The World Health Organization estimates that by the year 2025, Canada will be one of the ten countries in the world with the highest percentage of senior citizens aged 65 years or older (seniors)1. Currently, there are 3.8 million Canadians aged 65 years and older2, and it is projected that by 2021 the senior population in Canada will reach 6.7 million, with one in four residing in a rural setting3.
Currently in Canada mental health services are publicly funded; the provincial and territorial governments provide primary jurisdiction of service delivery and the federal government funds research on mental health4. Mental health services are offered in hospitals (inpatient and outpatient) and some community mental health services are also available5.
There is inadequate knowledge regarding the prevalence, nature, and severity of mental health issues for rural senior women6,7. However, the research available in Canada suggests that senior women experience twice the rate of depression as senior men, and that overall, senior women experience higher rates of all mental health issues compared with senior men8,9. Rural senior women are not only at increased risk of experiencing depression and other mental health issues, but these difficulties can be exacerbated by inadequate mental health services, undiagnosed mental health issues, social isolation, stigma associated with mental health issues, and stress in relation to decreased income and health status, which have all been found to affect rural senior women's overall wellbeing2,7,9-12.
The limited research that has been conducted has tended to focus on identifying mental illnesses that rural senior women experience, often overlooking factors that contribute to mental health problems6,7,9. Therefore, this research, in its examination of mental health issues rural senior women experience and factors that negatively and/or positively affect rural senior women's mental health, will advance understanding of this important issue.
A secondary analysis13 was conducted on the primary study entitled Rural women's health promotion needs and resources: A photovoice perspective{11-12}. The purpose of the primary study was to identify the health promotion needs and resources of rural senior women. Secondary analysis is a research technique employed to re-analyze previously collected data with a new research question11-13. Secondary analysis was employed in this research study as the method allowed for more in-depth exploration of an emerging issue that had been presented in the primary study but had not been directly addressed. For this research, the data from the primary study were re-analyzed with new research questions. The research questions for the primary study were: (i) What do older rural women experience as needs and resources related to the promotion of their health? (ii) What are the socio-cultural, economic, geographical, and community environments in which rural older women's health promotion is located?
The research questions used for the current, secondary analysis study were:
- What are the mental health issues of rural senior women in southwestern Ontario?
- What factors affect rural senior women's mental health both positively and negatively in southwestern Ontario?
Photovoice, the research approach used in the primary study, is both a methodology and a method14. The photovoice approach is a unique qualitative participatory research method where participants are provided a camera and invited to take photographs, then asked to discuss their photos, experiences, and perspectives in interviews and logbooks14. In the primary study rural senior women were given a camera and asked to take pictures of what they viewed as social and health promotion needs and resources in their community, and give the pictures titles.
Participants
Participants were recruited from four rural communities in southwestern Ontario which will be called community A, community B, community C, and community D. There are numerous definitions of 'rural', but in this study, rural was defined as living 'outside of urban centres with 10 000 or more population' (p1)15. Community A and community B populations were less than 1000. Community C population was 1020, and community D had the largest population with 7069 residents. The distance from an urban centre for each community ranged from 15.9 km to 67.5 km. Communities A, B, and C each had one group of participants, with communities A and B consisting of women with European and Canadian backgrounds. In Community C the research was conducted on reserve with Aboriginal senior women. Community D included two groups of women: Mennonite women, and women from mixed white European backgrounds. Income levels for participants were: <$10,000-$19,999 (n=8); $20,000-$39,999 (n=11); $40,000-$59,999 (n=6); no data were supplied by three participants, and three participants did not complete the socio-demographic questionnaire.
Thirty-one women participated in the present study with ages ranging from 65 to 89 years, although the Aboriginal women who participated were 55 years and older due to the limited number of women aged 65 years and older on the reserve. Compared with the general population, the Aboriginal population in Canada is relatively young. Thus, those aged 55 years and older are often considered older or senior adults16. Four participants were Mennonite, five participants were Aboriginal (on-reserve), and the remaining 22 women represented mixed white European backgrounds. Aboriginal women's mental health is somewhat unique as is often influenced by their historical experiences of residential schools and reserve life16; Mennonite women's mental health may be affected by their perceptions of health, cultural experiences such as gendered roles, and lack of understanding of health services available17.
Data analysis
Participants gave written informed consent and permission for the dissemination of photos and narrative data. The data used in this secondary analysis study included 10 audiotape recordings, 27 logbooks (37 pages total), 28 socio-demographic questionnaires, 579 photographs, and 10 transcribed focus groups, which ranged from 20 to 35 pages for each group session (379 pages total). Data analysis was undertaken in four parts. First, to begin the analysis process the first author listened to all audiotaped recordings of the focus group sessions to familiarize herself with each participant's tone of voice, expressions, and perspective13. Second, analysis of the transcribed logbooks and focus group session transcripts was undertaken. The first author read through each logbook and focus group session to identify the issues and ideas that the participants' noted as affecting their mental health. The qualitative data software NVIVO v7 (www.qsrinternational.com) was used to assist the authors in categorizing and labeling this information. Third was a four-stage analysis process to examine participants' photographs12,18, similar to the process used in analyzing the photos in the primary study. Fourth, the researchers reviewed all codes and key themes for both the photographs and narrative data and determined key themes by considering common factors the women identified as affecting their mental health, as well as the intensity with which participants spoke about issues related to their mental health, and the duration.
Ethics approval
Ethical approval for the primary study was obtained from the University of Western Ontario Health Sciences Research Ethics Board (R3530A06).
Limitations of secondary analysis
There were some limitations in using secondary analysis. The first issue was that the primary researcher (first author) was not present during the primary research process, thus limiting knowledge about participants' non-verbal communication, such as their demeanor, attitudes and behaviours, that occurred during the focus group sessions. In addition, the primary researcher was not able to use probe-questions to further explore participants' mental health issues or to ask them to clarify or elaborate on their statements, and could not verify findings with the participants. To mitigate these limitations throughout the research process the primary researcher consulted frequently with the principal investigator of the primary study (second author).
An issue that became apparent early on in the research process was a lack of information about how to undertake secondary analysis19,20. Heaton, one of the leading scholars on secondary analysis, reviews previous secondary analysis studies that have been completed, but does not specifically address the methods used to undertake these secondary analysis studies13. The researcher addressed this issue by meeting with the principal investigator of the primary study several times to jointly discuss the analysis approach to take for this research.
In summary, although some limitations were encountered while using secondary analysis, with careful review of the research data and consultation with the lead investigator of the primary study, it was possible to address these limitations and use secondary analysis effectively.
Study findings that emerged from the focus group transcripts, logbooks, and photographs revealed that the key mental health issues of the study participants were loneliness and negative self-concept. Factors that positively affected their mental health included social and community resources, and personal characteristics and resources. Factors that negatively affected their mental health were inadequate resources and loss in community; and devaluing of rurality, ethnicity, and gender (Fig1).
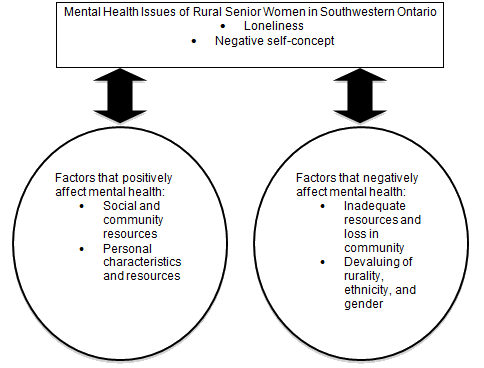
Figure 1: Mental health issues and factors that affect mental health
issues of rural senior women residing in southwestern Ontario.
Mental health issues of rural senior women
The two overarching mental health issues identified by the study participants, loneliness and negative self-concept, were discussed as follows.
Loneliness: Several of the women discussed issues related to loneliness. Many of the women talked about isolation (n=11), which often resulted from not being able to drive a vehicle; a consequence of this isolation was loneliness. Some of the women spoke about having to depend on others and not wanting to inconvenience their families because 'they had enough to worry about'. This situation often resulted in women staying at home alone because they did not want to ask their family members for transportation. As one woman noted:
Talking about it, you realize how isolated you are. You know, we're on our own.
Because of the older ages of the participants, not surprisingly many were widows. Widowhood meant being alone without their partner usually for several years, which they associated with loneliness. One woman who had recently moved her husband to a nursing home said, 'The only pain I have...I'm lonely'. Many of the participants did not have a driver's license and had depended on their husbands for transportation; therefore, the loss of their husbands often resulted in the women becoming isolated.
Negative self-concept: The second mental health issue that arose in this research related to negative self-concept. Some participants talked about not being able to praise themselves, which they viewed as the result of seldom being praised for their good work. As one woman put it, 'You were taught not to blow your own horn in our generation, so you don't do that'. In the focus groups, the behaviours of a few women illustrated that they had a negative self-concept. When asked about their backgrounds and life experiences, some women shied away from talking about themselves. For example, one woman said, 'There's nothing about me', indicating that she feels her life experiences and accomplishments are not important enough to note and, thus, reflects a negative self-concept. The Aboriginal participants spoke about issues related to children's residential schools, Indian day schools, and land ownership disputes, which for many resulted in severe emotional turmoil and often negative self-concept. One participant highlighted this in a logbook entry:
Residential schools' effect on Native people overall was horrific. On the other hand, education on the reserve was not good either. Although we had well meaning teachers, they too came with a mission to either teach us how to live like the rest of the world (we were encouraged to learn the non-native ways) or to Christianize us. I do not regret any of this teaching, it was just the way it was done. Discipline was harsh, but mostly very demeaning, very emotional and psychologically abusive.
Furthermore, many of these women noted that the psychological abuse they experienced in Indian day schools caused them to constantly try to prove to themselves they were not what teachers and administrators had told them they were. This point is illustrated by one participant who said that her grade 8 teacher would yell at the students, saying, 'Do you want to be stupid Indians all your life?', which resulted in her constantly trying to prove to herself that this was not true.
In summary, study participants experienced two mental health issues: loneliness, which was related to widowhood, isolation, and transportation issues; and negative self-concept which was related to not being able to praise themselves, undervaluing themselves, and the abuse and neglect they had experienced in the past.
Factors that positively affected rural senior women's mental health
Two main factors in the rural environment were found to positively affect the mental health of the participants: social and community resources; and personal characteristics and resources.
Social and community resources: Social and community resources emerged as an important factor affecting participants' mental health. The women took many pictures of friends and family. The titles that these women gave these pictures included 'Enjoyment of Socializing' and 'Merry Widows' (Fig2). Many of the women commented that they looked forward to seeing their friends because they were good supports to them and, as one woman put it, 'mentally [it] helps talk[ing] to others'. The importance of friendship and socializing for rural senior women was illustrated by another participant's comment:
I think all women need to get out and socialize, if you're rural and you're away from people. This gives you the opportunity ... by making new friends, you discuss new ideas.

Figure 2: Merry widows
Family was an important source of social support for many of the women. This was illustrated by the numerous pictures taken of children and grandchildren, logbook entries, and discussion during the focus groups surrounding the importance of family. Many of the women pointed out that their families helped them with daily chores, transportation, and support. As one woman put it:
My children are very helpful and will do anything I ask them to do. They check up on me daily to make sure I'm safe and healthy - I am blessed.
The resources within their communities that were listed as important for these women's mental health included community physician services, pharmacy services, grocery stores, community seniors' programs, and banking services. Having these services in town meant that study participants did not have to travel long distances, which resulted in services being more accessible and less stressful to utilize. As one woman highlighted in her logbook, 'Doctors' offices - every area needs them ... we are an aging society, medical help and assistance is a necessity'. In addition to the women's numerous comments about the importance of these resources, their significance was also highlighted by taking pictures of doctors' offices, pharmacies, banks, and community centres.
Personal characteristics and resources: The second factor that was identified as positively affecting these women's mental health was personal characteristics and resources. Resiliency emerged as an important personal characteristic and was identified as having a positive effect on their mental wellbeing. Resilience has been defined as 'flexibility in response to changing situational demands, and the ability to bounce back from negative experiences'(p23)19. The ways in which the participants expressed this personal characteristic included speaking about how they always found a way to cope with 'a bad situation' they encountered, and how they kept a positive outlook on life. This point was illustrated by one woman, who stated:
I always wanted to be a nurse ...it came up in Simcoe that the registered nursing assistant course would be given and I jumped to the ceiling ... my husband didn't want me to work even in the hospital ... he says he didn't want me to take bedpans and all that to patients. So I worked nights ... I did go and he got me pregnant. I finally got it [RNA Diploma] in 1958. So I did get it and I was very happy.
Although this participant experienced obstacles to fulfilling her dream of becoming a nursing assistant, her resilience meant she still thrived and never gave up, eventually accomplishing her dream.
A few women who had immigrated from other countries talked about the struggles they endured when they arrived in Canada and how they overcame these struggles and carried on. A Mennonite participant commented:
I was born in Mexico ... I had eight children ... we came here in 1987 - came to Ontario. Have a good life. We are going through hard times, but that's life. I am not unhappy because of circumstances. I'm glad I came to Canada.
Although these women experienced adversity in their daily lives after coming to Canada, their adaption to new ways of life demonstrates their resilience.
Regarding personal resources, many of the participating women (n=15) emphasized the importance of recreational activities and hobbies in positively affecting their mental health. For example, one woman participated in a craft circle:
I've been doing crafts for the seniors place for 17 years ... we have coffee, we crochet something ... it's good for your mental state.
Other recreational activities that these women participated in included lawn bowling, shuffleboard, swimming, and golfing (Fig3). The women noted that these activities were important because they fostered new friendships, relieved stress, exercised mind and body, facilitated relaxation, and helped them to socialize with old friends. One participant explained:
I took up golfing when I retired ... I was 60 years old and I love it. It's good exercise, fresh air and socializing with friends.
Another woman commented on the importance of joining a lawn bowling team after her husband died by saying: 'My husband passed away, and I went there and it's mentally good for you. It helped me [an] awful lot'. Other hobbies that the women enjoyed included quilting, senior craft groups, making 'dream catchers' and floral arrangements, and doing puzzles and Sudoku.

Figure 3: Actively enjoying the summer.
In summary, community and social supports and personal characteristics and resources were found to be significant protective factors against mental health issues.
Factors that negatively affected rural senior women's mental health
Two factors were identified as negatively affecting rural senior women's mental health: inadequate resources and loss in community, and devaluing of rurality, ethnicity, and gender.
Inadequate resources and loss in community: Inadequate resources and loss in community were revealed in pictures of closed signs in windows, infrastructure issues (eg cracked sidewalks), desired but unavailable recreational programs (such as an indoor swimming pool for winter recreation), and closed churches. The women titled some of these pictures 'Unforgiven Priorities', 'Sign of the Times', and 'Loss of Community Church'.
Regarding community infrastructure issues such as cracked sidewalks and poor road conditions, some participants felt that these issues resulted from inappropriate use of money by town administrators. For example, one woman wrote about this issue in her logbook and took a picture of one of the sidewalks in her community: '...uneven sidewalks where we can trip are plentiful in our town so we always have to look down instead of enjoying our surroundings'. These situations affected senior women's ability to enjoy walking on the sidewalk and maintain a healthy lifestyle.
Many of the participants also commented that there were inadequate healthcare resources in their towns, which meant they had to travel to large cities for healthcare services. This situation was stressful for women who did not drive, and the stress they experienced affected their mental health. For example, in one of the communities a drugstore had recently closed and, as one woman noted, 'Well, like I say, this is the negative in that we're losing a drug store'.
In one community, the women discussed loss in their community in regards to the loss of economic stability their town had experienced since the tobacco industry's decline, which had sustained their community's economic wellbeing for decades. This decline had a negative effect on the town's resources, which directly resulted in many stores closing. One woman commented: '...stores closing is a sign of the times and it makes me sad to see towns going'. Another woman commented on the effect of this situation on town residents: 'Well, I find that the community just gets run down.... And everybody feels bad because there's nothing in the town anymore'. In this community, the church was also closing, which had a direct effect on the mental health of many of the women in this research (Fig4). Many had years of memories of marriages, baptisms, funerals, and other events at this church. Therefore, it was difficult to consider not having this important institution in their town; as one woman pointed out: '[The] church closing ... has [caused] a lot of stress'.

Figure 4: Faith
Loss in their community was also illustrated when participants spoke about loss of relatives, friends, and other members of their communities, and was noted by several of the women as negatively affecting their mental health. In two of the communities, participants commented that cancer rates and, consequently, death rates, were very high. Participants noted that community members feel fearful and worry for the health of their families, as well as grieve the loss of those who have died. One woman stated:
Because this is a small close-knit community, everyone has known and usually has had a connection with the deceased person, so a death is very significant.
Devaluing of rurality, ethnicity, and gender: Devaluing of rurality, ethnicity, and gender was also described as negatively affecting rural senior women's mental health. Some of the women (n=7) discussed being negatively labeled according to their living environments. For example, one woman pointed out that rural people are sometimes called 'hicks', 'rednecks', or 'hillbillies', which can be hurtful. Furthermore, the Aboriginal women discussed experiencing discrimination based on their ethnic background, as one woman commented:
It can be pretty hurting...how you were treated. When I went to high school I thought I had a real good friend and we were going down the co-op to get popsicles and she says, 'Are you an Indian?' And I said, 'Ya'. She says, 'Well I 'gotta' go over here then.'
The Aboriginal women went on to speak about experiences of being discriminated against and how they felt hurt by these situations. For example, a participant explained: 'You grow up with it [covert discrimination]. You feel stuff and you feel how you're supposed to act or not act'. They also spoke about government initiatives, such as residential schools and land appropriation, that have had a great negative impact on them, their communities, and Aboriginal women in general.
Rural women not being heard in their community was also identified as negatively affecting rural senior women's mental health. Some of the women noted that they felt ignored and undervalued in their community. A Mennonite participant stated what many participants perceived: 'We got a problem because we get ignored here'. However, information about who ignored women or why they were ignored was not revealed. Participants from another focus group spoke about rural women's general lack of awareness of the importance of getting their voices heard, which caused frustration. A participant firmly emphasized, 'Just more awareness even for women that they are able to get their voices across'.
In summary, two factors were found to negatively affect rural senior women's mental health: inadequate resources and loss in community; and devaluing of rurality, ethnicity, and gender. As illustrated in the study findings, limitations and social and other characteristics of rural communities, such as traditional gender roles and declining or non-existent resources, may result in mental health issues for rural senior women, such as loneliness, and negative self-concept.
Discussion
Nature of rural communities and resources
An interesting finding of this study was the language participants used, specifically in relation to loneliness. Participants spoke about being lonely which they related to losses of family and friends, and feeling alone, isolated, and sad. Although other mental health issues, such as depression and anxiety, may be relevant to loneliness, the participants did not discuss these issues, perhaps because rural seniors often value self-reliance and 'making do', accepting that that's life, you just get on with it21.
A major issue that arose for the women in this study was inadequate community infrastructure. The women spoke about cracks in sidewalks and poor road conditions which caused them constant worry because they feared that they may fall. This fear of falling, especially in the winter months, isolated them, and being isolated was identified as negatively affecting participants' mental health. Poor road conditions (like cracks in sidewalks) and limited infrastructure have been noted as issues for rural communities and identified as causing increased injuries to rural residents22. However, the present research advances knowledge on this topic by illustrating the effects, such as increased worry and stress in relation to falling, that inadequate road conditions and infrastructure have on rural residents and their mental health.
The present research findings also advance knowledge on how loss of resources in rural communities, such as churches, can affect rural senior women's mental health. Churches in rural communities are often the centre of the community and offer opportunities for community members to socialize. Socialization has been identified as important for rural senior women's self-identity and wellbeing23, as well as contributing to a strong sense of community connection. Thus, the loss of community churches contributes to a loss of identity, diminished opportunities to socialize, and decreased community connection. This research reveals that, although the closure of churches in rural communities may have a negative effect on all community members, it may be especially significant for rural senior women, due to their history, commitment to, and longer term connectedness to their rural communities.
Federal and provincial funding cuts for health services in past years have resulted in hospital closures and the loss of other health services in rural communities, which have greatly affected seniors' ability to access health care24-26. The present study findings advance understanding of how funding cuts have negatively affected rural senior women and their mental health. For example, the loss of pharmacies in rural communities was noted as an issue for participants, especially for seniors who were unable to drive. These seniors must find transportation, which was identified as frustrating and stressful by participants. Due to transportation issues, these seniors may not be able to fill their prescriptions which may increase their health issues. Participants also noted that emergency services, such as hospitals and ambulances, were often located far from their homes, causing them worry and fear that, in an emergency situation, an ambulance would not arrive in time to help them or their loved ones. In summary, these research findings advance understanding of how certain factors in the rural environment are detrimental to rural senior women, a growing population in rural Canada. The implications of these findings, in particular regarding the significance of social supports in rural communities for rural senior women's mental health, are important for practice and service delivery in rural areas, and the utility of secondary analysis with under-researched populations.
Significance of social supports in rural communities
Social supports, such as recreational and craft groups, were described by many of the participants as contributing to their overall positive mental health by assisting them to get out of the house, socialize, and exercise their body and mind. Participants noted that social programs of this kind were limited in their communities. Without these programs seniors may become isolated, which could lead to mental health issues such as depression27.
As decreased funding for programs is often an issue in rural communities, public resources, such as service clubs and churches, could be utilized to develop, sustain, and locate these activities. Rural residents could (and increasingly do) fundraise and make donations to service clubs and churches to support costs for seniors' programs. In addition, incorporating seniors more into rural communities and resources, such as with school children and in community events, would benefit not only seniors but also rural communities as a whole. Increased programming in rural communities may result in decreased need for mental health services, because social integration has been associated with enhanced emotional wellbeing28 and good mental health29.
Practice and service delivery in rural areas
The findings revealed that factors such as social support and rural conditions affect mental health. To effectively support the health of rural residents, healthcare practitioners need to be aware of the factors related to rural living30. This research also illustrates the importance of healthcare practitioners advocating for enhanced mental health practice and service delivery in rural communities. In addition, healthcare professionals, such as public health nurses and nurse practitioners, could be utilized more effectively in rural communities, as they have expertise in health promotion and illness prevention, as well as treatment, and are able to effectively assess and support patients' health needs and resources30-32. Public health nurses and nurse practitioners do not exist or are currently underutilized in many rural communities in Canada; sufficient and sustained political support and funding are required for these effective rural healthcare strategies33-35.
Utility of secondary analysis with under-researched populations
This research is one of the first secondary analysis studies of a photovoice research study. Advantages to using the secondary analysis method include increased opportunities to explore the abundant rich data of qualitative studies, and decreased need for limited resources such as money and time to conduct additional research36. This approach also proved to be valuable in exploring the sensitive topic of mental health in a population that is often marginalized, under-researched, and under-served - in this case rural senior women. Thus, secondary analysis could be used more often with other qualitative research studies that explores rural health topics, especially in under-researched populations and with sensitive topics such as those related to health and local community.
Over the next 10 years there will be a significant increase in seniors residing in rural settings in Canada as baby-boomers retire to bucolic settings3, and currently there is limited information on the mental health of rural senior women. Therefore, the findings of this study on the mental health issues and factors that positively and negatively affect the mental health of rural senior women significantly enhance our understanding of senior women's experience of mental health in a rural context. Nevertheless, more research is needed, specifically regarding the mental health of rural senior women residing in other geographic locations and cultures in Canada, because these women may experience mental health issues and factors differently from the participants in this study.
This study also highlights the utility of the secondary analysis method, specifically with under-researched populations, and for sensitive topics, and is a method that is cost-effective and gets the most from the rich data that are often found in qualitative studies. Thus, more secondary analysis studies are highly recommended.
Acknowledgement
Financial support for this research was provided by Health and Rehabilitation Graduate Program Scholarship, The University of Western Ontario.
References
1. World Health Organization. Active ageing: A policy framework. Geneva: World Health Organization, 2004.
2. Bedard M, Gibbons C, Dubois S. The needs of rural and urban young, middle-aged and older adults with a serious mental illness. Canadian Journal of Rural Medicine 2002; 12(3): 167-175.
3. Health Canada. Canada's aging population. Ottawa, ON: Health Canada, 2002.
4. Health Canada. Mental health. (Online) 2009. Available: www.hs-sc.gc.ca/hl-vs/mental/index-eng.php (Accessed 22 July 2007).
5. Canadian Mental Health Association. Community mental health services. (Online) 2009. Available: http://ontario.cmha.ca/mental-health/services-and-support/ (Accessed 17 May 2013).
6. Califoux Z, Neese J, Buckwalter K, Litwak E, Abraham I. Mental health services for rural elderly: innovative service strategies. Community Mental Health Journal 1996; 32(5): 463-479.
7. Martens P, Fransoo R, Burland E, Burchill C, Prior H, Ekuma O. Prevalence of mental illness and its impact on the use of home care and nursing homes: A population-based study of older adults in Manitoba. Canadian Journal of Psychiatry 2007; 52(9): 581-590.
8. Canadian Mental Health Association. Seniors and mental health: demographic and prevalence statistics. (Online) 2005. Available: http://www.ontario.cmha.ca (Accessed 8 June 2010).
9. Public Health Agency of Canada. A report on mental illness in Canada. Ottawa, ON: Health Canada, 2002.
10. Whyte J, Havelock J. Rural and remote women and the Kirby-Keon report on mental health. A preliminary gender-place analysis. Winnipeg, MN: The Prairie Women's Health Centre of Excellence, 2007.
11. Leipert B, Landry T, McWilliam C, Kelley M, Forbes D, Wakewich P et al. Rural women's health promotion needs and resources: a photovoice perspective. In: J Kulig, A Williams (Eds). Health in rural Canada; Vancouver, BC: University of British Colombia, 2012; 481-501.
12. Leipert B, Landry T, Leach B. Closing the gap: rural women's organizations and rural women's health in Canada. In: B Leipert, B Leach, W Thurston (Eds). Rural Women's Health. Toronto, ON: University of Toronto Press, 2012; 62-77.
13. Heaton J. Reworking qualitative data. London: Sage, 2004.
14. Wang C, Burris MA. Photovoice: concept, methodology, and use for participatory needs assessment. Health Education Behaviour 1997; 24: 369-387.
15. du Plessis V, Beshiri R, Bollman R. Definitions of rural. Ottawa, ON: Statistics Canada. Rural and Small Town Canada Analysis 2002; 3(3): 1-16.
16. National Advisory Council on Aging. Challenges of an aging Canadian society. Ottawa, ON: Minister of Public Works and Government Services, 1999.
17. Armstrong D, Coleman B. Health care needs of Mennonite women. St Thomas, ON: Elgin-St Thomas Health Unit, 2001.
18. Oliffe J, Bottorff J, Kelly M, Halpin M. Analyzing participant produced photographs from an ethnographic study of fatherhood and smoking. Research in Nursing & Health 2008; 31(5): 529-539.
19. Corti L, Witzel A, Bishop C. Secondary analysis of qualitative data. Forum: Qualitative Social Research 2005; 6(1): 49. Available: http://www.qualitative-research.net/index.php/fqs/article/view/498/1073
20. Szabo V, Strang V. Secondary analysis of qualitative data. Methods of Clinical Inquiry 1997; 20(2): 66-74.
21. Eales J, Keating N, Rozanova J, Bardick A, Swindle J, Bowles R et al. Caring contexts of rural services. (Online) 2006. Available: http://www.veterans.gc.ca/pdf/pro_research/rural-seniors-technical-report-phase3.pdf (Accessed 10 May 2013).
22. Canadian Institute for Health Information. How healthy are rural Canadians? An assessment of their health status and health determinants. Ottawa, ON: CIHI, 2006.
23. Arbuthnot E, Dawson J, Hansen-Ketchum P. Senior women and rural living. Online Journal of Rural Nursing and Health Care 2007; 7(1): 35-46.
24. Romanow R. Shape the future of health care: Interim report. Ottawa, ON: Government of Canada: Commission on the Future of Health Care in Canada, 2002.
25. Armstrong P, Amaratunga C, Bernier J, Grant K, Pederson A, Wilson K. Exposing privatization: Women and health care reform in Canada. Aurora, ON: Garamond ; 2001.
26. Health Canada, Division of Aging and Seniors. Canada's aging population. Federal report on aging. Ottawa, ON: Health Canada, 1998.
27. Dugan E, Kivett V. The importance of emotional and social isolation to loneliness among very old rural adults. Gerontologist 1994; 34(3): 340-346.
28. Lee C, Russell A. Effects on physical activity on emotional well-being among older Australian women: Cross-sectional and longitudinal analyses. Journal of Psychosomatic Research 2003; 54: 155-160.
29. Clark K, Leipert B. Strengthening and sustaining social supports for rural elders. Online Journal of Rural Nursing and Health Care 2007; 7(1): 13-26.
30. Bushy A. Orientation to nursing in the rural community. Thousand Oaks, CA: Sage, 2000.
31. Molinari D, Bushy A (Eds). The rural nurse: transition to practice. New York: Springer, 2012.
32. Leipert B. Women's health and the practice of public health nurses in Northern British Colombia. Public Health Nursing 1999; 16(4): 280-289.
33. MacLeod M, Kulig J, Stewart N, Pitblade J, Banks K, D'Archy et al. The nature of rural practice in rural and remote Canada. (Online) 2004. Available: http://www.fcrss.ca (Accessed 22 May 2010).
34. Kirby M, Keon W. Out of the shadows at last: highlights and recommendations. Ottawa, ON: Senate of Canada, 2006.
35. Leipert B, Wagner Delaney J, Forbes D, Forchuk C. Canadian rural women's experiences with rural primary health care nurse practitioners. Online Journal of Rural Nursing and Health Care 2011; 11(1): 37-53.
36. Stage F, Manning K. Research in college contexts: approaches and methods. New York: Routledge, 2003.

