowing them to compete for customers. This approach was clearly infeasible for the most part for the DHC, because distances usually precluded the possibility of seeking alternative service providers.
Component 1: the capitation payment
We developed the capitation model in three main stages (i) definition of needs categories; (ii) estimation of service requirements; and (iii) determination of relative costs.
Deciding the categories of clients
All capitation models need to categorize clients into groups with similar needs for health care. We defined the categories by statistical analysis of judgments of approximately 200 health professionals, most of whom were directly involved in the provision of DHC services.
Each respondent was asked to complete a questionnaire that listed 'typical cases' described in terms of candidate predictor variables such as age, gender, family income, location of residence, health status, and health services utilization. The respondent merely provided an estimate of overall service need for each typical case using a Likert scale.
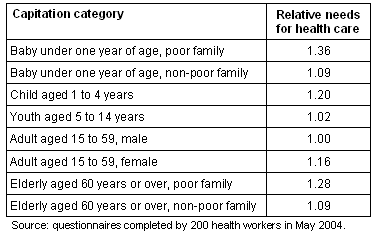
The resultant data were analyzed using regression tree analysis. This involves searching for effective ways of classifying objects (client categories in this case) according to their attributes (predictor variables such as age, gender, and family income) so they explain a variable of interest (the dependent variable, which was expected needs for care in this case). The most efficient classification was that shown (Table 1). For example, the health workers participating in the survey believed that the most care is needed for category 1 (children under one year from poor families) and the least care is needed for category 5 (males aged between 15 and 59 years). There was a reasonable degree of agreement among the respondents, and the relativities are similar to those in the FGP capitation model.
Table 1: relative needs for care of various subpopulations
Estimating service requirements
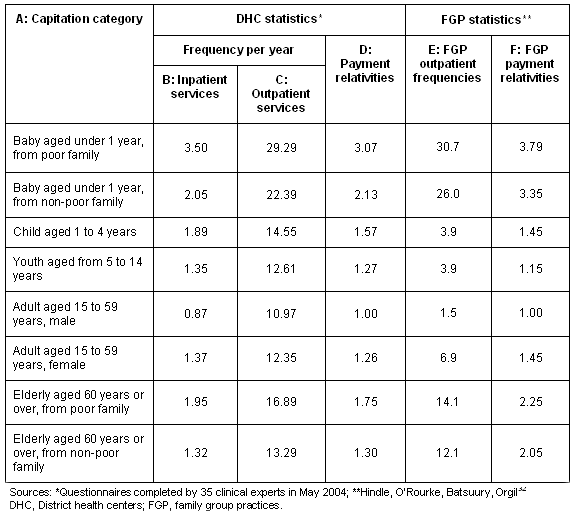
We used a second judgmental process, whereby we presented the descriptions of each capitation class and asked a mix of knowledgeable people to judge how many outpatient and inpatient episodes they needed on average in order to provide good care. The respondents included service providers (doctors, nurses, and administrators), and various concerned staff from government health administration offices and the National Health Insurance Fund. Good care was defined to be '... that mix of services which the average member of each capitation class should receive in one year if prevailing care guidelines were to be fully applied'. The results are summarized (columns B and C, Table 2).
Estimating the annual cost of each capitation class
In the final step, we made estimates of the actual average cost of an outpatient episode and an inpatient episode from routine accounting statistics. The resultant ratio (5.1 outpatient episodes to one inpatient episode) was applied to produce a combined measure of cost (and consequently payment) relativities shown (column D, Table 2). The relativities can easily be translated into payment amounts once the total available budget is known.
Table 2 also shows the recommended frequencies of client contacts for FGP that were developed in 1999, and the resultant payment relativities. The context is different, but it is encouraging to see that there is a reasonable degree of agreement with those that emerged from this study. Further research is needed in order to understand the differences.
Table 2: estimated number of contacts per year by capitation category
Component 2: reimbursement of some fixed costs of operation
Some of the costs of DHCs are fixed - that is, they vary hardly at all in the short term according to the numbers and types of people living in the service area. The boundary between fixed and volume-dependent costs is not precise but the distinction is often relevant. Indeed, this idea is used in the existing payment method, but it is not working well for reasons noted above.
We obtained statistics on the expenditures of DHC by line item. We estimated the percentages of each line item that were fixed and volume-dependent, and combined these to produce an overall estimate of 30% fixed. This became the relevant value in the payment model.
Component 3: special payments for distance and remoteness
Some districts have clients distributed over large areas, and this increases the costs for both the clients and for the DHC. We decided that 5% of the payments should be distributed to take account of this factor, largely on the basis of estimated actual costs.
Our initial intention was to make estimates of traveling distance and time, based either on actual travel in a previous period or on desirable travel (in accordance with the recommended number of contacts for each capitation category). Then distance and time could be translated into travel costs. Two main types of travel should be defined - within the district (to and from clients' homes and the DHC) and between the district and higher levels of care. Account should also be taken of distance costs associated with the acquisition of supplies and facility services.
However, we did not have the data that are required for this approach. We therefore developed a simple estimation model that used population size and area of the district to compute a distance-weighted population (populationi * areai/mean area across all districts), and used this to allocate the available budget for distance.
This approach has several technical weaknesses. For example, no account is taken of the degree of dispersion of the population. It might therefore be argued that implementation of a distance component should await further research and data collection. However, to do so would simply prolong the assumed inequities.
We therefore recommended this component be introduced from the outset. It would not only represent a step towards greater equity, but also provide the stimulus for collecting the data required by a more sophisticated model that could be introduced later.
Component 4: performance-based payments
The fourth component was intended to provide incentives for improvements in quality of care. The idea was that performance standards would be selected according to several criteria including the potential for improvement in cost-effectiveness, evidence of success of the standard, auditability, ease of implementation of changes on the part of DHC staff, consistency with government policies, and the extent to which the changes would be self-financing.
The last point is important in the short term because it is difficult to encourage improvements in clinical practice if an initial investment is required. An example of a self-financing standard concerns more careful prescribing of antibiotics, which are over-used at present.
At the time of writing, the startup standards have not been finalized. This is because we have been waiting for outcomes of a project that is developing various guidelines. Leading candidates include appropriate referral to a provincial hospital, prescribing of antibiotics for upper respiratory tract infections, provision of quit smoking advice, starting of prenatal care early in pregnancy, and coverage of childhood immunizations.
It will be necessary to audit the degree to which the selected targets are met. We propose there be only self-auditing in the first year of use of the new payment contract, to encourage openness, ownership, and commitment. However, a low level of external auditing may be needed in future.
We decided that 5% of the payments should apply to this fourth component. This reflected a group judgment that the amount should be sufficient to capture the interest of all or most service providers.
Implementation
The Ministry of Health has decided to implement the model as soon as possible. Many details remain to be addressed but they will be handled on an ongoing basis.
As preparation for its introduction, workshops were conducted in late 2004 that raised many issues. After further analysis, it was decided that the share of payments for fixed assets should be reduced from 30% to 20%. The distance-related payments were increased from 5% to 10%, mainly on the grounds that the original model had not taken account of the costs of transportation of patients referred to provincial hospitals. The capitation payments component was increased from 60% to 65%. The performance-based payment amount remained at 5%.
Discussion
The new model was based on poor data for the most part, and refinements will be needed after further research and practical experience. Perhaps the most important issue concerns clinical practice improvement. At present, the relative costs of the capitation classes are based on subjective judgments about service needs that are influenced by current practice. A better approach would involve defining clinical practice guidelines for the capitation classes, and then undertaking standard costing according to the numbers and types of activities that should occur in each type of year-of-care. The dominant aim is to improve clinical practice, rather than merely to make fair payments for current practice.
Many other matters need to be addressed that are not central to the payment formula itself but have important associations. For example, attention needs to be paid to the balance between providing greater freedom for DHC staff to innovate, and ensuring their increased accountability to interested parties, and especially to the communities they serve. Referral rules need to be reviewed because the new payment model will affect care providers' incentives. The rules that control self-referrals also need to be reviewed.
Considerable attention had to be paid to the problem of having two often-competing purchasers. One option would have involved excluding DHC services from cover by the Fund. All DHC services would then be covered by the government budget. This would largely resolve the problems of conflicting financial incentives and administrative complexity. However, it would create new problems. For example, the Fund and other agencies would now have an incentive to argue about the definition of 'essential services'.
The option that was finally chosen involves transferring the funds from all sources to the provincial government, and requiring it to make a single annual contract with each DHC. As noted earlier, there was some reluctance on the part of the two.
A more significant problem was that of obtaining agreement between the two main funding agencies to pool their funds within a single contract for each care provider. In part, this reflected a genuine concern about the legality of so doing. There might also have been a reluctance to cede a degree of control to any other agency.
Fortunately, there was high-level commitment to implementation, in part because of the determination of the government (and especially of the Ministry of Finance and Economics) to implement output-based budgeting across all government sectors. The new model provided a convenient way of applying output-based budgeting to one major component of the health sector.
In spite of its many limitations, the new model has the great strength of validity. Even in its current form, it represents a significant improvement on current methods - which are only marginally valid and are of largely unknown but probably inadequate accuracy. One of the advantages of valid methods is that continual improvements are easier to make.
We believe it will lead to greater equity of funding across all districts, and consequently to greater equity for rural Mongolians. It will also encourage and reward improvements in efficiency and quality of care. For example, there will no longer be separate payments for each inpatient episode. This will provide health workers with more freedom to choose the setting and method of care, such as giving greater emphasis to outpatient services and health promotion.
The new model will also allow everyone to better understand whether DHC are operating efficiently and delivering high quality care. If DHC can show they are making good use of the current level of resources, it will be easier to obtain government support for increased budgets in the future.
We believe that this kind of model, and the approach used in its design, are relevant to rural health in most countries, to varying degrees. There has been a tendency to assume that rural health services, because they are less sophisticated in some respects, do not merit the same degree of technical rigor in their design. This is a mistake, if only because the challenges of measurement and the needs for cost-effectiveness are much the same regardless of geography. In consequence, we believe that the Mongolian model may be of interest in most countries, in that it avoids the common error of over-simplification. It is still common for rural health services to be funded by use of a model that (say) uses capitation without an appropriate degree of risk adjustment or to make output-based payments that ignore the possibility of under-servicing due to difficulties of access.
Finally, many countries could do more to involve rural health professionals in model-building. This might be said of all types of payment system design tasks, but it is particularly relevant to rural health service providers because they are typically less influential in health policy formulation than (say) clinical professors in tertiary hospitals.
References
1. Reschovsky JD, Staiti AB. Physician incomes in rural and urban America. Issue Brief Cent Studies in Health System Change 2005; 92: 1-4.
2. Ricketts TC. Workforce issues in rural areas: a focus on policy equity. American Journal of Public Health 2005; 95: 42-48.
3. Touati N, Contandriopoulos AP, Denis JL, Rodriguez C, Sicotte C. Care access in rural areas: what leverage mechanisms do regulatory agencies have in a public system? Health Care Management Review 2004; 29: 249-257.
4. Forbes DA, Janzen BL. Comparison of rural and urban users and non-users of home care in Canada. Canadian Journal of Rural Medicine 2004; 9: 227-235.
5. Sempowski IP. Effectiveness of financial incentives in exchange for rural and underserviced area return-of-service commitments: systematic review of the literature. Canadian Journal of Rural Medicine 2004; 9: 82-88.
6. Brabyn L, Barnett R. Population need and geographical access to general practitioners in rural New Zealand. New Zealand Medical Journal 2004; 117(1199): U996.
7. Gleeson M. Let's have more equity and justice in rural health services provision. Australian Health Review 2004; 28: 115-116.
8. Kmietowicz Z. Health of people in rural parts of Britain is being neglected. BMJ 2005; 330(7485): 216.
9. Benson JS. The impact of privatization on access in Tanzania. Social Science and Medicine 2001; 52: 1903-1915.
10. Bogg L, Dong H, Wang K, Cai W, Vinod D. The cost of coverage: rural health insurance in China. Health Policy and Planning 1996; 11: 238-252.
11. Khe ND, Toan NV, Xuan LT, Eriksson B, Hojer B, Diwan VK. Primary health concept revisited: where do people seek health care in a rural area of Vietnam? Health Policy 2002; 61: 95-109.
12. Thomason J, Mulou N, Bass C. User charges for rural health services in Papua New Guinea. Social Science and Medicine 1994; 39: 1105-1115.
13. Tang S, Bloom G. Decentralizing rural health services: a case study in China. International Journal of Health Planning and Management 2000; 15: 189-200.
14. Yip WC, Wang H, Liu Y. Determinants of patient choice of medical provider: a case study in rural China. Health Policy and Planning 1998; 13: 311-322.
15. Ensor T, Rittmann J. Reforming health care in the Republic of Kazakstan. International Journal of Health Planning Management 1997; 12: 219-234.
16. Sari N, Langenbrunner JC. Consumer out-of-pocket spending for pharmaceuticals in Kazakhstan: implications for sectoral reform. Health Policy Planning 2001; 16: 428-434.
17. Segall M, Tipping G, Lucas H et al. Economic transition should come with a health warning: the case of Vietnam. Journal of Epidemiology and Community Health 2002; 56: 497-505.
18. Habicht J, Kunst AE. Social inequalities in health care services utilisation after eight years of health care reforms: a cross-sectional study of Estonia, 1999. Social Science and Medicine 2005; 60: 777-787.
19. Falkingham J. Poverty, out-of-pocket payments and access to health care: evidence from Tajikistan. Social Science and Medicine 2004; 58: 247-258.
20. Krizova E, Simek J. Rationing of expensive medical care in a transition country - nihil novum? Journal of Medical Ethics 2002; 28: 308-312.
21. Hrabac B, Ljubic B, Bagaric I. Basic package of health entitlements and solidarity in the Federation of Bosnia and Herzegovina. Croatian Medical Journal 2000; 41: 287-293.
22. Ensor T, Rittmann J. Reforming health care in the Republic of Kazakhstan. International Journal of Health Planning and Management 1997; 12: 219-234.
23. Ensor T, Amannyazova B. Use of business planning methods to monitor global health budgets in Turkmenistan. Bulletin of the World Health Organization 2000; 78: 1045-1053.
24. Ensor T, Thompson R. Rationalizing rural hospital services in Kazakhstan. International Journal of Health Planning and Management 1999; 14: 155-167.
25. Street A, Haycock J. The economic consequences of reorganizing hospital services in Bishkek, Kyrgyzstan. Health Economics 1999; 8: 53-64.
26. McKee M, Figueras J, Chenet L. Health sector reform in the former Soviet Republics of Central Asia. International Journal of Health Planning and Management 1998; 13: 131-147.
27. Sharmanov T, McAlister A, Sharmanov A. Health care in Kazakhstan. World Health Forum 1996; 17: 197-199.
28. Balabanova D, McKee M, Pomerleau J, Rose R, Haerpfer C. Health service utilization in the former soviet union: evidence from eight countries. Health Services Research 2004; 39: 1927-1950.
29. Veenema TG. Health systems and maternal and child survival in Central Asian Republics. Journal of Nursing Scholarship 2000; 32: 301-306.
30. Manaseki S. Mongolia: a health system in transition. BMJ 1993; 307(6919): 1609-1611.
31. Hindle D, Van Langendonck J, Tsolmongerel T. Mongolian experiences with health insurance: are success factors unique? Australian Health Review 2002; 25: 26-37.
32. Hindle D, O'Rourke M, Batsuury R, Orgil B. Privatising general practice in Mongolia: a trial of needs-adjusted capitation. Australian Health Review 1999; 22: 27-43.
33. Orgil B, Hindle D, Sonin S, Dashzeveg G, Batsuury R. Privatised family group practices in Mongolia: an initial assessment of service access. Australian Health Review 2002; 25: 19-30.
Abstract
This article describes experiences in Mongolia in designing and implementing a new method of payment for rural health services. The new method involves using a formula that allocates 65% of available funding on the basis of risk-adjusted capitation, 20% on the basis of asset costs, 10% on the basis of variations in distance-related costs, and 5% on the basis of satisfactory attainment of quality of care targets. Rural populations have inferior health services in most countries, whether rich or poor. Their situation has deteriorated in most transition economies, including Mongolia since 1990. One factor has been the use of inappropriate methods of payment of care providers. Changes in payment methods have therefore been made in most transition economies with mixed success. One factor has been a tendency to over-simplify, for example, to introduce capitation without risk adjustment or to make per case payments that ignored casemix. In 2002, the Mongolian government decided that its crude funding formula for rural health services should be replaced. It had two main components. The first was payment of an annual grant by the local government from its general revenue on the basis of estimated service population, number of inpatient beds, and number of clinical staff. The second was an output-based payment per inpatient day from the National Health Insurance Fund. The model was administratively complicated, and widely believed to be unfair. The two funding agencies were giving conflicting types of financial incentives. Most important, the funding methods gave few incentives or rewards for service improvement. In some respects, the incentives were perverse (such as the encouragement of hospital admission by the National Health Insurance Fund). A new funding model was developed through statistical analysis of data from routine service reports and opinions questionnaires. As noted above, there are components relating to per capita needs for care, capital assets, distance, and quality of care. The risk-adjusted capitation component determines needs classes by use of age, gender, and family income. The model was accepted by all concerned parties, and steps are now being taken to implement it under transitional arrangements. Many of the data used to parameterize the model are inaccurate and will need to be updated in the near future. However, the model is inherently valid, and procedures have been set in place that will ensure accuracy is improved on a continuing basis. An important reason why the government strongly supported implementation was its commitment to implement output-based budgeting across all government sectors. The new model provided a convenient way of applying output-based budgeting to one major component of the health sector.
Key words: funding model, rural health service, Mongolia.
You might also be interested in:
2020 - Tribute to David Heaney

