Introduction
The World Health Organization (WHO) defines menopause as 'the permanent cessation of menstruation as a result of the loss of ovarian activity'1. Menopausal period has an important role in the reproductive life of a woman and gives rise to many physical and mental problems. Life expectancy is increasing age at menopause remains relatively unchanged, so women are spending more of their life in the post-menopause period. Changes in menopause experience for women in different parts of the world and in different ethnic groups provide evidence for specific cultural and ethnic impacts of menopause. As such, healthcare workers need significant information on menopause in order to be able to plan healthcare services2,3.
The menopause rating scale (MRS) is a health-related quality of life scale, developed in Germany (by The Berlin Center for Epidemiology and Health Research) in the early 1990s4. Its intent was to measure the severity of aging-symptoms and their impact on the quality of women's lives. The MRS is well accepted internationally. Translations have been performed following international methodological recommendations for the linguistic and cultural adaptation of HRQoL instruments5. The first translation was from the original German into English. The English version was used as the source language for translations into the French, Spanish, Swedish, Mexican/Argentine, Brazilian, Turkish, and Indonesian languages6-8.
For the Turkish version of MRS, reliability estimation was performed by two studies in Turkey with low sampling rates: the study of Heinemann K et al. covered 9 countries and included 30 Turkish women9; Bekiroglu et al. studied 60 women who were referred to the menopause clinic of a hospital in İstanbul10. The outcomes of these two urban studies were similar to those from other countries. Another unvalidated study of the MRS in rural areas was conducted by Budakoğlu11.
Turkey is a middle-income country that has experienced substantial economic growth over the past 50 years. It has a high rate of migration from rural to urban areas. The 65 years and over age group comprises 7% of the total urban population, but 9% in rural areas. Compared with urban areas, rural Turkey is characterised by low education levels and high unemployment rates. According to Turkey's National Burden of Disease cost-effectiveness study, total Disability Adjusted Life Year DALY values for rural women are higher than for urban women and rural men12.
In the rural areas of Turkey, healthcare services are offered mainly in primary healthcare centers, and maternal and child healthcare centers operated by the Ministry of Health. Basic health services in these clinics are primarily provided by GPs, midwives and nurses12.
As is the case in many developing countries, it is difficult for women living in rural Turkey to obtain access to healthcare services, and this is due to insufficient numbers of midwives and physicians, reduced quality of healthcare services, difficulties in travel to city centers for economic reasons, low education level, and poverty. The prevalence of inability to reach health services among women is a gender issue in Turkey11-14. Determining the applicability of the MRS as a screening test for rural women would assist rural healthcare workers to identify women with severe menopausal symptoms and to refer them to secondary level physicians (gynecologists) for appropriate medical attention.
The objectives of this study were to: test the validity and reliability of the MRS in rural areas of Turkey; determine estimation values for referral to the secondary level of health care; use a screening test for the identification of women with severe menopausal symptoms in rural areas; and assess the prevalence of severe menopausal symptoms among rural Turkish women.
Methods
Study design
The study was conducted in geographic areas with rural characteristics in Central Anatolia, in the Eskisehir region of Turkey. Eskisehir is among the more developed provinces of Turkey but its rural areas remain underdeveloped. The main regional sources of income are farming and livestock breeding. The literacy rate is 95%, and 93% of the population has social security. Within the scope of the Health Transformation Program in the region, a Family Medicine System was established in 2008 and 15 public health centers (PHCs; 4 urban and 11 rural) were founded, providing preventive health care.
At the commencement of the study, the sample size was estimated at 600 (confidence interval = 95%, d = 4%, in women >40 years, assuming the frequency of menopausal symptoms to be 50%). A stratified random sample was drawn using two-stage stratified sampling methodology, during a 6 month period from June to November 2008. In the first stage, the rural area of Eskisehir was divided into 11 PHC strata, with 2 of those PHCs (Alpu and Beylikova) selected randomly. The population consisted of 2878 women aged 40-70 years, identified using the medical records of the two PHCs. In the second stage, interviewers visited mapped areas of the selected PHCs and made a list of the streets in each PHC. A random number table was used to select the first house to be visited in each street, and the targeted number of women from each area was reached by visiting one house out of every five.
Study population
A total of 600 women were enrolled in the study. The age range of the women was 40-70 years and the median age was 52.01±9.04 years. Approval of the local committee and verbal consent from the participants were obtained.
All enrolled women were visited in their homes and the questionnaire was completed during face-to-face interviews. The women were asked to complete the MRS and the Kupperman index7,15,16. A subgroup of 150 women (one-quarter) was randomly selected from the study population to conduct a reliability assessment. Women were excluded from the subgroup if they had had surgical menopause. After 15 days, a second interview was performed with 124 of the 150 women in peri-menopause and post-menopause, to comply with the test-retest method. The remaining 26 women did not participate in the second interview due to their absence from home at the time of the visit (n=19) or an inability to obtain informed consent (n=7).
Survey instruments
Data were collected using a two-part questionnaire. Part 1 dealt with background variables including socio-demographic, reproductive, and menopausal characteristics of the women17. Women were also asked if they had any medically diagnosed chronic diseases, and they rated their own general health status. Part 2 consisted of the MRS and Kupperman index6,8,15,16. For assessment of menopausal symptoms, the 11 item Turkish version of the MRS was used. Three dimensions were extracted from the menopausal symptoms: somatic, psychological, and urogenital symptom complexes. A 5 point rating scale allowed the women to describe the perceived severity of symptoms for each item (severity: 0 = no complaints to 4 = very severe symptoms). The composite scores for each dimension (sub-scale) are based on adding the item scores in the respective dimensions.
The Kupperman index serves as an indicator of climacteric symptoms16,18. This index was compared to the MRS to assess the validity of the MRS15,18.
Statistical analysis
Data were analyzed using the Statistical Package for the Social Sciences v 13.5 (SPSS Inc; Chicago, IL, USA; www.qrsinternational.com). Reliability of the MRS was evaluated using Cronbach's alpha as an indicator of internal consistency, with coefficients above 0.70 considered acceptable. Cronbach's alpha was evaluated in conjunction with item-total correlations. Corrected item-total correlations indicate the degree to which an individual item relates to the total score, excluding the item in consideration. Correlations below 0.15 were considered low and indicated that the item should be considered for deletion. Correlations were expected to range from 0 to 0.40, with correlations above 0.30 considered good19. The test-retest correlation coefficients were calculated using Pearson's correlation to provide evidence of good temporal stability of the total scale.
Concerning the objective to assess the use of MRS as screening test in a rural area, the impact of the MRS in regard to the decision to seek medical advice due to menopausal symptoms was considered the validity criterion, and sensitivity and specificity of the test were established according to this variable20. The reference standard was seeking medical advice due to menopausal symptoms. A receiver operating characteristic (ROC) curve was constructed by calculating the specificity and sensitivity of MRS cut-off values, and the area under the curve (AUC) was computed. The optimal cut-off point was defined as the point at which the sum of sensitivity and specificity was maximal21.
The severity of menopausal symptoms was at first compared according to background characteristic categories, using the χ2 test and an un-adjusted logistic regression model. Multiple regression models were applied in the second step to identify independent risk factors for the severity of menopausal symptoms. Variables with p-values greater than 0.10 were not included in the stepwise model.
Results
Study population
Table 1 presents the characteristics of the study group, the mean age of which was 52 years (SD=9.04). Of the 600 women, 347 (57.8%) were going through natural menopause, and 47 (7.8%) were menopausal due to surgical intervention.
Table 1: Respondents' demographic characteristics
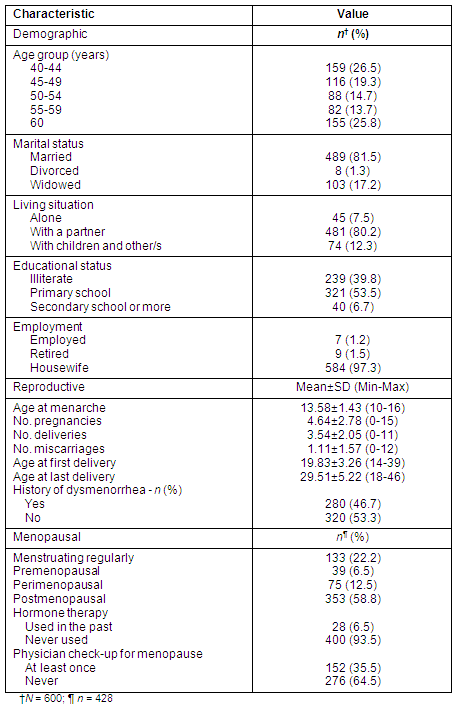
While 152 women (35.5%) had been referred to a gynecologist at least once due to menopausal symptoms, only 28 women (6.5%) had received hormone replacement treatment for more than 6 months. A total of 399 women (66.5%) reported their self-rated general health status to be poor, while 201 (33.5%) described their health status as good. There were only 195 women (32.5%) with no physician-diagnosed chronic disease.
Reliability of the menopause rating scale test
An evaluation of the reliability of the MRS test in determining the need to refer rural women to a gynecologist at least once, due to the severity of menopausal symptoms, was carried out on 124 women. Women included in this section of the study were peri-menopausal and postmenopausal and their average age was 57.7 years (SD=7.4). Other sociodemographic characteristics (marital status, lifestyle, occupation, level of education) proved to be no different from those of the main study group (p >0.05).
Internal consistency for the MRS (Cronbach's alpha) was estimated via test-retest reliability. While the Cronbach's alpha value for women in the study group was 0.81, it was found to be 0.87 in the re-test group (n=124). Item-total correlations were not lower than 0.30 except for a single item ('physical and mental exhaustion' was 0.27; Table 2).
Table 2: Reliability of the Turkish version of the menopause rating scale
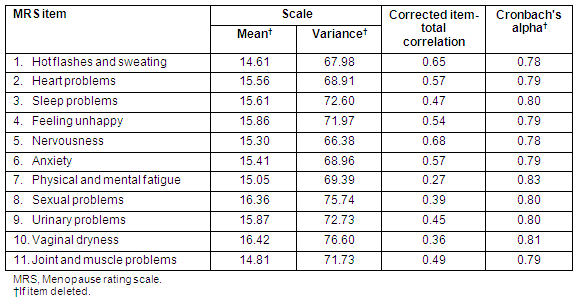
When checking the test and retest scores, a positive correlation was found between total scores (Pearson correlation coefficient r=0.93, p=0.000). A similar correlation was demonstrated for the sub-scale scores of the MRS (somatic scale: r=0.896, p=0.000; psychological scale: r=0.881, p=0.000; urogenital scale: r=0.837, p=0.000).
Validity of the menopause rating scale test
In order to assess the validity of the scale, its association with the probability of rural women visiting a gynecologist at least once due to the severity of menopause symptoms was evaluated. The mean MRS score in women referred to a gynecologist (M±SD = 17.14±8.02) was found to be higher compared with the score of women who were not referred (M±SD = 13.95±8.86) (t=3.066, p=0.002). The average subscale scores were also higher in women who had visited a gynecologist (Table 3).
Table 3: Comparison of menopause rating scale scores and its domains according to having visited a gynecologist due to the severity of menopause symptoms
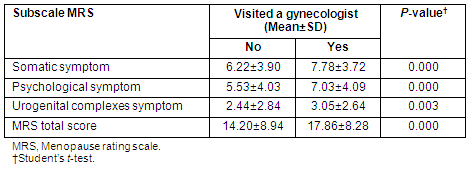
In the second step of the validity analysis, the correlation of the MRS with the Kupperman index was examined. The results of the analysis revealed a positive correlation (r=0.86, p=0.0000).
Menopause rating scale estimation value
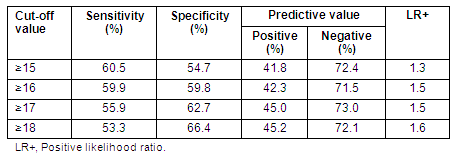
The estimated value of the MRS score that would predict whether a woman had visited a gynecologist at least once due to the severity of menopause symptoms was identified via ROC analysis, and found to be 16. The AUC was 0.621, with a 95% confidence interval of 0.567-0.676. When the estimated value of the MRS was defined at ≥16, and its sensitivity and specificity were both 60% (Table 4).
Table 4: Sensitivity and specificity of menopause rating scale cut-off values for predicting 'referral to a gynecologist for severe menopausal symptoms'
Variables affecting the severity of menopause symptoms in rural women
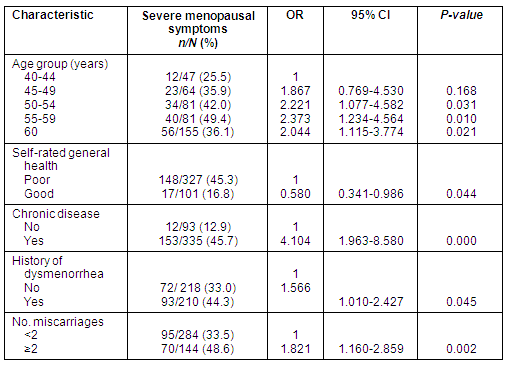
Among women living in rural areas, menopausal symptoms were deemed severe at a score of 16 and above on the MRS. In determining the variables affecting severity of menopausal symptoms, correlations with demographic, reproductive, and menopausal variables were tested through univariate analysis. Variables with a p-value <0.10 were included in the multivariate analysis. The MRS score was observed to be higher in participants who: reported their self-rated general health condition as poor; were of advanced age; had a chronic disease, a history of dysmenorrhea or had had two or more miscarriages (Table 5).
Table 5: Independent predictors for severe menopausal symptoms
Discussion
The duration, severity and impact of menopausal symptoms vary greatly from person to person and population to population22. Some population-based surveys, largely conducted among Caucasian subjects, have reported a high prevalence of menopausal symptoms at between 40% and 70%23,24. Conversely, studies of Asian women from differing ethnic backgrounds have reported lower symptom prevalence of between 10% and 50%25. The studies in Turkey showed a prevalence of 35%-90%11,26-28. Because Turkey lies geographically between the east and west, the life-styles of its population are broad and various. Some women (particularly rural women) live traditionally while others live more a 'western' style, supported by the laws of the secular republic.
Traditional life accepts menopause as a normal process, and cleanliness, maturity, the comfort of no longer menstruating and positive changes in health behaviour are concepts positively attributed to menopause. The absence of menstruation is very important for Muslim women due to religious practices, such as being able to pray in the absence of menses. Most rural women are agricultural workers. In addition, it is difficult for rural Turkish women to obtain access to healthcare service. Therefore, the experience of menopause should be assessed separately for rural women in Turkey and other developing countries.
The MRS was developed in order to monitor the clinical utility of hormone replacement therapy (HRT) by determining changes in the severity of symptoms before and after treatment, while also identifying advanced age/menopausal symptoms and measuring health-related quality of life in women of varying socioeconomic status6. The present was unique because the MRS was applied to women living in rural areas, attempting to evaluate its reliability and validity as a screening tool to identify individuals in need of specialist gynecological treatment for menopausal symptoms.
Reliability and validity are important in demonstrating the usefulness of a scale. Reliability measures (internal consistency and test-retest stability) performed thus far have shown the MRS to be a scale of acceptable quality18,29. One study reported correlation coefficients to vary between 0.60 and 0.90, confirming the acceptability of the MRS4. Also, in a test-retest study performed among randomly selected women between the ages of 45 and 65 years in Germany in 2002, Cronbach's alpha was found to be 0.70 and the correlation coefficient was 0.8230.
The item-total score correlation coefficient shows the effect of a given item on the total scale score20. In our study, the fact that correlation coefficients between test and re-test MRS total scores and Cronbach's alpha values were sufficiently high shows that the test has a high level of reliability, that is, a high ability to measure symptoms in the same manner.
Validity provides a measure of the accuracy of the collected data. For the MRS, the transcultural similarity of scale contents, the concordance of MRS scores, and its good correlation with such scales as the Kupperman index are among the validity criteria4,31,32. A study carried out in Poland, Greece, and Belarus reported a high level of correlation between the MRS and the Kupperman index (r=0.91) and found that the MRS is accepted as a modern and valuable scale in evaluating menopausal complaints33. However, direct comparisons among European/North America and Latin American countries and Asia should be considered with caution because the severity of reported symptoms seem to differ9.
In a study conducted by Bekiroğlu et al. on 60 women referred to the menopause clinic of an Istanbul hospital, the MRS was compared to the Kupperman index and Nottingham Health Profile (NHP) scales in an evaluation of validity; the MRS was found to be more reliable and more specific than the Kupperman index and the NHP10. Although the present study group had low socioeconomic and education levels, a higher correlation was observed between the MRS and the Kupperman index than was the case in other studies (r=0.86)6,10.
Because the MRS grades symptoms according to a Likert scale, a cut-off value determining whether a patient should visit a gynecologist must be identified. When the estimation value of the MRS score was defined at 16 in a simple dichotomous classification, sensitivity and specificity were both 60%. The reliability and validity of the MRS in measuring health-related effects of HRT were analyzed in various studies, and when the estimation value of the MRS score was defined at 16 in determining the success of HRT treatment, its sensitivity was 70.8% and its specificity was 73.5%6. Bearing in mind the characteristics of the study region and the purpose of the test, these sensitivity and specificity levels can be deemed sufficient. The MRS was found to be adequate for use with menopausal women by physicians or midwives in primary healthcare settings, and to channel women to gynecologists for complaints that require this level of care.
Overall, 25.3% of the study participants had visited a gynecologist at least once for menopausal symptoms (ie only one-quarter of rural area women). Of 165 women with high symptom severity based on the MRS, only 77 (46.7%) had been referred to a gynecologist, and 88 (53.3%) had not. This low referral rate calls for serious reflection. A study conducted in rural areas around Turkey's capital Ankara reported a physician referral rate of 32.9%, while another performed by Uncu et al. in a province of western Turkey (Bursa) reported a rate of 30%11,28. Access to a physician is important in that it allows women to receive medical attention apart from HRT.
Among study participants, the MRS score was higher in women who evaluated their general health condition as poor, were of advanced age, had a chronic disease, or had a medical history that included dysmenorrhea or two or more miscarriages. In a study conducted by Kakkor et al. in India, age was reported to have a remarkable impact on menopausal symptoms34. Another study by Jahanfar et al. reported higher MRS scores with more advanced age35. In the present study, the effects of age on menopause symptom severity were analyzed and found to be much higher in women aged over 50 years.
When analyzing the intensity of menopause symptoms compared with general health conditions, women who reported poor health had more severe symptoms than those in other groups; similarly, a study by Polit and LaRocco reported a high MRS score in the group with poor health36.
In this study, when evaluating the intensity of menopausal symptoms according to the presence of chronic disease, the severity of symptoms was much higher in the group with chronic disease. It may be that the symptoms of chronic disease were compounded by the symptoms of menopause.
Finally, the most significant limitation to our study was its cross-sectional design, because information about a history of visits to a gynecologist and HRT use was obtained from the women themselves. Although the MRS can be self-administered, this was not possible among our study group due to their low educational level.
Conclusion
This evaluation of the MRS indicates the instrument to be a comprehensible, useable, reliable screening test for the identification of women with severe menopausal symptoms. The intensity of menopausal symptoms depends on the presence of chronic disease, for the severity of symptoms was much higher in the group with a chronic disease than in the group with no chronic disease. It is possible for rural primary healthcare workers to identify women in need of referral to an upper-level healthcare institution (or gynecologist) by screening with the MRS.
References
1. WHO. HRP: Research on the menopause. (Online) no date. Available: http://www.who.int/reproductive-health/hrp/progress/40/prog40.pdf (Accessed 23 July 2008).
2. Twiss JJ, Hunter M, Rathe-Hart M, Wegner J, Kelsay M, Salado W. Perimenopausal symptoms quality of life, and health behaviors in users and nonusers of hormone therapy. Journal of the American Academy of Nurse Practitioners 2007; 19 (11): 602-613.
3. Rotem M, Kushnir T, Levine R, Ehrenfeld M. A psycho-educational program for improving women's attitudes and coping with menopause symptoms. Journal of Obstetric, Gynecologic & Neonatal Nursing 2005; 34 (2): 233-240.
4. ZEG Berlin. MRS - Menopause Rating Scale. (Online) no date. Available: http://www.menopause-rating-scale.info/ (Accessed 12 July 2008).
5. Schneider HPG, Heinemann LAJ, Thiele K. Menopause Rating Scale (MRS): cultural and linguistic translation into English. Life and Medical Science (Online) 2002. 3: DOI:101072/LO0305326.
6. Heinemann LAJ, DoMinh T, Strelow F, Gerbsch S, Schnitker J, Schneider HPG. The Menopause Rating Scale (MRS) as outcome measure for hormone treatment? A validation study. Health Quality and Life Outcomes 2004; 2: 67.
7. Heinemann LAJ, Potthoff P, Schneider HPG. International versions of the Menopause Rating Scale (MRS). Health Quality and Life Outcomes 2003; 1: 28.
8. Hauser GA, Huber IC, Keller PJ, Lauritzen C, Schneider HPG. Evaluation der klinischen Beschwerden (Menopause Rating Scale). Zentralbl Gynakol 1994; 116: 16-23. (In German)
9. Heinemann K, Ruebig A, Potthoff P, Schneider HPG, Strelow F, Heinemann LAJ et al. The Menopause Rating Scale (MRS): a methodological review. Health Quality and Life Outcomes 2004; 2: 45.
10. Bekiroglu N, Konyalioglu R, Ayas S, Akif A, Eren S. The Comparison of Menopause Rating Scale (MRS), Kupperman Index (KI) and Nottingham Health Profile (NHP) by means of reliability measures and responsiveness Indexes among menopausal women. Zeynep Kamil Tıp Bülteni 2008; 39(1): 11-16.
11. Budakoğlu II, Özcan C, Eroglu D, Yanık F. Quality of life and postmenopausal symptoms among women in a rural district of the capital city of Turkey. Gynecology and Endocrinology 2007; 23(7): 404-409.
12. The Ministry of Health Turkey. Health at a glance, Turkey 2007. Ankara: Refik Saydam Hygiene Center Presidency School of Public Health, 2008.
13. Ministry of Health Turkey. National Household Survey 2003, basic findings. Ankara: Ministry of Health, 2006.
14. Turkey Demographic and Health Survey. Women's characteristics and status. (Online) 2003. Available: http://www.hips.hacettepe.edu.tr/tnsa2003/data/English/chapter03.pdf (Accessed: 1 September 2009).
15. Hauser GA. Diagnosis and evaluation of climacteric symptoms. The 'Menopause Rating Scale' helps in diagnosis and evaluation of therapeutic effectiveness. Fortschr Medicine 1996; 114(5): 49-52.
16. Kupperman HS, Wetchler BB, Blatt MHG. Contemporary therapy of the menopausal syndrome. JAMA 1959; 171: 1627-1637.
17. Hurd WW, Amesse LS, Randolph JF. Menopause. In: JS Berek (Ed.). Novak's Gynecology, 13th edn. Philadelphia: Lippincott Williams & Wilkins, 2002.
18. Schneider HPG, Heinemann LAJ, Rosemeier HP, Potthoff P, Behre HM. The Menopause Rating Scale (MRS): Comparison with Kupperman Index and Quality of Life Scale SF-36. Climacteric 2000; 3: 50-58.
19. Bland JM, Altman DG. Statistics notes: Cronbach's alpha. BMJ 1997; 314: 572.
20. Wagner J, Lacey K, Chyun D, Abbott G. Development of a questionnaire to measure heart disease risk knowledge in people with diabetes: the heart disease fact questionnaire. Patient Education and Counseling 2005; 58: 82-87.
21. Youden WJ. Index for rating diagnostic tests. Cancer 1950; 3: 32-35.
22. Ayranci U, Orsal O, Orsal O, Arslan G, Emeksiz DF. Menopause status and attitudes in a Turkish midlife female population: an epidemiological study. BMC Womens Health 2010; 10(1): 1-5.
23. Nedstrand E, Pertl J, Hammar M. Climacteric symptoms in a postmenopausal Czech population. Maturitas 1996, 23: 85-89.
24. Dennerstein L, Smith AM, Morse C, Burger H, Green A, Hopper J et al. Menopausal symptoms in Australian women. Medical Journal of Australia 1993, 16: 232-236.
25. Boulet MJ, Oddens BJ, Lehert P, Vemer HM, Visser A. Climacteric and menopause in seven South-east Asian countries. Maturitas 1994; 19: 157-176.
26. Neslihan CS, Bilge SA, Oztürk TN, Oya G, Ece O, Hamiyet B. The menopausal age, related factors and climacteric symptoms in Turkish women. Maturitas 1998, 20: 37-40.
27. Discigil G, Gemalmaz A, Tekin N, Basak O. Profile of menopausal women in west Anatolian rural region sample. Maturitas 2006, 20: 247-254.
28. Uncu Y, Ozdemir HA, Bilgel N, Uncu G. The perception of menopause and hormone therapy among women in Turkey. Climacteric 2007; 10: 63-71.
29. Schneider HPG, Heinemann LAJ, Rosemeier HP, Potthoff P, Behre HM. The Menopause Rating Scale (MRS): reliability of scores of menopausal complaints. Climacteric 2000; 3: 59-64.
30. Heinemann K, Assmann A, Möhner S, Schneider HP, Heinemann LA. Reliability of the Menopause Rating Scale (MRS): investigation in the German population. Zentralbl Gynakol 2002; 124(3): 161-163.
31. Dinger J, Heinemann LA. Menopause rating scale as outcome measure for hormone treatment. Centre for Epidemiology and Health Research Berlin, Germany. (Online) no date. Available: http://www.menopause-rating-scale.info/documents/poster.pdf (Accessed 12 July 2008).
32. Alder EM. How to assess quality of life? Aspects of methodology. International Congress Series 2002; 1229: 31-37.
33. Krajewska K, Krajewska-Kułak E, Heineman L, Adraniotis J, Chadzopulu A, Theodosopoyloy E et al. Comparative analysis of quality of life women in menopause period in Poland, Greece and Belorussia using MRS scale. Advances in Medical Sciences 2007; 52(1): 140-143.
34. Kakkar V, Kaur D, Chopra K, Kaur A, Kaur IP. Assessment of the variation in menopausal symptoms with age, education and working/non-working status in North-Indian sub population using menopause rating scale (MRS). Maturitas 2007; 57(3): 306-314.
35. Jahanfar Sh, Rahim A, Reza S, Azura N, Nora S, Asma' btS . Age of menopause and menopausal symptoms among Malaysian women who referred to health clinic in Malaysia. Shiraz E-Medical Journal 2006; 7(3): 1-9.
36. Polit DF, LaRocco SA. Social and psychological correlatesof menopausal symptoms. Psychosomatic Medicine 1980; 42(3): 335-345.
