Introduction and literature review
The Spencer Gulf Rural Health School (SGRHS) combines one of the nine Australian Federal Government funded Rural Clinical Schools (RCS) established in 20011 and one of the eleven University Departments of Rural Health (UDRH). Situated in multiple learning centres in north-west South Australia, the SGRHS provides clinical teaching and administrative support for short and long placements for medical, nursing, pharmacy, allied health and other students participating in health related courses. Placements range in length from one-week introductory Rural Week programs for all medical2 and some health sciences students, to one-year placements for medical students in their clinical years. Placements range in scope from observational or 'shadowing' through to senior students being integrated into the health-care setting as valuable team members.
As medical, nursing and health education is embracing the ambulatory setting and moving students to rural health placements, it becomes important to analyse the capacity of the preceptors involved in such initiatives2-4. The concept of 'preceptoring' first began to be used in the literature of health science education in the 1960s5,6. Sachdeva argues that the educational value of using preceptors is firmly grounded in the principles of adult education7. The terms 'clinical supervisor' and 'preceptor' have been used loosely in the literature with some confusion. The literature from medical, nursing and allied health fields is in general agreement about the role of the preceptor7-10 and suggest that it includes supervising, teaching, role modelling, assessing and evaluating3-7,9,11-16. Specifically, this article relies on the recent literature review article by Mills et al. and the succinct definitions they found16. Preceptors focus on skill acquisition, socialisation and assessment for short-term student placements. Clinical supervisors focus on clinical practice for practicing professionals through reflection and provision of professional guidance over a longer period of time. The term 'preceptor' is used throughout this paper.
A number of studies have documented the benefits and disadvantages of preceptoring3,5,6,11,17-19. One of the major benefits of teaching a student can come from the increased enjoyment of practice and enhancing existing knowledge through activities that further professional growth such as increased reading of literature19. There is also patient benefit6. Some of the negatives have included increased costs of practicing and decreased productivity11.
There have been fewer studies, however, that have looked specifically at rural health practitioners as preceptors19,20.
There are a number of skills that have been associated with preceptoring4,7,12,13. One study documented seven main categories of effective teaching behaviours or skills for rural family medicine preceptors4. A very recently published literature review reports that time management is the biggest issue for rural general practitioners20. Little evidence exists as to the opinions or influential factors with regards to nursing and allied health staff members preceptoring medical students. Broad exposure of students to a multidisciplinary health-care team through preceptoring may underline the importance of multidisciplinary health care which would become integral to them if they become rural medical practitioners.
Preceptor view
Currently there is a paucity of research in Australia20,21 and internationally22-24 regarding the evaluation of experiences of the rural/remote preceptor. What literature exists is predominantly focused on the nursing profession21,22,25-27, is discipline specific28, centres on the views of students' experience29 and is metropolitan based17,29,30.
The available literature identified both positive and negative aspects of the experience of preceptoring. Common themes centre on the challenges of time management such as decreased productivity, while personal professional growth, including the updating of the preceptors' clinical knowledge, was identified as a positive17,23,26. Dilbert and Goldenberg summarise their view: 'positive aspects of the preceptor role to be associated with personal and professional growth and job enrichment', and highlight the 'negative aspects relate more to a lack of administrative support, workload adjustment and financial recompense for the additional responsibilities.'29 p.1145.
While preceptoring of students within rural South Australia has occurred for years, no evaluation data on preceptors experiences/perceptions have been consistently gathered. By understanding the incentives and barriers to being a preceptor it is hoped to improve the sustainability of preceptors and ensure their ability to educate the next generation of rural health professionals.
Methods
The SGRHS commenced a program to evaluate preceptors in 2002 with a questionnaire developed as an undergraduate student research project by one of the authors (KB)31. The aims for this evaluation were to establish:
- What factors influenced the professional's decision to precept students?
- Did preceptors report having adequate skills and preparation for preceptoring?
- What were the variations in professional streams with regards to the factors and skills of the staff involved?
- What were preceptors' overall perceptions of their role?
The questions were derived from the preceptor literature. The survey instrument was piloted with 36 valid responses in 2002 and subsequently modified. In 2003 it was retested when 25 questionnaires were distributed to preceptors involved in Rural Weeks2.
This questionnaire has now become the standard preceptor survey tool in SGRHS (Appendix I). The questionnaire uses Likert scales and open-ended questions, contains questions relating to demographic information about the preceptor, as well as questions establishing what influences health professionals to undertake the preceptor role, and seeks preceptors' experiences and opinions of rural placements.
Analysis of Likert scale questions was carried out using SPSS vers. 12 (SPSS Inc, Chicago, IL), Microsoft Excel 2000 and Xpro vers 5.4 (Statistical Solutions; Saugus, MA, USA). Qualitative coding of open-ended answers was undertaken by one of the authors (SS) using grounded theory methodology32. Thematic analysis revealed 22 codes for Question 5 (with between 1 and 25 comments attributed to each code) and 26 codes for Question 6 (with between 1 and 37 comments attributed to each code). The questionnaire was voluntary and anonymous and respondents were able to withdraw at any time. There was no benefit nor disadvantage to respondents for questionnaire completion or non-completion and cohort data only was accreted. As such, this evaluation fulfills a role as quality assurance of education and human research ethics committee approval was neither required nor sought.
Results
By 2004, SGRHS had established a large rural placement program over many disciplines in multiple locations. In October 2004 all preceptors who had supervised students in the previous 12 months (n = 255) were invited to participate in an evaluation using a mailed-out, paper-based questionnaire.
Six were returned without completion, for reasons such as that the preceptor had left the practice and these were deleted from the preceptor database. There were 145 valid responses (58% response rate, 145/249). This response is considered adequate for a once-off personalised mail-out survey, which did not utilise the Dillman protocol33. No further attempts to contact preceptors again were made bearing in mind the anonymity of respondents.
The questionnaire results will be presented in three categories:
- Demographic data (Questions 1-4)
- Factors influencing the decision to precept students (Question 5 in 7 parts)
- Preceptors' experiences of the student placement (Question 6 in 7 parts and the 3 qualitative open-ended questions).
Demographic data (Q1-4)
Preceptors were asked to nominate details of their professional stream and how many years they had spent working in a rural or remote area. They were asked whether they had preceptored before and for which discipline(s) of student.
Table 1 reveals that overall the distribution of professions for respondents is similar to the overall distribution in the target population. Almost half the responses (n = 70, 48%) were from medical professionals and they represented 40% of the sample of preceptors (102/252). Examples of the professional stream of those who classified themselves as 'other' were pharmacy, pathology, volunteer ambulance officer, medical research, medical receptionist, aged care worker and community health worker.
One hundred and forty-four respondents reported how many years they had spent in rural areas (Table 2). They are predominantly either recently arrived in a rural area or long-term residents.
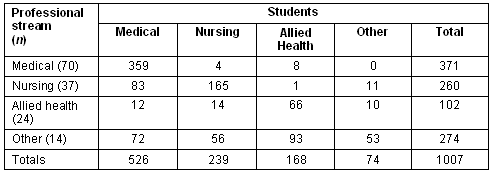
Most respondents (139/145) indicated how many students they had preceptored (n = 1007), with the majority being medical students (526) (Table 3). Preceptors report often supervising students from professional streams other than their own. Most (n = 133 /143, 93%) respondents had preceptored previously.
Table 1: Representativeness of the respondents - a limitation to the study
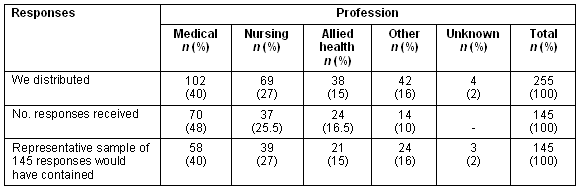
Table 2: Number of years spent working in a rural or remote area in numbers and (relative frequency as a percentage)
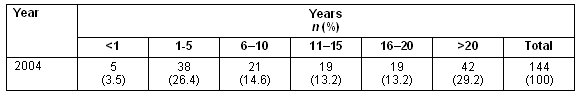
Table 3: Number health professional and number of students preceptored
Factors influencing the decision to supervise/precept students (Q5)
In question 5 and 6 respondents were invited to rate their agreement with a statement or question on a 5 point Likert scale where 1= strongly disagree and 5 = strongly agree. Preceptors had mostly chosen to precept because of their enjoyment of teaching, desire to see student's knowledge and skills improve and to promote a rural career (Table 4). They were less motivated by the opportunity for contact with academic faculty staff.
Table 4: (of Question 5) Factors influencing your choice to precept students
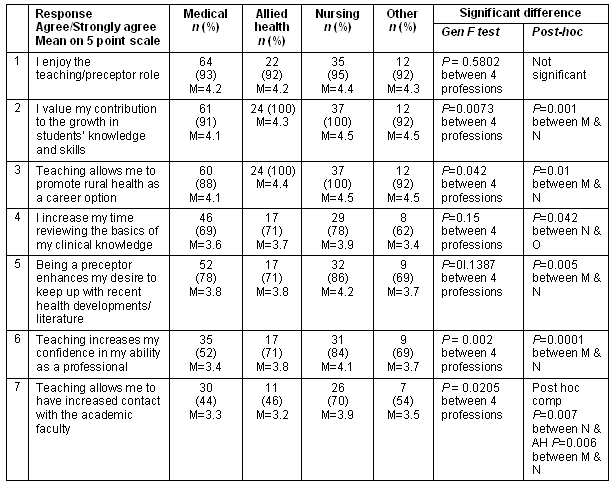
Further analysis of the data by professional stream provided an insight into the different perceptions and attitudes among the preceptors by discipline. While there were no significant interdisciplinary differences in the data for Questions 5.1. and 5.4, the other responses revealed interdisciplinary differences. In particular, the post hoc tests showed that there was a very significant difference (p = 0.001) between medical and nursing, stronger in nursing, for Q5.2 'I value my contribution to the growth in student's knowledge and skills'. That was also true for Q5.3 'I enjoy the teaching/ preceptor role' where post hoc tests showed that there was a significant difference between medical and nursing, stronger in nursing (p = 0.01) and for Q5.5 'Being a preceptor enhances my desire to keep up with recent health developments/literature' where nursing scores were significantly higher than medical (p = 0.005). When considering the proposition Q5.6 'Teaching increases my confidence in my ability as a professional', nurses scored significantly more highly than medical and post hoc comparisons revealed the very significant difference between medical and nursing (p = 0.0001). Last, analysis of the proposition Q5.7 'Teaching allows me to have increased contact with the academic faculty' revealed a weak overall significant difference among the four professions (p = 0.02). Post hoc comparisons showed that there was a very significant difference between nursing and allied health (p = 0.007) and between nursing and medical (p = 0.006). The nursing scores were the highest (M = 3.86) against allied health (M = 3.17) and medical (M= 3.31).
Preceptors' experiences of the student placement (Quantitative Q6 and qualitative Q7-9)
The questionnaire sought feedback from respondents about their placement experience (Table 5). The preceptors reported strong agreement that the placements allowed promotion of rural careers, seemed to be educationally useful for the students, and that prior communications were the least satisfactory part of the placement.
Table 5: (of Question 6) Preceptor experience of the student's rural placement experience 2004
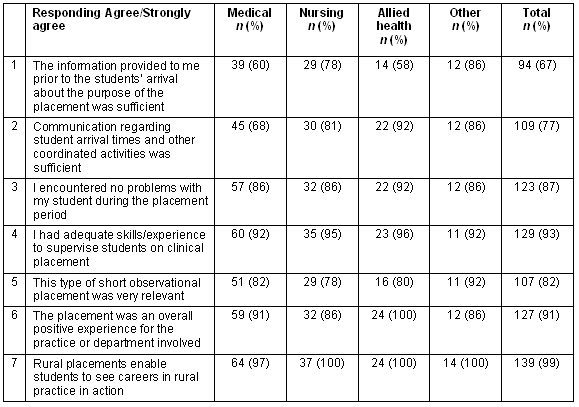
The responses were categorised by professional discipline grouping. None of the differences among professional groupings was significant except Table 5, Question 2 'Communication regarding student arrival times and other coordinated activities was sufficient' where medicine scores were lower overall than nursing and allied health (p = 0.023).
Qualitative results preceptors' experiences of the student placement
Three open-ended questions were included in the questionnaire (Appendix 1). Responses were coded and analysed using grounded theory analysis techniques. Codes are available from the analyst (SS).
The most enjoyable aspect of preceptoring for respondents was their desire to share youthful students' enthusiasm for learning (25 respondents), to teach about rural health and 'ignite the spark' about rural health care (22), to teach and foster learning behaviours (21) and to see students' skills, attitudes and confidence improving (20). Nineteen respondents also valued interacting with students academically and learning from their contemporary knowledge and values. Medical practitioners most enjoyed the enthusiasm of youthful students, and teaching as well as fostering learning behaviours; whereas, nurses believed that the most enjoyable aspect of preceptoring students was encouraging their understanding of rural health care. Medical, nursing and allied health preceptors all valued seeing students' confidence and skills improving; while medical preceptors valued interacting with students academically and learning from their contemporary values more than the other groups.
When respondents were asked to reflect on the least enjoyable aspect of preceptoring, by far the most prevalent response related to time (37 respondents) - the shortage of time and the pressure preceptors placed on themselves when they were simultaneously preceptoring a student and practising. Associated issues highlighted were the slowing of consultation time (n = 14), increased workload (7) and lowered income (6). Expectations of both the preceptor and the student were at times not met, for example a student's skill level being lower than expected (7), or that students had unrealistic expectations of the preceptor (4). Administration of the placement - communication, information follow up and insurance - were mentioned eight times.
Teasing out interdisciplinary differences, more than any other topic, medical preceptors mentioned 'Time management constraints' (23 respondents), including too little time for tasks such as teaching and normal workload, report writing and too busy to interact with student as the least enjoyable aspect of preceptoring. This was also associated with slowing of consultation time (12 medical responses) and lowered income (four medical responses). Seven nurses also mentioned the time constraint issue and four nurses noted that students' skills were not as expected.
Twenty-six respondents took the opportunity to provide constructive criticism of matters related to administration of the program, their role as a preceptor, and their relationship with the universities. More general comments about students' wellbeing were also proffered, reflecting respondents' interest in students' general welfare while on placements. Most prevalent of these general responses were requests for improved communication between the academic supervisor and the preceptor (three respondents). Eight respondents (8/145) took a further opportunity to provide positive feedback about the placement students they preceptored or supervised and the placement program citing, for example, that 'the current program is ideal'; that 'students motivate the staff to increase their knowledge' and that 'I love teaching' and it is 'enjoyable working with students'.
Discussion and Conclusion
SGRHS has established an ongoing evaluation of preceptors who teach health professional students in clinical disciplines. A questionnaire was developed and tested in 2002 and 2003. At the end of 2004 it was mailed to 255 preceptors who had accepted 1007 students for SGRHS. Preceptors tended to be recent (<5 years) or highly experienced (>15 years) rural practitioners. Generally they enjoyed their role of increasing student knowledge and skill but also recognised an opportunity to promote rural careers. Comparing the professional groups, nurses were more positive in their responses than were medical or allied health professionals. Overwhelmingly preceptors believed that students obtained a valid experience of rural practice, that as preceptors they were appropriately skilled for their role, and that their workplace benefited from the presence of students.
These preceptors are highly valued by SGRHS and this evaluation was motivated by a desire to understand their situation so that we can react to their needs. The observed differences between professional disciplines may be a result of fundamental differences in the way health services are funded in rural Australia. Doctors are predominantly in private fee-for-service practice and are eligible for financial support through the Practice Incentive Payments program, while nurses are the professional groups most likely to be in salaried employment. The allied health professionals in the Spencer Gulf region are in a mixture of private and salaried practice. Doctors are aware that imposts on their time have a direct effect on income generated, whether to cover practice costs or to flow on to take-home pay. For salaried nurses, preceptoring students will have a similar impact on their daily workload but without the direct financial cost. Also decisions to accept nursing students will usually be taken by senior management who will then place the students into various wards and departments.
While the overall response rate (58%) was acceptable, the low numbers of respondents from the 'other' group was regrettable, and there is a significant difference between the number of responses expected and received from this sub-grouping. Despite this limitation, there are no significant differences between the expected and received response rates from medical, nursing and allied health professionals, despite over-representation by medical professionals, and we believe that the discipline-streamed data can be validly considered. We acknowledge recall bias as a study limitation - respondents may not have recalled accurately how many students within each discipline they supervised.
This is a bounded study of SGRHS preceptors and of data collected in 2004 only. Although it best informs the management and administration of SGRHS placements, valuable general insights may be provided for other universities and other community placement settings.
The Rural Undergraduate Support and Coordination (RUSC), UDRH and RCS programs have been funded by the Australian government to enable rural health student placements. The medical student programs have been in existence longer, largely as a response to the earlier recognition of a rural doctor shortage than of the existence of the same problem among all rural health professional groups. Our experience in SGRHS is that the medical student programs have been more generously funded. These funds have been disbursed into private medical practices to address the financial disadvantages of accepting medical students. These evaluation results support our belief that our regional doctors are able to sustain the student teaching load that has expanded rapidly with the development of SGRHS.
It is reassuring to see that nursing professionals are enthusiastic about their role as preceptors. SGRHS is anticipating a large increase in the number of nursing students with the revision of the University of South Australia's curriculum and the initiation of an undergraduate nursing course at the University of Adelaide. Urban public sector hospital work is changing rapidly and financial constraints are having a negative impact on students' urban placements. The UDRH program does not have adequate funds to support this expansion on a background of presumed contraction of state department of health funds flowing into rural areas. The enthusiastic nursing preceptors in the 2004 survey may not remain so if they are inundated with nursing students while remaining inadequately resourced by either governments or the universities.
Fit with literature
The results of our analysis have been compared with the international literature on what motivates clinicians to precept and what makes preceptoring sustainable. The SGRHS data is consistent with research conducted by Stone et al.23, Baldor et al.17, Dilbert and Goldenberg30, and Usatine et al.6. Their consistent theme of personal professional growth through having the students present, counterbalanced by the pressure of time and financial incentives, are consistent with our findings. Our results are consistent with both Walters et al.20 and Stone et al.23 who reported the positivity of clinical teaching, for example 'teaching was a way to update their clinical knowledge'23 and the negativity of time pressure 'the single most significant pressure when supervising medical students is time management'20.
This is further supported by Usatine et al.'s study of medical student preceptors where they highlight the 'worries about balancing time with the student vs maintaining a busy practice' and conclude that while 'preceptors experience professional growth through students' direct presence in their offices, time management while precepting is the greatest challenge reported by preceptors'6.
SGRHS supports all preceptors by conducting rural student clinical supervision training for health professionals in rural and/or remote locations, but to ensure sustainability of preceptors a number of areas need to be improved. This study's findings suggest that recommendations to be enacted include:
- acknowledging the time and loss of productivity incurred for the preceptors whether or not a financial incentive is offered
- improving communication and administrative support between the sending institution and the placement site
- maintaining a multi-disciplinary approach to selecting preceptors for all health professional students
- persisting with rural placements in acknowledgment that preceptors themselves believe that this type of placement allows students to see careers in rural practice in action, which is the overarching goal for rural placements.
For the duration of the rural health workforce shortage the sustainability of RUSC, RCS and UDRH programs will critically depend on a high percentage of rural health professionals being preceptors for the universities. Thus, responding to evaluation findings such as these is an essential element of maintaining stable rural health professional education.
Acknowledgements
The authors acknowledge Dr Ian Blue for suggesting that the SGRHS evaluate rural preceptors' attitudes during his tenure at SGRHS; and Dr Andrew Thornett for supervision of Kate Brown's project in 2002. Financial support from the Australian Government Department of Health and Ageing is provided to The University of Adelaide and the University of South Australia for the Rural Undergraduate Support and Coordination, Rural Clinical School and University Department of Rural Health programs.
Teofilonestor Cayetano, who devoted a large amount of energy to the background for this article, died suddenly on 21 August 2005.
References
1. Prideaux D, Saunders N, Schofield K, Wing L, Gordon J, Hays R, Worley P, Martin A, Paget N. Country Report: Australia. Medical Education 2001; 35: 495-504.
2. Newbury JW, Shannon S, Ryan V, Whitrow M. Development of 'rural week' for medical students: impact and quality report. Rural and Remote Health 5: 432. (Online) 2005. Available: http://rrh.org.au (Accessed 22 February 2006).
3. Zachary T, Smith-Barbaro P. Value of a family medicine preceptorship/clerkship to students, preceptors, and communities: observations from a 25-year-old program. Family Medicine 2001; 33: 500-501.
4. Goertzen J, Stewart, M, Weston, W. Effective teaching behaviours of rural family medicine preceptors. Canadian Medical Association Journal 1995; 153: 161-168.
5. Ferenchick G, Chamberlain J, Alguire P. Community-based teaching: defining the added value for students and preceptors. The American Journal of Medicine 2002; 112: 512-517.
6. Usatine RP, Hodgson CS, Marshall ET, Whitman DW, Slavin SJ, Wilkes MS. Reactions of family medicine community preceptors to teaching medical students. Family Medicine 1995; 27: 566-570.
7. Sachdeva AK. Preceptorship, mentorship, and the adult learner in medical and health sciences education Journal of Cancer Education 1996; 11: 131-136.
8. Geyman JP, Hart LG, Norris TE, Coombs JB, Lishner DM. Educating generalist physicians for rural practice: how are we doing? Australian Journal of Rural Health 2000; 16: 56-80.
9. Lang F, Ware BR. A national study of required family medicine clinical rotations. Family Medicine 1991; 23: 516-520.
10. Elliott-Schmidt R, Strong J. Rural occupational therapy practice: a survey of rural practice and clinical supervision in rural Queensland and northern New South Wales. Australian Journal of Rural Health 1995; 3: 122-131.
11. Vinson DC, Paden C. The effect of teaching medical students on private practitioners' workloads. Academic Medicine 1994; 69: 237-238.
12. Usatine RP, Nguyen K, Randall J, Irby, DM. Four exemplary preceptors' strategies for efficient teaching in managed care settings Academic Medicine 1997; 72: 766-769.
13. Keenan JM, Seim HC, Bland CJ, Altemeier TM. A workshop program to train volunteer community preceptors. Academic Medicine 1990; 65: 46-47.
14. Taylor CA, Lipsky PMS. How to 'activate' medical students in the office teaching setting: giving students permission to be activate learners. Family Medicine 2001; 33: 421-423.
15. Hennen BK, Morrissy J, Grinrod A. How an ethics workshop for preceptors affects medical students Canandian Family Physician 1994; 40: 1292-1298.
16. Mills JE, Francis KL, Bonner A. Mentoring, clinical supervision and preceptoring: clarifying the conceptual definitions for Australian rural nurses. A review of the literature. Rural and Remote Health 5: 410. (Online) 2005. Available: http://rrh.org.au (Accessed 22 February 2006).
17. Baldor RA, Brooks WB, Warfield ME, O'Shea K. A survey of primary care physicians' perceptions and needs regarding the precepting of medical students in their offices. Medical Education 2001; 35: 789-795.
18. Grayson MS, Klein M, Lugo J, Visintainer P. Benefits and costs to community-based physicians teaching primary care to medical students. Journal of General Internal Medicine 1998; 13: 485-488.
19. Crouse BJ, Norris TE, Wolff LT. Rural physicians as educators: Why take on another job? American Family Physician 1996; 54: 1457-1460.
20. Walters LS, Worley PS, Prideaux D, Rolfe H, Keaney C. The impact of medical students on rural general practitioner perceptors. Rural and Remote Health 5: 403. (Online) 2005. Available: http://rrh.org.au (Accessed 22 February 2006).
21. Usher K, Nolan C, Reser P, Owens J, Tollefson J. An exploration of the preceptor role: preceptors' perceptions of benefits, rewards, supports and commitment to the preceptor role. Journal of Advanced Nursing 1999; 29: 506-514.
22. Bain L. Preceptorship: a review of the literature. Journal of Advanced Nursing 1996; 24: 104-107.
23. Stone S, Ellers B, Holmes D, Orgren R, Qualters D, Thompson J. Identifying oneself as a teacher: the perceptions of preceptors Medical Education 2002; 36: 180-185.
24. College of Health Disciplines. Preceptor effectiveness. Online (2001) http://www.health-disciplines.ubc.ca/pm/precepting/preceptoreffectiveness.htm. (Accessed 20 April 2005).
25. Charleston R, Happell B. Attempting to accomplish connectedness within the preceptorship experience: The perceptions of mental health nurses. International Journal of Mental Health Nursing 2005; 14: 54-61.
26. Drennan J. An evaluation of the role of the clinical placement coordinator in student nurse support in the clinical area. Journal of Advanced Nursing 2002; 40: 475-483.
27. Yonge O, Krahn H, Trojan L, Reid D, Haase M. Supporting preceptors. Journal for Nurses in Staff Development 2002; 18: 73-79.
28. Quinlivan J, Black K, Peterson RW, Kornman L. Differences in learning objectives during the labour ward clinical attachment between medical students and their midwifery preceptors Medical Education 2003; 37: 913-920.
29. Schultz KW, Kirby J, Delva D, Godwin M, Verma S, Birtwhistle R et al. Medical students' and residents' preferred site characteristics and preceptor behaviours for learning in the ambulatory setting: a cross sectional survey. BMC Medical Education 2004; 4: 12.
30. Dibert C, Goldenberg D. Preceptors' perceptions of benefits, rewards, supports and commitment to the preceptor role. Journal of Advanced Nursing 1995; 21: 1144-1151.
31. Brown K. Rural health professionals: why precept medical students?
32. Patton MQ. Qualitative research and evaluation methods. Thousand Oaks, CA: Sage, 2002.
33. Dillman DA. Mail and internet surveys: the tailored design method. New York: John Wiley & Sons, 2000.





