Case report
A seventeen-year old man presented to the Bedford Orthopaedic Centre (BOC) in South Africa with immobility due to an inability to straighten his legs. He had been confined to a wheelchair for approximately 6 months. He had no prior history of mobility problems or joint disease.
The patient had been admitted to the intensive care unit of a large teaching hospital 8 months previously in septic shock following a circumcision as part of his initiation ceremony. Clinical examination at that time had revealed perineal cellulitis and hypotension. He required vigorous fluid resuscitation and antibiotic administration. Culture of two pus swabs identified erythromycin-sensitive Streptococcus pyogenes and Staphylococcus aureus, although blood cultures were negative. His urological condition gradually improved following intravenous antimicrobial therapy. Mobilisation was attempted after 2 months' treatment in the ICU. However, he was found to have progressive knee contractures which prevented walking and an orthopaedic review was requested.
On presentation to the BOC, the patient was found to be in a poor general condition although systemically well. He was afebrile but below average weight with marked atrophy of his thigh and leg muscles. His knees were swollen with a mild effusion although there was no evidence of acute infection. He had a fixed flexion deformity of both knees: 95 degrees on the left side and 100 degrees on the right side (Fig 1). Examination of his spine, hip joints and ankle joints was normal and there was no neurological deficit. The skin quality of the lower limbs was poor and there was ulceration on the right leg.
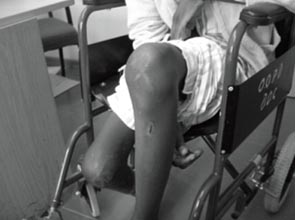
Figure 1: Patient presents to clinic with bilateral knee contractures.
Full blood count revealed normal haemoglobin and white blood cell count. Chest X-ray was normal. Adequate knee X-rays were difficult to obtain and showed gross joint destruction with loss of joint space (Figs 2,3) and bone erosion. Radiologically and clinically the right knee was most severely affected. Testing for HIV was negative.
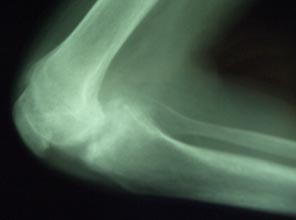
Figure 2: Plain lateral radiograph of the right knee.
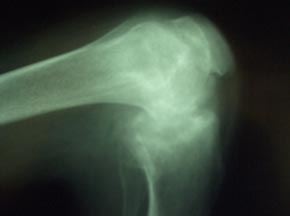
Figure 3: Plain lateral radiograph of the left knee.
In view of his poor general condition, major surgical correction was deemed inappropriate. In order to allow some mobilisation and to facilitate nursing care, both knee joints were assessed under general anaesthetic and gentle manipulation was performed (Fig 4). Three manipulations under analgesia were performed in 4 weeks, and the lower limbs were immobilised in cylinder casts between manipulations. After the third manipulation his left knee was at 5 degrees of flexion and the right knee was at 15 degrees. The procedures were tolerated well.
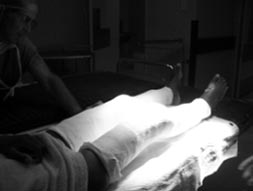
Figure 4: Progressive joint manipulations under anaesthetic.
He commenced an intensive physiotherapy program and was mobilised with the aid of a walking frame. His progress was slow but at the time of this report he is able to transfer safely for hygiene, and can walk a few hundred metres with the aid of a walking stick. Examination shows comfortable left-knee range of movement from 10 to 35 degrees. Although the right tibia is subluxated posteriorly he has a comfortable range of movement from 10 to 30 degrees. He has undergone successful split skin grafting of the ulcerated area on his right leg and the infection has subsided.
Discussion
In some African communities in South Africa, initiation ceremonies that include circumcision are considered necessary in order for young men to become adult members of their communities1. Circumcision is also considered necessary for health reasons. Most initiates undergo the procedure without incident. However, a minority suffer medical complications from the circumcision, which may not be carried out under aseptic conditions. While there are little published data on the incidence of complications, anecdotal evidence suggests infection rates are significant. This case highlights one of the rarer complications of such a circumcision.
In the developing world, the presentation orthopaedic conditions are often delayed. The delay in referral of this challenging case was compounded by diagnostic uncertainty. Initial pus swabs confirmed the presence of Staphylococcus aureus and Streptococcus pyogenes, both organisms that commonly cause septic arthritis. Knee X-rays revealed extensive changes consistent with previous bacterial septic arthritis, and gross destruction of joint surfaces.
Acute septic arthritis is caused by bacterial seeding of the synovium and joint space2, as the result of haematogenous spread (bacteraemia or septicaemia), direct inoculation from open wounds, spread from adjacent metaphyseal osteomyelitis or soft tissue infection. The vascular space of the synovium is vulnerable to haematogenous spread of infection because it lacks basement membrane, providing relatively easy access to the joint space2. An intense inflammatory reaction follows, with migration of polymorphonuclear leukocytes and subsequent release of proteolytic enzymes, leading to destruction of articular cartilage. One-third of all such patients will suffer residual loss of function in the involved joint.
Septic arthritis is most likely in the large joints with the knee affected in 45% of cases. Other commonly involved joints include the hip (15%), ankle (9%), elbow (8%), wrist (6%) and shoulder (5%)3. Polyarticular disease is seen in 10% to 20% of cases, commonly among those who are elderly and chronically ill with problems such as diabetes mellitus and rheumatoid arthritis, and may be more common with gonococcal infection3. However, Staphylococcus aureus is the most common bacterial cause of septic arthritis, accounting for up to 44% of cases overall and 80% among those with rheumatoid arthritis or diabetes mellitus3. Of concern is the increasing prevalence of methicillin-resistant Staphylococcus aureus.
The rare non-gonococcal polyarticular septic arthritis involves two or more joints and has a poor prognosis4-6. Epstein et al.4 and Lins et al.5 found Staphylococcus aureus to be the most commonly involved organism, mainly affecting large joints and those with underlying rheumatoid arthritis. Streptococcus pyogenes is isolated in approximately 8% of these patients7.
Epstein et al. reported that 5 of their 7 patients died from polyarticular arthritis, although most had underlying rheumatoid arthritis4. Dubost et al. isolated Staphylococcus aureus in 20 of 25 patients with polyarticular arthritis, and reported a mortality rate of 32%6. Of Cabo Cabo et al.'s 10 patients with polyarticular arthritis, 54% had a poor functional result, while three of the 50% who presented in septic shock died7. Martens and Ho reported a mortality rate of 40% in their patients with polyarticular arthritis8.
Any patient with an acutely swollen joint may represent an infectious disease emergency, namely acute septic arthritis. The fundamental treatment principles of septic arthritis include prompt diagnostic joint aspiration (for microscopy and culture) followed by early adequate joint drainage, administration of appropriate antibiotics, and resting the joint in a stable functional position2. However, in some cases the cardinal features of infection may not be apparent, making diagnosis difficult6, particularly in immunocompromised patients. Delay in diagnosis and a failure to commence appropriate treatment are the most common reasons for the late complications of infection, which include joint contractures and stiffness, and late instability with joint subluxation and dislocation.
Without prompt antibiotic therapy and joint drainage, the morbidity and mortality are significant, and long-term disability is common. In order to prevent joint destruction, arthrotomy and joint washout is indicated9, although arthroscopic washout is an alternative. Repeated early stage joint aspiration has been advocated10; however, timely joint washout should be performed if rapid recovery does not occur. Post-operative management takes the multidisciplinary team approach with particular attention to early, intensive physiotherapy.
Severe contractures of the knees are extremely problematic for patients and their caregivers. Surgical options for managing such deformities are challenging and include percutaneous tenotomies and rotational osteotomy of the distal femur, followed by simple bracing11. Other methods include joint distraction and reconstruction with the use of external fixation12,13. However such methods, useful mainly in post-traumatic and paralytic flexion contractures, are questionable in the management of post-sepsis contractures, especially in a resource-poor setting.
Conclusion
The management of untreated septic arthritis can be difficult. Clinicians should be alert to the possibility of septic arthritis following septicaemia, and be prepared to institute early aggressive treatment with prompt orthopaedic referral in order to prevent long-term morbidity.
References
1. Stoppard A. Rights-South Africa: fatalities blamed on initiation rituals. Inter Press Service English News Wire. (Online) 4 July 2002. Available: http://www.highbeam.com/doc/1P1-54182970.html (Accessed 24 July 2007).
2. Williams KD. Infectious arthritis. In: TS Canale (Ed.). Campbell's operative orthopaedics, vol 1, 9th edn. St Louis: Mosby, 1998; 601-625.
3. Garcia-De La Torre I. Advances in the management of septic arthritis. Rheumatic Diseases Clinics of North America 2003; 29: 61-75.
4. Epstein JH, Zimmermann B, Ho G. Polyarticular septic arthritis. Journal of Rheumatology 1986; 13: 1105-1107.
5. Lins RE, Hankin FM, Kaufer H, Granger JF. Septic polyarthritis and its relation to systemic disease processes: a report of three cases. Journal of Arthroplasty 1988; 3: 359-362.
6. Dubost JJ, Fis I, Denis P, Lopitaux R, Soubrier M, Ristori JM et al. Polyarticular septic arthritis. Medicine (Baltimore) 1993; 72: 296-310.
7. Kaandorp CJ, Dinant HJ, van de Laar MA, Moens HJ, Prins AP, Dijkmans BA. Incidence and sources of native and prosthetic joint infection: a community based prospective survey. Annals of Rheumatic Diseases 1997; 56: 470-475.
8. Martens PB, Ho G Jr: Septic arthritis in adults: clinical features, outcome, and intensive care requirements. Intensive Care Medicine 1995; 10: 246-252.
9. Nade S. Acute septic arthritis in infancy and childhood. Journal of Bones and Joint Surgery 1983; 65-B: 234.
10. Wilson NIL, Di Paola M. Acute septic arthritis in infancy and childhood. Journal of Bones and Joint Surgery 1986; 68: 584-587.
11. Huckstep RL. Management of neglected joint contractures. Clinical Orthopaedics and Related Research2007; 456: 58-64.
12. Devalia KL, Fernandes JA, Moras P, Pagdin J, Jones S, Bell MJ. Joint distraction and reconstruction in complex knee contractures. Journal of Pediatric Orthopedics 2007; 27: 402-407.
13. Herzenberg JE, Davis JR, Paley D, Bhave A. Mechanical distraction for treatment of severe knee flexion contractures. Clinical Orthopaedics and Related Research1994; April (301): 80-88.


