Introduction
The availability of maternity care in rural areas is changing1,2. Rural maternity units are closing and doctors are withdrawing from obstetrics, forcing more rural women to travel significant distances to deliver their babies. Travelling away from home to deliver a baby has considerable economic and psychosocial costs for the patient, their family and their local community1-4. Nevertheless, at present some women do actively choose to deliver away, even in towns with staff and obstetric services.
Maintaining the viability and availability of obstetric services in rural Australia is a current priority for health-care providers, care planners, educators and policy-makers1,5. Although doctors can maintain obstetric skills with a small caseload6, rising indemnity costs and dwindling numbers affect the economic viability of general practitioners (GPs) providing obstetric care7-9. A decline in the number of private patients in particular will impact on GPs doing only private deliveries7,10. It is therefore important to understand the factors that influence women when choosing obstetric provider. We aimed to gain a better understanding of factors that influence the decision-making of rural women about childbirth provider location.
Methods
Setting
Roma is a provincial centre in south-west Queensland, Australia, approximately 490 km west of Brisbane, with a population of approximately 15 000 living in town or surrounding areas. It has a public hospital with a maternity unit supported by a flying obstetrician and a paediatrician who, although based in Roma, also provides services for other towns. At the time of the study, Roma had one GP-obstetrician doing private deliveries who also supported the hospital doctors with public deliveries.
The Queensland State Health Department perinatal data register recorded 802 women from Roma or surrounding districts (post code 4455) who gave birth from 1995 to 2003; of these, 71% (568) delivered in Roma and 29% (234) delivered elsewhere. However, these data do not include women from neighbouring post code areas who also gave birth in Roma during this time and are, therefore, only an indication of birth activity in the area.
Study design and participants
Participants were recruited through notices in doctors' surgeries, the local hospital, advertisements in the local newspaper and by word of mouth. Twenty-five women volunteered.
We conducted face-to-face, semi-structured interviews with 20 women who had delivered a baby between 1 January 2001 to 31 August 2004, or who were pregnant at the time of the interview, and lived in Roma or surrounding areas at the time of delivery. Interviewing ceased when no new information was forthcoming. Written informed consent was obtained from all participants.
Ethical approval was obtained from the University of Queensland Behavioural and Social Science Ethical Review Committee.
Data collection
An interview guide with open-ended questions and themes was used to prompt the discussion throughout the interviews (Appendix I). It was developed after a comprehensive literature review about health services utilisation, discussions between researchers and conducting a pilot interview to clarify the content and structure of the interview guide.
The interviews lasted up to 60 min and all were done by the principal researcher. The interviews were audio-taped, and notes were taken during and after the interviews to supplement the data.
Data analysis
Recurrent themes were identified in the data by reviewing the recordings and transcripts and reflecting on the field notes. Thematic analysis involved the development of a framework consisting of a number of principal themes divided into sub-categories11. The principal themes were:
- factors that influenced the participant
- factors that could potentially influence the participant in different circumstances
- factors the participant perceived to have influenced other people.
Themes were then analysed by manually grouping the relevant quotes from the transcripts. Both authors independently reviewed a subset of interviews, emergent themes were compared and the final themes reflect consensus by both researchers.
Results
Of the 20 women interviewed, 14 (70%) delivered their babies in Roma, and six (30%) travelled away. These proportions are comparable with the perinatal data. Table 1 presents the range of models of obstetric care used by the participants.
Table 1: Patterns of obstetric care used by participants

A list was compiled of the factors that the women considered influenced their choice of childbirth provider location. Common themes of factors included safety concerns, availability of support, familiar environment, cost, convenience and the people delivering the obstetric services.
Safety
Different women were influenced by a different set of factors; however, all the participants stated that they were influenced by perceived safety. Their own safety, but more importantly the safety of their baby, was paramount for all participants. Anything that influenced the actual or perceived safety of the obstetric service or facility had the potential to influence participants' decision-making. The requirements for safety varied among individuals, depending on their susceptibility to threat, their risk tolerance and their personal characteristics.
Women with a low risk tolerance were more likely to deliver elsewhere, as one said: 'I would never forgive myself if I lost a baby purely because I was out here'. Medical complications or increased health risk also lowered participants' tolerance of risk. Participants who had delivered in Roma previously and had had an adverse experience resulting in feelings of vulnerability, were also likely to travel away from town to deliver.
Participants with a medical background or employment at the local hospital tended not to deliver in Roma. Their decision was influenced by their increased knowledge of both the risks associated with labour and the limitations of the local obstetric services. Privacy and confidentiality issues also influenced these women to travel away.
Participants who delivered in Roma commented that they believed that their needs would be met by the local service, particularly following a medically uneventful pregnancy: 'I felt that because I had a normal pregnancy I wouldn't need backup'.
Support
Once the participants felt their own safety and the safety of their baby was assured, the availability of family support before, during and after the confinement was a very important influence on their choice of childbirth provider location. The participants were more likely to deliver where their partner could attend the birth, and where they had additional family support.
Familiarity of environment
Familiarity with their doctor, the maternity unit and staff as well as the town influenced the participants' decision-making, with most participants choosing the familiar environment to deliver. For the majority of participants who delivered locally, a good doctor-patient relationship was either an influencing factor or a benefit of their decision: 'it's very private having a baby, I needed to know the doctor'. However, one participant who was new in town chose to deliver away with the doctor she knew before coming to town.
Familiarity was a positive influencer for most participants. However, familiarity of the local community influenced some women to travel away from Roma to deliver their baby. A few participants reported concerns about the potential lack of privacy and confidentiality associated with delivering in their local community. One participant recounted that a friend had relayed an anecdote about a woman who had delivered in Roma and had allegedly 'made a fuss' during the birth. The participant realised that the anecdote was about her own experience. A professional and personal relationship with the doctor influenced one participant to deliver elsewhere.
Nevertheless, all the participants, including those who delivered elsewhere, considered it important to have the choice to deliver locally.
Cost
The financial status of the participants' families impacted on their choice, however safety considerations over-rode affordability. For example, one participant reported being willing to endure financial hardship to travel elsewhere to deliver her baby because of safety concerns.
Possession of private health insurance did not appear to strongly influence where a woman would deliver her baby. One participant with private health insurance delivered publicly in Roma because of convenience and a perceived lack of additional benefits for private patients at the hospital. One participant without private health insurance delivered privately in Roma while another delivered elsewhere because they could afford it, even without private health cover.
Convenience
All participants agreed that, logistically, it was much easier to stay in Roma to deliver their baby. Travelling elsewhere to deliver a baby is inconvenient. There are natural risks of animals on the roads, floods or damaged roads, medical risks of travelling shortly before and after labour, and the discomfort of travelling with a newborn baby and possibly other children. These inconveniences were sufficient to influence some of the participants to deliver in town, as long as they felt their safety needs would be met. For those who decided to travel elsewhere, the inconvenience was not an influencing factor, but rather a disadvantage of their choice.
People
The staff involved in the care of a woman during her confinement impacted on her experience and appeared to influence her future choices. Good communication with both doctor and midwife contributed to a positive birthing experience and, conversely, poor communication negatively impacted on the experience. One participant reported difficulties communicating with a doctor for whom English was a second language: 'I wasn't sure I made myself understood'.
Some participants reported being attended by doctors who they perceived to have a lack of medical skills and experience, and that this had negatively impacted on their birthing experience. However, this did not necessarily impact on choice of childbirth provider location for their next baby.
Midwives also had a significant impact on the birthing experience and, consequently, on future delivery choices. Most participants spoke very positively about their experiences with the midwives, stating that 'most midwives were wonderful' and that 'they treat you more like a person [in Roma] and not like a number'. However a few participants reported negative experiences, commenting that 'I didn't ring for assistance when she [the midwife] was on; I waited until the next shift'. One participant commented that she would deliver in Roma again on the proviso that she was not in the care of a particular midwife. Midwives who appeared unsympathetic, or who lacked empathy may have a bigger impact than a doctor on future choices about where to deliver. This is possibly because the relationship between the woman and midwife is for a longer duration and is potentially more personal.
Other factors
Other factors that influenced the participants' choice about delivering in Roma included:
- loyalty to the local services - a few participants reported a belief that the town was in danger of losing its obstetric services if it was not adequately utilised
- a belief that a local delivery would result in enhanced continuity of care through the antenatal, delivery and postnatal phases
- family tradition and expectations - one participant reported that she and her siblings had all been born in the local hospital, her sisters had delivered locally, and that it was expected she would deliver there too
- rural background of the mother
- ownership of a local business or self-employment - for several participants, owning a small business or being self-employed meant that it was impossible to choose to leave town for the delivery
- school age children - the disruption to their schooling if they are taken out of school for a period to travel away for the confinement.
Other factors influencing participants to travel away from Roma to deliver their baby included:
- a referral by their doctor
- better facilities for private patients, eg ensuite bathrooms
- status of facility, for example one participant expressed concern that there could be a social stigma attached to having Roma as the place of birth on the child's birth certificate.
Discussion
The aim of this study was to obtain a broad view on as many factors as possible that played a role in the decision-making process that affects utilisation patterns. It was not the aim to determine which factors were more important than others. A broader study across a wider population would be needed to investigate the impact of each factor on the final decision in relation to locality of child birth. However, our results suggest that some factors are more important than others. All women mentioned safety, even though it resulted in a different utilisation pattern for each individual. A Canadian study looking at the effect of geographical location of the obstetric care provider on parturient women9, using Maslow's hierarchy of needs to analyse the data, showed similar results.
Safety is a basic need, and according to Maslow's hierarchy of needs, is a primary motivator for human behaviour. Failure to satisfy this need has been demonstrated to have negative consequences on the birthing experience9. Participants' assessment of safety needs were personal judgements, based on a combination of influences such as health risk to self and baby, past experiences and risk tolerance.
The results of this study are consistent with Poole et al's model (Figure 1) suggesting that personal characteristics (socio-demographics, knowledge and attitudes) predispose an individual to decide to deliver locally or away12. For example, a woman who has a low risk tolerance, and who feels particularly fearful and vulnerable about giving birth, is more likely to travel away to a health service that meets those needs.
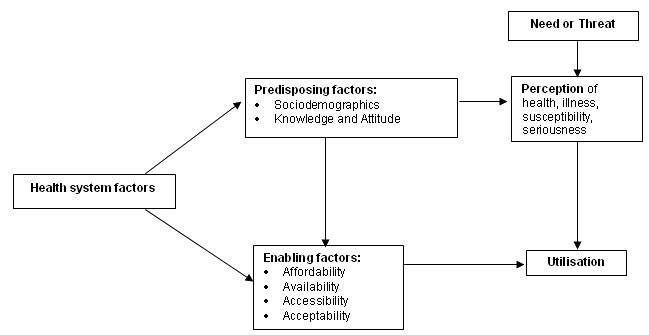
Figure 1: A model of health care utilisation. Adapted from: Poole and Carlton, reference 12.
The decision about where to deliver a baby is also strongly influenced by the potential impact of the decision: the affordability, availability, accessibility and acceptability of the decision12. Issues such as cost and the economic status of the family dictate whether the preferred option is affordable. Factors influencing choice are only relevant if choice is available. Accessibility relates to the ability of the women to reach the health service at the appropriate time. It was also important that her partner, family and friends were able to access the chosen facility. Finally, the choice has to be acceptable to all involved, including the woman's GP and community.
Also impacting on the woman's choice are health system factors12. A health service facility that is perceived to be, or actually is, unable to provide and support the services necessary to ensure the safety of both the mother and baby, may influence the woman to choose another facility against her preference (eg travel away from her own community to deliver her baby).
Limitations
Some caution is needed when interpreting these results. Participants self-selected and, therefore, may not be representative of all rural women who have to choose childbirth provider location. In addition, one researcher and her partner were GPs in Roma and had provided medical care to some of the study participants. This could have impacted on the interview responses. The risk of such social desirability bias is a reality for practitioner-researchers working in isolated rural communities in Australia. However, the rigorous standards of qualitative research were applied, in particular the analysis of the data involved two independent researchers in order to identify and account for potentially biased accounts.
Conclusion
The literature suggests that access to medical services locally improve health outcomes2,13. Local demand and utilisation are of utmost importance to ensure viability of rural health services9,10. Changing utilisation patterns starts with an increased understanding of the moderators of choice. This study highlights the pivotal importance of safety considerations on women's decision-making about where to deliver their babies. Measures to increase the number of deliveries in rural towns must address actual and perceived safety issues to be successful and to prevent further withdrawal of rural obstetric services.
Acknowledgements
The study was performed as part of a Novice Researcher Fellowship awarded by the Centre for General Practice at The University of Queensland, through the Primary Health Care Research Evaluation and Development (PHC-RED) Strategy, an initiative of the Australian Government Department of Health and Ageing. We thank the women of Roma who participated in this study and told us their stories. Without their involvement, this study would not have been possible. We gratefully acknowledge Dr Pierre Smith for posing the question, Associate Professor Geoff Mitchell, Research Facilitator PHC-RED University of Queensland, for his valuable comments on the project and Professor Moyez Jiwa for his input into this article.
References
1. Stratigos S, Nichols A. Procedural rural medicine: Strategies towards solutions [Discussion paper]. (Online) 2002. Available: http://rdaa.com.au/uploaded_documents/ACF3B35.pdf (Accessed 1 June 2004).
2. Peck J, Alexander K. Maternal, infant, and child health in rural areas: a literature review. Rural Healthy People 2010: A companion document to Healthy People 2010. Volume 2. College Station, TX: The Texas A&M University System Health Science Center, School of Rural Public Health, Southwest Rural Health Research Center, 2003.
3. Marshall BS, Javalgi RG, Gombeski WR Jr. Providing services to obstetrical patients: an overview and implications. Health Marketing Quarterly 1995; 13(2): 63-78.
4. Kornelsen J, Grzybowski S. Safety and community: the maternity care needs of rural parturient women. Journal of Obstetrics and Gynaecology Canada 2005; 27: 247-254.
5. Morgan TJ, Turner LW, Savitz LA. Factors influencing obstetrical care selection. American Journal of Health Studies 1999; 15: 100-106.
6. Jackson WD, Diamond MR. Procedural medicine. Is your number up? Australian Family Physician 1993; 22: 1633-1636, 1639.
7. Cameron B, Cameron S. Outcomes in rural obstetrics, Atherton Hospital 1991-2000. The Australian Journal of Rural Health 2001; 9(Suppl 1): S39-S42.
8. Bronstein JM, Morrisey MA. Bypassing rural hospitals for obstetrics care. Journal of Health Politics, Policy and Law 1991; 16: 87-118.
9. Jones JA, Humphreys JS, Adena MA. Doctors' perspectives on the viability of rural practice. Rural Remote Health 4: 305. (Online) 2004. Available: http://rrh.org.au (Accessed 22 August 2006).
10. Australian College of Rural and Remote Medicine. Research reports on: Barriers to the maintenance of procedural skills in rural and remote medicine & Factors influencing the relocation of rural proceduralists. Brisbane: ACRRM, 2002.
11. Pope C, Ziebland S, Mays N. Qualitative research in health care. Analysing qualitative data. BMJ 2000; 320(7227): 114-116.
12. Poole DL, Carlton TO. A model for analyzing utilization of maternal and child health services. Health and Social Work 1986; 11: 209-222.
13. Nesbitt TS, Connell FA, Hart LG, Rosenblatt RA. Access to obstetric care in rural areas: effect on birth outcomes. American Journal of Public Health 1990; 80: 814-818.


