Introduction
The work of allied health professionals (AHPs) in rural and remote areas is characterized by an increasing demand for services, workforce shortages1, a high turnover of staff2, and the challenges of delivering services to geographically dispersed populations. Delivering effective services in this environment has resulted in the need to explore alternative forms of service delivery that best meet the needs of rural and remote communities. Recently there has been substantial focus on therapy assistants (TAs) as an enhancement to allied health services in rural/remote Australia3-6.
Therapy assistants, also known as allied health assistants, deliver therapy programs to clients under the direction of AHPs. The use of 'skilled, technical health workers'7,8 to assist in the delivery of allied health services is not new. Historically TAs were aligned with one allied health discipline9-11 and often based within that department within the one facility. This was usually metropolitan facilities because they are of sufficient size and have large enough allied health departments to employ assistant staff. The concept of 'generic' assistants who work across a number of health disciplines has been raised12 and has previously encountered resistance from individual allied health disciplines10.
The rural and remote TA is different from the traditional assistant role. It is often integrated across a number of allied health disciplines such as physiotherapy, occupational therapy and speech pathology13. The multidisciplinary role, combined with the 'specialist-generalist' role of individual rural and remote allied health disciplines, results in TA work that is broad in scope and client mix. TAs complement rural and remote models of allied health service delivery, such as outreach services14, resulting in TAs who are located at a distance to the supervising AHPs15. Although there is accredited training available for TAs (Certificate III in Health Service Assistance - allied health assistance), in rural Western Australia (WA) a typical TA has no recognized qualification for their work in this area. The typical TA works part-time, and delivers individual 'one-on-one' physiotherapy, occupational therapy and/or speech pathology programs to children with disabilities, either in a school or a client's home15. Rural and remote TAs in WA are predominantly employed by the WA Country Health Service (WACHS), although education and Disabilities Services Commission (DSC) are also employers of TAs.
One advantage of TA programs is to improve access to allied health services in small towns without resident AHPs. TAs provide ongoing management of clients in between AHP visits, give continuity of services during AHP staff turnover, and build skills within the community5. TAs have also been investigated as a solution to allied health profession workforce issues16. Many rural AHPs, and people in rural communities, believe that TAs add value to therapy services delivered in the country17.
TAs form a significant part of the present rural and remote allied health workforce in Western Australia, with a substantial focus also in other areas of Australia3,5,6. A recent census of TA practice in WA15 showed that at the beginning of 2005, 98 TAs were identified working in rural/remote WA with a further 23 positions vacant. The majority of TAs had begun working within the last 5 years. Most TAs received multidisciplinary supervision, from physiotherapists, speech pathologists and occupational therapists, and half of the WA TA workforce were located at a distance to AHP supervisors.
Supervision, training and standards of practice of TAs are critical features of TA programs14. To date there are no common guidelines for TAs in the rural context. This article will focus on the first of the three critical features - supervision of TAs.
Supervision
Supervision has three important functions. First, supervision provides education and develops skills in those under supervision18. Second, supervision provides support. This includes personal validation, planning, feedback and refection18. Finally, the managerial role of supervision is critical in monitoring quality of care and protecting the welfare of clients seen by unqualified staff or those in training18,19. The rural context is a complex environment for supervising TA practice. Lowe14 has outlined a number of variables contributing to a lesser or greater degree of complexity to the TA work setting (Fig 1). Factors including the location of the AHP and TA, diversity of client mix, and number and experience of TA and supervisors influence the degree and methods required for supervision in a rural or remote context.
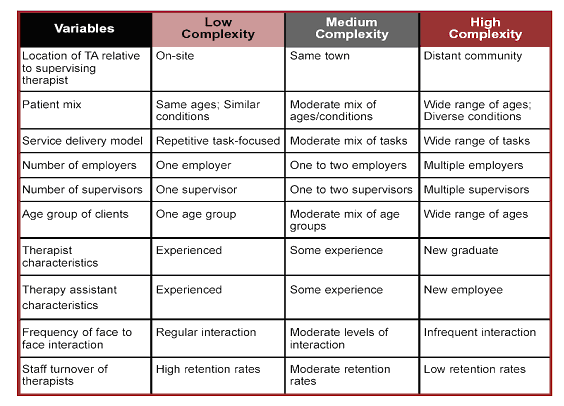
Figure 1: Outlining factors impacting on the complexity of TA work setting14 (reproduced with permission).
The therapy assistant project
The Therapy Assistant Project (TAP) was conducted between July 2003 and September 2004 in the WACHS Midwest Murchison Region (MMR) (Fig 2). The focus for the TAP was the regional centre of Geraldton and nine small rural towns receiving outreach speech pathology, occupational therapy and physiotherapy services. Small midwest towns range from 60 to 240 km from Geraldton, with populations ranging between 300 to 2000 people. A total of 13 TAs and 16 AHPs were working in the TA program, with five TAs working in Geraldton and the remainder based and working in towns in the surrounding region. TAs in WACHS MMR perform work 'typical' of WA rural and remote TAs as described previously. That is, their primary work includes delivering speech pathology, physiotherapy, and/or occupational therapy programs to school aged children with disabilities, in schools or client homes.
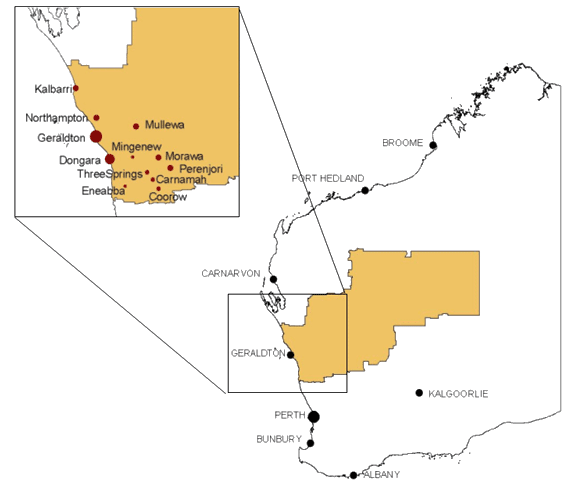
Figure 2: The WA Country Health Service - Midwest Murchison Region showing the site of the Therapy Assistant Project.
Building on substantial work previously undertaken in this area14,17 the aim of the TAP was to continue to develop a model of rural and regional TA practice. A planned outcome of the TAP included the development of resources with applicability to TA programs in other areas. The start of the TAP coincided with an expansion of the TA program within the WACHS MMR.
Improving supervision was one of a number of key project foci and had been identified as a significant concern by AHPs and TAs in the WACHS MMR. This study reports on two strategies utilized to improve supervision of TAs in the WACHS MMR: the development and implementation of minimum standards for supervision of TAs by AHPs and, secondly, training AHPs in supervisory skills.
Methods
Development and implementation of minimum standards in supervision
Formative steps in the development of minimum standards of supervision included reviewing published AHP guidelines for the supervision of assistants, development of draft guidelines suitable for the MMR, and consultation and review of draft guidelines by stakeholders in the TAP.
A search for guidelines and recommendations for the supervision of allied health assistant staff was conducted of electronic databases (MEDLINE and CINAHL) with keywords: therapy assistant, allied health assistant, and individual allied health professions and assistant. Physiotherapy, occupational therapy and speech pathology professional associations were contacted to source guidelines relating to assistants.
Eleven documents were retrieved and reviewed7,11,20-28. Particular note was made of guidelines that made explicit reference to the supervision of assistants, accounted for the complex nature of rural supervision14, were as up to date as possible, and represented speech pathology, occupational therapy and physiotherapy, the three allied health professions involved in the TAP. Three key guidelines were identified from Occupational Therapy Australia20, the Australian Physiotherapy Association7 and American Speech-Language-Hearing Association21.
Draft guidelines were formulated and reviewed by the project steering group, AHPs, TAs and allied health managers in the WACHS MMR. The project steering group included an AHP, a TA, a rural health service manager and project officer from Health Service Development from the MMR, a representative from DSC, Combined Universities Centre for Rural Health (CUCRH), the Australian Government Department of Health and Ageing, and the TAP project officer. The role of the steering group was to advise and support the project officer on aspects of project implementation and recommendations. Because members were from a variety of organizations with a stake in TA practice, each individual consulted with and disseminated information to their representative groups on aspects of the project.
Minimum standards for supervision were formulated in three areas. These were:
- Discussion - this includes discussion on client progress or their program, and administrative factors. Administrative factors included performance development or training needs. This occurs a minimum of once per month.
- Observation by the AHP of the TA conducting a therapy session two times per therapy program. A least one must be face to face, with further observation face to face, by videoconference or video recording.
- Program demonstration, when a new TA program is given or there are significant changes to an existing program. This may be face to face or by videoconferencing.
A 'program' refers to the combined therapy goals to be addressed over one school term or approximately 8 weeks. A full copy of these guidelines are available in the completed TAP report: http://www.cucrh.uwa.edu.au/projects/files/050204_TAP_Report.pdf.
Supervision guidelines specify the frequency, timetabling requirements, and recommended methods for supervision (face to face, phone, videoconferencing and video recording), recording, and giving feedback. Training was provided to AHPs in technical and clinical aspects of videoconferencing. Minimum standards for supervision were introduced in January 2004.
Training in supervisory skills
A three-hour introductory supervision training workshop was conducted for WACHS MMR AHPs supervising TAs and students. Formative information for the workshop was gathered by discussions with AHPs on their needs and requirements in supervision. A workshop outline was created with an emphasis on practical supervision of and skill development for students and TA supervision.
Evaluation method
A mix of methods was used to measure the impact of introducing draft minimum standards of supervision. First, information relating to supervision was gathered though focus group discussion. Eight AHPs and 11 TAs participated in six focus group discussions 6 months following the introduction of supervision guidelines. Focus groups were semi-structured and elicited participant perspectives on a wide variety of issues relating to TA practice. Interviews lasted between 50 min and 1.25 hours. Interviews were tape recorded. Tapes and written notes kept by the interviewer were transcribed into Microsoft Word format.
Thematic analysis of transcripts was completed by the principal researcher (IL)29. Each transcript was read in detail. Significant themes were identified from focus group transcripts and notes taken during each focus group. Emerging themes were repeatedly checked against transcripts and discussed with members of the project steering group until coherent meanings were determined.
Second, changes in the amount and type of supervision were ascertained by an audit of TA supervision logs. Supervision logs were recorded by TAs and documented the date, amount, type and medium used for supervision. Supervision logs were introduced prior to the introduction of minimum supervision standards. This enabled baseline levels of supervision to be established prior to implementing supervision interventions and supervision levels and practices to be monitored during TAP.
Third, an audit of videoconference log books for supervision use was conducted. Videoconference log books specified the date, time, amount and purpose of videoconference use. Information from the supervision and videoconference logs were entered into Microsoft Excel and described using Excel functions.
Training evaluation
An evaluation form was completed following the introductory supervision workshop seeking participant perspectives on aspects of the workshop content and process. Further information related to the supervision training was elicited during focus group discussions as above.
Results
Focus group discussions
A high level of satisfaction was reported by AHPs and TAs following the introduction of supervision guidelines, methods to record supervision, and supervision training. Particular themes identified by AHPs included improved organization, the usefulness of the guidelines, and the supervision logs in the supervision process (four informants). The following comment typifies AHPs' responses:
It's good to have things standardized, it's good to have a system for supervision and so forth. [AHP 4]
It's a bit of an eye opener [the supervision logs], because you kind of go 'oh we're doing OK' and then you do kind of look at it and go 'oh that's probably not very much' kind of thing so from time to time. I think it's a good thing just to make you realise you know, what level is expected of you. [AHP 1]
Improved organization of supervision and increased amounts of supervision was also identified by TAs (eight informants).
...we've been given dates for supervision and usually we have to organise that ourselves before, so something has gone down where this has organised supervision across the board equally, we have supervision two times in the term so that's at least once a month. [TA 8]
Well by filling them in [supervision logs] made us all look at how much supervision we get and it's also making the therapists accountable for how much supervision and contact that they have with us as well. [TA 6]
Further themes identified by AHPs included aspects of supervision skill requirements (three informants) and the challenges of supervising experienced TAs as an inexperienced AHP (two informants): 'Competencies we need to fill to be good therapists [are important]... like what are good supervising techniques' [AHP 1].
There can be problems [supervising] when, and quite rightly so sometimes, the TA does have a lot more experience than the graduate therapist in their own way. [AHP 4].
Changes in supervision
The uptake of the supervision logs by TAs, as a means of recording supervision occurrences, increased during the TAP (Fig 3).
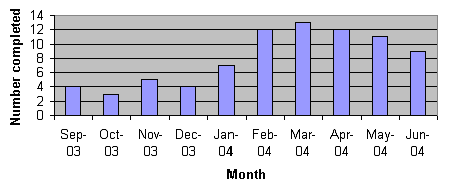
Figure 3: The number of completed supervision logs received from therapy assistants per month, September 2003 - June 2004.
Figure four displays information from the supervision logs of four TAs with complete supervision log data before and after introduction of minimum supervision standards and training. Minimum standards for supervision were introduced at the beginning of January 2004. This demonstrates an increase in the overall amount of supervision for these four TAs. It is worth noting that January and April coincide with school holiday periods and so TAs who work in schools would not have been seeing clients, frequently TAs holiday during this period and there are fewer supervision occurrences.
The majority of supervision occurrences recorded were program discussion, followed by program observation. Figure 5 displays the type of recorded supervision occurrences for the period of the TAP.
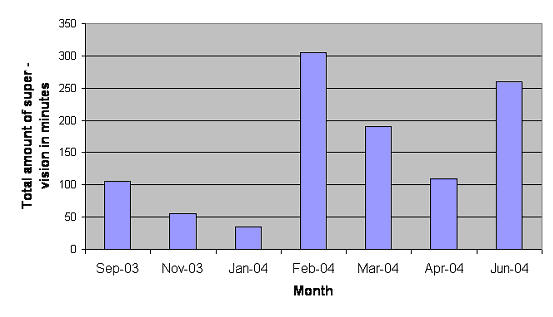
Figure 4: The total amount of supervision in minutes for each month for four therapy assistants with complete supervision log data before and following the implementation of supervision interventions.
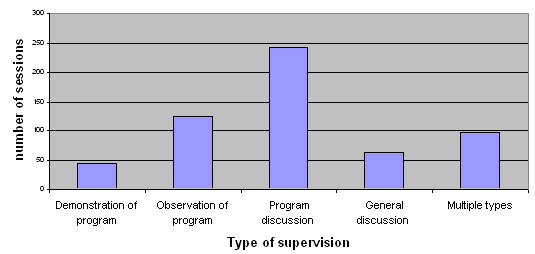
Figure 5: The type of supervision occurrences recorded in supervision logs between September 2003 and June 2004.
Sub-analysis of the types of supervision compared with the minimum standards of supervision was completed for four TAs with complete supervision log records. The majority of supervision by discussion met the minimum standards for speech pathology, occupational therapy and physiotherapy. In all cases supervision by observation did not meet the minimum standards.
Investigation of videoconference records indicated limited use of videoconferencing for supervision. Since the introduction of minimum standards of supervision there were only three recorded sessions of supervision by videoconferencing. Table 1 displays a comparison of methods used for supervision during the duration of the TAP.
Table 1: The number and method of therapy assistants' supervision occurrences in the West Australian Country Health Service Midwest Murchison Region, September 2003 to June 2004

Supervision training
Eleven AHPs attended an introduction to supervision workshop. The response of workshop participants to training was positive. Participants identified the use of scenarios, role plays and group activities for learning (six participants) as helpful. Insufficient time was identified (five participants) as a negative aspect. Some AHPs requested further training in supervisory skills (two participants).
The requirement for further training in supervision skills was also identified by AHPs with less experience during in-depth focus group interviews (three informants). Key topics identified by participants included training in the management of difficult supervision scenarios and using case examples specific to TA supervision:
...the TA hasn't been doing what you want and I haven't felt comfortable. Getting a kind of recommended format [for supervision] you'd follow in that kind of situation. [AHP 1]Discussion
To date there are no established guidelines or recommendations for supervising multidisciplinary TAs in a rural context. Supervision is a key aspect of TA practice and TAs presently form a significant part of the rural and remote allied health workforce. With a current focus on this area in rural and remote Australia it is a priority to develop resources to support TA programs. In this study, supervision of TAs improved with the introduction of supervision guidelines, a means to record supervision, and training for AHPs in supervisory skills.
By introducing a framework to guide supervision (minimum standards of supervision) and monitor supervision (via supervision logs) the amount of supervision of TAs increased. AHPs and TAs also demonstrated greater satisfaction with the supervision process. As was evident from comments by TAs, having established guidelines in place empowered them to seek supervision from their AHP supervisors.
The supervision logs served two purposes in this project. First, they provided feedback to AHPs and TAs on supervision performance. AHPs in particular indicated that receiving feedback on the amount of supervision was a critical 'eye-opener' for them on their supervision performance. Although they were aware of the importance of supervision of TAs, this was frequently de-prioritised in a busy therapy caseload, and so a mechanism for feedback was seen as crucial. Second, supervision logs enabled the monitoring and evaluation of supervision practices coinciding with strategies introduced to support supervision. Supervision logs are now used as part of routine supervision practice in the WACHS MMR TA program and as a part of the ongoing evaluation of the program.
Although the overall amount of supervision increased, not all supervision types achieved the recommended minimum standard. This implies either the minimum standard stipulated in the guidelines was not feasible or realistic, or there is insufficient supervision of this type occurring or recorded. There was very limited uptake of videoconferencing as a method of supervision. The use of videoconferencing has been advocated to improve access for rural and remote areas to health services30,31, and also in the use of supervision, for example student supervision32. The reason for low levels of supervision by observation and videoconference use, which can be used to observe a TA delivering a therapy session, is presently unclear and would be valuable information to ascertain in the future.
There were several limitations to this project. The minimum standards of supervision were developed specifically for the regional and rural outreach allied health service for this WA region. These guidelines have been endorsed locally for use as a part of policy for TAs in the WACHS MMR. In the WACHS MMR there are relatively few AHPs compared with some rural regions, which limits the potential sample size of this study. As a result the applicability of these resources for areas with different allied health workforce, population and geographical characteristics is unknown.
In WA an adapted version of these guidelines is currently undergoing consultation and review within WACHS for development into a policy for TAs across the WACHS region. There is a need for ongoing evaluation of these guidelines as other WA health services adopt them, and further evaluation of these resources in other contexts.
The American Speech and Language Association stipulates speech-language pathologists' completion of at least one pre-service course of continuing education unit in supervision'21. In the present study, training emphasizing interactive teaching methods including supervision role-play and case scenarios was viewed positively by participants. One three-hour session was insufficient, with participants requesting further training in complex supervisory situations.
As a sequelae to this project further training in supervision for therapists has been developed in a follow-up project: the WACHS/DSC Training Initiative33. The WACHS/DSC TA Training Initiative consists of a series of training modules in clinical and management aspects for TAs and AHPs working with TA programs. Modules are offered via videoconferencing. A training workshop on supervising TAs has been developed with delivery based on a 'train the trainer' approach and delivered face to face to therapist representatives from each WA country health region. The WACHS/DSC TA Training initiative will be the topic of a future publication. For further details please contact the author [BG].
Conclusion
Currently there is considerable focus on the role of TAs to enhance and work with AHPs in country Australia. This article has highlighted supervision as one important aspect in the emerging area of rural TA practice. It is hoped the minimum standards for supervision developed in this project, and the strategies used to support AHPs and TAs improve supervision, will be applicable to other rural health services.
There is more work required in order to better outline and understand the delivery of therapy services by TAs or other 'skilled, technical health workers' in the rural and remote context. Priorities include the development of appropriate and accessible training for these workers, and describing and testing models of allied health service delivery delivered by such workers, that best meet the needs of Australian rural, remote, and Indigenous communities. A further priority is research investigating the health outcomes from these well-supported programs.
Acknowledgements
The authors would like to acknowledge Suzanne Spitz, Maeva Hall and Peter Shaw for their considered assistance and advice during the project, and Ann Larson and Marisa Gilles for reviewing manuscripts of this article.
References
1. National Rural Health Alliance. Under pressure and under-valued: allied health professionals in rural and remote areas: Canberra: NRHA, October 2004.
2. O'Kane A, Curry R. Unveiling the secrets of the allied health workforce in Australia. Proceedings, 7th National Rural Health Conference, 1-4 March 2003; Hobart, Tasmania, 2003.
3. Telfer J. Workforce planning-thinking outside the square for a flexible allied health workforce. Walking Together - side by side. Proceedings, The National SARRAH Conference, August 26-28; Alice Springs, Northern Territory, 2004.
4. Goodale B, Lin I. Therapy assistants - a model in rural/remote Western Australia. Walking Together - side by side. Proceedings, The National SARRAH Conference, 26-28 August 2004; Alice Springs, Northern Territory, 2004.
5. Battye KM, McTaggart K. Development of a model for sustainable delivery of outreach allied health services to remote north-west Queensland, Australia. Rural & Remote Health; 3: 194. Online (2003). Available: http://rrh.org.au (Accessed 19 January 2004).
6. Frakes K-A, McGrath D. Tapes, scales and monofilaments. Walking Together - side by side. Proceedings, The National SARRAH Conference, 26-28 August 2004; Alice Springs, Northern Territory, 2004.
7. Australian Physiotherapy Association. Physiotherapy assistants: policy statements and guidelines. Melbourne: APA, 2002.
8. OTA. Occupational therapy assistants: policy statements and guidelines. Perth: Australian Association of Occupational Therapists, WA Inc, 2005.
9. Kimbarow M. Ahead of the curve: improving service with speech-language pathology assistants. American Speech Language Hearing Association 1997; 39(4): 41-44.
10. Ellis B, Connell NAD. Factors Determining the Current Use of Physiotherapy Assistants. Physiotherapy 2001; 87: 73-82.
11. Russell KV, Kanny EM. Use of aides in occupational therapy practice. American Journal of Occupational Therapy 1998; 52: 118-124.
12. Knight K, Larner S, Waters K. Evaluation of the role of the rehabilitation assistant. International Journal of Therapy and Rehabilitation 2004; 11: 311-317.
13. Hall M. Integrated therapy assistants and video-conferencing. Proceedings, 7th National Rural Health Conference, 1-4 March 2003; Hobart, Tasmania, 2003.
14. Lowe W. Rural Western Australian therapy assistant project. Perth: Disabilities Services Commission and Combined Universities Centre for Rural Health, 2003.
15. Lin I, Villaneuva K, Goodale B, Spitz S. Therapy assistants in WA: where, who and what does it mean? Proceedings, 2nd WA Rural and Remote Allied Health Forum. Health Communities: Closing the Gap. 24-25 June 2005; Fremantle, WA, 2005.
16. Watson C. Discussion paper: the feasibility of an allied health training program to address allied health work force shortages in the Australian Capital Territory: Canberra: ACT Health/Therapy ACT Allied Health Services Allied Health Assistant Project, 2004.
17. Loud J. Evaluation of the Midwest Health Service integrated therapy assistant program. Geraldton: Combined Universities Centre for Rural Health, 2000.
18. Hawkins P, Shohet R. Supervision in the helping professions. Buckingham: Open University Press, 1989.
19. Bernard J, Goodyear R. Fundamentals of clinical supervision. Boston: Allyn and Bacon, 1992.
20. Riches J, Olsson H, Doughty S, Peacock J, Gelle R, Bestow C. Guidelines for the supervision of occupational therapy support staff. Perth: Occupational Therapy Australia (WA), 1992.
21. American Speech-Language-Hearing Association. Guidelines for the training, credentialing, use, and supervision of speech-language pathology assistants. Rockville: ASHA, 1996.
22. Chartered Society of Physiotherapy. Physiotherapy assistants code of conduct. London: The Chartered Society of Physiotherapy, 2002.
23. Brayman SJ, Strickland LR. Supervision guidelines for certified occupational therapy assistants. American Journal of Occupational Therapy 1990; 44: 1089-1090.
24. Australasian Podiatry Council. Guidelines for the use of Podiatry Assistants. Melbourne: APC, 2001.
25. Glantz CH, Richman N. OTR-COTA collaboration in home health: roles and supervisory issues. American Journal of Occupational Therapy 1997; 51: 446-452.
26. Paul-Brown D, Goldberg LR. Current policies and new directions for speech-language pathology assistants. Language, Speech & Hearing Services in the Schools 2001; 32: 4-17.
27. Puccetti D. Supervision of the certified occupational therapy assistant: developing a knowledge base and strategy. Occupational Therapy in Health Care 1988; 5: 23-35.
28. Stevens A. Speech pathology Australia position statement on therapy assistants. Melbourne: SPA, 2004.
29. Taylor SJ, Bogdan R. Introduction to qualitative research methods, 3rd edn. New York: John Wiley & Sons,1998.
30. Western Australian Country Health Service. Telehealth. Available: http://www.wacountry.health.wa.gov.au/default.asp?documentid=408 (Accessed 19 January 2006).
31. Ellis I, James R. Enhancing interactivity in videoconference sessions: tips and tools for health promoters. Australian Journal of Primary Health 2004; 10: 92-95.
32. Liu L, Miyazaki M. Telerehabilitation at the University of Alberta. Journal of Telemedicine & Telecare 2000; 6(Suppl 2): S47-S49.
33. Western Australian Country Health Service - Disabilities Services Commission. WACHS-DSC TA Training Initiative. (Online) 2005. Available: http://www.mmhr.org.au/Home.asp?documentid=348 (Accessed 19 January 2006).

