Introduction
Suicide is an important public health problem, with a disproportionate impact on young adults. In Scotland the highest rates are among men aged less than 45 years1. A national suicide reduction strategy, 'Choose Life', has been developed1. Deprivation is associated with increased rates of suicide2,3, and rates in Scotland have changed over time, with an increase among younger men and a decrease in most age groups among women4. The national suicide prevention strategy has a particular focus on younger men in its first phase, but also encourages wider exploration of risk factors for suicide1.
Suicide rates tend to be high in urban areas of the UK5,6, but high rates are also found in rural areas in some countries, particularly among young adults7-10. The Scottish strategy lists rural areas as one of the areas of intervention. Previous work in Scotland found higher male rates in the Highlands11. People sometimes travel to scenic areas to kill themselves. These deaths contribute to higher rural rates, but the rate in Highland remained high even when the deaths of visitors were excluded from the figures12. Further research found that some other rural parts of Scotland had higher than average male suicide rates among people resident in the area4. Levin and Leyland3 reported that small remote rural communities have higher standardised mortality ratios than urban areas, but no information has been available on the relationship between population density and suicide in Scotland.
This study aimed to identify the association between population density and suicide by sex, taking into account the influence of deprivation and time period.
Methods
Anonymised information on deaths by suicide and undetermined deaths provided by the General Register Office for Scotland (GROS) was used. Deaths registered during the period 1981-1999 were included if the cause of death was recorded as suicide or as undetermined cause (ICD-9 E950-E959, ICD-10 X60-X84 and E980-E989 or Y10-Y34, respectively).
Population figures were taken from the GROS annual reports for the mid-year of each period. For analyses by area, if a death was registered away from the person's home address, the death was allocated to their area of residence, rather than the area in which they died. Deaths of people resident outside Scotland were identified using country codes, and were excluded. As far as possible, therefore, results reflect the rates of suicide and undetermined deaths of people resident in each area of Scotland. In time period descriptions, the periods 1981-1985, 1986-1990, 1991-1995 and 1996-1999 were used. Data were analysed by sex and age group. Age groups and time periods were chosen in order to increase comparability with previous work. Data were analysed using Microsoft Excel and SPSS (SPSS Inc, Chicago, IL, USA).
Each postcode sector was assigned a deprivation and density score. Adjustments for differences in deprivation between cases were made using the Carstairs index of deprivation from the 1991 census13. In the Carstairs score, four variables are used to identify the affluence of an area, including unemployment, lack of a car, overcrowding and social class. There are limitations to the application of the Carstairs score in rural areas, because limited public transport may mean that car ownership is essential, even when it imposes a substantial financial burden. It is, however, the only national deprivation score available for Scotland in the whole of the time period reviewed, and is therefore used in this study. The index was categorised into quintiles (1 = the most affluent areas, 5 = the most deprived areas).
Population density, a measure of the number of people in an area of given geographical size, is often used as a proxy for rurality14,15. Population density is available by postcode sector in Scotland, and so it was used as an accessible measure of rurality for the analysis. Density quartiles were derived based on the number of residents per hectare for each postcode sector, with 1 indicating a less populated area and 4 a highly populated area. Small area population estimates for each postcode sector were used to calculate suicide/undetermined death rates.
Log linear models were fitted to the number of suicides in each sex and age group per head of population. These models were used to test the statistical significance of the effects of time period (grouped into four periods, each of 5 years), deprivation quintiles, population density (grouped into four quartiles) and their interactions. A significance level of 5% was used throughout. Adjusted rate ratios and 95% confidence intervals were based on models that included only significant factors and interactions.
Results
Deprivation (D), population density (PD) and time period (TP) were examined. The factors significantly associated with suicide rates in the loglinear analysis are shown in Table 1. Deprivation was significantly associated in all age groups in both sexes (Table 1). Time period was independently significant in all groups other than men aged over 45 years. Population density was significant in all groups other than young women. Interactions were seen in several age groups, and are discussed further below.
Table 1: Significant factors by age group and sex

Where interactions between variables were present, relative risks could not be calculated and findings are shown in separate tables.
Men
15-24 years: Deprivation, rurality and time period were independently significant (Fig1). Rate ratios increased over time, and with increasing deprivation. The highest rate ratios for population density were in the most urban and most rural areas, with the highest rate ratio in the most rural quartile.
25-44 years: There were interactions between time period and deprivation, and rurality and deprivation. Table 2 shows time period and deprivation. In every period male suicide and undetermined death rates were higher among more deprived groups. Over time, rates increased in each level of deprivation. The gradient between least deprived and most deprived increased over the time period.
Table 3 shows deprivation and population density. Across all categories of population density, suicide rates increased as deprivation increased. In deprivation quintiles 1 to 3, the highest rates were in the lowest population density group and a J-shaped relationship was seen overall.
45 years and over: Rate ratios increased as deprivation increased (Fig 2). The highest rates were in the most rural areas followed by the most urban, with intermediate rates in the other population density quartiles.
Women
15-24 years: There was an interaction between deprivation category and time period (Table 4). Within each time period, the highest rates were in the most deprived quintile. There were large increases in rates in all but the most affluent quintile. This increase occurred earlier in more deprived groups.
25-44 years: Suicide and undetermined death rate ratios increased with deprivation (Fig 3). The highest rate ratios for population density were in the most rural and most urban quartiles, with lower rate ratios in the intermediate groups. There was an increase between the second and third time periods.
45 years and over: In this older age group, rates increased as population density increased (Fig 4). Rates were also higher in more deprived areas, although the gradient was not as large as in younger women or in men in the same age group. Suicide rates decreased over time, with the greatest decrease occurring in the first two time periods.
Table 2: Suicide and undetermined intent death rate per 100 000 in males aged 25-44 years in Scotland, by time period and deprivation category
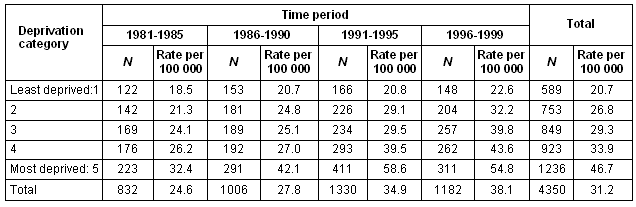
Table 3: Suicide and undetermined intent death rate per 100 000 in males aged 25-44 years in Scotland, by density quartile and deprivation category
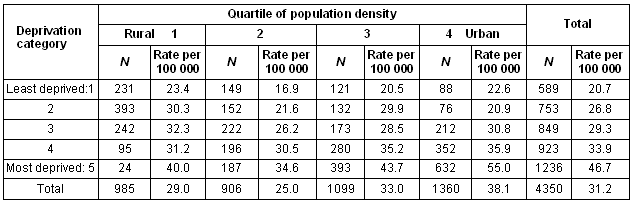
Table 4: Suicide and undetermined intent death rate per 100 000 in women aged 15-24 years in Scotland, by time period and deprivation category
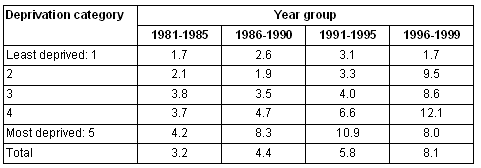
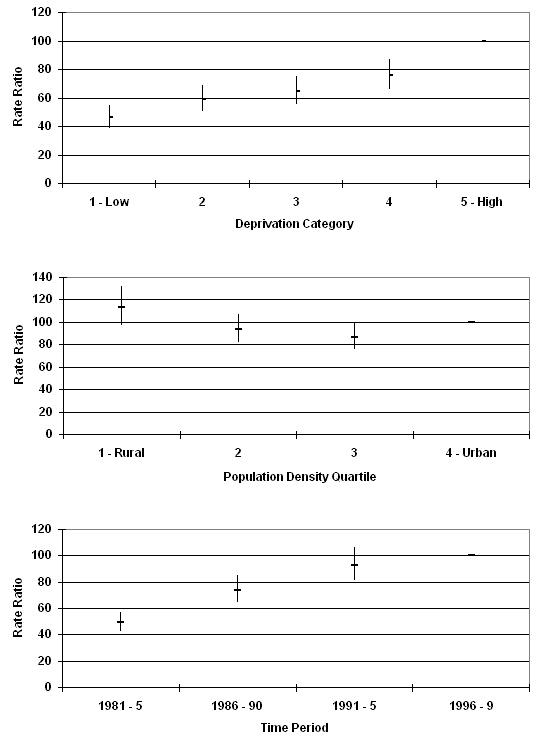
Figure 1: Suicide and undetermined intent deaths in males in Scotland aged 15-24 years. Rate ratios by population density, deprivation category and time period.
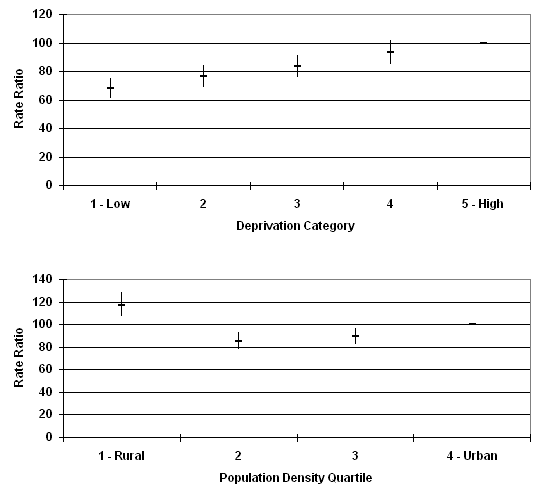
Figure 2: Suicide and undetermined intent deaths, 1981-1999 in males in Scotland aged 45 years and over. Rate ratios by population density and deprivation category.
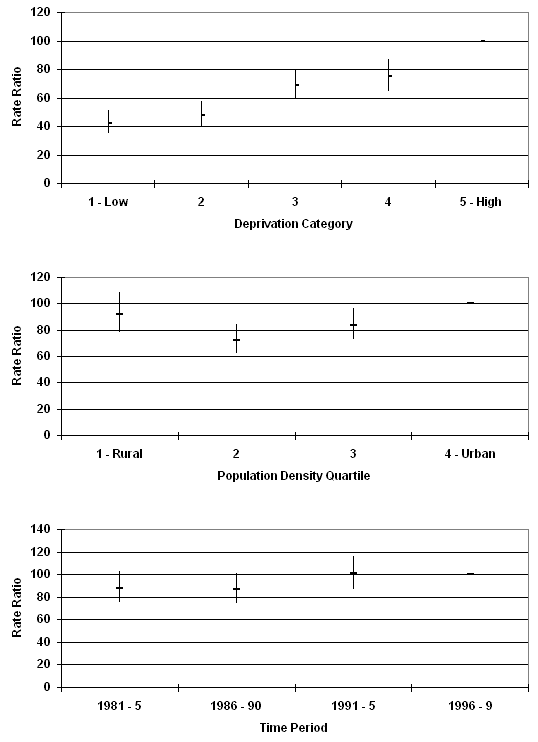
Figure 3: Suicide and undetermined intent death rate per 100 000 in females aged 25-44 years in Scotland. Rate ratios by population density, deprivation category and time period.
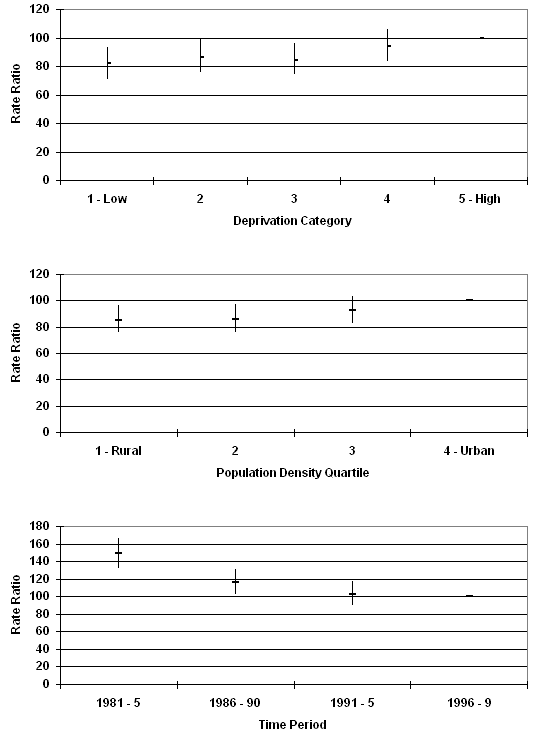
Figure 4: Suicide and undetermined intent deaths in females in Scotland aged 45 years and over. Rate ratios by population density, deprivation and time period.
Conclusions
Population density was independently associated with the rates of suicide and undetermined deaths in both sexes and in all age groups other than younger women. Deprivation showed a significant association in all age groups. Time period was independently associated with rates in all groups other than older men. This confirms previous findings on age group and sex, and provides new information on population density and deprivation.
Deprivation
As might be expected, deprivation is strongly associated with suicide rates in Scotland2,16, and it was important to take its effects in to account in the analysis. Deprivation measures were independently significant at all ages. A previous analysis, focusing on changes in deprivation association over time, described changes in the 15-44 year and 45 year and over age group2. The present study finds that the gradient of suicide rates with deprivation was not confined to one group within the under 45 year age group, but was present in both the 15-24 year age group, and the 25-44 year age group in both sexes.
The measure of deprivation used in this study, the Carstairs score, was developed for Scotland as a whole and not for rural areas in particular. It is possible that the measure of deprivation used for this study underestimates rural deprivation. Variation within an area can be great, leading to an averaging of deprivation that ignores within-area differences14-16. By comparison, deprivation in urban areas may be relatively homogeneous17.
The association between increased suicide rates in the UK and higher levels of deprivation is well documented18,19. In a time-series analysis of information for the last half of the twentieth century in England and Wales, Gunnell et al.20 reported that increases in income inequality were one of the factors most consistently associated with the increase in younger male suicide. It seems likely that social changes are also implicated. Whitley et al.21 found that measures of social fragmentation were significantly associated with suicide rates in England and Wales. Increases in divorce and declines in marriage rates also appear to be associated with higher rates of suicide among younger men22.
Time period
Time period was similarly significant. Suicide and undetermined death rates increased in younger men in Scotland in the 1980s and 1990s and decreased in most female age groups 4. Interactions between deprivation and time period were seen among 25-44 year old men, and among younger women. In each case, the effect was of a greater increase in the most deprived groups earlier in the period, and with a greater rate of increase, leading to a widening of inequalities over the period.
Population density
A J-shaped association between rurality and health has been reported in other areas of work23-25, with the best reported health in the more accessible countryside. Analysing census data, Barnett et al.15 found that self-reported limiting long term illness (LLTI) was higher in urban areas, and lower in semi-rural areas in the south-west of England, and concluded that there was a U-shaped relationship with rurality. Deprivation indices explained 67% of the variation in LLTI in urban areas, but only 7% of the variation in the rural fringe, and 3% in very rural areas. Men reported higher levels of LLTI than women. Controlling for isolation, using a 'nearest neighbour' measure reduced the level of unexplained variation in rural areas. Population density, in this area of England, became insignificant in a multi-level regression model when isolation was introduced.
Levin and Leyland3 reported that the remotest Scottish settlement types had a high male suicide rate. This may reflect the heterogeneity of rural areas, and the difficulties of defining rurality. Low population density is often taken to be a defining characteristic of rural areas, but density operates in different ways. A rural area may have a low population density, but if people live in settlements, distance between individuals may be small despite low overall density25. Similarly, including urban areas in the calculation of the overall density of an area, known as gross population density, may be misleading compared with 'net' population density, which includes only non-urban areas in the calculation25. Irving and Davidson26 examined social density as the amount of person-to-person interaction taking place in an area in unit time, and more subtle measures of this type may help to elucidate the mechanism for this relationship between suicide rates and population density.
Rurality and suicide
A key finding may be the difference in apparent impact of rurality on older men and older women. Many of the changes in rural areas have affected both sexes. Often grouped together under the term 'rural restructuring' these changes include diversification of rural activity and of farm income; changes to the population structure; counterurbanisation in some areas with population moving from more urban areas; increased environmental limits to land use, and changes to public services27,28.
There may be a greater impact on men than women on aspects relating to employment. There is now a greater concentration on the service industry. Many men in rural areas are unwilling to consider such employment, and may also rely, in a more competitive job market, on more traditional approaches. Jobs in rural areas in the past have often been found through extended social networks and community contacts, and these may be less efficient employment-seeking strategies than those used by some newer migrants to rural areas, who are familiar with working in a more structured job market27,29. Those in the rural fringe may be better able to access urban markets than those in more isolated settings.
Barnett et al.21 also raise the question of service access. Philo et al. argue that the impact of mental ill-health may be mediated by the characteristics of rural areas30. Cloke suggests that 'a sense of belonging and cultural acceptance of their situation may well ameliorate...issues of the structuring of opportunities in the experience of rural people'31. In his view, the 'non-affluent, the young and the different' may not be welcomed. Rural communities may have social norms that limit behaviour32. Kane and Ennis33 suggested that 'Gemeinschaft characteristics' of areas, the day-to-day social interactions that define and limit behaviour, may be important. It is not clear if these factors affect men and women in different ways, but men have often been found to access services less than women, and rural visibility and cultural approaches to mental illness may further exacerbate this. Further research should be directed to service access by sex.
Philo et al.30 point out that many studies assume that community support is better in rural areas. This may not, however, be the case. Parr, Philo and Burns34 describe the experience of being ill in the Highlands of Scotland. The lived experience they describe is likely to be applicable in any small town or village in the UK. Service users portray landscape in which little is private. Acts influenced by illness are noted, discussed and remembered. Accessing services becomes even more difficult than usual, because of the high probability that such access will be noted. Some respondents described social isolation in their community stemming from knowledge of their mental health problems. Some felt that they would have greater anonymity in urban settings. At the same time, some people identified benefits associated with where they lived, including a feeling of being less hurried and of having a firmer base in life. Parr et al. observed that as many people reported adverse effects of living in a rural area as found it to be of benefit34.
Previous work in Scotland has found higher than expected rates of male suicide in some rural occupations, including farming and forestry35. One reason for this might be access to lethal means of suicide, including firearms36, but changes to occupational practice, including lower levels of farm employment, and greater lone working are also likely to be relevant.
Recommendations
These findings argue for further work in Scotland on suicide prevention in rural areas. Men appear to be relatively disadvantaged compared with women. There is no published information in Scotland on the more detailed nature of male suicide in rural areas, so we do not know the relative importance of mental illness, self-harm, service use and socio-economic differences. Work to examine mental health service use before suicide in rural and urban areas would be valuable in helping to identify if service access issues are important.
Without such work, it is still possible to identify areas of possible intervention. Gun safety is important for those with occupational or sporting access to firearms, and advice to rural doctors and police officers on this should be useful. Awareness in rural areas may still be limited, and help seeking in Scottish men has often been poor. There is a national program in Scotland on stigma reduction in mental health, the 'See Me' campaign. There is also a helpline introduced by the Scottish government and targeted particularly at young men, called 'Breathing Space'. While stigma reduction is an important long-term project, encouraging the use of support mechanisms such as Breathing Space offers immediate support to men in rural areas who may be reluctant to reveal difficulties. Directing some of the national publicity on suicide prevention, stress and stigma to rural areas would be a practical step.
The response people receive in rural areas is important, and increasing community capacity both by training staff in recognition and management of suicide risk, and by making training available to community groups would be a proportionate response which would increase general mental health-related skills as well as those that are suicide-specific. Locating suicide as a rural problem is challenging, and awareness of suicide risk in rural communities should be increased by targeted work by local 'Choose Life' groups, balanced by the availability of training.
This work, taken together with other findings, argues for the importance of suicide as a problem for rural Scotland. Further research is required, but practical steps to increase awareness, reduce stigma, and increase coping capacity in services and communities, while also encouraging help-seeking will be practical first steps in reducing the burden of preventable suicide deaths in rural communities.
Acknowledgements
This work was undertaken with a grant awarded by the Scottish Executive's Remote and Rural Areas Resource Initiative. NHS Highland supplied staff time from CS and PH. Mike Muirhead of ISD, Professor David Gunnell of the University of Bristol and Professor David Godden of the University of Aberdeen provided helpful advice during the study.
References
1. Scottish Executive. Choose Life: A national strategy and action plan to prevent suicide in Scotland. Edinburgh: Scottish Executive, 2002.
2. Boyle P, Exeter D, Feng Z, Flowerdew R. Suicide gap among young adults in Scotland: population study. BMJ 2004; 330: 175-176.
3. Levin KA, Leyland AH. Urban/rural inequalities in suicide in Scotland, 1981-1999. Social Science and Medicine 2005; 60: 2877-2890.
4. Stark C, Hopkins P, Gibbs D, Rapson T, Belbin A, Hay A. Trends in suicide in Scotland 1981-1999: age, method and geography. BMC Public Health 2004; 4: 49. Available: http://biomedcentral.com (Accessed 19 June 2007).
5. Kelly S, Charlton J, Jenkins R. Suicide deaths in England and Wales, 1982-92: the contribution of occupation and geography. Population Trends 1995; 80: 16-25.
6. Saunderson TR, Langford IH. A study of the geographical distribution of suicide rates in England and Wales 1989-92 using empirical bayes estimates. Social Science & Medicine 1996; 43: 489-502.
7. Dudley M, Waters B, Kelk N, Howard J. Youth suicide in New South Wales: urban-rural trends. Medical Journal of Australia 1992; 1556: 83-88.
8. Middleton N, Gunnell D, Frankel S, Whitley E, Dorling D. Urban-rural differences in suicide trends in young adults: England and Wales, 1981-1998. Social Science and Medicine 2003; 57: 1183-1194.
9. Personen TM, Hintikka J, Karkola KO, Saarinen PI, Antikainen M, Lehtonen J. Male suicide mortality in eastern Finland - urban-rural changes during a 10-year period between 1988 and 1997. Scandinavian Journal of Public Health 2001; 29: 189-193.
10. Singh GK, Shiahpush M. Increasing rural-urban gradients in US suicide mortality, 1970-1997. American Journal of Public Health 2002; 92: 1161-1167.
11. Crombie IK. Suicide among men in the highlands of Scotland. BMJ 1991; 302: 761-762.
12. Stark C, Matthewson F, O'Neill N, Oates K, Hay A. Suicide in the Highlands of Scotland. Health Bulletin 2002; 60: 27-32.
13. Carstairs V, Morris R. Deprivation: explaining differences in mortality between Scotland and England and Wales. BMJ 1989; 299: 886-889.
14. Gilthorpe MS, Wilson RC. Rural/urban differences in the association between deprivation and healthcare utilisation. Social Science and Medicine 2003; 57: 2055-2063.
15. Barnett S, Roderick P, Martin D, Diamond I. A multilevel analysis of the effects of rurality and social deprivation on premature limiting long term illness. Journal of Epidemiology and Community Health 2001; 55: 44-51.
16. Barnett S, Roderick P, Martin D, Diamond I, Wrigley H. Interrelations between three proxies of health care need at the small area level: an urban/rural comparison. Journal of Epidemiology and Community Health 2002; 56: 754-761.
17. McLaren G, Clarkson A. A picture of employment deprivation in Scotland: secondary analysis of the Scottish Index of Multiple Deprivation 2003. Edinburgh: Scottish Neighbourhood Statistics Development Group, 2004.
18. Sturgeon SR, Graubard BI, Schairer C, McAdams M, Hoover RN, Gail MH. 2003. Population-density and county-level variation in breast cancer mortality rates among white women residing in the Northeastern and Southern United States. Cancer Causes and Control 2003; 14: 923-931.
19. McLoone P. Suicide and deprivation in Scotland. BMJ 1996; 312: 543-544.
20. Gunnell D, Peters T, Kammerling M, Brooks J. The relation between parasuicide, suicide, psychiatric admissions, and socio-economic deprivation. BMJ 1995; 311: 226-230.
21. Whitley E, Gunnell D, Dorling D, Davey Smith G. Ecological study of social fragmentation, poverty and suicide. BMJ 1999; 319: 1034-1037.
22. Gunnell D, Middleton N, Whitley E, Dorling D, Frankel S. Why are suicide rates rising in young men but falling in the elderly? A time-series analysis of trends in England and Wales 1950-1998. Social Science and Medicine 2003; 57: 595-611.
23. Bentham G. Mortality rates in the more rural areas. Area 1984; 16: 219-226.
24. Shouls S, Congdon P, Curtis S. Modelling inequality in reported long term illness in the UK: combining individual and area characteristics. Journal of Epidemiology and Community Health 1996; 50: 366-376.
25. Smailes PJ, Argent N, Griffin TLC. Rural population density: its impact on social and demographic aspects of rural communities. Journal of Rural Studies 2002; 18: 385-404.
26. Irving HW, Davidson RN. A working note on the measurement of social interaction. Transactions of the Barnett Society 1973; 9: 7-19.
27. Mitchell CJA. Making sense of counterurbanization. Journal of Rural Studies 2004; 20: 15-34.
28. Stockdale A, Findlay A, Short D. The repopulation of rural Scotland: opportunity and threat. Journal of Rural Studies 2000; 16: 243-257.
29. Lindsay C, McCracken M, McQuaid RW. Unemployment duration and employability in remote rural labour markets. Journal of Rural Studies 2003; 19: 187-200.
30. Philo C, Parr H, Burns N. Rural madness: a geographical reading and critique of the rural mental health literature. Journal of Rural Studies 2003; 19: 259-281.
31. Cloke P. On 'Problems and solutions'. The reproduction of problems for rural communities in Britain during the 1980s. Journal of Rural Studies 1993; 9: 113-121.
32. Dixon J, Welch N. Researching the rural-metropolitan health differential using the 'social determinants of health'. Australian Journal of Rural Health 2000; 8: 254-260.
33. Kane CF, Ennis JM. Healthcare reforms and rural mental health: severe mental illness. Community Mental Health Journal 1996; 32: 445-462.
34. Parr H, Philo C, Burns N. Social geographies of rural mental health: experiencing inclusion and exclusion. Transactions of the Institute of British Geographers 2004; 29: 401-419.
35. Stark C, Belbin A, Hopkins P, Gibbs D, Hay A, Gunnell D. Male suicide and occupation in Scotland. Health Statistics Quarterly 2006; 29: 26-29.
36. Stark C, Gibbs D, Hopkins P, Belbin A, Hay A, Selvaraj S. Suicide in farmers in Scotland. Rural and Remote Health 6: 509. (Online) 2006. Available: http://rrh.org.au (Accessed 19 June 2007).
Abstract
Introduction: Suicide rates among men have increased in Scotland while falling in neighbouring countries. A national suicide prevention strategy has been produced. Previous work found that some rural areas of Scotland had higher than average rates of male suicide and undetermined deaths. This article describes the association between population density and suicide and undetermined death rates in Scotland.
Methods: Anonymised information on deaths from suicide and undetermined cause in Scotland were obtained from the General Registrar Office for 1981-1999, including information on postcode sector. Each postcode sector was assigned a deprivation and population density score. Loglinear models were used to examine the effects of time period (grouped into four periods), deprivation quintiles, population density (grouped into four categories) and their interactions in each sex in three age groups. A significance level of 5% was used throughout. Adjusted rate ratios and 95% confidence intervals were based on models that included only significant factors and interactions.
Results: In men, there were higher rate ratios in the most densely populated and least densely populated quartiles, with intermediate rate ratios in other areas. There was no association with population density in women aged less than 25 years, a similar pattern to men in 25-44 year old women, and lower rates in rural areas in older women. Higher levels of deprivation were associated with higher rate ratios of suicide in both sexes and all age groups. Rate ratios over time increased in younger men and women, remained stable in older men, and declined in older women.
Conclusions: Deprivation is associated with higher rates of suicide and undetermined deaths at all levels of population density and in all age groups. The highest rates of suicide among men are in the most and least densely populated areas, after adjusting for deprivation. The effect is different among women, with no effect among younger women, and lower rates among older women in areas with lower population density.
Key words: age, deprivation, sex, population density, Scotland, suicide.
You might also be interested in:
2004 - Oil doom and AIDS boom in the Niger Delta Region of Nigeria



