Introduction
Snakes bite millions of people annually creating 'one of the neglected health problems of the tropics' due to a lack of antivenoms1. Contributing to this in developing nations is also deficiencies in the management of complications, transportation, hospital equipment and public knowledge of appropriate first aid, which result in a mortality rate '100-fold higher' than in developed countries2.
Snake bite is a major problem in Sri Lanka with over 32 000 being reported in the year 2000 from a population of approximately 20 million3. Many bites occur in drier, flatter regions of the country that are home to a range of viperidae and elapid species of snakes, and rural humans4. It could be expected that management of such bites would be deficient in one of such regions, the north-east, because it has endured over two decades of warfare and economic sanctions that have resulted in shortage of medical and nursing officers, facilities and medicines.
In 2005, during the relative peace of a cease fire agreement between the Government of Sri Lanka and the Liberation Tigers of Tamil Eelam (LTTE), a retrospective review of the management of snake bites in the war-torn region was undertaken at the district hospital in Kilinochchi (the regional centre for medical care).
Aim
The aim of this study was to review characteristics of snake envenomations in victims who presented to the regional hospital in Kilinochchi, Sri Lanka, the administrative centre of the north-east, between 1 January and 15 November 2005.
Methods
A retrospective review of records of snake bite victims who presented to Kilinochchi hospital from January to November 2005 was undertaken, with reference to the type of snake; age and sex of the person bitten; site of the bite; place and time of bite; time to arrival at hospital; symptoms and signs; treatment; complications of treatment; and duration of hospital stay. The review was undertaken by final year practitioners of the Medical College of Tamil Eelam as part of a curriculum of paediatrics, delivered by the named author in his role as visiting lecturer at the College and consultant paediatrician for the region.
Results
Of the 14 500 people admitted to Kilinochchi Hospital in the period of review, 303 had been bitten by snakes; 94 were women (31%) and 209 were men (69%). Age distribution was that 68 (22%) were <18 years old; 138 (45%) were between 18 and 40 years; and 97 (32%) were over 40 years. The median age of victims was 32 years, with the youngest (1%ile) being 1.5 years and the oldest (99%ile) being 79 years. The peak incidence of bites was in the harvesting season from February to March, but almost 23 bites occurred every month. The place of bite was close to the home (25%) and the rest in or around the fields. The time of the bite was during the day for 133 (44%), and at night for 168 (56%). The location of the bite on the body was on the legs for 146 (48%); on the feet 121 (39%); on the hands 22 (7%), on the arms 7 (2%) and on the toes 7 (2%).
Type of snake
Only 97 snakes (32%) were identified, of which 42 were saw-scaled vipers (43%), 14 Russell's vipers (14%), 6 cobras (6%) and 6 kraits (6%). However 29 were undistinguished vipers (30%; triangular head and short body), and 206 snakes (68%) were not identified.
Time to arrival at hospital
For 117 victims (39%) arrival at hospital was within 1 hour of the bite, and they were given antivenom immediately if the clotting time was prolonged or if there any suggestion of drooping of the eyelids (ptosis) which denoted the onset of neurological weakness. Otherwise, 145 victims (48%) arrived and were treated within 1 to 3 hours, 28 (9%) from 3 to 6 hours, and 13 (4%) arrived more than 6 hours from the time of the bite.
Clinical effect of envenomation
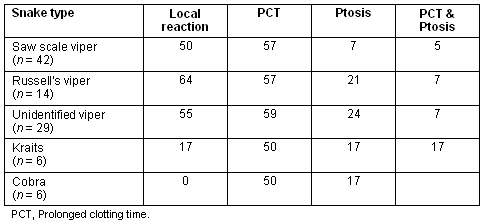
Of 303 people bitten, 145 (48%) demonstrated a local reaction of pain and swelling; 134 (44%) developed a prolonged clotting time and 46 (15%) developed ptosis. There were no local signs of envenomation in 48 of those who developed a prolonged clotting time, or in 21 of those who developed ptosis. In 20 of the people who were bitten, there was both prolongation of the clotting time and ptosis from bites of all the snakes except cobras. Respiratory failure occurred in five victims (2%) who were intubated, hand ventilated and transferred to the teaching hospital in Jaffna. Three of those bites were from unidentified snakes (one was an unidentified viper), one from a saw-scaled and one from a Russell's viper. The latter patient died. Prolonged clotting times and ptosis occurred with bites of all types of snake, and local reactions were seen in all bites except those due to cobras (Table 1).
Table 1: Percentage of victims (to nearest whole number) displaying local reactions, prolonged clotting times and ptosis, and both PCT and ptosis, after bites by saw-scale vipers, Russell's vipers, unidentified vipers, kraits and cobras
Treatment
A course of 10 vials of polyvalent snake antivenom (ASV) (Vins Bioproduct Ltd; Mumbai, India) was given intravenously at the first sign of ptosis, which denoted neurological weakness, and or a prolonged whole blood clotting time and was repeated every 6 hours as long as these signs persisted. The dose was decreased proportionally for children in accordance with their weight. In all, 183 victims received ASV, of whom 119 received one course, 44 two courses, 16 three courses, 3 four courses and one person received five courses. In all, approximately 2500 vials of antivenom were infused in the period of the study.
Reactions to the ASV were noted in 70 victims (38%). Sixty-eight victims were noted to develop a blotchy erythematous rash and six of these developed facial oedema. Two victims were recorded as having only facial oedema. The absence of any follow up of discharged patients precluded assessment of such long-term complications as serum sickness.
However, 61 patients with reactions to ASV were treated with hydrocortisone and promethazine, to which subcutaneous adrenaline was added in 56. No side effects of this therapy were noted. No differences were noted between the rates of reaction to ASV or the administration of adrenaline to victims aged <18 years, 19-40 years or >40 years (p = 0.540).
Duration of hospitalisation
The average duration was 2.6 days (not including the hospitalisation of patients referred to Jaffna). There was no age difference in the duration of stay (p = 0.078).
Discussion
Snake bite is a major problem in north-east Sri Lanka where rural dwellings, fields and forests predispose to frequent contact of humans and four of the main poisonous snakes of the island: saw-scaled and Russell's vipers, cobras and kraits. In contradistinction to other regions of Sri Lanka, bites from the hump-nosed viper were not noted in Kilinochchi.
The north-east has endured over two decades of unresolved civil conflict and there is a shortage of medical personnel and infrastructure, which could be expected to result in an increased morbidity and mortality from envenomation. However, the morbidity as revealed by time to discharge, the need for ventilatory support, and death is surprisingly low in Kilinochchi, comparing favourably with more stable and developed areas of Sri Lanka and other developing countries.
Only one victim died after admission to hospital in Kilinochchi, compared with a national death rate of 0.6%; however, in reality the death rate throughout the country is likely to be much higher because of uncounted deaths before treatment5. Case-fatality rates greater than 20% have been reported in hospitalised victims in Nepal6, 3.5% in north India, and rates of 14.6% in children and 8.2% in adults have been reported in Papua New Guinea (PNG).
The low rate of complications in Kilinochchi appears to be due to public recognition of the value of early presentation to hospital, and to a standardised regimen of therapy, enacted regardless of a shortage of medical personnel and deficiencies in medical infrastructure. In Kilinochchi, 47% of recipients of ASV had received it within 3 hours of being bitten whereas. In contrast, in PNG only 5% of victims had received ASV within 4 hours. In one centre in north India, the median time to arrival in hospital was 9 hours7. Because of early treatment, only five patients needed ventilation in Kilinochchi, compared with 82.5% of those admitted for intensive care in PNG and 75% of those bitten by elapid snakes in north India. The effect of delayed treatment was worse in children in PNG, but in Kilinochchi there was no difference in complication rate, duration of stay, amount of ASV or rate of reaction in children.
The rate of reaction to antivenom is high throughout Sri Lanka. Only one antivenom is used, a lyophilised polyvalent enzyme-refined product (from Vins Bioproduct Ltd, Mumbai) to which reactions were reported in 38% of cases in Kilinochchi, and in up to 68% to 81% of cases elsewhere. Empirical regimens of hydrocortisone and chlorpheniramine are common in Sri Lanka and are of questionable effect, but the use of subcutaneous adrenaline appears uncommon, although it has been shown to reduce the rate of adverse reactions to ASV8, and has not been shown to cause significant changes in pulse rate or blood pressure9. It was used in 92% of reactions to ASV in Kilinochchi as part of the protocol of management, and no serious reactions to the ASV or to the therapy were recorded.
Snakebites are expensive. Because of the effects of warfare and sanctions, one vial of ASV costs almost twice as much in the north-east (1200 Rupees) as elsewhere in Sri Lanka (650R or US$6.5), resulting in a total cost during the period of study of approximately US$30,000. The significance of this cost is emphasised by the daily wage of a tea plucker in Sri Lanka being approximately US$2, and by the fact that recent studies have revealed widespread wasting and stunting of children in the north-east because of undernutrition (Pers. data, J Whitehall et al, 2005).
The present study concluded that public health measures for reduction of snake bite should include removal of hiding and breeding places for snakes in and around the house because 25% of the bites occurred in that vicinity. Also, because almost 80% of bites occur on the legs and feet, field workers should wear leggings and boots, particularly in the harvest period.
Because of the relative peace under the Cease Fire Agreement, supplies of antivenom were not restricted during the period of the study; however, the current deterioration in the political situation and the resumption of armed conflict and blockade of the north-east has resulted in even greater shortages of medicines and personnel. Some 10% of all snake bites in Sri Lanka appear to occur in the north-east and the outcome is likely to be much worse if antivenom is restricted, if there is insufficient staff to ventilate a victim to the regional centre, and if the road to the tertiary hospital in Jaffna is blockaded.
Conclusion
Snake bites are common in north-east Sri Lanka and are an expensive challenge to public health. The complication rate, however, has been markedly reduced compared with other developing countries, due to public recognition of the importance of early medical care and because of standardised management which is not influenced by shortages of medical staff. Early administration of the polyvalent antivenom has reduced morbidity and mortality in all ages but is associated with a high rate of the allergic phenomena of skin rash and oedema. These side effects responded to liberal use of adrenaline without complication. The current resumption of hostilities is likely to complicate the management of snake bites by restricting access to essential medicines.
Acknowledgements
Mrs Yarlini and Arunthathy, Mr Varan, Mr Kaanthan, Mr Isaivanan and Mr Vanprasath, all medical practitioners, Medical College, Tamil Eelam, Kilinochchi, Sri Lanka are acknowledged for their fundamental contribution to this article. Due to the internal conflict in Sri Lanka, direct contact with these research assistants/participants has been interrupted.
References
1. Cheng AC, Winkel KD. Antivenom efficacy, safety and availability: measuring smoke. Medical Journal of Australia 2003; 180: 5-6.
2. McGain F, Limbo A, Williams D, Didei G, Winkel KD. Snakebite mortality at Port Moresby General Hospital, Papua New Guinea 1992-2001. Medical Journal of Australia 2004; 181: 687-691.
3. Gawarammana IB, Kularatne S, Dissanayake WP et al. Parallel infusion of hydrocortisone +- chlorpheniramine bolus injection to prevent acute adverse reactions to antivenom for snakebites. Medical Journal of Australia 2004; 180: 20-23.
4. Kasturiratne A, Pathmeswaran A, Fonseka MMD, Lalloo DG, Brooker S, de Silva HJ et al. Estimates of disease burden due to land-snake bite in Sri Lankan hospitals. Southeast Asian Journal of Tropical Medicine and Public Health 2005; 36: 733-740.
5. Fox S, Rathuwithana AC, Kasturiratne A, Lalloo DG, de Silva HJ. Underestimation of snakebite mortality by hospital statistics in the Monaragal District of Sri Lanka. Transcripts of the Royal Society of Tropical Medicine and Hygiene 2006; 100: 693-695.
6. Sharma SK, Khanal B, Pokhrel P, Khan A, Koirala S. Snake bite - reappraisal of the situation in Eastern Nepal. Toxicology 2003; 41: 285-289.
7. Sharma N, Chauhan S, Faruqi S, Bhat P, Varma S. Snake envenomation in a north Indian hospital. Emergency Medicine Journal 2005; 22: 118-120.
8. Premawardhena AP, de Silva CE, Fonseka MMD et al. Low dose subcutaneous adrenaline to prevent acute adverse reactions to antivenom serum in people bitten by snakes: randomised, placebo controlled trial. BMJ 1999; 318(7190): 1041-1043.
9. Dassanayake AS, Karunanayake P, Kasturiratne KT, Fonseka MM, Wijesiriwardena B, Gunatilake SB et al. Safety of subcutaneous adrenaline as prophylaxis against acute adverse reactions to anti-venom serum in snakebite. Ceylon Medical Journal 2002; 47: 48-49.
