Introduction
Australian adults have a prevalence rate of asthma of 10-12% which is one of the highest in the world1. In addition, hospitalization rates are highest among Aboriginal and Torres Strait Islanders and in rural and remote areas1. Evidence-based guidelines for asthma2,3 exist and form the basis of New South Wales (NSW) Health's guidelines for the management of acute asthma. Despite this there is evidence that these guidelines are not always followed4. Developing guidelines is an important component in summarizing evidence from research, but unless there is a successful implementation process, the translation of this knowledge into clinical practice will not necessarily occur. Translating evidence into clinical practice is difficult5 and remains a major barrier to improving health6. There is an increasing knowledge base about what implementation strategies are most effective, and some researchers have questioned whether evidence-based implementation (EBI) of evidence-based guidelines is possible7.
Increasingly, there has been a focus on equity of access and quality of health care in the rural environment8. Some advocate that small rural hospitals should become centres of quality health care and training9. In the vast majority of cases of asthma, and many other emergency department (ED) presentations, the achievement of best practice does not require access to the additional resources usually only found in large metropolitan hospitals. Therefore, best practice for the majority of asthma presentations is achievable in even the smallest rural hospital. There is evidence too that, despite barriers, rural GPs view EBM positively10 and support a regional approach to asthma management based on National Asthma Council (NAC) guidelines11.
With regard to the implementation of best practice, there is little evidence to indicate what strategies are most likely to be beneficial in rural district hospitals in Australia, let alone rural district emergency departments (ED). This article will report the results of an EBI, adapted from an implementation strategy at a rural referral hospital, designed to improve ED assessment and management of acute asthma in adults.
The aim of this study was to determine if an evidence-based approach to implementation of asthma guidelines would translate into improved compliance with evidence-based care for acute asthma in adults in a number of small, rural district ED.
The lead author was an emergency physician working clinically within the Area Health Service that the study and control hospitals are in, and has for many years performed retrievals, provided advice and been involved in accepting the transfer of patients from these hospitals.
Methods
A pre-intervention audit of asthma management (assessment and treatment) was conducted in eight rural district hospitals. Audit was performed by the author for three hospitals in each group and by senior nurses, trained in the use of the data collection form, at the other two hospitals. From these audits evidence-practice gaps (EPG) were identified. All identified patients aged 14 and over were included. Audit data was entered into a de-identified data-base.
Pairs of hospitals were matched based on size, and one randomly allocated to the study group with the other serving as a control. The sample size required to detect a 30% improvement in compliance with a clinical indicator, with a level of significance of <0.05 and a power of 0.9 was 56 patients. Based on estimates of attendances with asthma for these hospitals, 7 months of pre-intervention data were collected from 1 January to 31 July 2004 and 7 months of post-intervention data were collected from 1 October 2004 to 30 April 2005. The intervention at the four study hospitals occurred between August and September 2004.
The study hospitals were subjected to an EBI outlined below. The control hospitals had no additional intervention to help implement established guidelines for asthma. The National Asthma Council and Respiratory Therapeutic Guidelines2,3 have been available for years and form the basis of the NSW Health guidelines, which have been disseminated to hospitals throughout NSW. Dissemination of guidelines without a dedicated implementation plan is a common method used by health departments to transfer knowledge to clinicians.
All eight hospitals were staffed by GP visiting medical officers (VMOs) with no dedicated on-site medical staff. Each of the ED registered between 2000 and 8000 patients per year, although the data collection systems do not allow differentiation between ED presentations and outpatient visits. The ED were staffed by nurses who also had to fulfill other duties throughout the hospital and, hence, were not full-time ED nurses. The eight towns were situated between 50 km and 200 km from the nearest base referral hospital and serviced populations between 1000 and 14 000 people12. All towns had a rural, remote and metropolitan area (RRMA) rating of 5.
There was no standard ED data collection system across the eight hospitals. Admitted patients were identified by ICD9 coding. Non-admitted patients were identified by a manual search of the hand-written ED attendance register. Documented attendances for 'asthma', 'wheeze', 'short of breath' and similar phrases were reviewed. Only those patients with an ED diagnosis of asthma were included in the database. Data for all patients identified were included in the study. Data for an individual clinical indicator (eg the prescribing of corticosteroids) were excluded if the patient was already on the treatment prior to presenting to the ED.
When assessment of severity was not documented, the reviewer made an assessment of severity based on the clinical record and in consultation with the features of severity outlined in the NAC asthma management handbook2. Any one feature of moderate severity led to classification as moderate, and any one feature of severe led to classification as severe. The only caveat was if the only feature was pulse rate, the reviewer had to make a decision based on the degree of tachycardia, amount of previous ventolin use and any other factor which may have influenced pulse rate.
Data for all indicators in both the study and control hospitals were subject to c2
While this was primarily a quality improvement process, it did involve accessing and reviewing patient records at other public hospitals and, hence, ethics approval was sought and gained from the New England Area Health Service (NEAHS) ethics committee.
An evidence-based approach to implementation was devised and this has been extensively detailed in a previous article13. The main points of this implementation, including variations to suit the rural district environment, involved as follows.
Identifying evidence-practice gaps
An initial audit identified areas where ED practice deviated from evidence-based recommendations. These EPG were discussed with medical, nursing and administrative staff at the study hospitals to determine which areas to attempt to address. The areas identified are listed in the Results section.
Identifying barriers
Identifying barriers to change at the level of the patient, individual doctor or nurse, the ED team and the organization and processes within the ED. These were identified at each study hospital. Barriers were different from those identified at a rural referral12 hospital and the specific differences and reasons for changes to the implementation strategy are discussed in more detail in the Discussion.
Guideline development
Re-formatting of the NAC guidelines for acute asthma into a simple, usable format, consisting of a single-sided A4 tick-box guideline. The guideline became part of the medical record and was commenced at triage. Clinicians at each hospital could comment and recommend variations to the guideline, based on local issues.
Reminders
By being incorporated into the medical record, the guideline itself served as a reminder. During the implementation and follow-up phase, the author visited each study hospital on two occasions to talk to nursing staff and once to talk to medical staff. A senior nurse at each hospital was also encouraged to remind staff about the guidelines.
Education
Education sessions were arranged with medical and nursing staff at the time of implementation, focusing on barriers to change, evidence for asthma management and the guideline itself. As part of the implementation, all the doctors were sent pre-written material of two draft papers, subsequently published14,15, on the history of and arguments for and against evidence-based practice.
Audit and feedback
Presentations for acute asthma at any individual hospital was low and, hence, auditing only occurred once or twice at each hospital during the seven-month follow-up period. Given this, audit and feedback was not used as a strategy.
Implementation team
A specific implementation team at each hospital was not possible due to staffing levels. Most contact between the author and the study hospitals was via one senior clinical nurse at each hospital.
Results
Evidence-practice gaps
Six EPG were identified and targeted for change. These were:
- lack of formal documentation of severity (mild, moderate or severe) in the clinical record
- low rates of spirometry for the assessment of acute attacks
- over use of ipratropium for mild asthma
- Under utilization of systemic corticosteroids
- low utilization of written short-term asthma management plans (STAMP)
- over-use of antibiotics for acute asthma.
Total presentations
For the study hospitals there were 51 patients in the pre-intervention phase and 47 in the post-intervention phase. For the control hospitals, the numbers of presentations were 47 and 42, respectively. At the study hospitals, to detect a change in compliance of 30% with a level of significance of <0.05, this sample size gives a power of 0.84. The grading of severity is shown (Table 1).
Table 1: Assessment of asthma severity
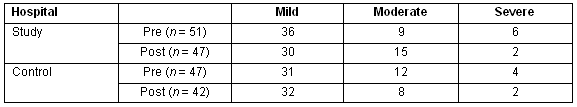
Given the low number of presentations with severe asthma, statistical analysis of assessment of severity compared mild asthma with moderate-severe combined. From the pre- to post-intervention period, there was no significant change in the rate of mild versus moderate-severe asthma in the study hospitals (p = 0.5, c2 = 0.5, 1 degree of freedom) or in the control hospitals (p = 0.3, c2= 1.1, 1 degree of freedom).
Table 2 shows the pre- and post-data for both the study and control hospitals for the six evidence-practice gaps, and for all indicators combined.
Table 2: Evidence-practice gaps data pre- and post-intervention
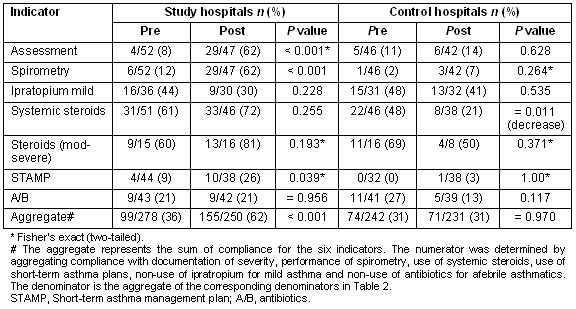
Statistically significant improvements were noted for the following clinical indicators at the study hospitals.
- assessment of severity increased from 8% to 62%
- spirometry use increased from 12% to 62%
- spirometry or peak flow rate use increased from 31% to 68%
- use of STAMP increased from 9% to 26%
- the aggregate of all six indicators from 36% to 62%
There was an increase (non-statistically significant) in use of systemic corticosteroids from 61% to 72%, including an increase from 60% to 81% for the moderate-severe subgroup.
There was a non-significant decrease in ipratropium use for mild asthma in the study hospitals from 44% to 30%. Ipratropium use in mild asthma was largely confined to one medical practice at one of the study hospitals. If data from this study hospital are removed, then the rate of ipratropium use for mild asthma at the other three hospitals has fallen from 13/29 (45%) to 4/24 (17%) (p <0.05, Fisher exact test, two-tailed).
There was no change in antibiotic prescribing for afebrile patients with asthma.
There were no significant changes in practice at the control hospitals except a significant decrease in systemic corticosteroid use from 48% to 21% (p = 0.011). At the control hospitals systemic corticosteroid use for the moderate-severe group fell from 69% to 50%, although this did not reach statistical significance.
Discussion
The ultimate aim of any quality improvement (QI) project is to change clinician behaviour for the better. A concept that emerged during the implementation process, and from meetings with clinicians was the concept of metanoia. The ancient Greek meaning of metanoia was to change people's hearts and minds towards something or someone. Successful implementation of change requires the targeted clinicians to believe in the evidence for and the value of the change. The evidence-based approach to implementation was designed to try and achieve this aim.
QI in rural areas
Criticisms of QI projects include that there is often no rationale for the method of implementing change and that they generally have poorly described methods7. In addition, many QI projects don't provide any evidence that any resultant change is due to the intervention and not some other factor16. This study has sought to address some of these limitations and has demonstrated that an EBI, can lead to significant improvements in compliance with evidence-based guidelines for asthma. Previous research suggests that attempts to increase compliance with guidelines can expect to yield changes in the order of 10%5,7. For some of the areas targeted for improvement the changes were of much greater magnitude in this study.
The implementation did not confine itself to the individual because there is evidence that targeting individual clinicians alone is of limited value in a complex environment such as an ED, and that the practice environment itself also needs to be addressed17,18,19. The intervention used in this study targeted not only individuals, but also processes within the ED and the organizational aspects of the departments.
The guideline was formatted to adhere to principles that are known to increase compliance with guidelines, these being compatibility with existing beliefs, simplicity, reducing (or not increasing) workload, being well validated, being from a respected source and requiring fewer new skills to be learned7,20.
Reminders and education, especially outreach education, have been shown to be among the most successful strategies for change5,7,21,22,23 and both strategies were used as part of the intervention.
The lead author visited sites, discussed evidence, discussed the guidelines and advocated compliance with the guidelines. In doing so, the lead author became a part of the implementation process as a knowledge broker, or a link between research evidence and clinical practice. There is evidence that such a role is crucial in implementing change24.
Uniqueness of rural medicine
There are a number of factors that make the rural environment different. Nearly half of the rural population (44%) live in an area that has a shortage of doctors9. In addition, 30% of rural Australians account for only 20% of Medicare rebates and are serviced by only 15% of the medical workforce9.
Those doctors who do provide services to rural district hospitals are usually GP VMOs or GP registrars, and attend to patients in the ED on an on-call basis. This is unlike regional referral hospitals where a hierarchy of full-time staff, from specialists trained in emergency medicine, to registrars, through to junior doctors and locums, practice. Attempts were made to visit each VMO either in their practice or at a scheduled hospital meeting but not every VMO was willing or able to be met face to face. Difficulties meeting each VMO and discussing the implementation and rationale behind the desired clinical behaviour was a significant impairment to the implementation process and may have impacted on the degrees of change. Rural GPs have identified barriers to practicing EBM that includes environmental barriers such as remoteness, professional isolation, workload and lack of evidence 'at hand'10. The same GPs have identified possible solutions to improve access to EBM10 and these solutions include better access to clinical practice guidelines, medical detailing and 'traveling road shows', all of which were components of this intervention.
Nursing staff at rural district hospitals are not full-time, dedicated ED nurses and within the same shift they may work in a number of different areas of the hospital. This again is different to staffing in regional base hospitals where nursing staff are generally working in the ED only, many of them with extensive emergency nursing experience. The implementation for the nursing staff included Power Point presentations on evidence-based medicine, the NAC guidelines and the planned guideline use. Asthma nurse educators were also involved in providing education on spirometry use and asthma management.
The ED team and organization also differ in rural district hospitals. The numbers of presentations of any condition are much lower which means there is a lower frequency of exposure to any condition, such as asthma and, therefore, less opportunity to use and become familiar with the guidelines. In these hospitals, fewer pathways are in use and so it is more difficult to establish a 'culture' of guideline use. Following on from this, there is often no obvious physical structure or place where the guidelines are kept and they are filed with other bits of paperwork. Despite attempts at addressing these issues, during site visits to two different study hospitals during the follow-up phase, the guidelines could not be easily found.
During the timeframe of this study a number of other projects were occurring across the area health service including both study and control hospitals. These included a pilot project of paediatric emergency guidelines, including asthma, being run by the Clinical Excellence Commission (CEC), a chronic care collaborative for chronic obstructive pulmonary disease and an extensive education campaign by clinical nurse specialists including spirometer use and asthma management. All these projects had the potential to impact on the ED management of asthma.
Improvements in compliance
There is evidence to support the six EPG identified in this study. Assessment of severity is self-evident because asthma guidelines2,3 have different treatment strategies for different degrees of severity. The documentation of severity improved by 54% in the study hospitals with no change in the control group. Failure of documentation of severity was generally associated with the guideline not being found in the medical record.
Spirometry is the preferred method for diagnosing and monitoring the progress of asthma1 and has been identified as an area of need with respect to ongoing education by GPs25. Very significant improvements in spirometry use were noted in the study hospitals. Despite other initiatives occurring across the area that had the potential to increase spirometry rates, there was no significant improvement in spirometry use in the control hospitals.
In severe asthma, ipratropium significantly improves spirometry and admission rates26,27 but these benefits have not been demonstrated for moderate asthma28,29. An evidence-based review found ipratropium to be beneficial for children or adults with acute severe asthma but of no benefit in those with mild to moderate asthma30. Even though ipratropium is commonly used4,31, Australian guidelines2,3 recommend that it not be used for mild asthma and list it as 'optional' for moderate asthma.
In this study there was a decrease in ipratropium use for mild asthma at the study hospitals of 14% compared with a 9% reduction in the control hospitals, neither group reached statistical significance. However, as noted in the Results, ipratropium use after the intervention was confined largely to just one study hospital and if the data from this hospital are removed, then significant reductions occurred at the other three.
A short course of systemic steroids reduces relapses, decrease beta-agonist use and decreases admission rates32 in acute asthma, especially with more severe attacks33. The increase in use of systemic steroids in the study hospitals was 11% overall but 21% for the moderate to severe group. Neither figure reached statistical significance, but the 81% figure for the moderate to severe group is higher than the national average4.
Unexpectedly there was a significant decrease in systemic corticosteroid use at the control hospitals from 48% to 21% including a non-significant decrease for the moderate to severe group from 69% to 50%. While not specifically audited, there was an anecdotally noted increase in inhaled corticosteroids at the control hospitals with many patients receiving inhaled but not oral corticosteroids acutely. It is possible that, in the absence of an evidence-based guideline, other external factors have influenced this prescribing practice. While there may be some evidence that high dose inhaled steroids alone are as effective as systemic steroids for mild asthma, this still needs to be clarified34. Cochrane reviews have determined that there is insufficient evidence that inhaled steroids are as effective as, or provide any additional benefit above and beyond systemic steroids34,35.
The intervention utilized a simple preformatted STAMP for the doctor to complete and give to the patient on discharge and the 17% increase in use was statistically significant though clinically modest. Rural patients want written instructions and advice for the first 24-48 hours after an acute asthma attack11.
The role of antibiotics in the treatment of acute asthma is difficult to assess from the current literature36; however, the general consensus is that most infectious triggers of asthma are viral. The EBI did not alter the rate of antibiotic prescribing.
Overall, the compliance for the six clinicial indicators increased from 36% to 62% at the study hospitals with no change in the control hospitals. These data highlight that despite well respected guidelines being available, and despite asthma being a common disease, compliance with best practice remains low. This emphasizes the importance of knowledge translation.
Limitations
There are a number of limitations to this study. The desired sample size of 56 patients was not met in the follow-up period with data for only 47 patients being recorded. For a level of significance of <0.05, this reduces the power to 0.84 which is still adequate for a study of this nature. The overall, aggregate, increase in compliance with the six clinical indicators was 26%, which was less than the targeted improvement of 30%, although still in excess of the 10% average described in the literature5,7.
In the pre-intervention phase, only approximately 10% of patients in the eight hospitals had formal documentation of severity in their notes. The initial audit, therefore, had to make an assessment of severity based on the clinical record with reference to the NAC 'Initial assessment of severity of acute asthma in adults' table in the Asthma management handbook2. While a Kappa analysis was not performed for this phase of the study, it has been performed in a parallel study, yielding a result of .756, which confirmed that this method of retrospective review is capable of making an adequate assessment of severity. The assessment of severity is important because evidence-based treatment for acute asthma varies depending on the severity2,3. Nevertheless, the retrospective assessment of severity, even if based on sound criteria, remains a limitation of this study.
The initial audit demonstrated that compliance with some clinical indicators including assessment of severity, spirometry and STAMP was poor, and there is evidence that improvement is greater when the starting base is lower37. These results cannot, therefore, be extrapolated to departments that are performing better in these areas.
The outcomes measured are all surrogate outcomes and there was no attempt to demonstrate decreased admission rates, adverse events, length of stay, representations or symptom duration. Nonetheless, evidence supports our view that these surrogate outcomes lead to clear clinical benefits, for example a short course of systemic corticosteroids will reduce admission rates, representations and symptom duration32,33.
As noted, the lead author became an integral part of the implementation process. This may limit the applicability of this approach, because other individuals looking to use the EBI at other centres will have different personal and professional qualities, interpersonal skills and interpersonal relationships with their target audience, which may help or hinder the process. Once the implementation was complete, the ability of the lead author to maintain this role was diminished and this may have an impact on the sustainability of these changes.
A final limitation is that no attempt was made to determine how prepared any of the eight hospitals in the study were to carry out change successfully. It was beyond the capacity of the study to conduct an assessment such as the Change Achievement Success Indicator38.
Hence, it is possible that by chance the study hospitals as a group were more or less susceptible to change and that if the two groups had been reversed the results may have been different.
A qualitative study is being planned to follow up which aspects of implementation were the most crucial to the success of this strategy, and a follow-up study to determine if the changes have been sustained is also planned.
Conclusion
This study has demonstrated that an EBI can significantly improve compliance with evidence-based guidelines with the potential to achieve much greater gains than in many previously published QI projects. The study design has also demonstrated that the changes in clinical practice were more likely due to the EBI rather than some other confounding variable.
Acknowledgements
The authors would like to acknowledge the assistance of statistician Associate Professor Christian Alexander - Hunter New England Health Rural Training Unit and University of New England. Steven Doherty has a fellowship with the National Institute of Clinical Studies who provided the funding for this research paper.
References
1. Marks GB, Correll PK, Williamson M. Asthma in Australia 2005. Medical Journal of Australia 2005; 183: 445-446.
2. National Asthma Council. Asthma Management Handbook. Melbourne, VIC: National Asthma Council, 2002.
3. Therapeutic Guidelines. Therapeutic Guidelines: Respiratory, Version 3. Melbourne, VIC: Therapeutic Guidelines, 2005.
4. Kelly A-M, Powell C, Kerr D. Snapshot of acute asthma: treatment and outcome of patients with acute asthma treated in Australian emergency departments. Internal Medicine Journal 2003; 33: 406-413.
5. Grol R, Grimshaw J. From best evidence to best practice: effective implementation of change in patients' care. Lancet 2003; 362: 1225-1230.
6. Sung NS, Crowley WF, Genel M et al. Central challenges facing the national clinical research enterprise. JAMA 2003; 289: 1278-1287.
7. Grimshaw JM, Eccles MP. Is evidence-based implementation of evidence-based care possible? Medical Journal of Australia 2004; 180(6suppl): S50-S51.
8. Cameron I. Retaining a medical workforce in rural Australia. Medical Journal of Australia 1998; 169: 293-294.
9. Rural Doctors Association of Australia. Good health to rural communities. (Online) 2004. Available: http://www.rdaa.com.au/uploaded_documents/GOOD%20HEALTH%20TO%20RURAL%20COMMUNITIES_final.pdf (Accessed 17 October 2005).
10. Taylor J, Wilkinson D, Blue IA, Dollard JT. Evidence-based rural general practice: barriers and solutions in South Australia. Rural and Remote Health 2: 116. (Online) 2002. Available: http//rrh.org.au (Accessed 17 October 2005).
11. Greenway-Crombie A, Conners A, Snell T, Oerlemans M. Development of a Rural Asthma Management Model (RAMM). Rural and Remote Health 3: 149. (Online) 2003. Available from: http//rrh.org.au (Accessed 14 October 2005).
12. Australian Bureau of Statistics. Census of population and housing. (Online) 2006. Available: www.abs.gov.au/Ausstats/ABS@census.nsf (Accessed 17 October 2005)
13. Doherty S. Evidence-based implementation of evidence-based guidelines. International Journal of Health Care Quality Assurance. 2006; 19: 32-41.
14. Doherty S. History of evidence-based medicine. Oranges, chloride of lime and leeches: barriers to teaching old dogs new tricks. Emergency Medicine Australasia 2005; 17: 307-314.
15. Doherty S. Evidence-based medicine: arguments for and against. Emergency Medicine Australasia 2005; 17: 315-321.
16. Ovretveit , Gustafson D. Improving research to inform quality programs. BMJ 2003; 326: 759-761.
17. Solberg LI, Brekke ML, Fazio CJ et al. Lessons from experienced guideline implementers: attend to many factors and use multiple strategies. Joint Commission Journal on Quality Improvement 2000; 26: 171-188.
18. Solberg LI. Guideline implementation: what the literature doesn't tell us. Joint Commission Journal on Quality Improvement 2000; 26: 525-537.
19. Dawson S, Sutherland K, Dopson S, Miller R. Changing clinical practice: views about the management of adult asthma. Quality in Health Care 1999; 8: 253-261.
20. Grol R, Dalhijsen J, Thomas S et al. Attributes of clinical guidelines that influence the use of guidelines in general practice: observational study. BMJ 1998; 317(7162): 858-861.
21. Grol R. Successes and failures in the implementation of evidence-based guidelines for clinical practice. Medical Care 2001; 39(9supp2): II-46-II-54.
22. Grimshaw JM, Shirran L, Thomas R et al. Changing provider behaviour: An overview of systematic reviews of interventions. Medical Care 2001; 39(8supp2): II-2-II-45.
23. Thomson O'Brien MA, Oxman AD, Davis DA, Haynes RB, Freemantle N, Harvey EL. Educational outreach visits: effects on professional practice and health care outcomes. The Cochrane Database of Systematic Reviews 1997, Issue 4. Art. no: CD000409.
24. Lomas J. Health services research. BMJ 2003; 327(7427): 1301-1302.
25. Goerman DP, Hogan CD, Aronie RA et al. Barriers to delivering asthma care: a qualitative study of general practitioners. Medical Journal of Australia 2005; 183: 457-460.
26. Rodrigo GJ, Rodrigo C. Triple inhaled drug protocol for the treatment of acute severe asthma. Chest 2003; 123: 1908-1915.
27. Rodrigo GJ, Rodrigo C. First line-therapy for adult patients with acute asthma receiving a multiple-dose protocol of ipratropium bromide plus albuterol in the emergency department. American Journal of Respiratory Critical Care Medicine 2000; 161: 1862-1868.
28. Fitzgerald JM, Grunfeld A, Pare PD et al. The clinical efficacy of combination nebulised anticholinergic and adrenergic bronchodilators vs nebulised adrenergic bronchodilators alone in acute asthma. Canadian combivent study group. Chest 1997; 111: 311-315.
29. Weber EJ, Levitt MA, Covington JK, Gambrioli E. Effect of continuously nebulised ipratropium bromide plus albuterol on emergency department length of stay and hospital admission rates in patients with acute bronchospasm. Chest 1999; 115: 937-944.
30. Rodrigo GJ, Rodrigo C. The role of anticholinergics in acute asthma treatment. Chest 2002; 121: 1977-1987.
31. Gibson PG, Talbot PI, Hancock J, Hensley MJ. A prospective audit of asthma management following emergency asthma treatment at a teaching hospital. Medical Journal of Australia 1993; 158: 775-778.
32. Rowe BH, Spooner CH, Ducharme FM, Bretzlaff JA, Bota GW. Corticosteroids for preventing relapse following acute exacerbations of asthma (Cochrane Review). The Cochrane Database of Systematic Reviews 2001, Issue 1. Art. no: CD000195.
33. Rowe BH, Spooner C, Ducharme FM, Bretzlaff JA, Bota GW. Early emergency department treatment of acute asthma with systemic corticosteroids (Cochrane Review). The Cochrane Database of Systematic Reviews 2001, Issue 1. Art. no: CD002178.
34. Edmonds ML, Camargo CA Jr, Brenner BE, Rowe BH. Inhaled steroids for acute asthma following emergency department discharge (Cochrane Review). The Cochrane Database of Systematic Reviews 2000, Issue 3. Art. no: CD002316.
35. Edmonds ML, Camargo CA Jr, Pollack CV Jr, Rowe BH. Early use of inhaled corticosteroids in the emergency department treatment of acute asthma (Cochrane Review). The Cochrane Database of Systematic Reviews 2003, Issue 3. Art. no: CD002308.
36. Graham V, Lasserson TJ, Rowe BH. Antibiotics for acute asthma (Cochrane Review). The Cochrane Database of Systematic Reviews 2001, Issue 2. Art. no: CD002741.
37. Jamtvedt G, Young JM, Kristofferson DT et al. Audit and feedback; effects on professional practice and health care outcomes. The Cochrane Database of Systematic Reviews 2003, Issue 3. Art. no: CD000259.
38. Ovretveit J. Change Achievement Success Indicator (CASI). Available at http://www.ihi.org/NR/rdonlyres/6A824554-B0D3-4E0A-B31E-D53D35707646/361/xxChangeSuccessIndicator.doc Accessed 14 March 2006).

