There is considerable interest in community based medical education as a means of both providing medical students with access to an appropriate clinical case load and influencing their career choice towards primary care2-5. Retrospective studies, based on traditional student attachments of up to 6 weeks, have indicated this comes at considerable cost to the practices involved due to the student 'slowing down' the practice3,6-9.
To determine whether these findings also applied to longer attachments, the authors decided to investigate the financial impact of medical students in practices involved in the Parallel Rural Community Curriculum (PRCC) - a program that enables 3rd year (of a 4 year graduate entry course) medical students to undertake their entire year of clinical studies attached to a single general practice in rural South Australia10. As the doctors in these private practices are remunerated by their patients on a 'fee for service' basis, 'slowing down' or lengthening consultations for an entire year would mean significant financial losses.
Methods
Students in the PRCC are required to undertake a minimum of two formal, planned consultation sessions within the practice each week. In these sessions, the students often see patients in a separate consultation room prior to the general practitioner's consultation. For the remainder of the week, students are involved in theatre, tutorial, local hospital work, opportunistic patient contact and individual study. Thus we were able to study contiguous consulting sessions by the same doctor with, and without, a student involved in the consultation. For two separate one-week periods, at the 5 and 8 month points of their academic year, volunteer students and practitioners used separate logbooks to record: time spent with each patient; setting; patient demographics; complaint codes; investigations; and referrals. Complaint codes were modified from those developed by the University of Washington School of Medicine for their rural community attachments.
Direct observation by a research assistant 'sitting in' on the doctor's consultations was used to provide a further validation of the logbook data and to code for activities observed each minute of the consulting session using the method developed by Vinson et al9. A patient exit survey, based on questions used in the Rubin Patient Visit Rating Questionnaire11, provided a patient perspective to the quality of the consultation. As the practices studied assumed that the students would 'slow down' the practice, they booked less patients to see the general practitioner when a student was present. To account for this, a 'length of consultation' was used, rather than 'number of consultations per hour or day' as the indicative measure of productivity.
A total of 932 consultations involving 7 general practitioners, 3 practices and 4 students were sampled during the fifth and eighth month of the course. The study included 91 consultations where students were involved in the consultation, and 847 consultations with no student present. Direct observation was undertaken for 63 consultations, 28 with a student present and 37 without a student present. Ten patients (14%) chose not to have an observer present during their consultation and have been excluded from the study. No patients in the study refused to see the student. Results were analysed using SPSS software. Differences based on the presence or absence of a student in the consultation were tested using a two-tailed Student's t-test.
Results
There was no significant difference in the age, gender or presenting complaint of patients seen by the general practitioner with or without a student present. The student and practitioner log books showed that the mean length of time spent by the general practitioner per consultation decreased from 14.4 minutes to 9.5 minutes when a student was present (p<.001). The time spent by the general practitioner with the patient also decreased as the time spent by the student with the patient increased. Spearman's correlation co-efficient for this inverse association was .336 (p<.001). The third-party observational data concurred with these findings, but due to the small numbers of observed consultations, this did not reach statistical significance.
There was no significant difference in the percentage of consultations in which a referral was given when a student is present. However, when a student was present, the proportion of consultations in which a laboratory investigation was ordered increased by 15% (p<.05). Less than 10% of the consultation time was spent on student-related activities.
Other significant changes noticed in activities undertaken by the doctor during the consultation when a student was present are documented (Table 1).
Table 1: Significant changes in activities undertaken by the doctor during the consultation when a student was present, p <.05
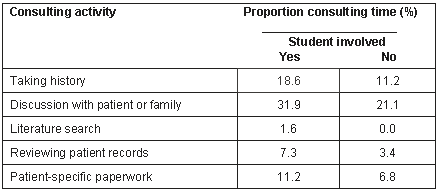
Patient satisfaction increased slightly when a student was present. This increase was not statistically significant due to the extremely high level of satisfaction that existed for all the consultations.
There were no statistically significant differences between the two reporting periods.
Discussion
There are a number of constraints on this study. It is a small study, and represents a currently unique program, with volunteer students. The methodology of direct observation intrudes into the doctor-patient relationship. This observation may influence the behaviour of both parties, but the potential change should be consistent with, or without, a student present. Although, for these reasons, some caution must be used in generalising these findings, the use of these results to generate a hypothesis for further enquiry is entirely valid.
These results challenge the traditional view that medical students are always a financial burden on rural general practices. In the study, where students had already been actively involved in all aspects of the practice for at least 5 months, we found that students appear to have a positive effect on general practitioner productivity, without any loss in patient satisfaction. This is in contrast to Vinson and co-workers9, who found that similar students were a daily financial burden on a practice for the entire period of a four-week attachment. In view of these findings, we put forward a hypothetical model of the financial impact a student has on a general practice over time (Figure 1).
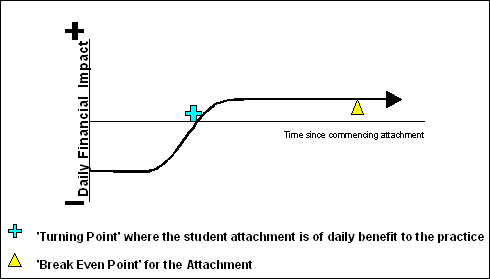
Figure 1: Hypothetical model of daily financial impact of student attachments on general practices.
This model acknowledges that for a period of time following the commencement of an attachment the practice will experience decreased income due to the time needed for the student to become familiar with the practice and for the practitioner to ensure the student has necessary skills. At some point between 4 weeks (Vinson's evidence) and 5 months (when the present authors first collected data) the student ceases to be a financial burden on the practice and becomes a financial benefit to the practice. This has been refered to as the turning point. The break-even point is the length of time needed in a practice in order for the latter financial benefit to counter the earlier loss.
Factors that may influence the location of these points may include, amongst others, the seniority and personal characteristics of the student, the curriculum expectations, the patient population, the availability (and rental cost) of a consulting room for the student, and the teaching experience of the practitioner. Our data on observed activities, and the inverse correlation between student-patient time and doctor-patient time, suggests that students are able to undertake certain time consuming tasks on behalf of the rural doctor. Payments for this extended rural teaching can then appropriately recognise the quality of the practice as a learning site and the intellectual contribution rural general practitioners make to student learning, rather than merely being an offset for income lost in the process.
With the current trend in medical schools to undertake increasing amounts of teaching in rural general practice, we suggest that it may be more economically sustainable if curricula are adapted to allow extended attachments, likely to be at least 5-6 months, rather than traditional shorter rotations. There is also evidence to support the educational validity of this approach12. Clearly, economic factors are not the only measurement used by rural general practitioners when undertaking teaching of medical students1, and more research is needed to determine the relative importance of all factors, including the attachment time, needed for the economic sustainability of rural community - based learning.
References
1. Barritt A, Silagy C, Worley P, Watts R, Marley J, Gill D. Attitudes of rural general practitioners towards undergraduate medical student attachments. Australian Family Physician. 1997; 26: S87-S90
2. Bland CJ, Meurer LN, Maldonado G, et al. Determinants of primary care specialty choice: a non-statistical meta-analysis of the literature. Academic Medicine 1995; 70: 620-641.
3. Grayson MS, Klien M, Lugo J, Visintainer P. Turning to primary care. Lancet 1995; 346: 1111.
4. Iliffe S. All that is solid melts into air: the implications of community based undergraduate medical education. British Journal of General Practice 1992; 42: 390-393.
5. Oswald N. Why not base clinical education in general practice? Lancet 1989; 2: 148-149.
6. Kollisch DO, Frasier PY, Slatt L, Storaasli M. Community preceptors' views of a required third-year family medicine clerkship. Archives of Family Medicine 1997; 6: 25-28.
7. Benefits and costs to community-based physicians teaching primary care to medical students. Journal of General Internal Medicine 1998; 13: 485-488.
8. Murray E, Jinks V, Modell M. Community-based medical education: feasibility and cost. Medical Education 1995; 29: 66-71.
9. Vinson DC, Paden C, Devera-Sales A. Impact of Medical Student Teaching on Family Physicians' Use of time. Journal of Family Practice 1996; 42: 243-249.
10. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The Parallel Rural Community Curriculum: an integrated clinical curriculum based in rural general practice. Medical Education 2000; 34: 558-565.
11. Rubin HR, Gandek B, Rogers WH. Patients' ratings of outpatient visits in different practice settings. Journal of the American Medical Association 1993; 270: 835-840.
12. Worley PS, Lines D. Can specialist disciplines be learned by undergraduates in a rural general practice setting? Preliminary results of an Australian pilot study. Medical Teacher 1999; 21: 482-484.
Published 2 March 2001; style modified and references re-ordered 17 July 2003.
Abstract
Background: Is teaching a medical student always a financial burden on rural general practice? If so, is the current trend towards increasing placement of students in rural practice sustainable? Retrospective studies of short-term attachments to rural general practice have repeatedly shown a financial cost to the practice. Might the results be different for extended attachments? This paper presents the results of a small prospective study of the financial impact of undergraduate medical students undertaking the Parallel Rural Community Curriculum, a 12 month clinical attachment to rural general practice in the Riverland region of South Australia.
Methods: Students and doctors involved in the program kept separate logs of patient contact time. These data were triangulated with third-party direct observation of consultations and an exit questionnaire on patient satisfaction.
Results: In this study, where students had already been actively involved in all aspects of the practice for at least 5 months, it was found that students had a positive effect on general practitioner productivity, without any loss in patient satisfaction.
Discussion: To account for these findings, a hypothetical model has been developed of the financial impact of a student on a rural general practice over time. With the current trend in medical schools to undertake increasing amounts of teaching in rural general practice, it is suggested that it may be more economically sustainable if curricula are adapted to allow extended attachments, likely to be at least 5-6 months, rather than traditional shorter rotations.
Key words: community-based medical education, education, general practice, medical students, student placement.
You might also be interested in:
2009 - Childhood obesity and elevated blood pressure in a rural population of northern Greece

