Introduction
The impact of mental health problems in Australia is greater among people living outside major cities, with access to mental health services in these regions known to be poorer than in metropolitan areas1,2. A number of factors contribute to this disparity including lower socioeconomic status, workforce shortages of specialised mental health professionals, attitudes to mental ill health and mental health literacy, longer distances between communities, poorer access to transport and prolonged drought and vulnerable industries/employment2-5. Program development and service delivery models that are designed for cities often neither adequately reflect rural and remote needs nor are readily translated well into rural and remote settings3. Innovative initiatives are required to meet rural and remote workforce shortages and improve rural and remote healthcare delivery.
The development of the University Departments of Rural Health (UDRH) program in 1997 was one such initiative. Similar to the Rural Clinical School program that followed, UDRHs were developed as a workforce strategy to provide a focus on rural and remote health training and address the shortage of health practitioners in rural and remote Australia6. The UDRHs operate as rural or remote satellite location(s) to major metropolitan universities with the intention of encouraging the emerging health workforce into practice within rural and remote locations.
To address the specific deficits in mental health expertise in rural and remote locations, the UDRH Mental Health Academic (MHA) project was established in 2007. Additional funding was provided by the Australian Government (Department of Health) to support the appointment of MHAs. Each of the 11 UDRHs appointed an MHA. The aim of the MHA role was to improve the mental health status of rural and remote Australians through key activities set by the Department of Health (Table 1).
The genesis of this article was a national meeting of the MHAs in 2014 at which the MHAs sought to compare and contrast their varying roles in their respective regions by identifying the different types of activities they had undertaken under each key performance indicator (KPI). The identified activities were collectively analysed and categorised by the MHAs. The derived categories frame the present article, which includes examples of each type of activity. For example, for the increased access to mental health services KPI, the categories identified were workforce development, increased recruitment and retention, and direct clinical services.
Distinctive characteristics of the MHAs' role, as it has developed, can be identified. MHAs are university academics employed to meet four specific KPIs (Table 1). Effective delivery of these KPIs is facilitated by the background of those appointed to the MHA positions. Typically the MHAs have established connections to their rural or remote communities, often as both a health professional and participating community member, bringing knowledge of both local mental health needs and sensitivities pertinent to the provision of mental health in rural and remote areas. Some recruitment difficulties were experienced, especially initially and in more remote locations. MHAs come from a number of disciplines including psychology, mental health nursing, medicine and social work. In each location a range of initiatives to address the project KPIs have been undertaken. Examples are described in the following section. Typically these local initiatives are evaluated as part of an ongoing monitoring process and for the regular half-yearly report from each location to the Australian Government. Evaluation was limited by the absence of standardised measures applicable to the widely varied elements of the MHAs' activities.
Considering the difficulties facing rural and remote Australian communities in accessing mental health care, the MHAs play an important role: they are geographically located in rural and remote communities, they connect and engage with local resources, they provide a variety of services and they may assist in the development of intellectual mental health capital in regional, rural and remote Australia.
Table 1: Key performance indicators for the mental health academic role

The Mental Health Academic project
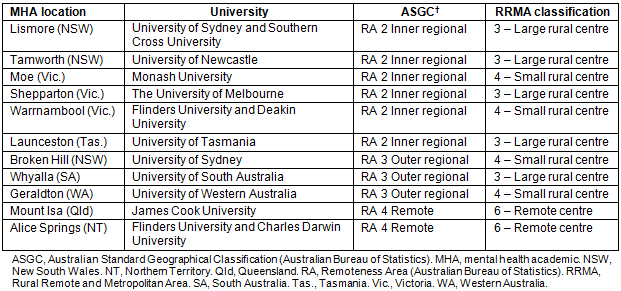
MHAs are located at eleven rural and remote sites around Australia (Table 2). From its inception the MHA program has been collaborative. Despite the geographic distances between the locations of each UDRH, the commitment to the role is reflected in the initiative shown by the MHAs in establishing and supporting mutually common ground. Although the framework of the KPIs sets the foundation for the MHAs' activities, each delivers activities addressing these KPIs in diverse ways, responding to individual community needs. A commitment to connect regularly was initially facilitated from within the informal MHA program network. This became a more formal structure within a national non-government organisation, the Australian Rural Health Education Network, as part of this organisation's role to support UDRHs. This network promoted innovative local responses to the common set of KPIs through sharing of ideas and broader collegial support.
Table 2: Location (states and territories of Australia) of mental health academics, university affiliation and geographic classification
Activities undertaken by the Mental Health Academic project
Increasing mental health recruitment and service access: Limited access to mental health services in rural and remote areas is a significant contributing factor to the mental health inequalities experienced in those communities4. The negative cycles of 'maldistribution of resources, access to appropriate and timely services, burnout and training of health workers and the financial cost of dealing with crisis over prevention' combine to contribute to overall inequalities of service5. Rural and remote mental health inequalities are at least partly associated with reduced access to appropriate services, which are in turn linked to reduced availability of mental health professionals.
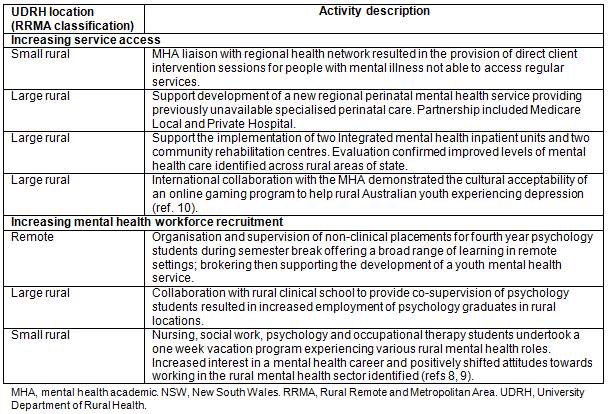
Strategies that may address health workforce maldistribution have been identified in the literature. These include increased exposure to rural and remote clinical practice in undergraduate training using rural and remote clinical placements, financial remuneration to work rurally and remotely, and increased professional support7. MHAs have developed collaborative engagements with a range of locally based service providers to support workforce development8,9 and increase the provision of mental health care by responding to identified barriers to access10. Table 3 shows examples of collaborative approaches to workforce recruitment and service access strategies.
Table 3: Activities increasing service access and workforce recruitment
Improving retention and the mental health workforce capability: Poorer access to mental health services in general, particularly in the specialty areas of mental health care, requires health professionals in rural and remote areas to widen their repertoire of skills11. The mainstreaming of mental health care has resulted in mental health issues being addressed in non-mental health settings, especially in rural and remote areas, highlighting the need to also improve the level of skill for both non-mental health professionals and community members who have closer association with people experiencing mental ill health12,13.
The MHA has a significant role in providing education and training throughout regional, rural and remote Australia. Providing training that is accessible and affordable is an important element contributing to workforce retention14. The MHA role provides specialised training to the existing rural and remote mental health workforce but also to health professionals who are working closely with people experiencing mental ill health. This includes GPs, allied health professionals, generalist nurses and those working in emergency services.
The MHA role is strategically placed within the rural or remote community to develop close collaborations and working relationships between agencies. MHAs respond to requests for training but are also in a position to identify and drive education dependent upon the community and workforce needs15. The diversity of the education provided by MHAs is demonstrated by the variety of teaching modes used (breadth), the educational roles undertaken (scale), the range of the audience participating in educational activities (scope) and the diversity of topics delivered (depth). Examples of education program provided by the MHA are reported in Table 4.
Table 4: Activities promoting workforce retention and supporting health workforce

Community awareness of mental health problems and suicide prevention: Rural and remote areas are particularly vulnerable to stigmatisation and confidentiality issues around mental health16. The contrast between urban and rural and remote perspectives on stigmatisation and confidentiality surrounding mental health has been reported, with rural residence described as 'physically distant but socially proximate', impacting on the 'silencing of mental health difficulties and the exclusion of people with mental illness in a manner more acute than in urban areas'17.
Community mental health awareness programs have been routinely organised by MHAs with community awareness programs on suicide identified as an important MHA activity18. Typically these initiatives occur in collaboration with the local community (Table 5).
Table 5: Activities supporting community mental health awareness

Mental health and wellbeing of Indigenous Australians: Nearly half of Australia's Indigenous population live in rural and remote locations, experiencing high to very high levels of psychological distress and double the risk for suicide compared to the wider community19-21. Engagement with this population has been a crucial component of many MHAs' workloads22. Addressing difficult issues such as mental health and suicide in all communities, including Indigenous communities, requires sensitivity, respect and trust23-26. The local connections, both pre-existing and developed by the MHAs in the role, have been important to the success of this aspect of the initiative (Table 6).
Table 6: Activities targeted towards improving mental health of Indigenous Australians

Collaboration: bridging the rural divide: The MHA initiative illustrates the benefits of collaboration on a national level. MHAs located across the country accessed the support and sharing of intellectual ideas through the formalised networking process of bimonthly teleconferences. This engagement was further promoted through two large collaborative projects.
In 2010, funding was provided through the Australian Rural Health Education Network to conduct a project comprising three components, which was jointly completed by MHAs from four UDRHs. The project, 'Improving mental health services in rural and remote Australia - recruitment and retention of rural health professionals', focused on the development of an online self-directed supervision training package. It included an early recruitment pilot for allied health student placements for those considering mental health as a career path and an evaluation of an online cognitive behavioural therapy training program for rural and remote health professionals27.
In 2012, a national collaborative project that scoped the provision of mental health placements in rural and remote Australia was undertaken by all 11 UDRHs, with MHAs playing a central role at each site. This project was divided into two key activities. The first activity examined which health discipline participated in mental health clinical placements, where these placements occurred, for how long, and what assisted or deterred the placement as an effective learning experience. The second activity examined the student, educational institution and service providers' perceptions of what influenced the mental health placement experience. Recommendations from the analysis conducted formulated a position statement including recommendations to shape the future of rural and remote mental health placements.
There is increasing recognition that mental health practice in rural and remote areas requires a different approach and that rural or remote based health professionals have common practice characteristics that are different from urban counterparts. The MHA initiative, developed to meet the needs of rural and remote Australia, reflects this, being strategically located to bridge the gap between education and practice, community consultation and improved health outcomes.
Flexibility, diversity and connectedness
The role has essentially adapted within each location to meet community needs and to support strategies required to provide quality local mental health care. Each academic, in a different setting, has responded to the broad guidelines of the program in flexible and diverse ways. Locally based and locally responsive MHAs define the work they do, not only according to the program KPIs, but also on the ability to connect with those in the rural or remote communities in which they work. As the MHA role is embedded within the community there is the opportunity to access and contribute to the intimate knowledge of what is required to enhance mental health care in rural and remote locations and to respond to the sensitivities of each community and region. Each MHA, being strategically placed in their current geographic location, not only identifies what is required from the ground up but has the opportunity to act as an advocate to promote change from the top down (ie through consultation with key mental health agencies and government). In addition to the broad program aims, the regular interaction between the geographically dispersed academics, each within an established academic department, has limited the dual risks of constantly 'reinventing the wheel' and of diverting resources into unhelpful approaches that may be avoided with the greater perspective of other colleagues.
The locally informed and connected approach undertaken by the MHAs may also be relevant to other areas of rural and remote health care, especially sensitive areas in which local knowledge, connections, credibility and flexibility are paramount. Whilst no single model will meet health needs in rural and remote Australia, based on the experience of the MHA initiative, supporting academics with clinical and community connections to promote rural and remote health and wellbeing in key health target areas is worthy of wider consideration.
Promoting recruitment and retention
MHAs recognise the value in supporting student learning and facilitating quality rural and remote placements in order to attract new graduates to mental health professions and build greater capacity of the rural and remote mental health workforce. In addition is a competing recognition of the need to support the retention of existing practitioners through the provision of rurally and remotely delivered quality education and training. The combination of academic skills and locally recognised health professional expertise has enabled the provision of evidence-informed education and training to rural and remote mental health professionals. A potential benefit of such locally provided ongoing professional education is the networking and associated peer support that may promote rural and remote mental health professional retention.
The MHAs in their role deliberately stepped outside the traditional expectations of academic teaching, often focused on large numbers of university students. The target group involved in MHA-supported education and training was wider, prioritising increased knowledge and skills of both existing health professionals and students in traditional health environments as well as those working in the mental health system in its broadest sense28.
Collaboration
In addition to the strength of partnership between the MHAs as a group, the strength of the partnerships developed between the MHAs, local health districts, primary healthcare agencies and community based health programs facilitated the ability of the role to integrate within each community. Figure 1 depicts the interchange between connectedness, diversity, flexibility and collaboration.
Establishing professional credibility was crucial to integration across all levels of liaison activities and negotiation. For the MHA role to fully understand local community and service provider needs in supporting the development of quality mental health care, a strong foundation of reciprocity and commitment is required. The leadership provided by the MHAs to engage with change and be accessible have been common characteristics of the MHA culture.
Collaboration amongst the MHAs has extended beyond mere peer support. Regular MHA contact has maintained focus on the agenda for rural mental health, with benefits in overcoming academic isolation. A further valued element has been the range of professional backgrounds and perspectives the MHAs have brought to the initiative.
Some difficulties of the MHA role have been highlighted. Perhaps not unexpectedly, recruitment of suitable staff has sometimes been problematic, especially in more remote locations. Another issue has been the need to support services that do not readily fit within the KPIs - for example the need to provide supervision, not only for students (as in KPI 4), but also for early career rural mental health professionals who do not have access to suitable support.
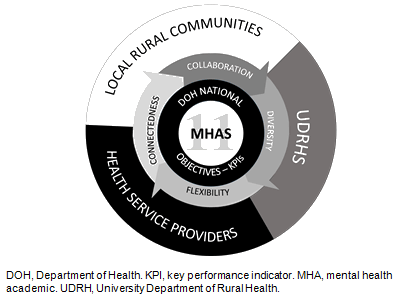
Figure 1: Mental health academics - interaction of connectedness, diversity, flexibility and collaboration.
Conclusion
This report, on the Australian MHA project, suggests that placing MHAs in rural university departments can help to address important rural and remote health issues including limited access to mental health care and limited community awareness of mental health issues. Furthermore, MHAs can enhance mental health skill development across a range of rural health professionals. Important factors in the success of this initiative include adopting a flexible approach, responding to local mental health needs, engaging with both local health services and community groups and collaborating as a network of MHAs across the country in supporting the current and future workforce.
References
1. Department of Health and Ageing. National strategic framework for rural and remote health. Canberra: Department of Health and Ageing, 2012.
2. Dunbar JA, Hickie IB, Wakerman J, Reddy P. New money for mental health: will it make things better for rural and remote Australia? Medical Journal of Australia 2007; 186: 587-589.
3. Bourke L, Humphreys J, Wakerman J, Taylor J. Understanding rural and remote health: a framework for analysis in Australia. Health & Place 2012; 18: 496-503. http://dx.doi.org/10.1016/j.healthplace.2012.02.009
4. Smith JD (Ed). Australia's rural and remote health: a social justice perspective. Croydon, Victoria: Tertiary Press, 2008.
5. Allan J. Determinants of mental health and well-being in rural communities: do we understand enough to influence planning and policy? Australian Journal of Rural Health 2010; 18: 3-4. http://dx.doi.org/10.1111/j.1440-1584.2009.01121.x
6. Department of Health. University Departments of Rural Health (UDRH) program 2011-14. Operational framework. (Internet) 2011. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/7F45C5C70FDD4DA6CA257BF0001C96C7/$File/UDRH%20Program%20Operational%20Framework%202011-14.pdf (Accessed 2 February 2015).
7. Grobler L, Marais BJ, Mabunda SA, Marindi PN, Reuter H, Volmink J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database of Systematic Reviews 2009, Issue 1. art. no.: CD005314.DOI:10.1002/14651858.CD005314.pub2. http://dx.doi.org/10.1002/14651858.CD005314.pub2
8. Sutton K, Maybery D, Patrick K. The longer term impact of a novel rural mental health recruitment strategy: a quasi-experimental study. Asia-Pacific Psychiatry 2015; 7: 391-397. http://dx.doi.org/10.1111/appy.12183
9. Sutton, K, Maybery D, Moore T. Bringing them home: a Gippsland mental health workforce recruitment strategy. Australian Health Review 2012; 36: 79-82. http://dx.doi.org/10.1071/AH11003
10. Cheek C, Bridgman H, Fleming T, Cummings E, Ellis L, Lucassen M, et al. Views of young people in rural Australia on SPARX, a fantasy world developed for New Zealand youth with depression. JMIR Serious Games 2014; 2: e3. http://dx.doi.org/10.2196/games.3183
11. Ellis IK, Phillip T. Improving the skills of rural and remote generalists to manage mental health emergencies. Rural and Remote Health (Internet) 2010; 10: 1503. Available: www.rrh.org.au (Accessed 7 September 2016).
12. Reed F, Fitzgerald L. The mixed attitudes of nurses to caring for people with mental illness in a rural general hospital. International Journal of Mental Health Nursing 2005; 14: 249-257. http://dx.doi.org/10.1111/j.1440-0979.2005.00389.x
13. Hungerford C. Treating acute mental illness in rural general hospitals: necessity or choice? Australian Journal of Rural Health 2006; 14: 139-143. http://dx.doi.org/10.1111/j.1440-1584.2006.00789.x
14. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. Geneva: WHO, 2010.
15. Hawkins R, Little F, Olds K. The supervision training project. In: Proceedings of 4th Australian Rural and Remote Mental Health Symposium, 19-21 November 2012, Adelaide, South Australia.
16. Parr H, Philo C, Burns N. Social geographies of rural mental health: experiencing inclusions and exclusions. Transactions of the Institute of British Geographers 2004; 29: 401-419. http://dx.doi.org/10.1111/j.0020-2754.2004.00138.x
17. Boyd CP, Aisbett DL, Francis K, Kelly M, Newnham K. Issues in rural adolescent mental health in Australia. Rural and Remote Health (Internet) 2006; 6: 501. Available: www.rrh.org.au (Accessed 7 September 2016).
18. Carey TA. In Control. a new approach to living well. Psychology Today. (Internet) 2015. Available: https://www.psychologytoday.com/blog/in-control (Accesssed 14 October 2015).
19. Australian Bureau of Statistics. Population characteristics: Aboriginal and Torres Strait Islander Australians. Canberra: ABS, 2006.
20. Australian Bureau of Statistics. Framework for measuring wellbeing: Aboriginal and Torres Strait Islander Peoples. Cat. no. 4703.0. Canberra: ABS, 2010.
21. Australian Indigenous HealthInfoNet. Summary of Australian Indigenous health. (Internet) 2014. Available: http://www.healthinfonet.ecu.edu.au/health-facts/summary (Accessed 14 October 2015).
22. Bennett-Levy J, Wilson S, Nelson J, Stirling J, Ryan K, Rotumah D, et al. Can CBT be effective for Aboriginal Australians? Perspectives of Aboriginal practitioners trained in CBT. Australian Psychologist 2014; 49: 1-7. http://dx.doi.org/10.1111/ap.12025
23. Singer J, Bennett-Levy J. Rotumah D. 'You didn't just consult community, you involved us': transformation of a 'top-down' Aboriginal mental health project into a 'bottom-up' community-driven process. Australasian Psychiatry 2015; 23: 614-619. http://dx.doi.org/10.1177/1039856215614985
24. Carey TA, Tai SJ, Stiles WB. Effective and efficient: using patient-led appointment scheduling in routine mental health practice in remote Australia. Professional Psychology: Research and Practice 2013; 44: 405-414. http://dx.doi.org/10.1037/a0035038
25. Isaacs AN, Maybery D. Improving mental health awareness of rural Aboriginal men: perspectives from Gippsland. Australasian Psychiatry 2012; 20: 108-111. http://dx.doi.org/10.1177/1039856212437256
26. Isaacs AN, Lampitt B. The Koorie Men's Health Day: an innovative model for early detection of mental illness among rural Aboriginal men. Australasian Psychiatry 2014; 22: 56-61. http://dx.doi.org/10.1177/1039856213502241
27. Bennett-Levy J, Hawkins R, Perry H, Cromarty P, Mills J. Cognitive behavioural therapy (CBT) training for therapists: outcomes, acceptability, and impact of support. Australian Psychologist 2012; 47: 174-182. http://dx.doi.org/10.1111/j.1742-9544.2012.00089.x
28. Health Workforce Australia. Mental health workforce planning data inventory. Adelaide: Health Workforce Australia, 2013.


