Introduction
Complementary and alternative medicine (CAM) has achieved an exponential growth over the last two decades in Western industrialised countries1. Studies are now showing a dramatic increase in support for, and usage of, therapeutic practices outside mainstream medicine. This trend is particularly strong among cancer patients who are the most prolific users of CAM2. Similarly, despite increases in access to biomedical treatments in developing countries, research shows that traditional medicine (TM) also continues to receive considerable support3.
Despite anecdotal evidence suggesting continued support for 'non-conventional' (ie, non-biomedical) therapeutic modalities, we know little about patterns of usage of TM and CAM among cancer patients in the developing world. Studies in Western nations show distinct patterns in usage according to patient characteristics (eg age, socioeconomic status and cancer type)4; yet, we know little about potential stratification in access to, and usage of, CAM and TM in developing countries.
Pakistan presented an excellent case study for examining the roles of TM and CAM in cancer care in a pluralistic healthcare setting Pakistan remains a predominantly rural country with 67% living in rural areas and 57% engaged in agriculture5.
The limited research performed on CAM/TM use by cancer patients in Pakistan suggests that, as in the West, CAM/TM use is relatively high6. For example Milak and Qureshi's study6 of cancer patients in Karachi indicated that use of 'unconventional' methods of therapy by cancer patients was 48%. Their study found that the main alternative therapies being used were homeopathy and Hikmat (Hakeems). Malik, Khan & Kahn's study found even more widespread use of 'unconventional' methods of therapy (54.5% of all cancer patients), with traditional herbal medicines and homeopathy the most commonly employed methods (70.2% and 64.4% of the sample, respectively)7.
Our study is the first on cancer treatment in this area of Pakistan (Lahore and surrounding provinces). Although useful, the aforementioned studies were conducted some years ago and there is a need for updated and relevant data that reflects the current socio-cultural context of Pakistan. Furthermore, these studies had very different foci than the current study, tending not to separate CAMs from TMs in their analyses, thereby producing rather oversimplified representations of cancer patients' use of 'unconventional' therapies.
We aim to build on the limited amount of existing work to begin to map out some basic trends in cancer patients usage of CAM/TM, focusing on what practices are being used (ie, CAM/TM), by whom (ie, gender/age/caste), and in what socio-geographic contexts (ie, nature of the hospital/geographic location).
Defining health practices
One problem in discussing 'traditional' and 'complementary' or 'alternative' medicine is that these very categories are contestable and changeable over time and space. There is no set notion of what constitutes a 'complementary' or 'alterative' practice, or what can be considered 'traditional' in a given socio-historical context. In fact, notions of 'alternative' or 'conventional' are highly political and agenda-driven with considerable cultural and historical variation8. However, although definitions of TM and CAM are continually debated and, at times, reconfigured as practices and drawn into the mainstream9, we can usefully and pragmatically employ definitions that delineate CAM and TM from each other and from allopathic medicine.
Defining 'traditional' and 'complementary' medicine
CAM, in this context, generally refers to healthcare practices not offered as biomedical treatments in Western nations9. Many CAM practices have emerged from traditional health practices, but over time, they have been shaped by Western models of care. Examples include Herbalism, Reiki or Naturopathy. Certain CAM have emerged from traditional belief systems, but have moved away from their philosophical roots (eg Chinese acupuncture), resulting in different, but not entirely distinct, healthcare modalities (eg Western forms of acupuncture)8. Other CAM have emerged within Western contexts (ie, homeopathy) but are distinct from allopathy in terms of the paradigmatic basis for their treatments. Encompassing a disparate range of modalities10, what largely characterises CAM is, first, a lack of integration into bio- or allopathic medicine11, and second, their tendency to espouse models of care which incorporate physical and metaphysical elements in treatment processes (however, this is not true of all CAM)9. Such CAM are ubiquitous across Western nations and there is anecdotal evidence that suggests they are beginning to achieve a presence in developing countries like Pakistan. There is, therefore, some merit in identifying them as 'globalised CAM' - in distinction to localised TM. This is also a distinction that is being employed beyond academia, most notably by the World Health Organisation12.
Thus, TM refers to local knowledges, belief systems and therapeutic practices that are used in developing countries for health-related purposes. Whereas CAM have historically operated on the periphery of most Western healthcare systems, traditional medicines have often been the dominant means of treatment for health problems for centuries (eg Hakeems in Pakistan). In some developing countries they continue to dominate healthcare beliefs and practices13. TM is, thus, characterised by longevity, cultural specificity, religiosity14 and having Indigenous roots13, rather than by its position relative to other modalities (as has been the case for CAM). Moreover, paradigmatically, there is not consistency among TM, whereas for CAM, a case could be made for a degree of congruence in the ideological positioning of many complementary and alternative health practices (eg holism or naturalism).
Pakistan: social, economic and medical context
Pakistan is the seventh most populous country in the world with a population of 144 million15. The population is predominantly Muslim (96.7%) with a minority of other faiths including Christians, Hindus, Ahmadis, Zoroastrians, Buddhists and Sikhs. Both Urdu and English are the official languages, however, eight other languages are spoken in different parts with different dialects making Pakistan a multi-lingual society. Largely agricultural, nearly 70% of the population live in rural areas and approximately 57% of its civilian labor force are employed in agricultural occupations. The average per capita income in Pakistan in 1990-1991 was about US$400 with approximately 30% of the population living below the poverty line16. In 1999, life expectancy for men and women was reported to be 64 and 66 years, respectively.
The medical system in Pakistan
Pakistani health services currently receive only approximately 1% of gross national product. The public sector provides 20% of healthcare services and a large proportion of people use the private sector. The private sector includes doctors, pharmacists, paramedical health workers, and traditional practitioners of various systems of medicine. Within this pluralistic health system, patients may receive treatment from a number of diverse, and at times paradigmatically disparate, therapeutic disciplines5. While modern allopathic medicine is frequently used for more serious conditions, people often use CAM or TM in combination with, or instead of, allopathic medicine16.
Traditional medicines in Pakistan
It is important to provide a background to the most common traditional medicines used in Pakistan. The first - the Hakeem - is a practitioner who subscribes to the Hikmat approach to the body and illness. This is a traditional system of medicine practised mainly among Muslim communities in South Asia. It is a reorganised Muslim development of the system of medicine outlined by Hippocrates and Aristotle and involves use of a variety of herbs and minerals. Although there are a number of well-established institutions training people in Pakistan, Hakeems are generally trained through a process of apprenticeship and frequently come from a well-established lineage of healers. Recently the government of Pakistan recognised the importance of treatments given by Hakeems and have recruited them in several Government hospitals, albeit at a lower grade than allopathic doctors5.
Spiritual healing, and the specific practice of Dam Darood, are forms of practice that depend on prayers, prophetic medicine and other local practices5. These types of healing are usually delivered by holy men called Pirs, either personally or through a designee. Patients often visit associated places, such as mosques or tombs (or sometimes in their offices or homes), for the purpose of healing. This routinely involves the Pirs reading verses from Quran and blowing the words towards the patient. This process is called Dam, Dam Darood or Dua (prayer). Multiple repetition of certain Quranic verses for an extended periods of time (weeks or months), called Wazifa, is another popular method of religious healing5.
Method
The analysis presented in this article is based on data collected in a structured survey of cancer patients in four different hospitals in Lahore, Pakistan (to retain anonymity the names of the hospitals will not be used in this article). The survey was carried out between April 2003 and August 2003. Data were analysed in SPSS for Windows 11.0.0 (SPSS Inc., Chicago IL, USA), with associations between CAM/TM use and sex, caste, education, cancer type and hospital explored using c2 analysis. An alpha level of 0.05 was used for all statistical tests.
Sample
Of the hospitals from which patients were recruited, three were general hospitals that treated a range of patients (including those suffering from cancer) from the Punjab and North-west Frontier Province provinces. The fourth hospital was a 25-bed specialist cancer hospital, exclusively treating cancer, and drawing patients from all regions of Pakistan. The decision to draw our sample purely from the four aforementioned hospitals was made due to the centralisation of cancer-related health facilities in Lahore, rather than in rural parts of the Punjab province. Because of this centralisation of health services, the majority of cancer patients in the Punjab province come to Lahore for treatment, providing a fairly representative sample of the whole province, incorporating its rural as well as urban areas.
We had no prior knowledge about the proportion of patients who would be users of CAM/TM within the studied population. Thus, we took p = 0.5 as a conservative estimate for the population proportion of the cancer patients having access to CAM/TM in and around Lahore. Furthermore, it was decided that the sample estimate of this proportion to be accurate to within 0.05 (precision of the estimate) at 95% confidence. The resulting sample size was 385 patients. Working with this figure, it was decided to aim to survey 350 to 400 cancer patients over a 4 month period. Furthermore, it was decided that the respondents/patients would be distributed among the four hospitals according to the bed capacity of their cancer wards. All the hospitals treated patients from different parts of the province/country; however the specialist cancer hospital had the most diverse geographical representation of patients. All 362 patients approached during these times completed the survey. In this cultural context, a high response rate is expected because patients are highly unlikely to refuse a request for information from a researcher or medic.
Fieldwork
The medical and research directors of the hospitals were approached for permission to undertake the study and all subsequently gave permission. Two sociologically trained male and two female researchers undertook the survey, which took place in the oncology departments of each hospital. Generally the male researchers surveyed the male patients and female researchers the female patients but, at times, female researchers surveyed male patients as well. When recruiting began, researchers reported on a daily basis to the hospitals' management to ensure the appropriate authorities were aware of their presence and that the study being conducted. The researchers approached all patients admitted in the hospitals during week days, on different days and at different times of the day (between 10.00 and 16.00 hours) until the predefined number of surveys for a particular hospital was reached. The researchers gained written consent from the patients before the survey was completed. The patients were told that they were being interviewed as part of a survey to seek information about their disease and treatment behaviours. Usually patients had one or two family members/carers with them while the survey was being completed. The interviewers themselves filled in the questionnaires, not the patients.
Results
In the final sample 41.2% (n = 149) were women. The reason for men being overrepresented is unclear. It may be that, as in Western contexts, men are also overrepresented due to their tendency towards high risk behaviour17. Existing statistics on Pakistani cancer patients do suggest a higher representation of men for certain types of cancer15 but give little explanation as to why. In terms of marital status, 24.6% (n = 89) of the sample were single, 69.3% married (n = 251), 0.3% (n = 1) divorced, 5.2% (n = 19) widowed and 0.6% (n = 2) were widowers. Over 73% (n = 264) of the sample earned between 1000 and 6000 rupees per month (between US $17 and $102 per month) which is broadly within the range of the reported national average in 199118. The sample was well distributed in terms of age, socio-economic status and level of education. These statistics illustrate the general low socioeconomic status of Pakistani cancer patients, lack of access to education, and a fairly low numbers of older patients (ie, in line with low life expectancy). This is not inconsistent with demographics in the wider Pakistani population.
Cancer types
There was a wide distribution in terms of the range of cancers, and typically, as we see in Western studies, breast cancer (27.6% n = 100) emerged as the most common form19. Pakistan has the highest rates of breast cancer of any Asian population19. After breast cancer, haematological malignancies (11.6% n = 42), throat cancer (9.7% n = 35), cancer of the uterus (8.3% n = 30), and cancer of the abdomen (5.8% n = 21) were the most common forms in this sample.
Use of traditional medicine and complementary and alternative medicine
Use of TM and CAM was significantly higher in this sample of cancer patients than reported previously. Only 16% of those surveyed reported not using a traditional medicine or CAM/TM. This is compared with usage levels of 48% and 54.5% by Milak and Qureshi6 and Malik, Khan & Kahn7. This means that the large majority (84%) of cancer patients surveyed here had used one or more forms of TM or CAM19.
Table 1: Prevalence of use of complementary and alternative medicine /traditional medicine
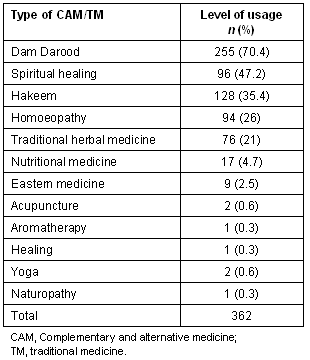
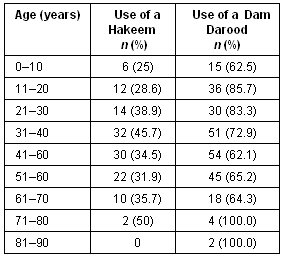
In terms of use of particular TM, Dam Darood emerged as the most commonly used, with 70.4% of the sample using this therapy at some point during their treatment. Age also seemed to mediate use of TM. For example, it is apparent in Table 2 that it had an influence on the use of a Dam Darood and Hikmat, with use highest among cancer patients between the ages of 11 and 30 years, and then reducing in older patients.
Table 2: Relationship between age and use of selected traditional medicines
Combining complementary and alternative medicine/traditional medicines
We were also interested in investigating whether patients were using a single CAM/TM or combining different CAM/TM. This is particularly important in terms of whether patients were drawing on their traditional beliefs systems (ie, consulting a Hakeem) or whether they are actively seeking and combining different CAM/TM. Although the largest group of people only used one CAM/TM (23.8% of the sample), 13.8% used four, 20.4% used three and almost 18.8% used two. The most common combinations were Dam Darood and Hikmat (use of a Hakeem).
Sex and complementary and alternative medicine usage
CAM/TM usage in Western countries has typically been stratified according to sex, with females tending to use CAM/TM more frequently4. Moreover, females with breast cancer have the highest rates of CAM/TM usage among cancer patients. However, results from this Pakistani survey indicate that this may be a culture-specific process, and that sex may mediate use of CAM/TM very differently (or be supplanted by cultural and religious belief systems) in Pakistan. Females reported use of CAM/TM less than males (81.2% of females vs 86.6% of males), however, there was no statistically significant relationship between sex and CAM usage (c2 = 1.36 [df = 1] p = 0.31).
Moreover, although a relatively small difference, approximately 10% more males used Dam Darood (76.5%) than females (66.2%) in the sample. Sex was not a factor in the use of a Hakeem with 35.3% of females using a Hakeem versus 37% of men. However, as with the case with the Dam Darood, there was a small increase (although not statistically significant) in use of a Hakeem among patients between the ages of 11 and 40 years.
Cancer type and complementary and alternative medicine use
As mentioned, studies have indicated that there may be relationships between cancer types and CAM usage20. We were interested in exploring the degree to which use of CAM/TM was linked to particular cancer types. Studies in Western nations have shown distinct patterns in use of CAM and, in particular, higher usage among female breast cancer patients20. However, this study showed no clear stratification in terms of use of CAM/TM by cancer type (c2 = 0.77 [df = 1] p = 0.419) and, importantly, when compared with all other cancers, breast cancer sufferers actually had slightly lower levels of CAM/TM usage (85% for 'all other cancers' versus 79% for 'breast'). Bear in mind that males and females were almost equally represented (males = 57% females = 43%) in the 'other cancers' category (ie, the cancer type differentiation was not merely a result of a gender split).
Education and use of complementary and alternative medicine /traditional medicine
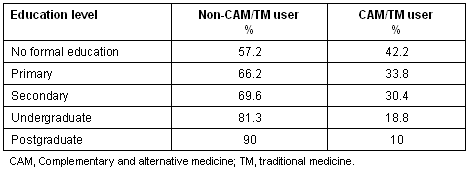
The level of education was also examined in terms of being a potential mediator of CAM/TM usage. However, no clear relationship emerged between general usage of CAM/TM and the level of education. Each education bracket had between 80% and 95% CAM/TM usage (c2 = 2.0 [df = 4] p = 0.736). However, when the usage of individual CAM/TM was examined, there was a distinct relationship between level of education and use of particular CAM/TM. For example, use of a Hakeem was closely related to level of education within this sample. The higher the level of education, the less likely patients were to utilise Hikmat.
Table 3: complementary and alternative medicine/traditional medicine use and level of education

Table 4: Use of a Hakeem and level of education
Differences between hospitals
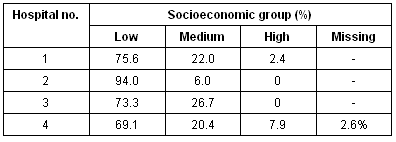
It is also worth noting that there were statistically significant differences in use of CAM/TM among the hospitals used for recruitment (c2 = 15.5 [df = 3] p = 0.01). For example, of the patients surveyed at one hospital, 90.8% (n = 138) had used CAM/TM versus 68.3% at another hospital which had the lowest level of CAM/TM usage (Table 5). This may relate to the fact that those surveyed at the former were on average of a higher socioeconomic status (Table 6) than those patients at the other hospitals, and thus could afford to use a range of treatments. However, this was contradicted by the overall data that showed no relationship between socioeconomic status and use of CAM/TM. Average income for the patients in hospitals 1 and 2 were significantly lower than expected, whereas those in hospitals 3 and 4 were higher.
Table 5: Complementary and alternative medicine /traditional medicine use by hospital
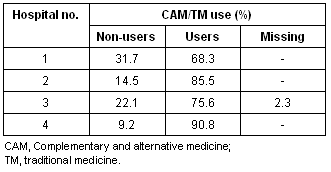
Table 6: Socioeconomic status by hospital
Discussion
This study gives us initial insight into patterns in cancer patients' usage of CAM and TM in Pakistan, providing a basis for a larger nation-wide survey exploring treatment choices.
At a basic level, the frequencies of particular cancer types shown in the results of this survey are broadly consistent with past reports on cancer prevalence in Pakistan15,19; although, data is severely limited by the lack of a cancer registry. Only one patient had prostate cancer, which is an unusually low figure given normal rates of prostatic malignancies in other study populations. This, we can only hypothesise, may be due to inaccurate diagnoses (ie, cancer patients diagnosed according to their metastases - eg in the lung or liver), or the tendency of older men to die of other conditions before being diagnosed with, or developing, prostatic malignancies. The low levels of skin cancer are also interesting, although not unusual among other Asian populations. Given previously reported rates of lung cancer in Pakistan, one would have also expected these to be higher21.
This study was limited for a number of reasons. Firstly, we only surveyed cancer patients who had been admitted to the four major hospitals treating cancer patients in Lahore. Given the likelihood that significant numbers of patients do not have access to allopathic cancer facilities in Pakistan (particularly in remote areas), it is likely that significant numbers of people with cancer could not be accessed in this survey. Moreover, it is also likely that these very patients may have unique patterns of TM usage (ie, they may be higher TM users because they do not have access to allopathic cancer treatments). Furthermore, we know little about how the results may differ in a nation-wide study - that is, how specific they are to Lahore and its surrounding provinces. Cleary there is a need for a larger nation-wide study of treatment decisions by cancer patients. It is important to bear in mind that these data have been presented at a broad level; there are undoubtedly issues of complexity that will be revealed by a second level of study.
Despite these limitations, this study indicates that CAM and TM usage in Pakistan may be significantly higher than reported previously and, furthermore, that patients are combining multiple (and at times paradigmatically disparate) therapeutic modalities.
This study also provides preliminary data on how CAM/TM usage may be mediated by patient characteristics, and how this differentiation may differ from Western contexts. Results showed that although there is some differentiation in CAM and TM usage according to patient characteristics, this differentiation is smaller than in the West, but also, that it is quite different in nature. Specifically, as shown earlier, in stark contrast to studies of Western cancer patients, overall, in this survey, women used CAM/TM slightly less than men. Moreover, there exists little variation in cancer type and consumption of CAM or TM. Although Western studies show considerable differentiation in the case of breast cancer, breast cancer patients in this study on average used CAM/TM less than patients with other types of cancer. These results illustrate the need for studies that are specific to developing countries and, furthermore, more research to examine why patterns may differ within such contexts.
Without further in-depth work we can only hypothesise about the reasons for such patterns of use. Such analyses will, clearly, necessitate a focus on the specific socio-historical context of decision-making. It is not that interesting trends are not emerging, simply that they are of a different form from those seen in the West. So, for instance, whereas use of non-orthodox practices is related to higher levels of education in the West, in this case the only relationship with education was the decrease seen in use of Hakeems. Furthermore, use of a Hakeem was generally lower than for Dam Darood: a practice with an explicitly religious focus. Indeed, it may well be that the intermingling of TM and religion may also be implicated in the high levels of use by men - though again this requires more in-depth work to assess more fully. A detailed look at differentiation within the categories of TM and CAM as well as between them will also be facilitated by our qualitative work on the same topic in the same region22.
We are at the early stages of unpacking changing environments in poorer countries. While it clearly makes little sense to simply apply Western notions of CAM to use by Pakistani patients, it is also important to remember that countries such as Pakistan are not entirely 'separate' either. While still predominantly rural, people in villages are accessing cancer services in cities (albeit frequently at a very late disease stage). And, intersecting with Indigenous medicine are bio-medical orthodoxy and, at least to some extent and at the margins those CAM ubiquitous in the west. Health practice in Pakistan also takes place against a backdrop of global migration, not least to the UK. The current research highlights the need to get beyond monolithic categories such as (acceptance or rejection of) 'traditional medicine' as a whole in order to begin to understand how and why certain Indigenous practices are used to a greater extent than others and how the nature of such practices is being modified over time by the global processes of migration, communication, non-local CAM and, of course, allopathy.
Acknowledgements
The authors acknowledge the Economic and Social Research Council, UK for funding this project (grant number: L218252053).
References
1. Eastwood H. Postmodernisation, consumerism and the shift towards holistic health. Journal of Sociology 2000; 36: 133-155.
2. Cassileth B, Vickers A. High prevalence of complementary and alternative medicine use among cancer patients. Journal of Clinical Oncology 2005; 23: 2590-2592.
3. Wayland C. The failure of pharmaceuticals and the power of plants: medicinal discourse as a critique of modernity in the Amazon. Social Science and Medicine 2004; 58: 2409-2419.
4. Thomas K Nicholl J, Coleman P. Use and expenditure on complementary medicine in England. Complementary Therapies in Medicine 2001; 9: 2-11.
5. Tovey P, Chatwin J, Ahmad S. Towards an understanding of decision making on complementary and alternative medicine (CAM) use in poorer countries: the case of cancer care in Pakistan. Integrative Cancer Therapies 2005; 4: 236-242.
6. Malik I, Qureshi A. Communication with cancer patients, experience in Pakistan. In: A Surbone, M Zwitter (Eds). Communication with the cancer patient, information and the truth. The New York Academy of Sciences: New York,1997; 300-308.
7. Malik I, Khan N, Kahn W. Use of unconventional methods of therapy by cancer patients in Pakistan. European Journal of Epidemiology 2000; 16: 155-160.
8. Frank R, Stollberg G. Medical acupuncture in Germany: patterns of consumerism among physicians and patients. Sociology of Health and Illness 2004; 26: 351-372.
9. Zollman C, Vickers A. ABC of complementary medicine. BMJ 1999; 319: 693-696.
10. Ernst E. The role of complementary and alternative medicine. BMJ 2000; 321: 1133-1135.
11. Kelner M, Wellman B. Complementary & alternative medicine: challenge & change. Amsterdam: Harwood Academic, 1997.
12. WHO. WHO Global atlas of traditional, complementary and alternative medicine. Kobe, Japan: World Health Organisation, 2005.
13. WHO. Traditional Medicine Strategy 2002-2005. World Health Organization, Geneva, Switzerland, 2002. Available: http://www.who.int/medicines/publications/traditionalpolicy/en/ (Accessed 1 June 2005).
14. Adib S. From the biomedical model to the Islamic alternative: A brief overview of medical practices in the contemporary Arab world. Social Science & Medicine. 2004; 58: 697-702.
15. The International Network for Cancer Treatment and Research (INCTR). INCTR Reaches out to Pakistan. INCTR newsletter 2001; 3. (Online) 2005: Available: http://www.inctr.org/publications/2001_v01_n03_a07.shtml (Accessed 8 December 2005).
16. Zakar M. Coexistence of Indigenous and cosmopolitan medical system in Pakistan. International Public Health Series 1998; 1: 305.
17. White R. Social and political aspects of men's health. Health 2002; 6: 267-285.
18. Rukanuddin A, Ahmed T. Introduction. In: Findings of Pakistan Demographic and Health Survey 1990/1991 Islamabad: National Institute of Population Studies, 1992.
19. Liede A, Malik I, Aziz Z, de los Rios P, Kwan K, Narod S. Contribution of BRCA1 and BRCA2 Mutations to Breast and Ovarian Cancer in Pakistan. American Journal of Human Genetics 2002; 71: 595-606.
20. Salmenpera L. The use of complementary therapies among breast and prostate cancer patients in Finland. European Journal of Cancer Care 2002; 11: 44-50.
21. Bhurgri Y. Cancer incidence in Karachi, Pakistan: First results from Karachi cancer registry. International Journal of Cancer 2000; 85: 325-329.
22. Tovey P, Chatwin J, Broom A. Complementary and alternative medicine (CAM) and cancer care: An international analysis of grassroots integration. London: Routledge. (In press).
Abstract
Introduction: The healthcare systems of developing countries are complex in that they often accommodate a range of disparate and often competing paradigms of care. This is the case in Pakistan where Indigenous traditional medicine (TM) co-exists with Western allopathic medicine and, in theory at least, with 'globalised' complementary and alternative medicines (CAM). To date we know little about what treatments are being chosen and why in this still predominantly rural country. Aim: To gain a preliminary understanding of patterns of usage of traditional medicine and globalised complementary and alternative medicine by cancer patients in Pakistan.
Method: Structured survey of 362 cancer patients, from diverse regions in the Punjab and North-west Frontier Province provinces, who were being treated in four different hospitals in Lahore, Pakistan.
Results: Use of traditional medicine is high amongst cancer patients, with many patients using a combination of different therapeutic modalities. Unlike studies in Western contexts, this study indicated no relationship between cancer type or sex and use of CAM/TM. However level of education was influential in determining usage of particular TM. There is, however, no uniformity in patterns of use of different TM.
Conclusion: There is less differentiation between social groups in usage of CAM and TM in Pakistan than has been reported in studies of western cancer patients. Differing levels of use for specific TM highlight the need to get beyond monolithic categorizations (such as TM) to understand use patterns for specific indigenous practices (in their social and cultural context).
Key words: cancer, complementary and alternative medicine, Pakistan, traditional medicine.
You might also be interested in:
2018 - Expectations of Rural Community-Based Medical Education: a case study from Thailand
2018 - Prevalence of Exposure to Occupational Carcinogens among Farmers
