The Lao People's Democratic Republic (PDR) is a landlocked country in central South-East Asia, which shares borders with Thailand, Vietnam, China, and Myanmar1. Laos comprises 16 administrative provinces with one capital city (Vientiane Capital). The national health system is organized administratively into four strata: central (Ministry, University of Health Sciences (UHS) and reference/specialized centers); provincial (provincial health office, provincial and regional hospitals, and nursing schools, which serve 85 000 to 800 000 people); district (district health offices and district hospitals, which serve 9000 to 150 000 people)2,3 and village (health centers, which serve 1000 to 5000 people4. The main network for the provision of healthcare services in Lao PDR remains the public system. In 2013, health facilities encompass four central teaching and referral hospitals, four regional hospitals, 12 provincial hospitals, 129 district hospitals, and 894 health centers5.
The quota for new staff recruited by the Ministry of Health (MoH) is fixed once a year by the Cabinet of the Prime Minister, based upon the proposal by the Ministry of Finance. The Department of Health Personnel (DHP) at the MoH is responsible for the allocation of this quota at all administrative levels: central, provincial, and district. There are two recruitment rounds per year, in April and October. Posts are announced at the levels of provincial health offices (PHO), central, and other facilities. New staff are selected at PHO level, based on a proposal by the DHP. Lists of the selected candidates are submitted to the DHP, MoH, and Ministry of Home Affairs, for approval, allocation, and posting2. Within this system, candidates apply for their post freely; urban settings normally receive more applications and can choose the best qualified staff according to their needs2,6.
The Department of Training and Research is responsible for training, supervises all education and in-service training, and controls all health-related educational facilities. Since 2008, there have been three providers of health worker education; UHS, College of Health Sciences, and the nursing schools. UHS provides seven training programs: medicine, dentistry, nursing, pharmacy, medical technology, basic science, and postgraduate studies. There are three provincial Colleges of Health Sciences (in Luangprabang, Savannakhet, and Champasack) and eight provincial nursing schools (in Xien Khung, Luang Prabang, Vientiane, Khammuane, Champasack, Salavane, Oudomsay, and Savannakhet). The nursing schools provide nursing and midwifery training programs2.
Lao PDR, like most countries, has insufficient numbers of qualified health workers in rural and remote areas. In 2005, there were 1.98 health workers (including health management and support workers, such as accountants in hospitals, hospital clerical workers, and drivers)7 per 1000 population. Only 1.59 medical health workers were working in health facilities (healthcare providers) per 1000 population, and only 0.53 qualified medical health workers (physicians, medical assistants, nurses, and midwives with 3-7 years' training) per 1000 population2. While over 72.0% of the population lives in rural areas3, only about 42.0% of health workers work in these areas. In 2009, the ratio of health workers working in rural areas was 1.15 per 1000 population, whereas in urban areas it was 4.58. This has resulted in people living in rural and remote areas having limited access to health services.
Key health workforce challenges in Lao PDR include the management of geographical, institutional, and skill imbalances. These unbalances have many dimensions and different backgrounds. Since salaries alone do not adequately cover the basic costs of living, health workers, like other professionals, tend to prefer urban areas. Urban areas provide better employment opportunities and living conditions, and in urban areas health professionals have better opportunities to study, and conduct private practice to earn additional income2,6. In addition, many new health professionals cannot be absorbed into the Lao public health system, due to the lack of sufficient vacant posts for new graduates9.
The shortage of health workers in a rural area has become more severe due to the unbalanced distribution of an increasingly mobile health workforce. A study of the distribution and mobility of medical doctors in the Lao public health sector over the past 10 years showed that most moved from the peripheral to the central level10. The geographical distribution of health workers is skewed in favor of urban areas, because new recruits have mostly been allocated to the central level, especially high-level and mid-level staff (staff with 3-7 years' training). Although district-level health facilities received a reasonable share of new health workers, most are low-level staff (staff with 2-2.5 years' training). In non-urban health centers, low-level staff account for over three-quarters of the total complement, because high-level, trained health workers tend to refuse rural posts2. Remote districts, in particular, lack health staff. Many graduates from central training institutions do not want to work at district and health center levels6.
Several previous studies, focused mainly on medical students, have elicited a number of factors related to the intention of health science students to conduct rural practices: rural background11-14, rural field experience11,15,16, spouse or significant other who had lived in a rural area12, parents who did not attend college14,17, educational opportunities11,18, type of work available in the rural area, career opportunities19,20, and professional support15. However, at present, very little has been published in the literature on this issue in Lao PDR.
Therefore, this study aimed to assess the proportion of health science students in Vientiane, Lao PDR who intended to work in a rural area and associated factors, using the concepts of social support and self-efficacy. Social support has multiple functions that support the behavior change process. Social support for health science students working in a rural area can come from a variety of sources, including parents, neighbors, friends, and institutions. Self-efficacy makes a difference in how individuals feel, their beliefs, self-motivation, and perceived capability, as key components of performance21-23. These were investigated, to determine whether they directly affected the intention of health science students to work in a rural area.
Study site and samples
This cross-sectional study was conducted at the UHS, the only university in Lao PDR that produces high-level health science students for the country. There are three types of student: (1) continuing education students (public health workers who attend UHS to upgrade from middle or bachelor level to a higher level or doctors who attend family medicine training), (2) quota students (supported by the Government and selected from the provinces) and (3) self-supported students (special program), who bear the costs of studying themselves. The eligible subjects for the study were all 403 final-year undergraduate and postgraduate students at UHS. They were all willing to participate in the study and asked to fill out self-administered questionnaires. Those who took leave during the study or during field practice outside the institute, and those whose questionnaires were incomplete, were excluded from study. In all, 356 respondents returned the completed questionnaires: 137 medical, 21 family medicine, 40 dentistry, 104 pharmacy, 20 medical technology, and 34 nursing students. The response rate was 88.3%.
Measurements
The survey instrument was a four-part questionnaire in the Lao language. Part 1 consisted of 14 items about the respondent's baseline characteristics: course of study, category of student, age, sex, marital status, religion, ethnicity, current residence, home town, total monthly expenses, experience of living in a rural area in the past and while studying, and parental education.
Part 2 covered intention to work in a rural area. In this study, a rural area was defined as a district of a province outside a capital city; this equated with 132 of 142 districts in the whole country. An urban area was defined as a district located within a capital city of a province. Vientiane Capital has four urban districts, while the remaining 16 provinces have one urban district each. The scale comprised one question to determine health science students' intention to work in a rural area after graduation. There were three possible answers: 'yes, and prefer a rural area at either district or health-center level', 'no, and prefer an urban area', and 'not sure'.
Part 3 covered self-efficacy of health science students for working in a rural area. In this study, self-efficacy was defined as a health science student's belief in their capability to exercise control over their own functioning in a rural area, their confidence in their ability to live and work in a rural area, and their ability to apply their knowledge to working in a rural area effectively. The scale comprised 15 items: 8 items for working in a rural area, and 7 items for professional self-efficacy. The questions were derived, revised, and adapted from the study by Minisini et al23. Answers were rated on a five-point Likert scale, as '1 = very little confidence', '2 = little confidence', '3 = moderate confidence', '4 = quite a bit of confidence', and '5 = a lot of confidence'. Of the possible total score (75), a range of 14-45 (less than 60% of the total score) was classified as low/poor self-efficacy, 46-59 (60-79% of the total score) as moderate, and 60-75 (equal or greater than 80% of the total score) as high/good. The Cronbach's alpha coefficient was 0.954.
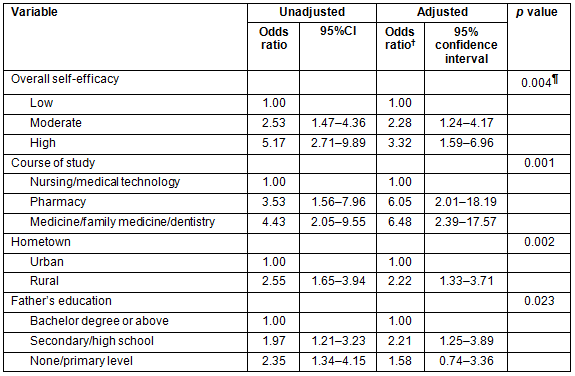
Part 4 involved social support for health science students working in a rural area. Social support was defined as financial and non-financial support provided by parents, neighbors, friends, and institutions, including care for, encouragement, motivation, accommodation arrangements, opportunity to enhance knowledge, and opportunity to get a promotion, provided to health science students working in rural areas. The scale comprised 18 items: 5 for parental support, 4 for neighbor support, 3 for friend support, and 6 for institutional support. The answers were rated according to a five-point Likert scale: '0 = not at all', '1 = a little', '2 = moderate', '3 = quite a bit', and '4 = a great deal'. Of the possible total score (72), a range of 0-43 (less than 60% of the total score) was classified as low/poor level of social support, 44-57 (60-79% of the total score) as moderate, and 58-72 (equal or greater than 80% of the total score) as high/good. The Cronbach's alpha coefficient was 0.905.
Data collection
Data were collected during February 2011. The principal investigator and two well-trained research assistants explained the objectives of the study before distributing the questionnaires to the participants and checked the completeness of the returned questionnaires.
Data analysis
Descriptive statistics (frequency, percentage, mean, and standard deviation) were used to describe all study variables. Multiple logistic regression analysis was used to obtain odds ratios (OR) and determine the associations between the study variables and health science students' intention to work in a rural area. Statistical significance was set at p<0.05.
Ethical considerations
The Ethics Committee of the Faculty of Public Health, Mahidol University (COA. No. MUPH 2011-047) and the National Ethics Committee for Health Research, Ministry of Health, Lao PDR (No. 12 /NECHR), approved the research protocol.
Of the 356 respondents, 38.5% were medical students, 29.2% were pharmacy students, and 11.2% were dentistry students. About 52.8% were quota students, 58.7% were aged 20-24 years (mean 26.8 years; range 20-46 years), 59.3% were female and 70.5% were single. Buddhists constituted 84.6% of respondents, and 77.8% were of Lao ethnicity; 31.5% stayed in their parents' houses and 52.2% were from urban areas. The median monthly expenditure was 800,000 LAK; the range was very wide, at 200,000-8,000,000 LAK. Of the respondents, 64.0% had experience of living in a rural area, and 45.2% had experience of field work/clinical clerkship while studying at UHS. Of respondents' fathers, 40.7% had completed a bachelor degree or higher, while 39.3% of respondents' mothers had finished primary school or had no education (Table 1).
Intention to work in a rural area after graduation
Of the 356 respondents, 40.7% intended to work in a rural area, whereas 17.1% had not yet decided. Among those who intended to work in a rural area, 90.3% (131/145) preferred to work at district level. For students who did not want to work in a rural area, 31.3% (47/150) wanted to work in a district or provincial hospital in an urban area, followed by 28.7% who wanted to work in a central hospital, and 20.0% who preferred to continue studying (Table 2).
Self-efficacy for working in a rural area
Only 21.3% of respondents reported high overall self-efficacy to work in a rural area - 20.5% in their profession, and 26.4% in working in a rural area (Table 3). Of 356 respondents, 12.6% were very confident that they were adequately prepared to work in a rural area, 11.2% were very confident that they had the skills to communicate with other staff in a rural area effectively and appropriately, and 7.3% were very confident that they could manage working with rural facilities. The students also reported that they were very confident in the following items: being able to leave the family to work in a rural area (16.9%), being able to live without electricity (16.9%), and being able to live where there is no water supply (19.4%) (Table 4).
Social support for intention to work in a rural area
About 79.8% of respondents reported receiving low social support. The lowest source of support was from neighbors (79.2%), followed by friends (73.0%), as shown in Table 3. Approximately 49.4% of respondents did not receive and 50.5% did receive a little support from parents in encouraging them to work in a rural area while studying and after graduation. Concerning social support from neighbors, 60.6% did not get or got little support from neighbors encouraging work in a rural area, and 58.7% did not receive support or received little support from neighbors to work in a rural area (Table 5).
Social support from friends, 55.9% received no or little encouragement or persuasion from friends to work in a rural area and 50.5% had no or few friends who wanted them to work closely in a rural area. Regarding institutional social support, 45.5% of respondents received no or little incentive from the government, and 37% received no or little promotion from the Ministry (Table 5).
Factors associated with health science students' intention to work in a rural area
Univariate analysis revealed nine variables were significantly associated with intention to work in a rural area after graduation: male gender, Buddhist religion, Hmong and other ethnicity, rented apartment/house and other accommodation, moderate/ high social support, moderate/high self-efficacy, course of study, rural hometown, and father finished secondary/high school (data not shown). In multiple logistic regression analysis, all variables with p<0.25 in univariate analysis were entered into the final model. Four variables were significantly associated with intention to work in a rural area: moderate/high self-efficacy, rural hometown, father finished secondary/high school, and being a medical/ family medicine/dentistry student (Table 6). The correlation matrix for intention to work in rural area model shows quite low correlations (r<0.30) between respondents' background characteristics and degree of self-efficacy. For example, correlations were very weak between degree of self-efficacy and hometown (r = 0.012 for moderate self-efficacy and r = -0.036 for high self-efficacy), father's education and hometown (r = 0.225 for none/primary level and r = -0.008 for secondary/high school level), course of study and hometown (r = -0.051 for pharmacy and r = -0.068 for medicine/family medicine/dentistry).
Table 1: General characteristics of 356 health science students
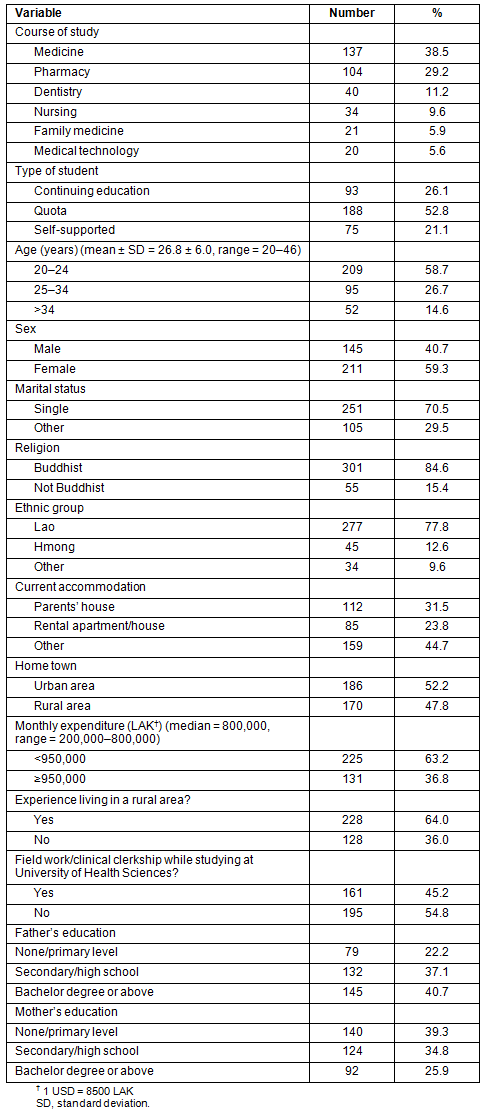
Table 2: Intention to work in a rural area among 356 health science students
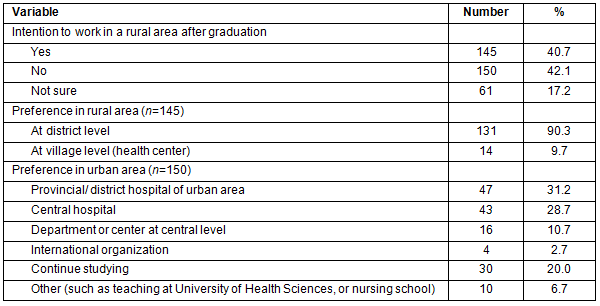
Table 3: Overall self-efficacy, social support, and intention to work in a rural area, among 356 health science students (%)
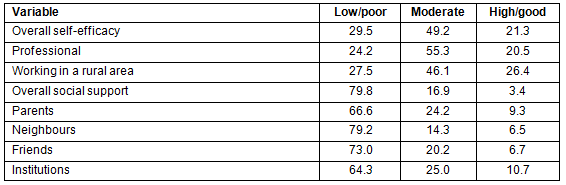
Table 4: Self-efficacy for working in a rural area among 356 health science students, by item (%)
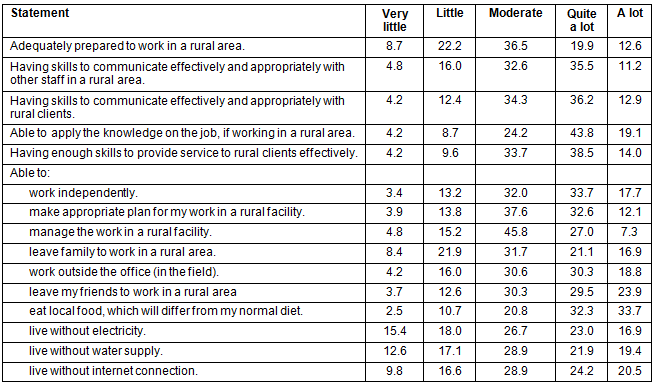
Table 5: Social support for intention to work in a rural area among 356 health science students, by item (%)
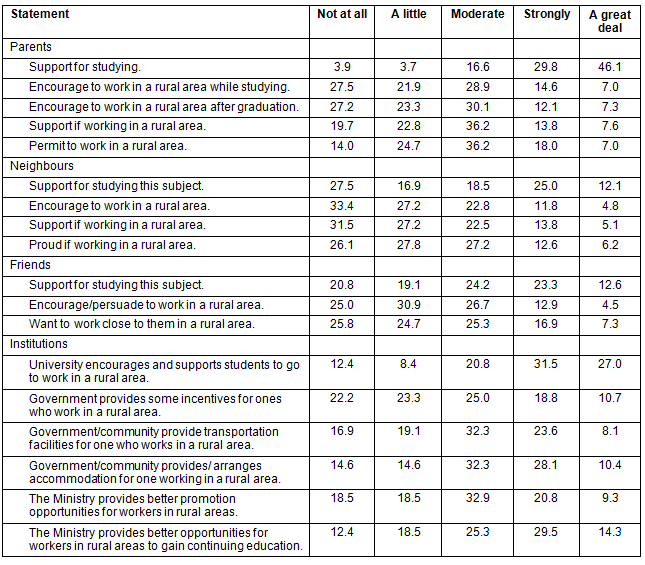
Table 6: Multiple logistic regression analysis for intention to work in a rural area among 356 health science students
Discussion
The proportion of students who intended to work in a rural area (district and health center level) was 40.7%, which was double that found in a study of occupational expectations among undergraduate medical and health technology students conducted by Soudachanh24. Possible explanation was that the previous study included only undergraduate health science students, while this study included both undergraduate health science students and family doctors who had a better understanding of the needs of the health workforce in a rural area.
In addition, about 17.1% had still not decided to work in a rural area, possibly because they lacked confidence to work independently in a rural area.
Students with moderate and high overall self-efficacy were 2.3 and 3.3 times, respectively, more likely to intend to work in a rural area than those with low self-efficacy. The possible reasons for this were as follows: when the students believed in themselves, that they could work independently and confidently in a rural area, they would intend to do so; and that students believed in their capacity to live and deal with problems and difficult or challenging situations. To the best of the authors' knowledge, no published research has directly linked the effect of health science students' self-efficacy and intention to work in a rural area after graduation. A study by Minisini et al23 reported that low self-efficacy among rural physiotherapists could result in impaired confidence in their ability to practice. They perceived that they lacked the skills and attributes to practice, which resulted in conflict with professional conduct and ethical standards.
Students with hometowns in rural areas were 2.2 times more likely to work in a rural area after graduation than those whose hometowns were in urban areas. These results were consistent with results of previous studies11,14,25-28 reporting that rural background was positively associated with rural practice.
Medical/family medicine/dentistry/pharmacy students were more likely to intend to work in a rural area than nursing and medical technology students. The possible explanation for this is that there are more vacant posts in rural areas for medical/family medicine/dentistry/pharmacy graduates than for nursing and medical technology graduates, because of mobility from rural and remote areas to urban or central areas, as mentioned earlier.
Lessons learnt from the compulsory Thai rural health service, and supportive strategies to maintain its effectiveness29,30 may be useful in solving the shortage of qualified rural health workers in Lao PDR. The MoH of Lao PDR has just launched the first phase of the Laotian health workforce recruitment and retention policy, whereby new graduates in medicine, pharmacy, and dentistry must complete 3 years of compulsory rural service in order to receive their licences to practice. Additional incentives for rural practice include postgraduate training and permanent civil service employment31,32.
Students whose fathers had finished secondary/high school were more likely to intend to work in a rural area after graduation than those with bachelor or higher degrees. This might be due to the fact that the more highly educated parents did not want their sons/daughters working in a rural setting where there was lack of infrastructure and a low living standard. The results confirmed the findings of Saini et al14, Wheat et al17, and Matsumoto & Kajii33.
Good social support is a positive predictor for rural practice intention15. In this study, social support was a significant predictor of intention to work in a rural area by univariate analysis (data not shown). However, it became non-significant when self-efficacy was included in the model. This suggested that, among UHS graduates, self-efficacy may serve as a suppressor between social support and intention to work in a rural area. The role of social support in predicting intention to work in a rural area may weaken when interacting with self-efficacy.
This study had some imitations. It relied on the self-reported intentions of final-year health science students at UHS, in Vientiane, Lao PDR. In addition, the cross-sectional study design was limited to determining causal associations between the study factors and intention to work in a rural area. A further longitudinal study is needed to ensure the factors affecting actual rural practice and the duration for which graduates were willing to work in a rural area. More variables should be included in the study, such as motivation, which will influence the decision of UHS graduates to work in a rural area.
The distribution of qualified health workers between urban and rural areas is still unbalanced. To increase the proportion of UHS graduates intending to work in rural areas, student recruitment at UHS should prioritize and provide increased quotas for those from rural areas. To improve students' self-efficacy for working in a rural area, the current curriculum should be reviewed and improved to ensure that all students have sufficient clinical practice in real situations, and that the duration for field work/clinical clerkship is extended to at least 3 months during the academic year. The Lao Ministry of Health and related organizations should focus more strongly on encouraging students to work in rural areas by providing appropriate incentives, accommodation and transportation arrangements, and discounted/free electricity and water for those prepared to work in rural areas. These supports should be introduced simultaneously with improvements to the work environments in rural facilities, the establishment of clear career paths, and the provision of promotion and educational opportunities.
Acknowledgements
Publication of this study was supported by the China Medical Board (CMB), Faculty of Public Health, Mahidol University, Bangkok, Thailand.
All authors have read and approved the manuscript. K.T. contributed to concepts, design, data collection, data analysis and manuscript review. N.S. contributed to the concept, design, definition of intellectual content, and manuscript review. N.H. was responsible for the concept, design, definition of intellectual content, statistical analysis, and manuscript preparation.
References
1. Asian tourism. Lao People's Democratic Republic. (Online) 2012. Available: http://www.aseantourism.travel//country/detail/lao-pdr (Accessed 10 April 2013).
2. Ministry of Health, Lao PDR. Human resource for health: analysis of the situation in the Lao PDR. Vientiane, Lao PDR: Ministry of Health & WHO, 2007.
3. Department of Statistics, Ministry of Planning and Investment, Lao PDR. Population and Housing Consensus 2005, Lao PDR. Vientiane, Lao PDR: Ministry of Planning and Investment, 2006.
4. Ministry of Health, Lao PDR. Ministrerial degree no 1274/MOH: The Role and Function of the Health Center. Vientiane, Lao PDR: Ministry of Health, October 2006.
5. Ministry of Health, Lao PDR. National Health Conference. Vientiane, Lao PDR: Ministry of Health, 2013.
6. Ministry of Health, Lao PDR. Lao Health Mater Planing Study. Vientiane, Lao PDR: Ministry of Health & Japan International Cooparation Agency, 2002.
7. Dal Poz MR, Kinfu Y, Dräger S, Kunjumen T. Counting health workers: definitions, data, methods and global results. Human Resources for Health. Discussion Paper. Geneva: World Health Organization, 2007. Available: http://www.who.int/hrh/documents/counting_health_workers.pdf (Accessed 11 April 2013).
8. Department of Organization and Personnel, Ministry of Health. Annual Health Personnel Statistis. Vientiane, Lao PDR: Ministry of Health, 2009.
9. Department of Organization and Personnel, Ministry of Health. Report of Health Personnel Statistics. Vientiane, Lao PDR: Ministry of Health, 2009.
10. Thongprachanh I. Distribution and migration of the Lao MD within the government public health sector in the past 10 years,1997-2007. (MPH thesis). Vientiane, Lao PDR: University of Health Sciences, 2008.
11. Bushy A, Leipert BD. Factors that influence students in choosing rural nursing practice: a pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: www.rrh.org.au (Accessed 20 December 2012).
12. Royston PJ, Mathieson K, Leafman J, Ojan-Sheehan O. Medical student characteristics predictive of intent for rural practice. Rural and Remote Health 12: 2107. (Online) 2012. Available: www.rrh.org.au (Accessed 14 January 2013).
13. Walker JH, DeWitt DE, Pallant JF, Cunningham CE. Rural origin plus a rural clinical school placement is a significant predictor of medical students' intentions to practice rurally: a multi-university study. Rural and Remote Health 12: 1908. (Online) 2012. Available: www.rrh.org.au (Accessed 20 December 2012).
14. Saini NK, Sharma R, Roy R, Verma R. What impedes working in a rural area? A study of aspiring doctors in the National Capital Region, India. Rural and Remote Health 12: 1967. (Online) 2012. Available: www.rrh.org.au (Accessed 20 December 2012).
15. McAuliffe T, Barnett F. Factors influencing occupational therapy students' perceptions of rural and remote practice. Rural and Remote Health 9: 1078. (Online) 2009. Available: www.rrh.org.au (Accessed 20 December 2012).
16. Eley D, Baker P. Does recruitment lead to retention? Rural Clinical School training experiences and subsequent intern choices. Rural and Remote Health 6: 511. (Online) 2006. Available: www.rrh.org.au (Accessed 20 December 2012).
17. Wheat J, Brandon J, Carter L, Leeper J, Jackson J. Premedical education: the contribution of local colleges. Journal of Rural Health 2003; 19(2): 181-189.
18. Schoo AM, Stagnitti KE, Mercer C, Dunbar J. A conceptual model for recruitment and retention: allied health workforce enhancement in Western Victoria, Australia. Rural and Remote Health 5: 477. (Online) 2005. Available: www.rrh.org.au (Accessed 20 December 2012).
19. Schofield D, Fletcher S, Fuller J, Birden H, Page S. Where do students in the health professions want to work? Human Resources for Health 2009; 7(1): 74.
20. Adams ME, Dollard J, Hollins J, Petkov J. Development of a questionnaire measuring student attitudes to working and living in a rural area. Rural and Remote Health 5: 327. (Online) 2005. Available: www.rrh.org.au (Accessed 20 December 2012).
21. Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychological Review 1977; 84(2): 191-215.
22. Bandura A. Social cognitive theory: an agentic perspective. Annual Review Psychology 2001; 52: 1-26.
23. Minisini M, Sheppard LA, Jones A. Self-efficacy beliefs and confidence of rural physiotherapists to undertake specialist paediatric caseloads: a paediatric example. Rural and Remote Health 10: 1426. (Online) 2010. Available: www.rrh.org.au (Accessed 20 December 2012).
24. Soudachanh S. Occupation expectation for undergraduate medical and health technology students (MPH thesis). Vientiane, Lao PDR: University of Health Sciences, 2007.
25. Azer SA, Simmons D, Elliott SL. Rural training and the state of rural health services: effect of rural background on the perception and attitude of first-year medical students at the University of Melbourne. Australian Journal of Rural Health 2001; 9: 178-185.
26. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Rural health research: demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15: 212-218.
27. Schoo AM, McNamara KP, Stagnitti KE. Clinical placement and rurality of career commencement: a pilot study. Rural and Remote Health 8: 964. (Online) 2008. Available: www.rrh.org.au (Accessed 20 December 2012).
28. Rourke J. WHO Recommendations to improve retention of rural and remote health workers - important for all countries. Rural and Remote Health 10: 1654. (Online) 2010. Available: www.rrh.org.au (Accessed 14 January 2013).
29. Wiwanitkit V. Mandatory rural service for health care workers in Thailand. Rural and Remote Health 11: 1583. (Online) 2011. Available: www.rrh.org.au (Accessed 20 December 2012).
30. Frehywot S, Mullan F, Payne PW, Ross H. Compulsory service programmes for recruiting health workers in remote and rural areas: do they work? Bulletin of the World Health Organization 2010; 88(5): 364-370.
31. Ministry of Health. Ministrerial Degree No 103/MOH: Allocating newly graduate students practicing in rural areas. Vientiane, Lao PDR: Ministry of Health, January 2012.
32. CapacityPlus. Laotian health workforce recruitment and retention policy informed by use of CapacityPlus tools. (Online) 2012. Available: http://www.capacityplus.org/laotian-health-workforce-recruitment-retention-policy (Accessed 19 April 2013).
33. Matsumoto M, Kajii E. Medical education program with obligatory rural service: analysis of factors associated with obligation compliance. Health Policy 2009; 90: 125-132.



