Introduction
In 2000-2001 the Australian Commonwealth Department of Health and Ageing provided significant funding to Australian medical schools to develop a national network of 10 Rural Clinical Schools1. The Rural Clinical Schools have provided an opportunity for medical students to undertake their clinical training across a network of hospitals, general practice surgeries and community medical centres in rural/regional locations throughout Australia. The primary goal of this national program is to improve rural medical practitioner workforce recruitment and retention. A key funding parameter was the requirement for a minimum of 25% of medical students within each relevant medical school to undertake 50% of their clinical training in a Rural Clinical School as from January 20041.
Background
In response to the Rural Clinical School initiative, the Rural Clinical School at the University of Queensland (UQ) was established in 2002, as the Rural Clinical Division (RCD) of the School of Medicine. The MB BS (Bachelor of Medicine, Bachelor of Surgery) at the School of Medicine provides a four-year program in which students undertake clinical training in years three and four. Students may elect to train in one of three clinical divisions, namely central, southern (both based in Brisbane), or rural (RCD). The RCD consists of four main teaching sites within south west and central Queensland. These are located at Toowoomba, Hervey Bay-Maryborough, Rockhampton and Bundaberg. In order to provide anonymity to these hospitals, they are hereafter referred to as Hospitals A, B, C, or D (in no particular order). Training must be of an equivalent nature throughout all three clinical divisions because all students are subject to identical assessment processes. On commencement in 2002, the RCD enrolled eight 3rd year and one 4th year student based at Hospital A, and eleven 3rd year plus eight 4th year students located at Hospital B. This has now risen to a total of just over 100 fulltime students across a total of four training sites for 2006. In 2004, all four sites were oversubscribed, with 91 applications for an initial 65 places. The increasing student demand for UQ RCD places is exemplified by an approximate doubling of applications for 2005 third-year places, as compared with 2004.
Rigorous evaluation of the RCD teaching program underpins the goals of continuing improvement of both education and resources, and is also a key component of the reporting mechanisms linked to ongoing Commonwealth funding. A positive educational and clinical experience has been shown to have a positive influence on rural career choice2-7.Therefore students' perception of their medical education at the RCD is the major focus of such evaluations, in order to assist both educational improvement and required student recruitment8. The provision of a positive medical education experience in a Rural Clinical School is also an avenue through which associated regional hospitals could directly recruit their interns and junior doctors. With these issues in mind, a questionnaire, the 'Year 4 Exit Survey', was developed to evaluate medical student perceptions of their 4th year experience at the RCD, coupled with an analysis of their internship choices. This article is based on preliminary results from a longitudinal study that aims to explore the ways in which Rural Clinical Schools can better prepare students for rural practice and provide for their transition into rural internship.
Methods
Ethical clearance
Ethical clearance for this project was obtained through the UQ Behavioural and Social Science Ethical Review Committee.
Setting
All year 4 students were based at the UQ RCD at either Hospital A or Hospital B.
Questionnaire - the Year 4 Exit Survey
The questionnaire was initially developed and piloted with both outgoing 3rd and 4th year MB BS students at Hospital B in 2004. The pilot results assisted in further refinement of the questionnaire and it was both shortened and re-worded for clarity.
The final version of the exit survey contained 63 questions and was a combination of open-ended and forced-answer items which asked students to rate both their agreement/disagreement with or place a value rating on statements. A space for comments was provided after all questions to elicit further explanation for their responses.
The survey was divided into several sections, these were:
- demographics
- career interests
- experience of rural living
- interest in rural medical practice
- perceptions of rural communities
- perceptions of the RCD
- ratings of their medical training
- the impact of the RCD on their desire to practice medicine in a rural area
- their opinions on the most and least valuable study experiences
- their suggestions on how that experience might be improved.
A final question asked them their choice of internship location and the reasons why they were or were not staying at their present RCD site for internship.
Data collection and analysis
The questionnaire was administered to all year 4 students at both locations during their last week of term in a classroom setting, that is, they completed and handed back the questionnaire to the administrator at that time.
Quantitative data were entered into SPSS (SPSS Inc; Chicago, IL, USA) and analysed for descriptive and frequency statistics. Independent t-tests and c2 tests were used to measure the level of association between variables. Free response comments were collated by question, analysed for dominant themes and reported as frequency data.
Results
The number of participants was too small to detect any differences in evaluation responses between sites, by gender or by age group. Therefore, all results are presented in aggregate form, with the exception of intern choice.
Demographics
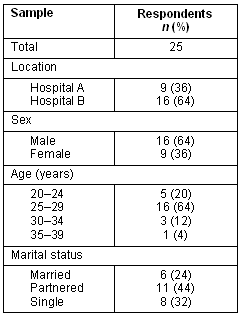
Table 1 presents the demographics of the sample. A total of 26 students completed their 4th year training at the RCD in either the Hospital A (10 students) or Hospital B (16 students). The sample size equals 25 because one questionnaire from Hospital A was not completed. The majority were male (64%), were within the 25 to 29 year age group (64%) and were married or partnered (68%). The most prevalent spouse/partner occupation was medical student (24%) followed by teacher and doctor. Forty-eight percent attended UQ for their first degree.
Table 1: Student demographics
Experience of living in a rural area
For purposes of this questionnaire, 'rural area' was described as communities of RRMA 4-79. An equal number of students were either born and/or raised in a rural area, that is, lived there for more than 15 years (37.5%) or had never lived in a rural area (37.5%). Only 25% of their spouses/partners had been born and raised rurally, with the majority (44%) never living in a rural area. The majority (52%) of students would consider living and working in a large rural centre (population of approximately 100 000). Only 26% chose a more remote rural centre (population less than 10 000) to live or work in. Approximately half (44%) of the students felt they would work in a rural or remote area sometime within 4 to 6 years after graduation with 35% feeling they might go out within one to 3 years and 22% were not sure. When asked how long they might stay working in a rural and remote area, 35% were not sure at this stage but an almost equal number (31%) felt they would stay indefinitely.
Perceptions of rural and remote
The students were asked several questions pertaining to their perceptions of rural and remote medicine and communities. Responses represented their agreement or disagreement to a corresponding statement on a Likert scale from 1 = strongly disagree, to 5 = strongly agree, therefore the higher the mean value (number in parentheses) the higher their agreement (Table 2).
These results indicate that most students have a strong interest in practising medicine in a rural or remote area (4.00) but that interest (3.35) only moderately influenced their decision to come to the RCD to study. Students were in high agreement (4.08) that qualifying as a rural or remote community is more about location (distance from larger centres) than about the size of its population, and they don't consider sites like Hospital A or Hospital B to be rural (2.96).
Table 2: Students' perceptions of rural and remote

Perceptions of medical education
Students were also asked to rate several aspects of their medical education at the RCD. Ratings were on a scale from 1 = very poor, to 5 = very good, therefore the higher the mean value (number in parentheses) the higher the rating.
Students rated their overall clinical training (4.17) and quality of teaching (4.45) highly. The effectiveness of consultants, doctors and residents with respect to formal teaching (4.21) and clinical guidance (4.46) were also rated highly. The effectiveness of health-care professionals (nurses, therapists etc) with respect to formal teaching (3.54) and clinical guidance (3.75) were rated slightly lower as was the Multi-professional Education Program (MPE) with the allied health staff (3.13). The usefulness of the library was rated (4.42) very good while the computer IT resources were rated slightly lower (3.83).
The final three questions also asked students to rate the quality of: the (i) teaching; (ii) the opportunities to practice; and (iii) the quality and quantity of feedback they received over the year with specific reference in each case to:
- history taking
- interview skills
- treatment/management plans
- clinical reasoning skills
- patient skills
- communication skills
- procedural skills.
Teaching: With regard to teaching, the highest rated were clinical reasoning skills (4.66) and communication skills (4.50) with all other elements receiving ratings of 4.0 or above.
Practice: With regard to opportunities to practice, the highest rated were again clinical reasoning skills (4.63) and communication skills (4.62) with all other elements receiving a rating of 4.13 or above. Only procedural skills was rated lower (3.92).
Feedback: Overall ratings on the quality and quantity of feedback received were slightly lower. The highest rated were clinical reasoning skills (4.17) and patient skills (4.04) followed by history taking and interview skills each rated (3.79).
Impact of the rural clinical division on desire to pursue rural medicine
A separate question asked students how their time at the RCD altered (either encouraged or discouraged) their desire to pursue a medical career in a rural or remote location. The mean response to this question on a scale of -5 to -1 (discouraged) to +1 to +5 (encouraged), with a mid-point of zero (nil effect), was +3.04 (SD = 1.58). Broken down, this showed that 20.8% of the students gave the question the highest rating at +5, 29.2% rated it at +4 and 33.3% rated it at +2. Only one student gave a minus rating of -3.
Reasons for choosing the rural clinical division
Students were asked to state in two sentences why they chose to come to the RCD at either Hospital A or Hospital B. All 25 students provided 34 comments which focused on six individual themes. Table 3 lists these themes and the number of times each was noted by the students. Teaching, the smaller nature of the RCD, and its associated learning environment were noted most often.
Table 3: State in two sentences (maximum) why you chose to come to the RCD?

Most valuable
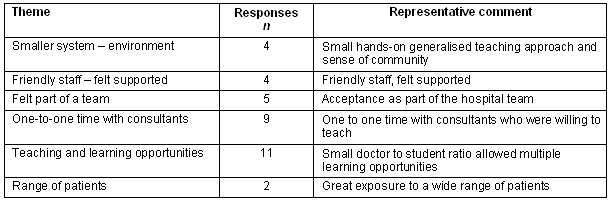
Students' comments regarding what they found most valuable about their study experience at the RCD are shown (Table 4). A total of 18 students offered 35 comments that focussed on seven themes reflecting teaching and learning opportunities and the smaller environment, more one-to-one time with consultants and exposure to a greater range of patients. Friendly staff, feeling supported and part of a team were also noted.
Table 4: What did you find most valuable about your study experiences at the rural clinical division?
Least valuable
Only eight students offered 11 comments with regard to what they considered least valuable about their study experiences at the RCD. Five of these had to do with administrative issues, such as accommodation or paperwork/teaching materials. Three comments reflected dissatisfaction with specific rotations and three stated 'nothing'.
Internship choice
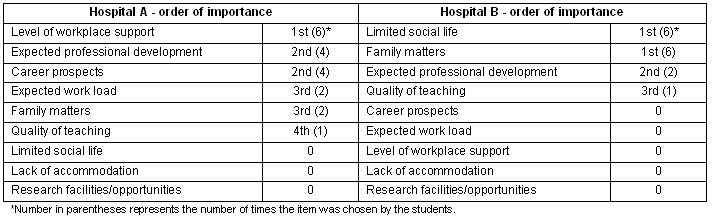
Six of the 26 students elected to stay at their respective rural teaching hospitals to begin internship training (one of 10 from Hospital A, and five of 16 from Hospital B). Students were asked to list the most important reasons for making this decision, in order of importance. These answers are provided (Table 5). The most important reasons for leaving Hospital B involved 'family matters' and 'social life'. In contrast, reasons cited for leaving Hospital A were inadequate 'level of workplace support', 'expected professional development' and 'career prospects'.
Two of these six students also provided reasons for deciding to stay for their internship. These were 'expected professional development' and 'level of workplace support'.
Table 5: Reasons for not staying in either Hospital A or Hospital B for internship
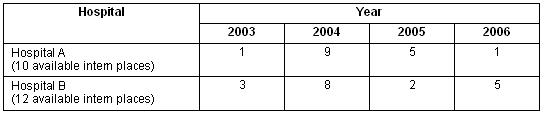
An evaluation of internship choice from initial rural clinical school graduate placements in 2004 to current 2006 appointments indicates that the number of RCD medical students choosing to undertake internships at Hospital A has dropped from a maximum of nine in 2004, to one in 2006, and at Hospital B from eight in 2004, to five in 2006 (Table 6). The increasing popularity of rural undergraduate clinical training has, therefore, not been matched by intern placement choices regarding either of the participating rural teaching hospitals.
Table 6: Number of locally trained year 4 medical graduates choosing internships at their rural clinical training site
Discussion
The results (frequency data and student comments) of the Year 4 Exit Survey suggest high levels of student satisfaction with the undergraduate program at Hospitals A and B.
One of the assumptions of the Rural Clinical Schools is that they attract a large proportion of students with a rural background and/or an interest in future rural practice. Approximately 50% of our year 4 student sample, and over 60% of their spouse or partners had no rural background, yet they chose to study at the RCD. This was an interesting finding in view of the considerable amount of rural workforce literature supporting a strong direct relationship between rural origin or exposure and choice of future practice location10-14. A rural educational experience has been reported to increase students' favourable attitudes toward rural affiliations15 and choosing a rural focus for the final year of study has been shown to be a predictor of graduates' selection of a rural practice16. Above all, the perceived quality of the rural educational experience is associated with an increased interest in a rural career5.
Without seeking in any way to diminish the major importance of such previous findings, it was apparent from our own data that the RCD is providing an important opportunity for students of both urban and rural background to gain experience and exposure to rural life, and to undertake 4th year clinical training with a rural focus. The unexpected popularity of the rural training program among medical students of non-rural background is felt to be an important finding in terms of potential future rural medical workforce improvements, and is of major research interest.
Providing this positive clinical training experience and a chance to discover what rural medicine is all about within a supportive educational environment is vital in nurturing a desire to pursue rural medical practice. The smaller size of Rural Clinical Schools in general may be a key factor here and several comments by the students support this concept. Perhaps this smaller learning environment is also conducive to providing a higher degree of pastoral care, another positive factor exemplified within Rural Clinical Schools.
The student's perceptions of what rural and remote meant to them were inconclusive. Questions in relation to future practise in a rural area showed that over half would consider working in a large rural centre (similar in size to Hospitals A and B) even though they didn't consider either site to be rural. Nevertheless, approximately half the students said they would consider working in a rural area within 4 to 6 years of graduation. Interestingly, an almost equal number of students were either not sure or indicated they would stay in a rural area indefinitely. These results suggest that by the end of their 4th year, most students are unclear as to their future career path.
Over 80% of the students felt their time at the RCD encouraged their desire to pursue a rural or remote medical career. This is encouraging and suggests that the RCD is providing a positive educational experience, which is said to be a predictor of graduates' selection of rural medical practice15,16.
Looking finally at internship choice, we see both a low number of students taking up internships at their respective training hospitals, particularly at Hospital A, and a different set of reasons pertaining to the two sites. Given there were no significant differences in undergraduate medical education experiences, and that these were very positive, other factors influencing these decisions needed to be identified.
Important differences emerge when the intern placement choices are examined. Although both sites have lost popularity since attaining a peak in 20046, Hospital B is recovering whilst Hospital A continues to decline. The reasons why rural medical graduates stayed or left were documented and, while it is understandable and even commonplace for students to change location based on personal reasons, their citing of an 'unsupportive workplace environment' and 'inadequate professional development opportunities' as major reasons for leaving are of concern.
This finding indicates the need for teaching hospitals to work collaboratively with Rural Clinical Schools as true partners in both medical education and local recruitment strategies and to value this relationship as an integral component of, and contributor to, regional health service delivery.
This finding also deserves further discussion regarding strategies to improve recruitment into local regional and rural hospitals. Although we did not see a high percentage of our graduates choose internships in the local hospitals, internship choice is not the only, or it could be argued, the most important outcome of the Rural Clinical Schools initiative. The ultimate goal of the Rural Clinical Schools' initiative is to increase the number of rural medical practitioners in the workforce1. This is a long term goal, but a crucial component of the initiative is to raise awareness and encourage a desire to 'go rural' at some point in their career.
A final point highlights what could be done to provide graduates with more internship options in order to make local and regional hospitals more attractive. For example, plans to enter a specific speciality may be important to some students at this stage. Is the relative lack of specialisation or subspecialisation available in rural hospitals affecting internship choice? Should Rural Clinical Schools also include a focus on how they might make internships more relevant to individual specialties? Consideration of strategies to address these issues may also improve the viability of rural and regional hospitals by retaining specialty services and doctors to provide those services.
Limitations
There are many limitations to this study that will eventually be addressed as subsequent cohort data are collected. However these results represent a small number of students from one cohort in one university in Australia. More data is needed regarding reasons for internship choice so that better collaboration between Rural Clinical Schools and their regional hospitals can be achieved. The factors that constitute a 'positive impact' on students need to be teased out so they may be replicable across successive cohorts of students. The tracking of graduates' career paths and the longitudinal nature of this process will address some of these issues and allow us to monitor and improve our program over the subsequent years.
Conclusion
These preliminary results have shown that a quality undergraduate rural medical education does not guarantee immediate transition to rural internship. The literature suggests that there is a high return of rural experience students who eventually practice rural medicine but longitudinal studies are required to determine when and to what degree this occurs. Studies are also needed to look more closely at the transition period between graduate and intern. This important transition period could be an ideal opportunity for local workforce partnerships to attract students' interest in rural medicine. Research is needed to determine gaps in these partnerships in order to provide a variety of rural options and resources to new interns.
Acknowledgements
The authors acknowledge Kerry Kruger and Kaye Lasserre of the Rural Clinical Division SWQ region who assisted in the early stages of this project.
References
1. Australian Government Department of Health and Ageing. Workforce Education and Training - Rural Clinical Schools (online) April 2002 Available: http://www.health.gov.au/clinicalschools (Accessed 3 November 2005).
2. Bushy A, Leipert B. Factors that influence students in choosing rural nursing practice: a pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: http://rrh.org.au (Accessed 3 November 2005).
3. Denz-Penhey H, Murdoch C, Lockyer-Stevens V. What makes it really good, makes it really bad. An exploration of early student experience in the first cohort of the Rural Clinical School in the University of Western Australia. Rural and Remote Health 4: 300. (Online) 2004. Available: http://rrh.org.au (Accessed 3 November 2005).
4. Igumbor EU, Kwizera EN. The positive impact of rural medical schools on rural intern choices. Rural and Remote Health; 5: 417. (Online) 2005. Available: http://rrh.org.au (Accessed 3 November 2005).
5. Shannon CK, Baker H, Jackson J, Roy A, Heady H, Gunel E. Evaluation of a required state-wide interdisciplinary rural health education program: student attitudes, career intents and perceived quality. Education for Health 2005; 18: 395-404.
6. Wilkinson D, Birk J, Davies L, Margolis S, Baker P. Preliminary evidence from Queensland that rural clinical schools have a positive impact on rural intern choices. Rural and Remote Health 4: 340. (Online) 2004. Available: http://rrh.org.au (Accessed 3 November 2005).
7. Zorzi A, Rourke J, Kennard M, Peterson ME, Miller KJ. Combined research and clinical learning make rural summer studentship program a successful model. Education for Health 2005; 18: 329-337.
8. De Witt DE, McLean R, Newbury J, Shannon D, Critchley J. Development of a common national questionnaire to evaluate student perceptions about the Australian Rural Clinical Schools Program. Rural and Remote Health 5: 486. (Online) 2005. Available http://rrh.org.au (Accessed 13 December 2005).
9. Australian Medical Workforce Advisory Committee (AMWAC). Doctors in vocational training: rural background and rural practice intentions. Australian Journal of Rural Health 2005; 13: 14-20.
10. Australian Rural and Remote Workforce Agencies Group. Review of the Rural and Remote Metropolitan Areas Classification System. (Online) 2005. Available www.arrwag.com.au (Accessed 13 November 2005).
11. Dunbabin J, Levit L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available from http://rrh.org.au (Accessed 3 November 2005).
12. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11: 277-284.
13. Wilkinson D. Evidence-based rural workforce policy: an enduring challenge. Rural and Remote Health 3: 224. (Online) 2003. Available http://rrh.org.au (Accessed 3 November 2005).
14. Wilkinson D, Beilby JJ, Thompson DJ, Laven GA, Chamberlain L, Laurence COM. Associations between rural background and where South Australian general practitioners work. Medical Journal of Australia 2000; 173: 137-140.
15. Woloschuck W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36: 241-247.
16. Rabinowitz HK, Diamond JJ, Marham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. Journal of American Medical Association 2001; 286: 1041-1048.

