The issue of emergency room (ER) visits for non-urgent/emergency problems is a recurrent topic of research in healthcare service1-22, and is a major concern for all involved in healthcare provision in Canada23. While in Ontario the media focus may be on large urban hospitals in Toronto that need to redirect serious cases because of clogged ERs24, non-urgent/non-emergency visits are also problematic for hospitals in under-serviced rural areas. In rural hospitals, family physicians usually run emergency departments, and must divide their time between on-call shifts at the ER and burgeoning family practices. In these regions, because of the misdistribution of Ontario's physicians, ERs are also too often used to provide general medical care. In addition to the extra burden imposed on rural family physicians, habitual non-urgent ER use could result in clients lacking the continuity of care of those who visit a family physician clinic.
Some argue that non-urgent ER use is also very inefficient and expensive3. For example, because doctors are less aware of a client's history, costly laboratory and radiological tests are used with greater frequency5. However, others have a dissenting opinion25,26. Whichever is the case, most studies of ER use are in urban settings, with rare exceptions12,27,28. Therefore, it is necessary to document better the use of ER in rural areas. To our knowledge, this is the first study of the kind in rural Northern Ontario, a region the size of France.
Elliot Lake is located near the north shore of Lake Huron, 160 km from the closest urban center (Sudbury). After the discovery of immense uranium deposits, the rural Northern Ontario community of Elliot Lake was formed in 1955 as 'the uranium capital of the world'. Drastic economic and population fluctuations followed the uranium market demands for 35 years, until complete shutdown of all mining operations by the mid-1990s. Since then, taking advantage of the infrastructure and housing left behind by the emigrating mining workers and families, Elliot Lake has been innovatively reinvented as a retirement community and recreational tourist destination29, now under a new nickname: 'a jewel in the wilderness'.
The stimulus for this research is the belief of healthcare professionals providing urgent and emergency services at Elliot Lake's hospital that the ER is greatly misused. And since the town has evolved into a retirement community, with a population pyramid very different from Canada as a whole (Fig 1), it is important to determine the effect the large elderly population has on the ER. Furthermore, the percentage of Canadians 55 years of age and older is expected to increase from 21% in 2001 to 32% in 2021. Hence, Elliot Lake can be also viewed as a model to project the population health care needs of future Canadian rural communities.
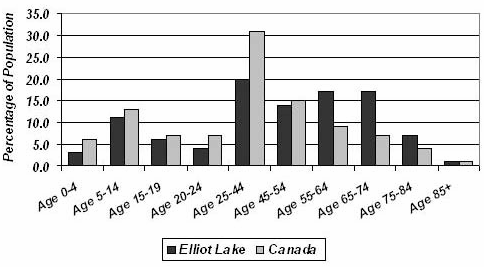
Figure 1: Comparison of population age cohorts between Elliot Lake and Canada (source: Statistics Canada).
Research into rural Northern Ontario ER utilization is also timely because a new family physician-oriented medical school with a focus on rural medicine is being created in the region. The Northern Ontario Medical School (NOMS), affiliated with Laurentian University in Sudbury and Lakehead University in Thunder Bay, Ontario, will accept the first 56 medical students in September 2005. NOMS students will benefit from an understanding of the issues surrounding rural ERs, which could help them to be better client educators and to be prepared for the cases that will be presented to them in the future.
This study was conducted to:
- Determine the demographics of ER clients in Elliot Lake, and the effect of its high elderly population.
- Learn about the reasons for visiting the ER.
- Compare the proportion of urgent/emergency and non-urgent/non-emergency visits as estimated by the clients and the healthcare professionals.
- Determine the ways that healthcare professionals suggest to cut down on ER misuse.
- Identify additional alternatives to minimise inappropriate use of the ER.
Setting and Methods
The study took place at the ER of Elliot Lake's St Joseph's General Hospital in July 2001. This month has a low caseload in comparison with the influenza season months of December to March (particularly during outbreaks/epidemics), which is a general feature of Canadian ERs24. St Joseph's General Hospital is a 57-bed acute care facility, with an adjacent 64-bed long-term care facility (St Joseph's Manor), and a sponsored 52-bed chemical dependency treatment facility (Oaks Centre). At the time of the study, Elliot Lake was serviced by 10 family physicians, a family physician anaesthetist, 1 general surgeon, 1 addictionist and 1 nurse practitioner. The 24 hour ER at St Joseph's General Hospital is the sole ER facility in Elliot Lake, and serves a catchment area with a population of approximately 18 000 people. For each 24 hour period, from 8 am to 8 am, the ER is staffed by one of the family physicians. There are three nursing ER shifts during the same 24 hour period. There is one registered nurse (RN) from 7 am to 7 pm, one RN from 9 am to 9 pm, and also an RN from 7 pm to 7 am, The nurse practitioner works at the ER from 8 am to 4 pm on weekdays.
Clients visiting the emergency room were interviewed verbally after obtaining their consent. The age, employment status, marital status, and reasons for visiting the ER were recorded. ER clients were asked if they had a family physician and if they had contacted this physician prior to their ER visits. In addition, clients were asked to rate the urgency of their visits:
On a scale from 1 to 5, with 1 being non-urgent and 5 being very urgent and possibly life-threatening, how would you rank your level of urgency?
Clients were also asked to name any agencies that they considered could have helped them to avoid an unnecessary visit to the ER. Clients making repeated visits to the ER were interviewed on each visit. Study participants were not identified so their anonymity was preserved.
Separate written questionnaires were administered to the attending nurse, and physician/nurse practitioner. These healthcare professionals' were asked to record their perceived level of urgency of each case on the same scale used for clients, and also recommendations that could prevent the client from using the ER for non-urgent/non-emergency visits in the future. If the healthcare professional felt that a client's visit was a valid urgency/emergency, no recommendations were made.
This research passed an ethical review and was approved by the Board of Directors of St Joseph's General Hospital.
Results
A total of 1472 visits were made to the ER during the study period, and 1096 clients were verbally interviewed (74.5% of visits). The remaining visits did not include an interview because clients were either missed by the interviewing team or refused to be interviewed. In the cases of children, the accompanying adults were interviewed. Physicians/nurse practitioner completed their written questionnaire for 1013 visits (68.8%), and nurses completed their written questionnaire for 1298 visits (88.2%).
Client demographics
Age: The age distribution of the interviewed sample is summarized (Fig 2). The age profile of ER clients reflects the age profile of the catchment area population (Fig 1). The only group that was represented somewhat above their catchment area population were children aged 0-10 years with 137/1096 visits (12.5%, 95% CI 11.5%-13.5%).The two age groups visiting the ER at a slightly higher frequency were persons of ages 41-50 years old with 154/1096 visits (14.0%, 95% CI 13.0%-15.0%), and from 61-70 years of age with 157/1096 (14.3%, 95% CI 13.3%-15.3%).
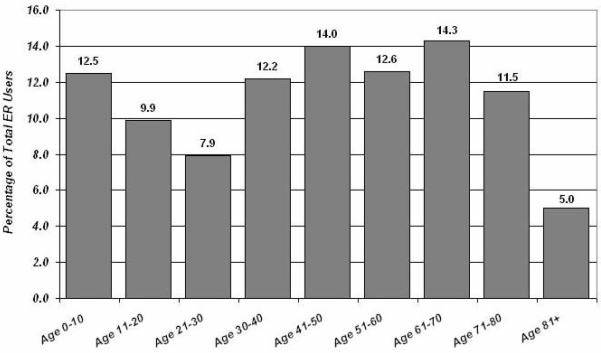
Figure 2: Age distribution of Elliot Lake ER clients
Sex: Males and females were represented in approximately equal numbers. Males accounted for 551/1096 (50.3%, 95% CI 48.8%-51.8%), and females for 545/1096 (49.7% 95% C.I 48.2%-51.2%) of the interviewed sample.
Marital status: Of the 1096 clients interviewed verbally, 460/1096 (42.0%, 95% CI 40.5%-43.5%) were married. Single persons were the next highest represented group with 322/1096 visits (29.4%, 95% CI 28.0%-30.8%), and children made 140/1096 visits to the ER (12.8%, 95% CI 11.8%-13.8%). Widows/widowers accounted for 95/1096 of the ER clients (8.7%, 95% CI 7.9%-9.5%), and divorced persons accounted for 56/1096 of the clients (5.1%, 95% CI 4.4%-5.8%). An additional 23/1096 of interviewed persons (2.1%, 95% CI 1.7%-2.5%) identified themselves as 'other'.
Employment status: Of all the interviewed clients, 396/1096 were retirees (36.1%, 95% CI 34.7%-37.5%). There were 247/1096 employed (22.5%, 95% CI 21.3%-23.7%); 248/1096 were children and students (22.6%, 95% CI 21.4%-23.8%); 106/1096 were unemployment insurance recipients (9.7%, 95% CI 8.8%-10.6%8.1); and 89/1096 clients on disability (8.1%, 95% CI 7.3%-8.9%). Welfare recipients accounted for 10/1096 of clients (0.9%, 95% CI 0.6%-1.2%).
Previous family physician consultation
The great majority of the interviewed sample had a family physician (887/1096 or 80.9%, 95% CI 79.7%-82.1%). However, only 316/1096 (28.8%, 95% CI 27.4%-30.2%) of the clients contacted their family physicians prior to their ER visit.
Reasons for ER visits
The presenting reasons for using the ER were grouped systemically and are summarized (Fig 3). There were 1126 listed reasons for visiting the ER within the interviewed sample, which is more than the number of interviewed clients (1096), because some clients presented more than one condition. Musculoskeletal conditions such as lower back pain, shoulder pain, fractures, and sprains accounted for 233/1126 of the reasons for using the ER (20.7%, 95% CI 19.6%-21.8%). Problems with the eyes, ears, and throat represented 231/1126 of the reasons for using the ER (20.5%, 95% CI 19.4%-21.6%). Scheduled visits to consult with the family physician on duty at the ER (most of them non-urgent/non-emergency) constituted 214/1126 of the reasons for clients to use the ER (19.0%, 95% CI 17.9%-20.1%). These scheduled visits were for conditions that could have been managed in the family physician's office, rather than for conditions requiring specialized emergency facilities and staff.
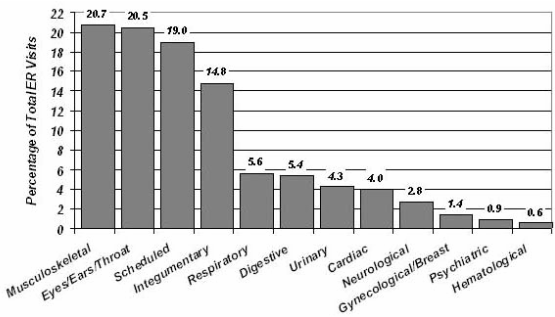
Figure 3: Reasons for Elliot Lake ER visits.
Levels of urgency
The results of the urgency level assessment by physicians/nurse practitioner and clients are summarized (Fig 4). Only approximately one-fifth (213/1096 or 19.4%, 95% CI 18.2%-20.6%) of the clients considered their visit to the ER to be non-urgent (level 1); whereas the physicians/nurse practitioner classified 458/1013 of the cases (45.2%, 95% CI 43.5%-46.9%) as non-urgent, and nurses assessed 827/1298 of the cases (63.7%, 95% CI 62.8%-64.6%) as non-urgent. Almost one-third of the ER clients (347/1096 or 31.7%, 95% CI 30.3%-33.1) cited an urgency of 3 out of 5, which is more than double the ratings of physicians/nurse practitioner at this level (152/1013 or 15%, 95% CI 13.8%-16.2%). Approximately one-fifth (227/1096 or 20.7%, 95% CI 19.5%-21.9%) of the clients perceived the urgency of their problem to be very urgent (14.7% level 4, and 6.0% level 5); while the physicians/nurse practitioner consider only 65/1013 of the cases (6.4%, 95% CI 5.6%-7.2%) to be very urgent (level 4) and only one case of 1013 to be life-threatening (level 5).
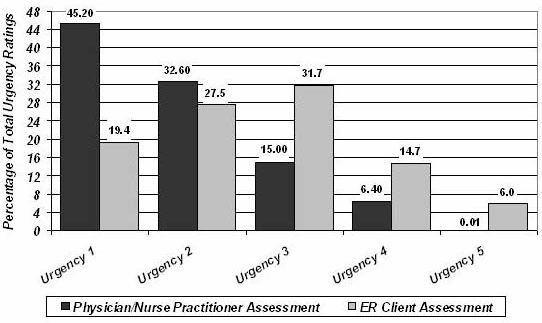
Figure 4: Comparison between physician/nurse practitioner and client perceived urgency of cases presented to Elliot Lake ER.
Alternatives to the ER
The recommendations by health professionals to alleviate the caseload of the Elliot Lake ER are summarized (Fig 5). The recommendations were made for each of the reasons for visiting the ER, and some clients had more than one reason. Physicians/nurse practitioner made recommendations for 1147 of the reasons, and nurses for 1498 of reasons. Physicians/nurse practitioner believed that the recruitment of additional family practitioners would reduce ER use for 444/1147 of the reasons (38.7%, 95% CI 37.4%-40.0%). They also recommended as an alternative the recruitment of nurse practitioners for an additional 315/1147 of the reasons (27.5% 95% C.I 26.3%-28.7%). Similarly, nurses suggested the recruitment of family practitioners for 560/1498 of the reasons (37.4%, 95% CI 36.5%-38.3%), and the recruitment of nurse practitioners for 398/1498 of the reasons (26.6%, 95% CI 25.8%-27.4%). Physicians/nurse practitioner considered that 235/1147 of the reasons for using the ER (20.5%, 95% CI 19.4%-21.6%) could have been handled by a walk-in clinic, if available (as of 2003 there is still no walk-in clinic in Elliot Lake). Nurses suggested the hypothetical use of a walk-in clinic for 435/1498 of the reasons (29.0%, 95% CI 28.2%-29.8%). The 'other' category includes all suggestions considered impractical or impossible to implement in Elliot Lake.
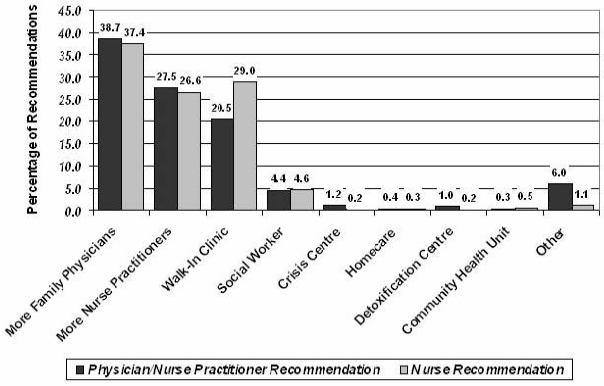
Figure 5: Alternative to ER recommendations for Elliot Lake ER cases from physician/nurse practitioner and nurses.
Almost-two thirds (61.3%, 95% CI 59.8%-62.8%) of the 1096 interviewed clients agreed that they would use alternative agencies other than the ER for non-urgent cases, if available. These agencies included crisis centers, community health units, home care programs, walk-in clinics, and rehabilitation centers. However, only 67/1096 of the clients (6.1%, 95% CI 5.4%-6.8%) had accessed any of the available alternative agencies in the past.
Discussion
This study is the first to capture the usage pattern of an ER in rural Northern Ontario, Canada. There are certain limitations that can be identified in the study design. No data is available for the 25% of ER attendees who were unable to be interviewed during the study period; however, the 75% capture rate is very good for this kind of study, and it is unlikely that the inclusion of the non-captured sample would have altered the results significantly. Although the study did not identify non-resident use of the ER, the authors' experience suggests that the number of Elliot Lake visitors seen in the ER was insignificant.
When considering the population of Elliot Lake, there is no specific demographic cohort that uses the ER anomalously. Groups are represented roughly proportional to their catchment area population. This is significant, considering the high proportion of elderly people in Elliot Lake, and because the community continues to actively recruit retirees to maintain economic stability. The median age reported among Ontarians by Statistics Canada is 37.2 years30. Elliot Lake has a median age of 49.4 years and a very high percentage of persons aged 65-74 years (25%) compared with the Canadian average (12%)30. The finding that elderly persons in Elliot Lake generally do not misuse the ER more than other age cohorts agrees with another Canadian study by Eagle et al.9. Also, in a previous study of physician visits by elders in Elliot Lake31, there was no clear trend on the mean number of visits with increasing age.
The finding that 80.9% of ER clients in this study have a family physician is remarkable, because persons with primary-care physicians would be expected to use the ER less frequently for non-urgencies/non-emergencies32. A major constancy in self-referred clients (71.2%, 95% CI 69.8%-72.6% of Elliot Lake ER clients) is the belief that their family physician is unavailable at the time when care is perceived to be needed, as noted by other authors5,21. Family practitioners in Elliot Lake report that clients must wait an average of 1 to 2 weeks to see them. Therefore, another likely possibility is that clients consider they have to wait too long to see their primary-care physicians, and this makes ER visits more convenient, since the ER serves as a 'walk-in clinic' in the absence of this kind of primary care facility in Elliot Lake. Although it appears that the majority in the community has a designated physician, the practices are overbooked and the number of family physicians does not seem to be adequate to provide proper continuity of care. The physician : client ratio of 1:1800 in Elliot Lake compares unfavorably with the national rural average of 1:1091 and 1:455 in urban centers. There is also only one nurse practitioner who works at the ER, which is clearly inadequate.
The common ailments presented in the Elliot Lake ER are similar to those presented in the ER study conducted in the town of Picton, Ontario12. Interestingly, Picton also has many elderly people. Statistics Canada reports a median age of 46.7 years for the town30. Musculoskeletal, otolaryngological, and dermatological conditions are all well represented in both studies. The number of actual urgencies was low during our study period. In fact, the pattern of presented conditions, and the demographic profile of the patients seen in the ER, is very similar to that of family practices and not that of a true ER. Furthermore, 19.0% of the visits were scheduled because of the need to supplement the availability of primary care outside of the ER. Most of the scheduled visits were for non-urgent procedures and follow-ups. It appears likely that this potentially unnecessary scheduled use of the ER is unavoidable while the physician : client ratio remains inadequate.
The percentage of non-urgent/emergency clients visiting the ER varies greatly from study to study. Non-urgent clients have accounted for as low as 7% of ER clients and as high as 94% of ER clients1. Much of this variation is caused by the varying definitions of non-urgent/emergency employed by researchers. Although there is great variation, most figures are between 30% and 60%1,2,4,8. The physicians and nurse practitioner staffing Elliot Lake's ER perceived 45% of the cases as non-urgent/non-emergency. This figure is comparable to the upper estimation of the 34-44% range of ER misuse documented in a study based on physician perception of urgency at two urban Ontario hospitals21. The marked lack of agreement in assessing the level of urgency between the clients and the ER staff indicates the need for relevant education of the catchment's area population. Kelly and Birtwhistle's12 recommendation is for governments and medical associations to develop public programs to reinforce the education done by physicians and other healthcare workers. This client education would focus on changing the public's perception of urgency, and on suggesting self-care measures and over-the-counter remedies for non-urgent health discomfort.
The most frequent recommendation of Elliot Lake physicians and nurses to curtail ER misuse is the recruitment of additional physicians and nurse practitioners, as it would reduce the amount of time that clients must wait to see their primary carers outside the ER, and also reduce the need for scheduled visits at the ER. The data and arguments above support this view, particularly because continuity of care has been shown to reduce ER utilization32,33. However, because Elliot Lake clients with family physicians only contacted their doctors 28.8% of the time before visiting the ER, there is also a need to educate the clients about the advantages of contacting their primary carer first. A similar situation was reported by Caplan5, because only 32% of ER clients with family practitioners called their doctors in this study. Caplan reports that clients with personal physicians visit the ER because they believe that their personal physicians are unavailable, and because they believe that hospital care is optimal. Thus, clients should also be educated that non-urgent visits to the ER might result in incomplete/inferior primary care, and duplication of procedures and tests5,19,34.
Walk-in clinics have been proposed, and used in Canada for some time now, to try reducing ER caseloads35,36. Only one-fifth of the recommendations of physicians/nurse practitioner in Elliot Lake suggested the creation of a walk-in clinic to reduce misuse of the ER, mostly because they feel that it would be just moving the problem to another location without addressing the local shortage of physicians/nurse practitioners (ie the same physicians/nurse practitioner would have to staff the ER and the hypothetical walk-in clinic).
The creation of the Northern Ontario Medical School, set to start in 2005, is a response to the shortage of physicians in rural Northern Ontario due to misdistribution. The hope is that physicians trained in Northern Ontario will stay and practice in the region. However, even if this were the case, the first contingent of physicians from this initiative will only be ready to practice at least 6 years later (4 years MD plus 2 years family medicine residence). Before then, other steps need to be taken to help curb ER misuse, which will certainly worsen as more physicians retire. The graduation of more nurse practitioners, and subsequent recruitment to Elliot Lake, could also help alleviate the problem, but it does not seem that this will happen at the necessary rate and in the foreseeable future.
Another way to reduce the number of inappropriate ER use is to suggest, at the time of the visit, other helpful agencies that non-urgency/emergency clients can access. Judging from the low rate of this kind of recommendations given by the interviewed health professionals, this measure would have a limited impact in ameliorating the ER misuse in Elliot Lake. Also, although the majority of clients responded that they would use other resources if indicated, only 6.1% of clients reported having used a healthcare agency other than the ER before. This could be due to their lack of knowledge about many of the agencies and their services in Elliot Lake, and it might be worthwhile to educate the community (including health professionals) in this respect.
There are other suggestions in the literature to reduce caseload in ERs not covered by the range of responses in our sample. According to Caplan5, family physicians could reduce inappropriate ER use by educating their clients in prevention. He states that client visits fall into patterns. If family physicians recognize these patterns and then anticipate them, many ER visits can be avoided. Physicians could also identify recurrent ER visitors and enlist them in a case management program, as described by Pope et al.37. Telehealth is now available in Ontario38,39 and could be more widely used, particularly to determine the level of urgency/emergency of the case before embarking on a trip to the ER. Other health professionals, such as pharmacists40, can also play a part in an integrated effort to reduce ER caseload in Elliot Lake and elsewhere.
Conclusions
The data suggest that the shortage of health professionals, and in particular family physicians, has created undesirable pressure on the ER of a rural hospital in Northern Ontario, both in terms of patient numbers and in skewing the caseload away from urgent conditions to non-urgent conditions that could be better managed outside the hospital. This pattern of ER misuse is probably common to all rural areas of Canada and needs to be documented more widely.
A new medical school is being created for the region, but the first family physicians from this initiative will only be available in 2012. In the meantime, to reduce ER misuse, healthcare professionals may need to take more preventive and educational measures about perceived urgency; and the use of other alternative town's agencies, Telehealth, case-management of recurrent clients, and collaboration with local pharmacists needs to be maximized.
Further research is needed into the effects on health outcomes in rural communities that may result from health services having to function beyond their capacity, and the economic impact to the health service of the misuse of the ER. It would also be important to determine the impact of working in this stressed environment on the health and family life of the rural physicians and how this may effect their future career plans.
Rural health clinicians, communities, researchers, and policy makers must work together to design and implement both immediate and longer term solutions to the problems identified in this study.
Acknowledgments
This research was supported by Grant S-PXJOS03 from the Ontario Medical Association CME Program for Rural and Isolated Physicians; and a Research Assistantship from Laurentian University.
References
1. Afilalo M, Guttman A, Colacone A et al. Emergency department use and misuse. Journal of Emergency Medicine 1995; 13: 259-264.
2. Béland F, Lemay A, Boucher M. Patterns of visits to hospital-based emergency rooms. Social Science and Medicine 1998; 47: 165-179.
3. Burnett MG, Grover SA. Use of the emergency department for nonurgent care during regular business hours. Canadian Medical Association Journal 1996; 154: 1345-1351.
4. Campbell PA, Pai RK, Derksen DJ, Skipper B. Emergency department use by family practice clients in an academic health center. Family Medicine 1998; 30: 272-275.
5. Caplan C. Emergency room use by clients from a family practice: patterns of illness and motivation. Journal of Family Practice 1975; 2: 271-276.
6. Coleman P, Irons R, Nicholl J. Will alternative immediate care services reduce demands for non-urgent treatment at accident and emergency? Emergency Medicine Journal 2001; 18: 482-487.
7. Davies T. Accident department or general practice? BMJ 1986; 292: 241-243.
8. Davison AG, Hildrey ACC, Floyer MA. Use and misuse of an accident and emergency department in the East End of London. Journal of the Royal Society of Medicine 1983; 76: 37-40.
9. Eagle DJ, Rideout E, Price P, McCann C, Wonnacott E. Misuse of the emergency department by the elderly population: myth or reality? Journal of Emergency Nursing 1993; 19: 212-218.
10. Habenstreit B. Health care patterns of non-urgent clients in an inner city emergency room. New York State Journal of Medicine1986; 86: 517-521.
11. Haddy RI, Schmaler ME, Epting RJ. Nonemergency emergency room use in clients with and without primary care physicians. Journal of Family Practice 1998; 24: 389-392.
12. Kelly L, Birtwhistle R. Is this problem urgent? Attitudes in a community hospital emergency room. Canadian Family Physician 1993; 39: 1345-1352.
13. Liggins K. Inappropriate attendance at accident and emergency departments: a literature review. Journal of Advanced Nursing 1993; 18: 1141-1145.
14. Mustard CA, Kozyrskyj AL, Barer ML, Sheps S. Emergency department use as a component of total ambulatory care: a population perspective. Canadian Medical Association Journal 1998; 158: 49-55.
15. Padgett DK, Brodsky B. Psychosocial factors influencing non-urgent use of the emergency room: a review of the literature and recommendations for research and improved service delivery. Social Science and Medicine 1992; 35: 1189-1197.
16. Powers MJ, Reichelt PA, Jaloweic A. Use of the emergency department by clients with non-urgent conditions. Journal of Emergency Nursing 1983; 9: 145-149.
17. Rubin MA, Bonnin MJ. Utilization of the emergency department by clients with minor complaints. Journal of Emergency Medicine 1995; 13: 839-842.
18. Sanders J. A review of health professional attitudes and client perceptions of "inappropriate" accident and emergency attendances. The implications for current minor injury service provision in England and Wales. Journal of Advanced Nursing 2000; 31: 1097-1105.
19. Satin DG, Duhl FJ. Help?: The hospital emergency unit as community physician. Medical Care 1972; 10: 248-260.
20. Vaughn HF, Gamester CE. Why clients use hospital emergency departments. Hospitals1966; 40: 59-62,121
21. Vayda E, Gent M, Hendershot A. Emergency department use at two Hamilton hospitals. Canadian Medical Association Journal 1975; 112: 961-965.
22. Wise M. Inappropriate attendance in accident and emergency. Accident and Emergency Nursing 1997; 5: 102-106.
23. Gutkin C. ER: a Canadian drama. Canadian Family Physician 2000; 46: 748.
24. Gray C. Hospital Crisis? What Crisis? Canadian Medical Association Journal 2000; 162: 1043.
25. Williams RM. The costs of visits to emergency departments. New England Journal of Medicine 1996; 334: 642-646
26. Urgency in the emergency. Canadian Medical Association Journal 1996; 155: 1038, 1040.
27. Hamdy RC, Forrest LJ, Moore SW. Use of emergency departments by the elderly in rural areas. Southern Medical Journal 1997; 90: 616-620.
28. Lishner DM, Rosenblatt RA, Baldwin LM, Hart GL. Emergency department use by the rural elderly. Journal of Emergency Medicine 2000; 18: 289-297.
29. Mawhiney AM, Pitblado J (Eds). Boom Town Blues: Elliot Lake, collapse and revival in a single-Industry community. Toronto: Dundurn Press, 1999.
30. Statistics Canada. Community profiles (online) 2003. Available from http://www12.statcan.ca/ english/profil01/PlaceSearchForm1.cfm. (Accessed 21 January 2004).
31. Pong RW, Salmoni A, Heard S. Physician visits by older persons in Elliot Lake: issues and challenges. In: AM Mawhiney, J Pitblado (Eds). Boom Town Blues: Elliot Lake, collapse and revival in a single-Industry community. Toronto: Dundurn Press, 1999; 240-251.
32. Stein AT, Harzheim E, Costa M, Busnello E, Rodrigues LC. The relevance of continuity of care: a solution for the chaos in the emergency services. Family Practice 2001; 19: 207-210.
33. Burge F, Lawson B, Johnston G. Family physician continuity of care and emergency department use in end-of-life cancer care. Medical Care 2003; 41: 992-1001.
34. Olsson M, Hansagi H. Repeated use of the emergency department: qualitative study of the client's perspective. Emergency Medicine Journal 2001; 18: 430-434.
35. Hutchinson B, Østbye T, Barnsley J et al. Client satisfaction and quality of care in walk-in clinics, family practices and emergency departments: the Ontario Walk-In Clinic Study. Canadian Medical Association Journal 2003; 168: 977-983.
36. Jones M. Walk-in primary medical care centres: lessons from Canada. BMJ 2000; 321: 928-931.
37. Pope D, Fernandes CMB, Bouthillette F, Etherington J. Frequent users of the emergency department: a program to improve care and reduce visits. Canadian Medical Association Journal 2000; 162: 1017-1020.
38. Ontario Ministry of Health and Long-Term Care. Telehealth Ontario Free Access to a Registered Nurse - 24 Hours a day, 7 days a Week. (Online) 2002. http://www.health.gov.on.ca/english/public/program/telehealth/telehealth_mn.html (accessed 23 Aug 2003).
39. Telehealth Task Force. Recommendations for a Telephone Health Education and Triage / Advisory Service. Final report to the Ontario Ministry of Health and Long-Term Care. (Online) 1999. http://www.health.gov.on.ca/english/public/pub/ministry_reports/telehealth/ telehealth.html (accessed 23 Aug 2003).
40. Bednall R, McRobbie D, Duncan J, William D. Identification of clients attending accident and emergency who may be suitable for treatment by a pharmacist. Family Practice 2003; 20: 54-57.




