Introduction
In line with the need to increase the numbers of health professionals working in rural and remote areas1-3, there are now various rural health education activities underway in many undergraduate health science programs. There is compelling evidence that the strongest variable associated with the recruitment and retention of health professionals in rural communities is rural background4. In part, this association can be explained by the existing familiarity that rural background students have with rural belief and value systems. The objectives of rural health education are twofold. First, rural health education aims to capitalise on rural background students' natural affinity with rural place. Second, rural health education aims to raise non-rural students' awareness of the social, cultural, historical and economic issues that influence the health and wellbeing of people living in rural and remote areas5. As such, many undergraduate health science programs often include a rural learning opportunity, which introduces students to the unique aspects of rural practice. These rural placements generally involve '...a period of experience (usually including clinical training experience) provided to a health science undergraduate in one or more health settings in a rural area'6.
The current global and national rural workforce shortages involve all health disciplines. The evidence emerging from the medical discipline is valid and useful. It is important, however, that strategies to attract and retain health professionals from disciplines other than medicine are based on evidence that is discipline specific. Only when a rigorous, comprehensive and multidisciplinary evidence base is established, can best-practice models of rural health education be developed. These models can then be implemented to attract students from a wide variety of health disciplines to rural practice.
Rural placements rely on an experiential model of education by using the rural context as a situated framework for students to learn through action. From these experiences it is expected that students will learn about the norms, values and beliefs that underpin rural practice and rural life6-9. Gaining and building on familiarity with rural culture introduces students to the positive lifestyle opportunities available in rural areas. It is often claimed that such 'rural exposure'5 increases the likelihood of students positively evaluating rural practice as a viable career option10,11. There are, however, many confounding variables that influence students' rural intentionality that are often not accounted for in research5. As such, evidence that rural exposure increases uptake of rural practice is mixed and inconclusive5. This article responds to recent calls for a stronger evidence base for understanding the effect of rural exposure on students' intentions to take up rural practice5.
Between January 2005 and December 2006, 336 undergraduate health science students participated in a University Department of Rural Health (UDRH) supported rural placement, in a variety of locations across Tasmania. Tasmania is unique among Australian states. Its small geographical size and comparatively large rural population base has resulted in a large number of rural healthcare facilities taking students on placement. The UDRH support initiatives include accommodation and IT facilities at a number of rural locations, and payment of travel and accommodation allowances. These initiatives are implemented in recognition of the lack of suitable and affordable accommodation, an absence of IT services, and the financial cost of travel as barriers to a successful rural placement program. The locations for rural placements in Tasmania are shown (Fig1).
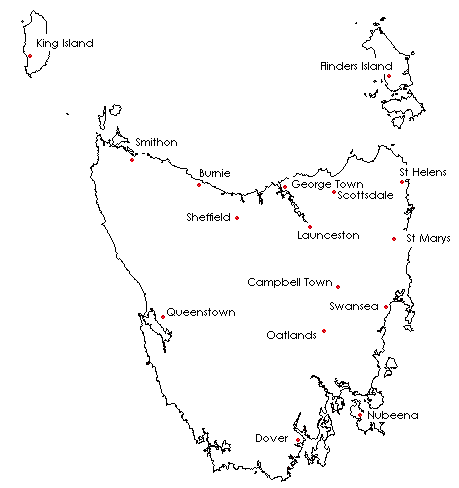
Figure 1: Geographical representation of rural placement sites in Tasmania.
On completion of rural placement in Tasmania, all students are asked to complete a survey. The objectives of the survey are to gather information about students' demographic profile, their views on rural placement experiences, and their past and future rural practice career intentions. Research questions that this article addresses include: 'Do rural placements influence undergraduate health science students' attitudes toward rural practice?' and, 'Is there an association between students' background and intention to practise in a rural location?' This article reports and discusses the findings from this survey with respect to these questions.
Methods
Design
A descriptive survey design was used to collect data. It was developed to fulfil the UDRH's reporting requirements to its funding body; the Australian Government Department of Health and Ageing. These data are also used to inform the UDRH and its key stakeholders on the relevance and value of the rural placement program.
Population and sample
The population under study consisted of undergraduate health science students from a wide range of disciplines, including nursing, medicine, pharmacy and allied health (which included audiology, nutrition and dietetics, occupational therapy, podiatry, physiotherapy, speech therapy, prosthetic and social work) who undertook a rural placement in Tasmania (n = 336).
Instrument
A survey consisting of 33 items was developed by UDRH staff. The survey contained a 10 point Likert scale and a combination of open (n = 12) and closed (n = 21) questions. The open questions related to demographics, satisfaction with patient numbers, the welcome and orientation to the agency, and academic and clinical supervision. In addition, closed questions rated students' satisfaction with the UDRH accommodation, IT facilities and their intention to work rurally before and after the rural placement. The data reported in this article includes students' demographic details relating to the discipline studied, gender, citizenship status, current year of study and the primary and secondary school that students attended. It also reports students' rural career intentions prior to (retrospectively), and immediately after the placement experience. These responses were categorised as either negative (5 and below) or positive (6 and above).
Procedure
The surveys were distributed to students on commencement of their rural placements. Students returned the survey anonymously to the UDRH and survey completion was considered to be implied consent to participate in this evaluation.
In order to measure the effect of exposure to rural communities on students' intentions to work rurally, it was necessary to control, and therefore classify, the rural background variable. There are numerous potential definitions of rural background that are based on factors such as where individuals were born, or where they attended primary or secondary school12. Rural background has been broadly defined as 'any rural experience or rural exposure'13. This definition has led researchers to use postal codes14, location of primary school15 or number of years living in a rural area16 as classification categories. For the purposes of this research, a student of rural origin has been classified using the Rural Undergraduate Support and Coordination (RUSC) program definition17 as having 'at least 5 years' rural residence, consecutive or cumulative from the commencement of primary school'17. Therefore, data on primary and secondary school location was used to determine students' rural background status.
In order to examine rural background and students' claims of rural practice intentionality, some clarity of the term 'rural' was also required. The difficulties and complexities involved with defining rurality are well documented18. In this study, degree of rurality was determined using the Rural and Remote Metropolitan Classification (RRMA) system (Table 1)19. The data on primary and secondary school location were categorised using the RRMA classifications.
Table 1: RRMA classification definitions
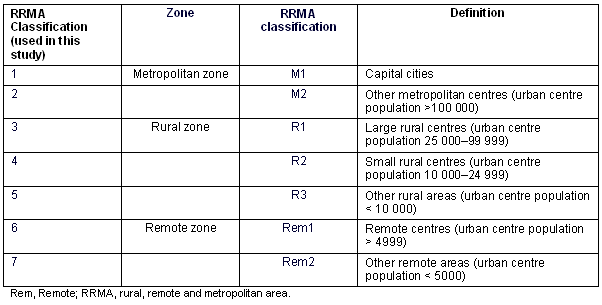
International students and those students whose answers were not able to be categorised into RRMA classifications (eg location of primary or secondary school stated as 'Western Australia') were excluded from analysis.
Data analysis
Data were analysed using the Statistical Package for the Social Sciences (SPSS Inc; Chicago, IL, USA) computer program. Five analytic tests were performed. First, frequencies of variables including gender, citizenship status and year of study were calculated. Second, rural background was cross tabulated according to disciplines, which provided a profile of participants involved in the study. Third, the mean intention to practise rurally, both prior to (retrospectively) and after the placement were compared using a paired samples t-test. The fourth test established the central tendency of the intention to practise rurally through cross tabulating the mean intention with the students' RRMA classifications. Finally, a Wilcoxon signed rank test was performed to show the direction of change (whether positive or negative) in students intention to practise rurally.
Results
Of 336 students who undertook a UDRH supported rural placement in Tasmania during January 2005 and December 2006, a total of 239 students completed the survey, a response rate of 71%. The demographic details relating to students gender, citizenship status, and current year of study are presented (Table 2).
Table 2: Participants' demographic details according to discipline of study
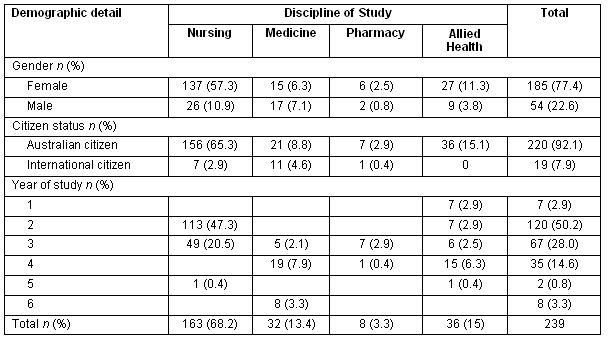
The largest cohort of respondents was female nursing students (57.3%), and 92.1% of respondents were Australian citizens. The majority of students were in their second (50.2%) or third (28.0%) year of study.
Using the RRMA classification system, Australian students' background status is presented (Table 3). These results are presented according to students' discipline of study. For Table 3, n = 203 because it was not possible to allocate an RRMA classification to all students.
Table 3: The RRMA classification of students with Australian citizenship
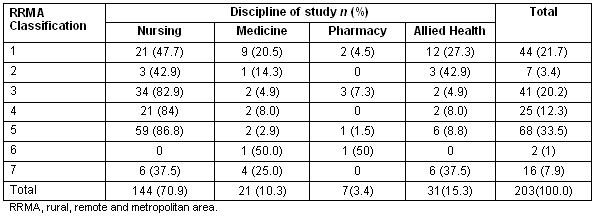
The greatest proportions of respondents attended primary and secondary schools in areas classified as RRMA 1 (21.7%) and RRMA 3 (20.2%).
Students' intentions to work rurally prior to (retrospectively) and after placement according to the discipline being studied were analysed using a paired t-test, as presented (Table 4).
Table 4: Students' mean intention to practise rurally prior to (retrospectively) and after placement, according to discipline
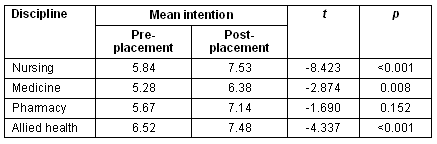
These results show that the average reported intention to practise rurally significantly increased after the placement for nursing, medicine and allied health students. While pharmacy students' reported intention to practise rurally increased post-placement, these results were not significant at the p ≤0.05 level.
Students' intentions to work rurally prior to (retrospectively) and after placement according to RRMA classification were analysed using a paired t-test, as presented (Table 5).
Table 5: Students' intentions to work rurally pre- and post-placement according to RRMA classification system
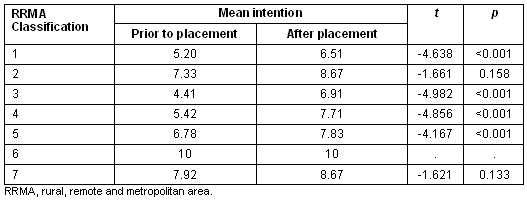
These results show that the average intention to practise rurally significantly increased after placement for students from RRMA classifications 1 and 3-5. Only two students came from RRMA classification 6 areas, and both these students stated a pre-placement and post-placement intention of 10, rendering comparison meaningless. While the mean intention to practise rurally increased for students categorised as coming from RRMA classifications 2 and 7, the difference in means were not significant at the p ≤0.05 level. It is, however, worth noting that students indicated a high level of intention to practise rurally, as stated both prior to and after placement for RRMA classifications 2 and 7. This information is visually presented (Fig2); the graphic spike for RRMA classification 6 is explained above.
A Wilcoxon signed ranked test was performed on the paired data to show the direction of change in students' intention to practise rurally. These results are presented (Table 6). For Table 6, n = 209 because not all students provided a ranking for their intentionality prior to and after the rural placement, and subsequently only paired data are reported.

Figure 2: Graph of students' mean intention to practise rurally prior to (retrospectively) and after placement, according to rural background.
Table 6: Direction of change in students' rural intentionality
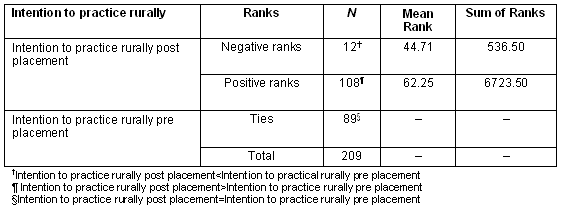
The Wilcoxon signed ranks test indicates that 12 students' (6%) intention to practise rurally decreased after rural placement. However, 108 (52%) of students' intention to practise rurally increased after their placement and 89 (42%) students' intention to practise rurally did not change.
Discussion
The results of this study show that across all disciplines students' intentions to work rurally increased after rural placement, although the results for pharmacy students were not significant. Numerous studies concerning the determinants of rural practice uptake have been conducted over the past decade. The results from this study contrast with research that reports undergraduate exposure to rural practice is not associated with intention to practise rurally4,20,21. Instead, these results support research reporting exposure to rural practice during undergraduate studies is an important positive influence on students' intentions to work rurally22-24.
The length of rural exposure may be one reason why changes in intention to practise rurally for pharmacy student in this study were not significant. In Tasmania, most disciplines undertake rural placements for a minimum of 2 weeks (medicine) and up to 6 weeks (nursing and allied health students). In contrast, while fourth year students can volunteer to undertake a 12 week clinical rotation in a rural location, most Tasmanian pharmacy students are only required to undertake 5 days of rural placement. While these findings might concur with research reporting longer rural rotations increases the likelihood of practising in a rural area5, it is a finding that requires further investigation. Our study had a small cohort of pharmacy students and greater detail regarding the length and nature of the rural placement is required.
The data from our study provide important justification for improving the efficiency of rural placements in Tasmania as a multidisciplinary rural health workforce supply strategy. Our data analysis suggests that across all health science disciplines, students' average intention to practise rurally increased after rural placement. While these findings augment similar research, most of this work has been exclusively within the discipline of medicine25-30. In disciplines other than medicine, only a few studies report students intentions to practise rurally as an outcome of rural exposure24,31,32.
The results of this study suggest that providing rural and remote clinical experiences for undergraduate nursing, medicine, pharmacy and allied health students, offers rural workforce recruitment possibilities. At present, the nursing, pharmacy and allied health disciplines do not receive the same level of Commonwealth funding that is available for schools of medicine to support rural health education initiatives32. An effective public health approach would include the support of professionals from all health disciplines to achieve better rural health outcomes.
Our results also show that across four RRMA classifications, students' average intention to practise rurally significantly increased. A small number of students' intentions either did not change or decreased. The recruitment of health professionals in rural communities is affected by numerous factors. These include rural exposure during undergraduate training, spousal commitments and opportunities, professional opportunities and lifestyle factors20. Of all these factors, rural background has been found to be most strongly associated with rural practice uptake4,33-36. Through taking into consideration rural background as an influence on intention to practise rurally, this study supports other research reporting that rural placement may be an important rural workforce recruitment strategy for all health disciplines22,24.
All research has limitations that must be acknowledged. The major limitation of this study is that the tool used to collect data has not been validated. The tool is currently being redeveloped and will be subjected to validity and reliability tests. Two Australian questionnaires37,38 have been published to assist researchers with measuring students' attitudes to working and living in rural areas. These questionnaires are designed for medical students who are participating in rural clinical school programs. In Tasmania, large numbers of students from a variety of health disciplines undertake rural placements independently from the Rural Clinical School program. It was therefore necessary to develop a questionnaire that could be used as a multidisciplinary tool for measuring the impact of rural placements on students' rural career aspirations.
In this study, students with a strong rural background reported higher intention to work rurally, than their urban counterparts, both pre- and post-placement. However, the effect of increased intentionality, post-placement was particularly powerful for urban background students who, as others have found39, after rural placement indicated a greater positive shift in their intentionality to work rurally. Existing rural health education models are targeted more towards students with a rural background. The results of this study suggest that greater emphasis should be placed on urban background students for their rural workforce recruitment potential.
Conclusion
The value of rural placements as a method for increasing health science students' intentionality to take up rural practice as a positive and viable career option is demonstrated by this study. A number of previous studies have examined students' intentions to work rurally after undertaking a rural placement. These studies are mostly from the medical discipline. However, this study involved undergraduate students from a range of health disciplines. Results show that across four disciplines, students' average intention to practise rurally significantly increased after rural placement. Many of the early studies of students' rural intentionality do not control for independent variables such as the influence of background. This study used the RRMA classification system to categorise students' background status by examining the location of their primary and secondary school education. This study provides further evidence on the role of rural placements in favourably influencing students' intention to work rurally. However, further research investigating the effects of providing students with a variety of rural and remote experiences, other than rural workforce recruitment, is needed.
References
1. Australian Health Ministers' Conference. National Rural Health Strategy Update. Canberra: Australian Government Publishing Service, 1996.
2. Australian Health Ministers' Conference. Healthy Horizons 1999-2003: A Framework for Improving the Health of Rural, Regional and Remote Australians. Canberra: Australian Government Publishing Service, 1999.
3. Australian Health Ministers' Conference. Healthy Outlook 2003-2007: A Framework for Improving the health of rural, regional and remote Australia. Canberra: Australian Government Publishing Service, 2003.
4. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160: 1159-1163.
5. Ranmuthugala G, Humphreys J, Solarsh B, Walters L, Worley P, Wakerman J et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Australian Journal of Rural Health 2007; 15: 285-288.
6. National Rural Health Alliance. A Quality Rural Placement System for Health Students. National Rural Health Alliance, 2004. Position Paper, p 3.
7. Hays R. Pulling rural training initiatives together. The Medical Journal of Australia 2001; 174(8): 428.
8. Hays R. Developing health education to address recruitment and retention issues. Proceedings World Rural Health Conference; 1-3 May 2002; Melbourne, VIC; 2002.
9. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The Parallel Rural Community Curriculum: an integrated clinical currculum based in rural general practice. Medical Education 2000; 34: 558-565.
10. Hays R. Establishing successful distributed clinical teaching. Australian Journal of Rural Health 2005; 13: 366-367.
11. Hays R, Gupta T. Ruralising medical curricula: the importance of context in problem design. Australian Journal of Rural Health 2003; 11: 15-17.
12. Owen J, Conaway M, Bailey B, Hayden F. Predicting Rural Practice Using Different Definitions to Classify Medical School Applicants as Having a rural Upbringing. The Journal of Rural Health 2007; 23(2): 133-140.
13. Laven G, Beilby J, Wilkinson D, McElroy H. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
14. Hensel JM, Shandling D, Redelmeier D. Rural medical students at urban medical schools: Too few and far between? Open Medicine 2007; 1(1): 1-23.
15. Somers G, Strasser R, and Jolly B. What does it take? the influence of rural upbringing and sense of rural background on medical students' intention to work in a rural environment. Rural and Remote Health 2007; 7(706): 1-11.
16. Smith S, Edwards H, Courtney M, Finlayson K. Factors influencing student nurses in their choice of a rural clinical placement site. Rural and Remote Health 1: 89. (Online) 2001. Available: http://www.rrh.org.au (Accessed 7 July 2008).
17. Anon RUSC funding parameters and draft reporting framework. (Online) no date. Available: http://som.flinders.edu.au/FUSA/GP-Evidence/rural/frame/RUSC%20Parameters%20and%20draft%20reporting%20framework.pdf (Accessed 1 September 2007).
18. Halfacree K. Locality and social representation: space, discourse and alternative definitions of rural. Journal of Rural Studies 1993; 9(1): 23-37.
19. Australian Institute of Health and Welfare. Rural, regional and remote health: a guide to remote classifications. AIHW cat no PHE 53. Canberra, ACT: AIHW, 2004.
20. Xu G, Veloski J, Hojat M, Politzer R, Rabinowitz H, Rattner S. Factors influencing physicians' choices to practice in inner-city or rural areas. Academic Medicine 1997; 72(Suppl10): S109-S111.
21. Veitch C, Underhill A, Hays R. The career aspirations and location intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural and Remote Health 2006; 6(537): 1-8.
22. Chan B, Degani N, Chrichton T, Pong R, Rourke J, Goertzen J et al. Factors influencing family physicians to enter rural practice. Canadian Family Physician 2005; 51: 1246-1247.
23. Eley D, Young L, Shrapnel M, Wilkinson D, Baker P, Hegney D. Medical students and rural general practitioners: congruent views on the reality of recruitment into rural medicine. Australian Journal of Rural Health 2007; 15(1) 12-20.
24. Larson A, Playford D, Wheatland B. Wither rural health students: Methodology and preliminary analysis of the student tracking project Western Australia Geralton, WA: Combined Universitites Centre for Rural Health, 2004.
25. Rabinowitz H, Diamond J, Hojat M, Hazelwood C. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. The Journal of Rural Health 1999; 15(2): 212-218.
26. Rabinowitz H, Diamond J, Markham F, Hazelwood C. A program to increase the number of family physicians in rural and underserved areas: Impact after 22 years. Journal American Medical Association 1999; 281(3): 255-231.
27. Wilkinson D, Birks J, Davies L, Baker P. Preliminary evidence from Queensland that rural clinical schools have a positive impact on rural intern choices. Rural and Remote Health 2004; 4(340): Available: www.rrh.org.au (Accessed 7 July 2008).
28. Woloshuk W, Crutcher R, Szafran O. Preparedness for rural community leadership and its impact on practice location of family medicine graduates. Australian Journal of Rural Health 2005; 13: 3-7.
29. Woloshuk W, Tarrant M. Does a rural educational experience influence students' likelihood of rural practice? Impact of student background and gender. Medical Education 2002; 36: 241-7.
30. Woloshuk W, Tarrant M. Do students from rural backgrounds engage in rural family practice more than their urban-raised peers? Medical Education 2004; 38: 259-261.
31. Murphy B, McEwen E, Hays R. The University of Sydney Rural Careers Project: a nursing perspective. Australian Journal of Rural Health 1994; (3) : 20-24.
32. Neill J, Taylor K. Undergraduate nursing students clinical experiences in rural and remote areas: recruitment implications. Australian Journal of Rural Health 2002; (10) : 239-243.
33. Barer M, Stoddart G. Toward integrated medical resource policies for Canada: geographic distribution of physicians. Canadian Medical Association Journal 1992; 147(5): 617-623.
34. Rourke J, Rourke L. Rural family medicine training in Canada. Canadian Family Physician 1995; 41: 993-1000.
35. Rourke J. Politics of rural health care: Recruitment and retention of physicians. Canadian Family Physician Journal 1993; 148(8): 1281-1284.
36. Curran V, S Bornstein, M Jong, L Fleet. Rural medical education: a review of the literature. Newfoundland: University of Newfoundland, 2004
37. Adams M, Dollard J, Hollins J, Petkov J. Development of a questionnaire measuring student attitudes to working and living rural areas. Rural and Remote Health 5: 327. (Online) 2005. Available: http://www.rrh.org.au (Accessed 7 July 2008).
38. DeWitt D, McLean R, Newbury J, Critchley S. Development of a common national questionnaire to evaluate student perceptions about the Australian Rural Clinical Schools Program. Rural and Remote Health 5: 486. (Online) 2005. Available: http://www.rrh.org.au (Accessed 7 July 2008).
39. Tolhurst H, Adams J, Stewart S. An exploration of when urban background medical students become interested in rural practice. Rural and Remote Health 2006; 6(452): 1-11.
Abstract
Introduction:
Each year growing numbers of undergraduate health science students, from a variety of disciplines, participate in a University of Tasmania Department of Rural Health supported rural placement program in Tasmania. This study aimed to investigate the influence rural placement and rural background had on students' intentions to live and work in a rural or remote location after graduation.Methods: Between January 2005 and December 2006, 336 students participated in the placement program. Students were requested to complete a survey at the completion of their placement. A response rate of 239 was achieved (71%). The survey measured students' stated rural career intentions and rural background status according to location of primary and secondary school attendance. A demographic analysis of respondents was undertaken and results cross tabulated according to the rural, remote and metropolitan area (RRMA) classification system. Statistical analyses, including paired t-tests and a Wilcoxon signed rank test, were conducted to compare reported mean intention to practise rurally both prior to and after placement.
Results: The results from this survey show that rural placements in the undergraduate health science programs have a predominantly positive influence on students' intention to work in a rural community post-graduation. While these findings were significant for the disciplines of nursing, medicine and allied health, the results were not significant for pharmacy students. Students' average intention to practise rurally significantly increased after the placement for students from RRMA classifications 1 and 3-5.
Conclusion: The value of rural placements as a method for increasing health science students' intentionality to take up rural practice as a positive and viable career option is considerable.
Key words: allied health, Australia, career intentions, medical, nursing, pharmacy, placements, Tasmania, undergraduate.


