Introduction
Iodine deficiency disorder (IDD) is a major health problem in Thailand, leading to visible goiter and other symptoms, especially a mental defect among sufferers. The Thai northern and northeastern regions are endemic for IDD, due to their geographic limitation of a marine iodine source.
Many control programs have been implemented in the community since the introduction of iodized salt in 1960s1. However a high prevalence of endemic goiter persists, estimated as up to 30% in northeastern Thailand by a previous study2.
Because iodine deficiency causes impaired intellectual development, primary school children and their parents form target groups of any control program. This study consisted of a field survey performed on school children and their parents in an endemic area where an iodine supplementation program had been instituted. The aim of the study was to discover why this nationally initiated program had been ineffective at community level.
Materials and methods
Setting
This cross-sectional survey took place during October and November 1999 in Non Sam Ran Village, Borabue district, Mahasarakarm province, Thailand, approximately 470 km from Bangkok. This village was selected because it is located in the northeastern Thailand area endemic for IDD, and it had been involved in a recent iodine supplementary program involving the distribution for use of iodised household salt.
Preliminary salt survey in the village
A home visit was performed to all houses in the village and a salt sample collected. This tablespoonful of daily used salt from each kitchen was labeled and classified according to type (mined salt, marine salt or iodine-fortified salt). Each sample was tested on site for iodine content using I-KIT test (Mahidol University, Thailand). The test kit estimates iodine content after the salt sample and test reagent are mixed, leading to a color change which is compared to a standard color strip. The quantitative levels identified by the kit are 0, 10, 30, 50 and 100 ppm.
Interviewing of the primary school students
All primary school students in the village primary school were interviewed. A questionnaire, already tested for validity and reliability, was used for data collection. The questions focused on knowledge of IDD, source of natural iodine and iodine supplementation. Subjects were excluded if they could not answer the question or refused a home visit.
Home visit for parent interviewing
A home visit was performed for each subject but each home was only visited once. At this visit, one of the subject's parents was interviewed with the same set of questions. A kitchen survey and observation of eating style as it impacted on IDD was performed.
Statistical analysis
All collected data were interpreted then analyzed. Descriptive statistical analysis was performed where appropriate. Difference was assessed using a proportional Z-test at statistical significant level of p = 0.05.
Results
Results from the salt survey
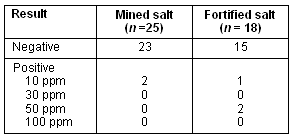
There were 43 salt samples collected and classified as 25 mined salt and 18 iodine-fortified salt samples. No marine salt was detected. After laboratory analysis, 38 samples (88.37%) were negative according to the iodine test (Table 1). There was no significant difference in iodine positive-samples between mined and fortified salt groups (p > 0.05).
Table 1: Salt samples analysis
Results from interviewing of the primary school students
There were 121 primary school children in the village. Five children were excluded due to an inability to understand the questionnaire, leaving a total 116 children enrolled in the study (Table 2). The average age of the subjects was 9.1 ± 0.4 years. All subjects lived in an agricultural family in the survey village area. Average number of members in subjects' families was 5 ± 0.2, and the yearly incomes were all below 30 000 baht.
Table 2: Data from village interviews
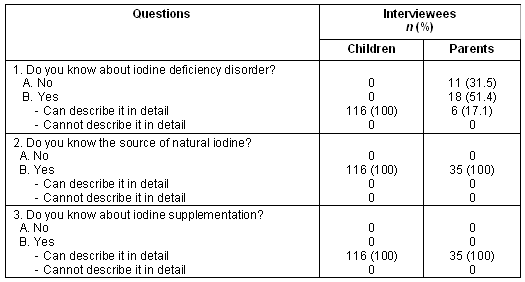
All school children replied that they knew of IDD but none could describe the symptoms of the disorder nor could they recall ever seeing such a patient. All children knew about and could describe in detail the natural source of iodine and iodine supplementation. All of them mentioned that the source of this knowledge was their school teacher. There was no sex difference in this knowledge (p > 0.05).
Home visit for parent interviewing
All 116 included primary school children lived in 35 houses in the village. A home visit and parental interview was achieved for all children. Considering the parents, only 24 of 35 reported that they knew of IDD, and only 18 parents could describe endemic goiter in detail (the others described it incorrectly as toxic goiter). All 18 parents correctly stated that the disorder was not contagious and that IDD patients would have an enlarged thyroid gland, which required specific treatment. However only four subjects knew that iodine was important in the intellectual development of children. Like their children, all parents knew and could describe in detail the natural source of iodine and significance of iodine supplementation. The major source of this knowledge was the mass media, especially radio (27 respondents, 77.1%) and television (8 respondents, 22.9%).
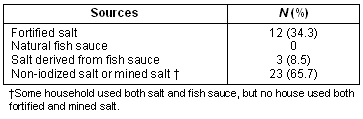
The kitchen survey revealed various sources of ingredients with a salty taste (Table 3). The most common was mined salt (65.7%), and only 34.3% of households had iodine supplementation (all from iodine-enriched salt). No iodized water was used for supplementation. Further enquiry revealed that iodized salt and iodized water were unpopular due to their unpleasant taste. In addition, natural fish sauce and salt-derived fish sauces were difficult to obtain and judged too expensive to use.
Table 3: Sources of salty taste ingredients from kitchen surveys
Discussion
Iodine deficiency disorder is an important and widespread health problem in Thailand; however, little is known of its distribution and there have been few publications concerning IDD3-6. Little work has been done in rural areas. A high incidence of IDD is still found in the northeastern region despite a long-established iodine supplementary program and socio-economic development.
Thailand is one of the most successful South-east Asian countries in addressing IDD and setting up programs to fight iodine deficiency. Nutritional intervention in terms of iodine-fortification of foods is a requirement in rural areas4-6. This study in an endemic IDD area where a supplementary program was in place revealed a good knowledge of natural iodine and iodine supplementation among school children. The children surveyed stated their knowledge was derived from school teachers, illustrating the effectiveness of providing basic health knowledge via school education.
A good level of knowledge about natural iodine and iodine supplementation was also present among the parents, reflecting the effectiveness of government iodine supplementation promotion. However, there were some gaps in parental knowledge with only approximately 50% being able to detail IDD. This may explain the high prevalence of IDD among primary school children in an endemic area in a previous study7, and suggests that health promotion to parents of child-bearing age could improvement their children's nutritional health status8.
However, of grave concern is that, despite effective knowledge of the need for iodine supplementation and sources of iodine, non-iodized salt was still the major source of salty taste ingredient in the daily life of the subjects. This taste preference meant that, although iodized salt and iodized water was cheaper than natural fish salt, subjects still preferred the better-tasting non-iodized salt.
As well as the taste preference, there was no significant difference in iodine level between the mined and iodine-fortified salt samples (p >0.05), indicating that those who did use iodised salt may not have been gaining the expected advantage. This is due to a quality control failure in iodine-fortified salt manufacture.
Recommendations
It is recommended that the following factors be addressed by health professionals instituting national nutritional interventions. Attention should be given to the finding that despite the effective transmission of health knowledge regarding iodine deficiency in rural Thailand, a taste preference subverted the application of that knowledge. In addition, national quality control surveillance should be instituted in fortified salt manufacture.
This study was performed in a small setting, and therefore generalization should be performed with caution. However, it can, at the very least, serve as a pilot study with further research indicated on a larger scale to underpin a national campaign on the manufacture and use of iodine-fortified salt in Thailand.
Acknowledgements
The author thanks Associate Professor Jamsai Suwansaksri who assisted in the laboratory analysis, and all the villagers who participated in this study. Some parts of this work were presented at the 8th World Congress on Clinical Nutrition, Phitsanulok, Thailand, 2000.
References
1. Suwanik R, Nondasuta A, Nondasuta A. Field studies of iodine metabolism in an endemic goiter village, Phrae Thailand. Journal of the Nutritional Research Council of Thailand 1961; 2: 1.
2. Supawan V, Tungtrongchitr R, Prayurahong B, Pongpaew P, Sanchaisuriya P, Kassomboon P, Saowakontha S, Schelp FP, Migasena P. Urine iodine concentration and prevalence of goiter among rural women of child bearing age in northeast Thailand. Journal of Medical Association of Thailand 1993; 76: 210-215.
3. Pandav CS, Anand K, Sinawat S, Ahmed FU. Economic evaluation of water iodization program in Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 2000; 31: 762-768.
4. Thurlow RA, Winichagoon P, Pongcharoen T, Gowachirapant S, Boonpraderm A, Manger MS et al. Risk of zinc, iodine and other micronutrient deficiencies among school children in North East Thailand. European Journal of Clinical Nutrition 2006; 60: 623-632.
5. Jaruratanasirikul S, Chukamnerd J, Koranantakul O, Chanvitan P, Ruaengrairatanaroj P, Sriplung H. The relationship of maternal iodine status and neonatal thyrotropin concentration: a study in Southern Thailand. Journal of Pediatric Endocrinology & Metabolism 2006; 19: 727-732.
6. Winichagoon P, McKenzie JE, Chavasit V, Pongcharoen T, Gowachirapant S, Boonpraderm A et al. A multimicronutrient-fortified seasoning powder enhances the hemoglobin, zinc, and iodine status of primary school children in North East Thailand: a randomized controlled trial of efficacy. Journal of Nutrition 2006; 136: 1617-1623.
7. Sittipongsakul S, Youngnoi W, Nanthasomboon I. Perception and self care of school children with iodine deficiency disorder in Amphur Maesarieng, Maehongsorn Province. Thai Journal of Nursing 1999; 48: 114-122.
8. Saowakontha S, Pongpaew P, Vudhivai N, Tungtrongchitr R, Sanchaisuriya P, Mahaweerawat U et al. Promotion of the health of rural women towards safe motherhood--an intervention project in northeast Thailand. Southeast Asian Journal of Tropical Medicine and Public Health 2000; 31(Suppl 2): 5-21.
Abstract
Iodine deficiency disorder (IDD) is an important health problem in Thailand. Due to the geographical limitation of marine salt distribution, the Northern and Northeastern regions of Thailand are endemic areas of this disorder. In this study, a cross-sectional survey on the domestic use of iodine-enriched salt by the people in a rural village, Non Sam Ran, Borabue district, Mahasarakarm province in the northeastern region of Thailand was conducted. A salt survey was undertaken in the village, involving the specific health knowledge of both primary school students and their parents, and including a home visit with kitchen salt sampling. As a result of this survey, despite the smallness of the sample, concern is raised regarding the application of public health information about IDD due to a taste preference for non-iodised salt, and the quality control of the manufacture of iodine-fortified salt.
Key words: children, iodine, Iodine deficiency disorder, primary school, salt.
