Diabetes mellitus is a global healthcare burden. In 2011 there were 366 million people with diabetes globally, and this is expected to increase to 552 million by 20301. Eighty percent of people with diabetes live in low- and middle-income countries and an estimated 183 million people (50%) with diabetes are undiagnosed2. The Indian Council of Medical Research-India Diabetes (ICMR-INDIAB) national study reported that in India 62.4 million people have type 2 diabetes and 77 million people have pre-diabetes3. These numbers are projected to increase to 101 million by 20301.
Diabetic retinopathy is a major cause of blindness among those of working age4. There are approximately 93 million people with DR, 17 million with proliferative DR, 21 million with diabetic macular edema, and 28 million with vision-threatening diabetic retinopathy worldwide5. The Chennai Urban Rural Epidemiology Study reported that nearly 25% of the Chennai population was unaware of a condition called diabetes6.
Seventy-four percent of India's population lives in rural areas with limited access to healthcare resources7.
Telemedicine can play a big role in screening diabetics at grassroots level. Before conducting mass telescreening, we must know how accurate it is when compared to the traditional camp-based screenings. We conducted a pilot study to determine the accuracy of telescreening in diabetic retinopathy.
To achieve near-universal coverage, the screening method should be community-based, and the point of delivery should be within easy reach of the population. Such screening can be either ophthalmologist-based or ophthalmologist-led8.
In the ophthalmologist-based program, a trained retina specialist travels along with the camp team and screens patients at the camp site for diabetic retinopathy. In the ophthalmologist-led program (telescreening), fundus photographs are transmitted to the base hospital for further evaluation and grading. There has been speculation about whether telemedicine overestimates or underestimates diabetic retinopathy. The present study compares the prevalence of diabetic retinopathy in an ophthalmologist-based model with an ophthalmologist-led model in people self-reporting with diabetes in rural South India.
Between January 2004 and December 2005, 39 free diabetic retinopathy screening camps were conducted in the rural areas of three districts of Tamil Nadu funded by Lions Club International. These camps were randomized into ophthalmologist-based and ophthalmologist-led groups. Of these, 21 camps were ophthalmologist-based and 18 were ophthalmologist-led (telescreening). A customized mobile van with in-built ophthalmic examination facility and satellite connectivity (courtesy of the Indian Space Research Organization) was used for telescreening; clinical examination was performed by an optometrist, and a social worker assisted him in villages.
Self-reported subjects with diabetes older than 30 years were examined. Visual acuity was measured using a log MAR chart. The anterior segment was evaluated with a hand-held slit lamp (Heine HSL 100 CE; http://www.heine.com), and measurement of intraocular pressure was performed with a Schiotz tonometer. After pupillary dilatation, a single 45-degree digital fundus photograph centered midway between the center of the macula and the disc was taken with a Topcon TRC NW 100 non-mydriatic camera (Topcon, Tokyo, Japan). The images were converted to DICOM (Digital Imaging and Communications in Medicine) format by PACS (Picture Archival and Communication Software) (Wipro InfoTech; http://www.wipro.com/industries/healthcare-segments/hospital-information.aspx). These images were transferred to the base hospital, a tertiary eye care hospital at Chennai, Tamil Nadu, by a satellite link using VSAT (very small aperture terminal) hardware. The transmission rate was 384 kilobytes per second (kbps). All images were examined by a retinal specialist, in real-time, using a videoconferencing system (Sony, Tokyo, Japan). The patient (who was in the mobile van) was then advised on the diagnosis, treatment, and follow-up.
In the ophthalmologist-based screening camps, the data sheet and routine evaluation were the same as that for the telescreening camps. Fundus evaluation to screen for diabetic retinopathy was done by binocular indirect ophthalmoscopy with magnifier (Keeler Ltd, Windsor, UK) by a retina specialist. Diabetic retinopathy was graded clinically using Klein's classification (Modified Early Treatment Diabetic Retinopathy Study scales)9. Sight-threatening diabetic retinopathy was defined as those eyes that had severe non-proliferative diabetic retinopathy, proliferative diabetic retinopathy, severe diabetic macular edema, or a combination of these. These patients were referred to the base hospital for further management. The data sheet variables from both types of screening camps were entered into Microsoft Access sheets. The data was analyzed by the Statistical Package for the Social Sciences (SPSS; http://www.spss.com).
For the ophthalmologist-based model of diabetic retinopathy screening we recruited 3522 subjects with diabetes, and 4456 subjects for the ophthalmologist-led model. The mean ages of subjects were 51±7.2 years and 52.5±5 years in ophthalmologist-based and ophthalmologist-led models (telescreening), respectively. The mean duration of diabetes was 4.9±5 years in the ophthalmologist-based model, and 5.2±5 years in the ophthalmologist-led model.
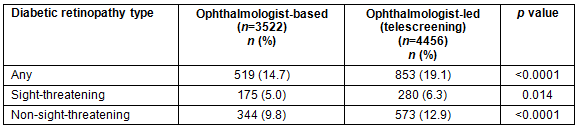
Table 1 shows the distribution of diabetic retinopathy in both the groups. Out of 3522 patients, 519 (14.7%) were diagnosed with diabetic retinopathy in the ophthalmologist-based model, and 853 (19.1%) in the ophthalmologist-led model (p<0.0001). Similarly, the ophthalmologist-led model identified more sight-threatening as well as non-sight-threatening diabetic retinopathies than the ophthalmologist-based model (6.3% vs 5%; 12.9% vs 9.8%), and the differences were significant (p=0.014).
Table 1: Prevalence of diabetic retinopathy (ophthalmologist-based vs ophthalmologist-led model)
Several studies have reported the prevalence of diabetic retinopathy in Indian population to be 17.6% in a population-based study10. The present study compares the diabetic retinopathy prevalence in self-reported individuals with diabetes in rural India screened in two different ways. This study shows that telescreening model detected more cases of diabetic retinopathy (19.1%) than the ophthalmologist-based model (14.7%), and this was also the case with respect to sight-threatening and non-sight-threatening diabetic retinopathy. There seems to be a funnel effect similar to that seen in photo-ROP study for telediagnosis of retinopathy of prematurity11.
We assume that the relative higher prevalence of diabetic retinopathy in the telescreening model is due to overdiagnosis. Possible contributing factors are the older age of this group of patients and increased duration of diabetes compared to those of the ophthalmologist-based model. The patients in the two groups are different, so we cannot pinpoint the cause of such a discrepancy.
Mode of transmission in our study was satellite-based. Satellite transmission of data eliminates the need for having local internet connectivity and the need for infrastructure at the village site. The images transmitted via satellite have high resolution and allow real-time conferencing between the patient and the ophthalmologist at the hub. The technical working group for standardization on telemedicine in India recommends satellite link as the best option for data transmission11,12.
In the telescreening model, single-field 45-degree photographs were used for screening. The American Academy of Ophthalmology has recommended that single-field fundus photography was not an adequate substitute in an urban population for a comprehensive ophthalmic examination because it may lead to a higher rate of underdiagnosis. However, level I evidence suggested that single-field images could serve as a screening tool for diabetic retinopathy to identify those patients who needed referral for further ophthalmic evaluation and treatment12,13.
The results of our study support telescreening (ophthalmologist-led model) as a screening tool for people with diabetes mellitus living in rural areas for referral and further management to higher urban healthcare centers. Several other studies data are required to ascertain the role of telescreening and its accuracy at grassroots levels.
Telescreening for diabetic retinopathy seems to be a good model, without undue fear of missing the diagnosis. Above all, it obviates the need for a physical presence of a retinologist in the field area, especially in countries like India.
References
1. Whiting DR, Guariguata L, Weil C, Shaw J. IDF Diabetes Atlas: global estimates of the prevalence of diabetes for 2011 and 2030. Diabetes Research and Clinical Practice 2011; 94: 311-321.
2. International Diabetes Federation. Diabetes atlas. 5th edn. Brussels: International Diabetes Federation, 2011.
3. Anjana RM, Pradeepa R, Deepa M, Datta M, Sudha V, Unnikrishnan R, et al. )(n behalf of the ICMR-INDIAB Collaborative Study Group). Prevalence of diabetes and prediabetes (impaired fasting glucoseand/or impaired glucose tolerance) in urban and rural India: Phase I results of the Indian Council of Medical Research-INdia DIABetes (ICMR-INDIAB) study. Diabetologia 2011; 54: 3022-3027.
4. Eye Diseases Prevalence Research Group. Causes and prevalence of visual impairment among adults in the United States. Archives of Ophthalmology 2004; 122: 477-485.
5. Yau JW, Rogers SL, Kawasaki R, Lamoureux EL, Kowalski JW, Bek T, et al. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care 2012; 35(3): 556-564.
6. Deepa M, Deepa R, Shanthirani CS, Datta M, Unwin NC, Kapur A, et al. Awareness and knowledge of diabetes in Chennai - the Chennai Urban Rural Epidemiology Study (CURES-9). Journal of the Association of Physicians of India 2005; 53: 283-287.
7. Sekher TV. Rural demography of India. In: LJ Kulcsar, KJ Curtis (Eds). International handbook of rural demography. International handbooks of population 3. New York and London: Springer, 2012; 169-173.
8. Sudhir RR, Frick KD, Raman R, Padmaja RK, Murali V, Sharma T. Mobile teleophthalmology: a cost effective screening tool for diabetic retinopathy in rural south India. eHealth International 2005; 1: 2-8.
9. Klein R, Klein BE, Magli YL, Brothers RJ, Meuer SM, Moss E, et al. An alternative method of grading diabetic retinopathy. Ophthalmology 1986; 93: 1183-1187.
10. Raman R, Rani PK, Reddi Rachepalle S, Gnanamoorthy P, Uthra S, Kumaramanickavel G, Sharma T. Prevalence of diabetic retinopathy in India: Sankara Nethralaya Diabetic Retinopathy Epidemiology and Molecular Genetics Study Report 2. Ophthalmology 2009; 116(2): 311-318.
11. Photographic Screening for Retinopathy of Prematurity (Photo-ROP) Cooperative Group. The photographic screening for retinopathy of prematurity study (photo-ROP). Primary outcomes. Retina 2008; 28: S47-S54.
12. Department of Electronics and Information Technology, Government of India. Recommended guidelines and standards for practice of telemedicine in India and health UnITe: the framework for Information Technology Infrastructure for Health (ITIH) for India. (Online). Available: http://www.mit.gov.in/telemedicine/home.asp (Accessed June 2009).
13. Williams GA, Scott IU, Haller JA, Maguire AM, Marcus D, McDonald HR. Single-field fundus photography for diabetic retinopathy screening: a report by the American Academy of Ophthalmology. Ophthalmology 2004; 111(5): 1055-1062.


