Background
Substance use is a global public health issue. Approximately 7.4 million people died worldwide in 2004 due to alcohol and tobacco use; this accounted for 12.6% of all deaths worldwide according to the World Health Organization (WHO)1. The same report highlighted substance use as the cause of approximately 245 000 deaths and the loss of over 13 million disability-adjusted life years (DALYs)1. The impact of substance use has been more pronounced in Europe. The WHO European region accounted for 13.7% of the world's population in 2004, yet 28.1% of deaths attributed to addictive substances occurred there1.
Most experimentation with substances of potential misuse begins in adolescence2,3. Early experimentation (at ages less than 13 years) can be problematic and can progress to misuse4,5. Long-term problems are associated with early initiation of substance use, such as greater likelihood of multiple substance use6 and increased incidence of psychosocial problems7,8. Geographical location is a factor that influences substance use. Living in an urban area has traditionally been associated with increased substance use while rurality was a protective factor9,10. This situation is changing as the gap between the patterns of substance use in urban and rural setting becomes narrower. Two reviews examining urbanisation as a risk factor for substance misuse found no conclusive evidence that it led to higher levels of substance misuse in urban areas compared with rural areas11,12. Another review examining the impact of substance abuse on rural areas found 'a convergence in substance use patterns between metropolitan and non-metropolitan areas'13. These articles suggest that it is too simplistic to discuss which area has a higher level of substance misuse. It is more appropriate to examine individual substance use patterns; one review noted that though overall levels were similar, cocaine and cannabis levels were higher in urban areas while alcohol, methamphetamine and inhalant use levels were higher in rural areas13. Other international studies concur with these findings and conclude that the differences are now to be found at the level of the individual substance14-20.
Data relating to urban-rural comparisons of substance use in Ireland are scarce. In a study of approximately 3400 young people in Ireland urban and rural alcohol use was examined and a marked difference was observed21. The study found that young people from rural areas reported having their first alcoholic drink at an older age and were less likely than their urban counterparts to have drunk alcohol in the last 30 days. The report focused solely on one substance, thereby making it impossible to generalise the findings. One study on the perceptions of parents who reside in rural areas suggests that differences in urban and rural drug use may be narrowing22. In the Cork and Kerry regions of Ireland, where the present study took place, a single study comparing urban and rural substance use levels in the general population has been published23. Substance use was compared in Cork city, Cork county and Kerry. Lifetime use of any substance was highest in Cork city (41%), followed by Cork county (31%) and Kerry (29%). The study also listed the lifetime use of individual substances. Use in Cork city was greatest for each substance listed except for over-the-counter codeine, where Kerry (4.4%) was greater than Cork city or county, with 3.0% and 1.8% respectively. There were no statistical analyses of these differences so no definite conclusions can be drawn. A recent review of Irish substance use has shown that substance use levels have changed since the report was published in 2004, so these patterns may have changed24.
Two studies have been conducted in substance misuse treatment centres in Ireland25,26. The treatment centres were almost exclusively for urban populations in Dublin. Both of the studies omitted location from their studies, so it was not possible to use these data as a comparator. Another limitation to these studies is that they focused on one or two substances. One of the studies examined concurrent alcohol and cocaine use25 while the other was an in-depth analysis of alcohol consumption26. It is often difficult to include rural substance users in studies such as these, as services are less prominent than in urban areas and substance users may not be captured by the system. However, the treatment centre in the present study treats has attendees from the counties of Cork and Kerry and thus serves a larger population from rural areas.
The Irish counties of Cork and Kerry have the third-highest level of substance treatment uptake in the country27. The level increased from 74.2 per 100 000 to 110.1 per 100 000 between 2005-2007 and 2008-2010 respectively. This increase highlights the need for more information about those who are entering these services. This review of the literature highlighted gaps in the knowledge of substance use in urban and rural areas in the general population: no studies that specifically make a comparison between urban and rural use have been published in nearly a decade. It also highlighted the lack of research into the nature of rural substance use; a need for research regarding those attending treatment centres, and how having urban or rural residence can affect the nature and success of treatment; and the need for an emphasis on adolescents in each of these areas, as substance misuse can harm adolescents immensely.
Aims
The aims of this study were to examine the data of young service-users (aged ≤ 21 years) attending a substance abuse treatment centre, and compare attendees from urban and rural areas, between 2007 and 2011.
Study design
Matt Talbot Services (MTS) is a substance abuse treatment centre for young people aged ≤ 21 years. It is the only Tier 3 substance misuse treatment centre in the Cork and Kerry counties that will admit people under the age of 18 years23. Before 2010, MTS exclusively treated males, but a policy change resulted in the admission of females. Young people must provide written informed consent to allow their data to be used for research as part of the requirements for admission. Between 2007 and 2011, 684 young people requested treatment from MTS. Of these, 457 (66.8%) young people received a place. A total of 436 of these service-users were included in this study's analysis. Seven were excluded because they were over the age of 21 years, and 14 were excluded because there were no data on their location of residence.
The Health Research Board (HRB) requires all treatment services receiving public funding to complete the National Drug Treatment Reporting System (NDTRS) form to collect information such as demographic information, treatment history, and substance use history (excluding tobacco use). Electronic copies of the NDTRS forms submitted by MTS from the years 2007-2011 were obtained from the HRB for the purposes of this study. In the Cork and Kerry counties, there is a single city, Cork city, so for the purposes of this study, urban service-users were those who resided in Cork city, while rural service-users resided outside Cork city (Cork county and Kerry).
Analyses
Descriptive analysis of demographic and recent substance use data was performed. Data about the highest level of education were taken directly from the NDTRS survey. In brief, options were as follows: (i) did not complete primary education (age approximately <12 years), (ii) completed primary education (age ≈12 years), (iii) completed the Junior Certificate (first national examination; age ≈15 years), (iv) received the Leaving Certificate (final examination of secondary education; age ≈18 years).
An independent t-test was performed to measure the difference in age at admission and the age of first substance use between urban and rural service-users, while the Mann-Whitney U test was used to test for significance in the differences between lifetime/previous month/daily use of multiple substances. For the remaining categorical data, Pearson's χ2 analysis was performed (with Yate's continuity correction for 2 x 2 tables); where expected values were below 1 (or 5 for 2 x 2 tables), Fisher's exact test was used. If contingency tables yielded significant differences, a column proportion test with Bonferroni correction was applied to identify the items that contributed to the significant value. A significance level of α=0.05 was used for any inferential statistics calculated. All statistical analyses were performed using Predictive Analytics SoftWare Statistics v18.0 (IBM Inc.; http://www-01.ibm.com/software/analytics/spss).
Ethics approval
Ethics approval for this research was obtained by the Clinical Research Ethics Committee (CREC) of the Cork Teaching Hospitals and University College Cork; ethics approval number ECM 4 (d) 02/10/12.
There has been a steady increase in the number of individuals who were accepted for treatment from 2007 to 2011. Of the total number of cases recorded during this period, 26 were in 2007, 70 in 2008, 90 in 2009, 101 in 2010, and 163 in 2011. The percentage gap between the urban and rural has lessened in the same period, with urban service-users accounting for 73.1% in 2007, 35.7% in 2008, 52.3% in 2009, 53.7% in 2010, and 45.3% in 2011. The regional breakdown of these service-users was 212 from Cork city, 223 from Cork county and a single person from Kerry, so further analysis using these categories was not performed.
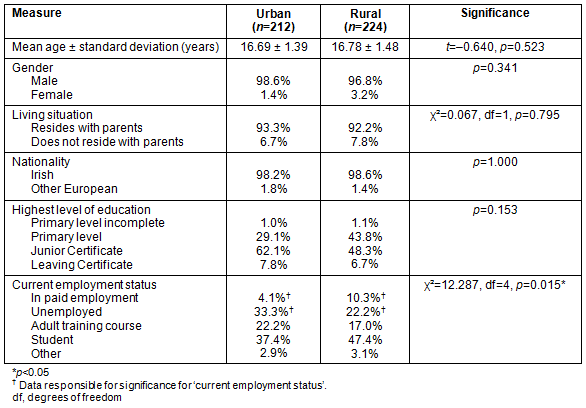
Table 1 presents data on urban and rural service-users. More service-users were from rural areas (51.3%) than from urban areas (48.7%). Both groups were similar in mean age for urban (16.7 ± 1.39 years) and rural (16.8 ± 1.48 years) service-users. Males accounted for most users from both urban and rural settings. The percentage of service-users that resided with their parents was also similar between urban (93.3%) and rural (92.2%). The highest level of education was found to be similar between urban and rural service-users. The service-users' current work/educational status was examined also; significant differences were observed between urban service-users and rural service-users. More urban service-users were unemployed than rural service-users.
Table 1: Demographics for urban and rural service-users of a substance
abuse treatment centre serving counties Cork and Kerry, Ireland, 2007-2011
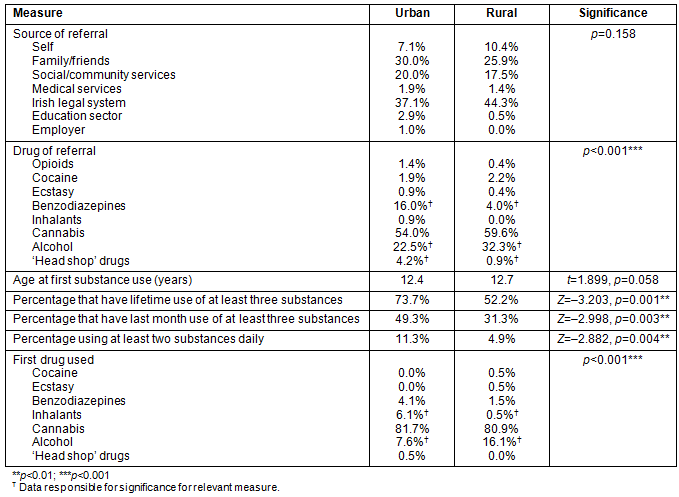
An examination of the source of referrals between urban and rural service-users showed that the distribution in the source of referrals was similar (p=0.158). However, when the drug of referral was examined, a difference was observed between the urban and rural service-users (p<0.001). More referrals related to benzodiazepine and 'head shop drugs' (psychoactive compounds, such as mephedrone, which in Ireland only became a controlled drug with restricted sales on 23 August 2010) were associated with urban service-users while more alcohol referrals were associated with rural service-users. Age of first substance use was also examined. Both groups had similar mean ages of first substance use (12.4 years for urban service-users and 12.7 years for rural service-users) (p=0.058). The percentage of urban service-users who had ever used three or more substances was significantly higher (p=0.001). A more detailed examination of their substance use histories revealed that usage was greater for urban service-users for the number of substances used monthly (p=0.003) and daily (p=0.004). There was a significant difference between the two groups when the first substance used was examined (p<0.001). A more detailed analysis found that first use of inhalants by urban service-users was significantly more frequent while alcohol use was more common in rural service-users (Table 2).
Table 2: Source of referral and substance use profile for urban and rural service-users of a
substance abuse treatment centre serving counties Cork and Kerry, Ireland, 2007-2011
Discussion
For both urban and rural service-users, the typical service-user was an Irish male aged between 16 and 17 years, who resided with his parents. Service-user characteristics were analysed to examine for differences between urban and rural service-users. A greater percentage of rural service-users than urban service-users were employed. There were differences in the drug of referral between urban and rural service-users, particularly for alcohol and benzodiazepines. A greater proportion of urban service-users had tried multiple substances in their lifetime and continued to use more substances regularly. A significant difference in the first substance used by service-users was also highlighted. More urban service-users' first substance was inhalants while their rural counterparts tried alcohol first. This differs from a study found on Irish alcohol use21, which noted that use of alcohol as a first substance was greater in urban adolescents. Greater rural use of alcohol as a first substance has been reported elsewhere, such as Scotland28 and the USA13. The results of the present study also showed that benzodiazepine referrals were greater in urban areas. A possible explanation for this is the trend of greater levels of prescribing benzodiazepines in urban areas29,30, which could result in more opportunities to access them. Early initiation of substance use has been linked with development of a substance-use disorder or dependence31, mental health problems32, educational under-achievement33, suicidal ideation34 and suicide attempts35.
A report from the Substance Abuse and Mental Health Services Administration compared urban and rural attendees of treatment centres in the USA in 201236. The report concluded that rural admissions were more likely to be in full-time employment and report alcohol as their main substance of abuse, while urban admissions were more likely to not be in the labour force and to report cocaine or heroin as their main substance of abuse. These results correspond with the findings in this study. It was not possible to compare results from the current study with research in Ireland or the UK, as there is a lack of research examining associations between attendees' residence and treatment centre attendance.
A limitation to this study is that there were a limited number of characteristics to analyse, and so confounding factors may be present, such as parental substance use37, romantic partner use38, physical abuse at a young age39, level of exercise40 and sexual preference41. Another limitation is that tobacco was not included as a substance of abuse. Tobacco and alcohol are often the first substances that pre-adolescents and adolescents will use42; excluding tobacco may raise the age of first substance use.
A further limitation is that service-users of a treatment centre were examined; differences in substance use are not generalisable to the Irish population. Service-users form a sub-section of the population that misuses substances. However the substance use of these young people may suggest the patterns of substance use in their peer group and their locality. This could be a reasonable explanation as MTS is the only Tier 3 centre for people in the region that are younger than 18 years. This means that a particular group of urban or rural substance users are not self-selecting, and therefore this bias is not introduced into the study.
Urban and rural service-users showed differences in their patterns of substance use. Policy in Ireland needs to take these differences into account. Policies are often formulated with urban service-users in mind and this can result in suboptimal preventative and treatment strategies for rural service-users. This is the first study in Ireland to compare service-users from an urban and rural setting; further work needs to be done to fully describe the differences between service-users, so that effective strategies to prevent and reduce substance use nationwide can be implemented.
References
1. World Health Organization. Global health risks: mortality and burden of disease attributable to selected major risks. Geneva: WHO, 2009.
2. O'Dowd A. Drug taking and drinking among 11-15 year olds in England have fallen over past 10 years. British Medical Journal 2012: 345: e5153.
3. Vega WA, Aguilar-Gaxiola S, Andrade L, Bijl R, Borges G, Caraveo-Anduaga JJ, et al. Prevalence and age of onset for drug use in seven international sites: results from the international consortium of psychiatric epidemiology. Drug and Alcohol Dependence 2002; 68(3): 285-297.
4. Hawkins JD, Graham JW, Maguin E, Abbott R, Hill KG, Catalano RF. Exploring the effects of age of alcohol use initiation and psychosocial risk factors on subsequent alcohol misuse. Journal of Studies on Alcohol 1997; 58(3): 280-290.
5. Chorlian DB, Rangaswamy M, Manz N, Wang JC, Dick D, Almasy L, et al. Genetic and neurophysiological correlates of the age of onset of alcohol use disorders in adolescents and young adults. Behavior Genetics 2013; 43(5): 386-401.
6. Lewinsohn PM, Rohde P, Brown RA. Level of current and past adolescent cigarette smoking as predictors of future substance use disorders in young adulthood. Addiction 1999; 94(6): 913-921.
7. Fiorentini A, Volonteri LS, Dragogna F, Rovera C, Maffini M, Mauri MC, et al. Substance-induced psychoses: a critical review of the literature. Current Drug Abuse Reviews 2011; 4(4): 228-240.
8. Tucker P. Substance misuse and early psychosis. Australasian Psychiatry 2009; 17(4): 291-294.
9. Carra G, Johnson S. Variations in rates of comorbid substance use in psychosis between mental health settings and geographical areas in the UK. A systematic review. Social Psychiatry and Psychiatric Epidemiology 2009; 44(6): 429-447.
10. Gilvarry E, McArdle P. Alcohol, drugs and young people: clinical approaches. London: McKeith Press, 2007.
11. Galea S, Rudenstine S, Vlahov D. Drug use, misuse, and the urban environment. Drug and Alcohol Review 2005; 24(2): 127-136.
12. Schifano F. Is urbanization a risk factor for substance misuse? Current Opinion in Psychiatry 2008; 21(4): 391-397.
13. Hutchison L, Blakely C. Substance abuse - trends in rural areas: a literature review. College Station, TX: The Texas A&M University System Health Science Center, 2010.
14. Forsyth AJ, Barnard M. Contrasting levels of adolescent drug use between adjacent urban and rural communities in Scotland. Addiction 1999; 94(11): 1707-1718.
15. Day C, Conroy E, Lowe J, Page J, Dolan K. Patterns of drug use and associated harms among rural injecting drug users: comparisons with metropolitan injecting drug users. Australian Journal of Rural Health 2006; 14(3): 120-125.
16. Lutfiyya MN, Shah KK, Johnson M, Bales RW, Cha I, McGrath C, et al. Adolescent daily cigarette smoking: is rural residency a risk factor? Rural and Remote Health 8(1): 875. (Online) 2008. Available: www.rrh.org.au (Accessed 17 March 2013).
17. Volzke H, Neuhauser H, Moebus S, Baumert J, Berger K, Stang A, et al. Urban-rural disparities in smoking behaviour in Germany. BMC Public Health 6: 146. (Online) 2006. Available: 10.1186/1471-2458-6-146 (Accessed 17 April 2013).
18. Coomber K, Toumbourou JW, Miller P, Staiger PK, Hemphill SA, Catalano RF. Rural adolescent alcohol, tobacco, and illicit drug use: a comparison of students in Victoria, Australia, and Washington State, United States. Journal of Rural Health 2011; 27(4): 409-415.
19. Rhew IC, David Hawkins J, Oesterle S. Drug use and risk among youth in different rural contexts. Health & Place 2011; 17(3): 775-783.
20. Hanson CL, Novilla MLLB, Barnes MD, Eggett D, McKell C, Reichman P, et al. Using the rural-urban continuum to explore adolescent alcohol, tobacco, and other drug use in Montana. Journal of Child & Adolescent Substance Abuse 2008; 18(1): 93-105.
21. Gavin A, De Roiste A, Nic Gabhainn S. HBSC Ireland: urban and rural patterns in alcohol consumption among Irish children. Galway: Health Promotion Research Centre, 2008.
22. Van Hout MC. Youth alcohol and drug use in rural Ireland - parents' views. Rural and Remote Health 9(3): 1171. (Online) 2009. Available: www.rrh.org.au (Accessed 3 March 2013).
23. Jackson T. Smoking, alcohol and drug use in Cork and Kerry 2004. Cork, Ireland: Department of Public Health, HSE South, 2006.
24. Murphy K, Sahm L, McCarthy S, Lambert S, Byrne S. Substance use in young persons in Ireland, a systematic review. Addictive Behaviors 2013; 38(8): 2392-2401.
25. Lyne J, O'Donoghue B, Clancy M, Kinsella A, O'Gara C. Concurrent cocaine and alcohol use in individuals presenting to an addiction treatment program. Irish Journal of Medical Science 2010; 179(2): 233-237.
26. Kearns C, James P, Smyth BP. Drinking patterns and preferences among irish substance abusing teenagers: a pilot study. Journal of Addictions Nursing 2011; 22(3): 124-129.
27. Bellerose D, Carew AM, Lyons S. Trends in treated problem drug use in Ireland 2005 to 2010. Dublin: Health Research Board, 2011.
28. Currie D, Small G, Currie C. Prevalence and profiles of substance and multi-substance use by adolescents: UK and international perspectives. London: Advisory Council on the Misuse of Drugs, 2005.
29. Gabe J, Williams P. Rural tranquillity?: Urban-rural differences in tranquilliser prescribing. Social Science & Medicine 1986; 22(10): 1059-1066.
30. Bellantuono C, Fiorio R, Williams P, Arreghini E, Cason G. Urban-rural differences in psychotropic drug prescribing in northern Italy. European Archives of Psychiatry and Neurological Sciences 1988; 237(6): 347-350.
31. Perkonigg A, Goodwin RD, Fiedler A, Behrendt S, Beesdo K, Lieb R, et al. The natural course of cannabis use, abuse and dependence during the first decades of life. Addiction 2008; 103(3): 439-449.
32. Stefanis NC, Dragovic M, Power BD, Jablensky A, Castle D, Morgan VA. Age at initiation of cannabis use predicts age at onset of psychosis: the 7- to 8-year trend. Schizophrenia Bulletin 2013; 39(2): 251-254.
33. van Ours JC, Williams J. Why parents worry: initiation into cannabis use by youth and their educational attainment. Journal of Health Economics 2009; 28(1): 132-142.
34. Swahn MH, Bossarte RM, Choquet M, Hassler C, Falissard B, Chau N. Early substance use initiation and suicide ideation and attempts among students in France and the United States. International Journal of Public Health 2012; 57(1): 95-105.
35. Swahn MH, Bossarte RM, Ashby JS, Meyers J. Pre-teen alcohol use initiation and suicide attempts among middle and high school students: findings from the 2006 Georgia Student Health Survey. Addictive Behaviors 2010; 35(5): 452-458.
36. Substance Abuse and Mental Health Services Administration. The TEDS Report: a comparison of rural and urban substance abuse treatment admissions. Rickville, MD: Center for Behavioral Health Statistics and Quality, 2012.
37. Li C, Pentz MA, Chou CP. Parental substance use as a modifier of adolescent substance use risk. Addiction 2002; 97(12): 1537-1550.
38. Gudonis-Miller LC, Lewis L, Tong Y, Tu W, Aalsma MC. Adolescent romantic couples influence on substance use in young adulthood. Journal of Adolescence 2011; 35(3): 638-647.
39. Caballero MA, Ramos L, Gonzalez C, Saltijeral MT. Family violence and risk of substance use among Mexican adolescents. Child Abuse & Neglect 2010; 34(8): 576-584.
40. Terry-Mcelrath YM, O'Malley PM, Johnston LD. Exercise and substance use among American Youth, 1991-2009. American Journal of Preventive Medicine 2011; 40(5): 530-540.
41. Marshal MP, Friedman MS, Stall R, Thompson AL. Individual trajectories of substance use in lesbian, gay and bisexual youth and heterosexual youth. Addiction 2009; 104(6): 974-981.
42. White HR, Jarrett N, Valencia EY, Loeber R, Wei E. Stages and sequences of initiation and regular substance use in a longitudinal cohort of black and white male adolescents. Journal of Studies on Alcohol and Drugs 2007; 68(2): 173.
