At the Alma Ata Conference of 1978, community participation was laid down as one of the key principles of primary health care (PHC)1. Soon after, developing nations accelerated PHC, especially among the rural and urban poor populations, in order to facilitate access to health and reduce endemic health inequalities2,3. Using community participation as the main underlying principle, communities were encouraged to contribute resources through representative volunteers commonly known as community health workers (CHWs)4. These CHWs were largely seen as channels through which the goal of health access for all by the turn of the millennium would be achieved5. CHWs played a key role in the functioning of PHC, an approach that was adopted as a rational strategy for healthcare delivery at the Alma Ata6. People from the villages were selected and trained to form a link between the communities and health systems. Many CHW programs were initiated and reported to have generated positive results in various interventions7.
During the first years of implementation, it was argued that CHWs, who became the embodiment of PHC, offered culturally acceptable support and were therefore looked upon as a panacea to the health human resource problems8-12. Critical studies into CHW programs showed that CHWs were not able to reduce mortality. Additionally, their quality of services were poor13, they offered poor-quality services, and thus were bypassed in cases of illness14. Various factors were given for this scenario including institutional factors, unrealistic expectations of poor volunteers, and poor initial planning3,15. It was also noted that in the 1990s, changes in macro-economic structuring led to shifting government priorities, which saw dwindling interest in community-based initiatives across developing countries12,16-18. Lack of financial remuneration for CHWs was also seen to contribute to the failure of the sustainability of CHW programs, although this remains a contentious issue19-23. Although early skepticism was raised about the representativeness of community volunteers it was not a main concern in the evaluation of CHW programs24.
The halfway point of the millennium development goals (MDGs), which coincided with the 30th anniversary of the Alma Ata conference, was marked with slow progress towards MDGs in the sub-Sahara region25. There was an increasing realization that attention needs to be directed at social interventions that influence healthy behavior, thus stakeholders in global health reaffirmed the need to promote CHWs to implement PHC interventions in the communities26-28. Today, developing countries have continued to scale up CHW programs with or without lessons learned from the mistakes in the past or the resolution of issues surrounding the concept29.
Uganda's village health teams (VHTs) strategy was initiated in the late 1990s24. Community health work in Uganda has its roots in the concept of 'defined area' used in the 1960s at Kasangati Health Center in Uganda's capital, Kampala, where the health center provided medical care while health extension workers carried out preventive programs in the 'defined area'. Numerous community initiatives by the government lasted until the political turmoil era from the 1970s to the mid-1980s30. In the 1990s, development partners rejuvenated CHWs, popularly known as community-owned-resource persons (CORPs)31. The national poverty report from 1995 increased the motivation towards PHC32. After the Abuja Declaration of 2001, which stressed the promotion of community health, Uganda rolled out the program for home-based management of fevers for children aged less than 5 years using volunteer community medicine distributors33, the precursor to the 1999 national health policy introducing the VHT concept. To date, the VHT coverage has not achieved 80%; in places where this coverage has been achieved, performance leaves much to be desired34. Recruitment of VHTs countrywide is reliant on development partners under the leadership of the Ministry of Health, which has put in place guidelines and training manuals for VHTs35.
Like many developing countries, Uganda is looking for strategies to achieve effective performance of its community health initiative sector. Much as community members express appreciation for the work of CHWs, they often remain passive, which hinders the operations36. In the literature on CHWs, it has been noted that there is no careful consideration of the selection and recruitment processes of CHWs despite evidence that elective program success is dependent on the level of embeddedness and links between the community5,37. While community involvement, belonging, and support are mentioned as critical and key in the functioning of CHWs, they have not been given their due place in the analysis of barriers to the functioning of CHWs1.
Community participation through community volunteers: a conceptual perspective
This article uses the concept of community participation as a lens for discussing PHC programs, a concept that has been fervently advocated for in PHC programs, becoming one of its cornerstones38. Lay volunteer CHWs have largely been seen as the channels for achieving community participation18. Although problems involving participation are widely recognized, the idea permeates many CHW programs because it is seen as a cost-effective means to achieve success in community interventions and it is morally consistent with the principles of equality and self-reliance that guide development thinking38. No consensus, however, exists on what community participation should mean or how it should work.
Participation can be distinguished at different levels: first and least in the form of passive beneficiaries, partners in activities through roles as volunteers, managerial responsibility, monitoring and evaluation; and second and most comprehensively as decision-makers about community needs and responses to them39. Community programs need to clarify what level of participation they aim to achieve40. Although participation has the potential to empower communities, it is widely appreciated that ambiguity in what is expected of communities can lead to trust problems, culminating in failure37. Following earlier efforts to scale up CHW interventions, critics argued that CHW programs would be paralyzed by insistence on single, one-size-fits-all guidelines that are haphazardly implemented in different community environments18,41.
In this article the framework of community participation is used to critically interrogate the dynamic interplay between the officials and the community in the selection of community volunteers in a rural community in Uganda. Vaguely defined participation guidelines are shown to hinder community involvement and breed mistrust within the community. This author concurs with others that participation should imply that the community controls the process of selecting volunteer health workers. The results have implications for community participation programs in rural communities in developing countries.
Setting
The research took place at various centers in a number of villages that constitute Kagugo parish, Luwero sub-county, in Luwero district (Fig1). These villages constitute a multi-ethnic population that has assimilated to the dominant Baganda people of central Uganda. The majority of the population is poor, engaged in peasant agriculture and/or petty trade in agricultural produce along the main arterial highway that runs north-south, connecting Kampala with northern Uganda and the republic of South Sudan. Luwero is generally characterized as a rural, resource-poor community in terms of infrastructure such as health centers, roads, and schools, which is typical of most communities in the Ugandan countryside.
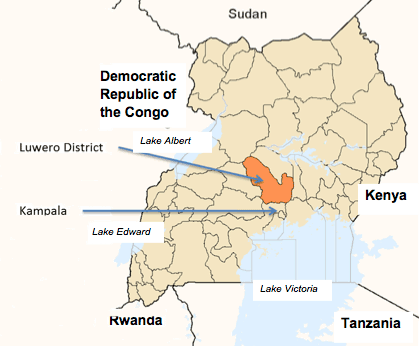
Figure 1: Location of the Luwero district in Uganda.
Data were collected during an extended fieldwork period over 1.5 years using ethnographic research techniques. Local research assistants provided note-taking and occasional language assistance before mastering of the local language, which happened rather quickly. Data was collected through participant observation of community events, 35 in-depth interviews, 20 focus groups, and 15 informal conversations. Initially, participants discussed problems that were affecting the community and how these problems had been solved. During these discussions, the theme of VHTs emerged and was explored further. The review of documents was an important source of information, especially on the activities of African Medical Research Fund (AMREF) as a project in Luwero district. Primary documents were accessed with permission from the project offices in Luwero.
Data analysis
Data analysis was done through an iterative process of reading and re-reading the transcripts during fieldwork to identify themes that emerged, which were investigated further through in-depth interviews. Transcripts were transferred into NVivo v10 (QSR International; http://www.qsrinternational.com) for qualitative data analysis using query searches for the terms 'Village Health Team', 'VHT', 'community health worker', or 'AMREF'. The query identified the usages of these terms within 49 documents in the data set. For each of these documents the broad context of these search terms was researched and coded using an inductive coding strategy for the following coding structure:
- introduction and history of VHT program
- community expectation and knowledge about the VHTs
- literacy requirement for VHTs
- local leaders' influence over VHT selection
- VHT income and benefits
- community trust of VHTs.
These codes were then analyzed into a narrative structure and reviewed by other researchers in the CoHeRe (Developing Sustainable Community Health Resources in Poor Settings in Uganda) project.
Ethics approval
Pseudonyms are used in this manuscript. Because of the intrusive nature of ethnographic methods, descriptions of respondents were minimized to ensure the anonymity of respondents. Respondent consent was obtained before audio-recording conversations. All records have been kept under password-protected files. The Institutional Review Board of Makerere University College of Health Sciences and the Uganda National Council of Science and Technology (SS3404) approved this study.
Introduction and supervision of the VHT program in Luwero
The VHTs were promoted as community volunteers to link communities to health centers. These teams were selected under national guidelines issued by the Ministry of Health, although implementation was managed at the local government level. In Luwero district, the VHT strategy was not implemented until the African Medical Research Foundation (AMREF) introduced the Malaria, HIV/AIDS, and TB project (MAT). Through this project they offered to partner with governments to facilitate the recruitment and training of VHTs. As clarified by one AMREF official:
Our MAT project needed community resource persons in the project area. This created an opportunity to fit within the district's plan to recruit VHTs who would serve in our project and remain in the community afterwards. We facilitated the local governments to do the recruiting using the Ministry of Health guidelines. We had to tailor our project needs to those of the local government.
When asked if they trained these VHTs, the respondent replied:
No, we facilitated the local government to recruit the VHTs but we ensured that during the training, our concerns about the link between malaria, TB, and HIV were included. The government issued a training manual, which was followed by the trainers. The mobilization of communities to select the persons to be trained as VHT volunteers was conducted by the local government but with financial support from AMREF.
The NGO partnership enabled the local government to implement a national strategy. The VHTs were popularized as an attempt to utilize volunteers from local communities, who were supervised by the local government.
The interview with the health assistant based at Luwero sub-county revealed how the process of selection was delegated to village leaders (LCs):
Practically, we asked the local council leaders [LCs] at the village level to mobilize and sensitize their respective communities about the idea of VHTs. We managed to supervision this process in some villages, but in most the LCs did that work without any supervision. We made sure they knew what the Ministry of Health guidelines were. Through community meetings LCs introduced the idea and led the selection of 5 persons per village who would work as volunteers to link the community to the health center, give health related information, and mobilize communities for other health related activities.
The responsibility to supervise the VHT selection process was delegated to LCs who were political leaders at the village level. At that point, recruitment became politicized. Without supervision, LCs would steer and influence the VHT selection process according to their own expectations. There was no oversight from the upper local government to ensure that guidelines were followed or to give leadership where guidelines had to be modified.
Authority, reward, and benefit expectations: motivation for volunteer recruits?
Because of the involvement of AMREF in facilitating the implementation of the VHT strategy, many people, especially the local council leaders, expected financial benefits in the form of salaries or allowances for the VHTs. As persons who would be charged with linking the community to the health centers, VHTs were expected to wield a lot of authority. These expectations influenced the recruitment process as LCs saw it as a way to wield more power in the community. It was not coincidental that most LCs, who were charged with leading the selection process, were selected to the VHTs. The financial provisions provided by AMREF for organizing the selection process amplified these expectations, and motivated the LCs to influence the process to their benefit, veering them further from the perception of volunteers. Commonly, volunteers are locally known as Nakyewa, a term that is more related to the type of help offered during periods of distress and communal responsibility. However, VHTs' expectations for financial benefits and the initial allowances for mobilizing community selection eroded that perception among many in the community, including among LCs. In a focus group, discussion of VHT selection revealed how such motivations were predominant in the selection process:
They [LCs] chose themselves but I think they struggled for nothing. Everybody wanted the opportunity to on a VHT. They fought each other. Those with power are the ones who struggle for these things.
The power struggle mentioned above accompanied the perception that VHTs were going to be important in the community as 'local doctors'. It was not surprising that LC chairpersons made sure they were selected and made sure that their friends out-maneuvered those who struggled to be on the VHTs.
During a focus group discussion with a VHT, participants expressed their expectations when they offered to volunteer:
We knew that we were to work as volunteers but we still expected some money from the AMREF. And they did initially give us some money for transport refunds and lunch allowances during training and monthly meetings. (R5)
Of course we expected some money, if we are required to spend our time, why wouldn't they give us a little token of appreciation? (R4)
This expectation to receive personal benefits in the form of allowances motivated many who struggled to be part of the VHTs. This struggle would most likely be won by the LCs since they controlled the selection process.
Politics of patronage: influence of local council leaders in the selection of VHTs
While providing LCs with the authority to lead the VHT selection, LCs became privy to information not open to the public and that they could use to their advantage. Since local leaders are politicians elected through adult suffrage, it was unsurprising that they, motivated by their own expectations, ignored the guidelines and influenced the process. As stated earlier, this was also facilitated by limited supervision from the local government, which delegated the roles to them.
One evening, while at a local bar, local community members were engaged in a conversation. The author's presence there prompted them to discuss the issue of VHTs since a number of them knew the author was interested in the subject. One elderly man, sounding frustrated, said:
The LCs always have their circles of friends with whom they always share whatever is meant for the community. Those projects [referring to AMREF] with the intention to help us come and give all the money to the chairman and his friends, and they think they are helping us.
When the author interjected and asked whether they inferred that all the VHT members in the community were friends of LCs and were receiving money, another man responded:
Those [the VHT members] were taken away from us and given money. The chairman and his friends, who wield the power in the community, have impoverished this community. They take everything meant for this community in the name of helping us.
Similarly, in an informal conversation, Mukasa, a male member of the VHT, told me how he has two bicycles, one as a volunteer National Agricultural Advisory Services peer educator and another as a VHT. He seemed to boast of how, because he is useful to the community, he is popular and volunteers for many agencies working in the community. One lady, Sophia, who operates a nearby food stall, was eavesdropping and quickly interjected:
That man is part of the group that eats everything meant for this village. Everything that comes, they take it. They know that something is coming and grab it before it reaches us. They take them and give them money, bicycles, we do not know how they help us.
In these quotes, one can sense the frustration about these interventions and how the LCs hijack the interventions to benefit themselves and circles of their friends. The previous two quotes refer to the perception that the chairman has a 'circle' of friends with the power to take advantage of community resources from outside agencies. The author felt that the people who spoke against this circle of power were taking the opportunity to report them to a foreigner who they perceived to be interested in hearing their frustration and who could reach the higher offices.
In an informal conversation one LC leader confided that he did not convene community meetings to select VHT members partly because people did not show up when he tried to, and because the local government wanted the names urgently. The LCs had to select those whom they trusted and felt could work effectively. Ironically, all LC chairpersons are members of the VHTs which is against the Ministry of Health guidelines, which state that VHTs must be selected by the community itself and not imposed by political structures. They should be five members per team per village; one per 25-30 households. Their selection should be through popular vote, and gender sensitive. Political leaders should not be eligible for purposes of ensuring checks and balances42.
The local leaders' decision to select themselves and their friends was partly influenced by the perceived benefits and lack of supervision from those above them in the local government structures. They overlooked the rules in order to influence the VHT selection process.
Literacy requirement: facilitating influences by the powerful?
In addition to other guidelines, one of the criteria for persons to be elected to the VHTs was the ability to read and write, preferably in English, the official language of Uganda, or at least in the local language. Typical of most rural and remote communities, where the majority of the illiterate populations live, the few who are literate are also the local leaders and power-holders in the community. They occupy gatekeeping positions in the community in many ways that facilitates elite capture, especially when external partners wish to collaborate with such communities. In an interview with the chairman of VHTs in Kagugo parish, his response revealed how the literacy requirement impacted the selection of VHTs:
They [district officials] said VHTs should be able to read and write. The selection process became easier because there are not so many in such villages. I can tell you the people that are literate from memory. Indeed the training and the work we were doing needed someone who was literate. I can show you the books and the things wrote, you cannot give it to the illiterate person ...
Aida - a 44-year-old VHT member and primary school teacher - when asked about how she heard about the VHT strategy, revealed how literacy played an important factor in her selection when she said:
I am lucky to always be selected. The chairman here is my friend; we have a good relationship. He always approaches me when there is a new program in the community that requires people to do some work, especially programs that require one to know some English. There were programs that trained us, and we were distributing mosquito nets, another [program] for the distribution of anti-malarial drugs for children.
Both quotes show how literacy requirement may have reinforced the LCs' choice of VHTs. Furthermore, if the community wished to have someone else, who was illiterate, they could not have sent him/her for training. This meant that, due to the guideline, the VHT selection process was already rigged, especially considering that in some communities literate people are limited. It is not coincidental that Aida (in the quote above) says that she is 'always' selected. The problem this leaves is whether this requirement helps in selecting volunteers who are motivated to do the work, or who have the community support. It was not surprising that once VHTs lost the allowances from AMREF, many gave up the work while others clung to the position in anticipation of future benefits.
Kibazo, a middle-aged primary school teacher, was selected as a VHT. When the author had a focus group discussion with VHTs, he did not come. His colleagues mentioned that they did not expect him to come. When the author met Kibazo, said that as a teacher with a small salary, he has to do private business that brings him money rather than going 'around the community' teaching people about toilet use. He was clearly not motivated to volunteer but may have been selected because of the literacy requirement. Informally, people in the village kept saying that VHT work was for the educated.
Ironically, the guidelines required that people with leadership and previous community work experience, like teachers, church readers, drug distributors, and traditional birth attendants, should have priority. This gives advantages to elites in the community, which in rural communities often includes LCs and other powerful members in positions of social responsibility due to similar qualification criteria.
The district health officer was rather indifferent about the literacy requirement in the selection of VHTs since he felt that basic literacy was not sufficient for the work VHTs were meant to do, such as health data collection and record-keeping. He was pessimistic that mere training could facilitate VHTs to take on such tasks.
Discussion
It is widely acknowledged that the biggest challenge in CHW programs is attrition. Many scholars have argued that in order to improve the sustainability of CHW volunteers, the need for community support cannot be ignored5,11. This therefore takes us back to the principle of community participation, which was the pivotal principle for PHC interventions at the Alma Ata. The community as a united entity may not exist in every community since communities are made up of actors with different aspirations, interests, power structures, and dynamics4. The stakeholders in community interventions need to pay close attention to economic, social, and cultural factors that are inherent in all communities, especially in the process of selecting community representatives43. In this article, the argument is that 40 years after the Alma Ata the principle of community participation has continued to be used rhetorically in PHC interventions across many communities.
First, the findings presented reaffirm the need for transparency in determining responsibility for the selection of CHWs from the community, as has been asserted11. The roles of the government and NGOs should be to provide oversight and ensure that CHWs reflect the will of the community without obstruction from community power-holders. Absence of this oversight permits the influence peddling of power-brokers within the dynamic community structures and thus may marginalize the population they ought to serve. Such obstructionism has been reported in studies evaluating CHW programs where researchers argue that without evidence of systematic inclusion of various community sections, the assumption that the selected CHWs represent the community from which they are drawn may be erroneous24. Influence peddling by LCs in this case, motivated by expectations of authority, reward, and other benefits, supports what has been called 'distortion of information' to facilitate elite capture44. The misconception that a rural community is a homogeneous entity with persons of shared interests oriented towards mutual cooperation has long been debunked45,46. Such a realization ought to have inspired pragmatic awakening in 21st-century PHC interventions.
Second, and surprisingly, the findings exemplify the issue of intransigent national guidelines that are deliberated in a top-down fashion from the national level to fit all rural communities in the selection of VHTs. Such guidelines ignore the transient nature of communities and heterogeneity within communities over space and time. The national guidelines became both a facilitator for the manipulation of local communities and elite capture by the community's local power-brokers. Powerful community members, namely LCs, used both laxity and strictness in following national guidelines to influence the VHT selection process. Such machinations have been variously acknowledged in other development change initiatives in development literature47. The fact that certain members of the community were privy to some information regarding the VHC project gave them an upper hand to flex others out, especially where high expectations of reward and benefit abound. It is not new that those who access information try to utilize it to gain undue advantage over their colleagues in such initiatives, as has been reported in some studies44. Strong supervision of the selection process at all levels is not just necessary but is an important safeguard against influence peddling by powerful leaders who may use the guidelines to benefit themselves and gain more power.
Timely engagement of all community members prevents haphazard implementation of the program and thus reduces the chances for alienating some community members. This corroborates Bishop and others48, who said that selection should take cognizance of the unique socio-political and cultural aspects that permeate the existing informal support networks. Such considerations ensure that volunteers who are motivated to volunteer and are seen as helpful to the community are selected. Since the value of the CHW is related to the embeddedness of the health worker in the community, consideration of the understanding of community dynamisms and structures cannot be over-emphasized.
This study re-highlights the importance of understanding the various social, economic, and cultural dynamics that underlie community dynamism in the implementation of PHC interventions in rural and remote communities. Community participation that is dictated by top-down, inflexible guidelines may be double-edged. While it may be phrased in such a way that calls for the empowerment of the rural poor, such an intervention may be too easily manipulated to deflect responsibility from powerful actors representing local governments, NGOs, and powerful elites, thus promoting further alienation and increased inequality.
When CHW programs are built on a screening and selection process designed from without the community and uniform criteria are applied in all communities across the country, there is the danger that peculiar situations in particular communities will not be considered. Flexibility in implementation of the criteria for selection and recruitment is necessary so that specific characteristics of various communities are taken into consideration. Communities are heterogeneous both internally and externally; applying standardized criteria may not work to the best interests of the communities that are targeted to benefit from such interventions. In a nutshell, there is need for progressive and constant community engagement that understands community participation as an iterative process. Forty years after the Alma Ata Declaration, which called for the participation of local communities in interventions for the improvement of their health, the failure of such CHW programs to learn these lessons underscores the sustainability challenges that continue to plague community health interventions in the developing world.
Although this study is limited in geographical coverage, it is rich in details about the interface between local leaders and community members in the selection of VHTs in a specific village of Luwero. The findings may not be extrapolated to other communities. However, this limitation does not disavow the fact that the findings are important. The findings in this study may be insightful in strengthening such CHW interventions where volunteers are selected from communities with similar characteristics, especially in Uganda and sub-Saharan Africa.
Acknowledgement
This work is part of the research program CoHeRe (Developing Sustainable Community Health Resources in Poor Settings in Uganda), which is financed by the Netherlands Organization for Scientific Research.
References
1. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. Geneva: WHO, 2010.
2. Cueto M. The origins of primary health care and selective primary health care. American Journal of Public Health 2004; 94(11): 1864-1874.
3. Standing H, Chowdhury AMR. Producing effective knowledge agents in a pluralistic environment: what future for community health workers? Social Science and Medicine 2008; 66(10): 2096-2107.
4. Rifkin SB. Paradigms lost: toward a new understanding of community participation in health programmes. Acta Tropica 1996; 61(2): 79-92.
5. van Ginneken N, Lewin S, Berridge V. The emergence of community health worker programmes in the late apartheid era in South Africa: an historical analysis. Social Science and Medicine 2010; 71(6): 1110-1118.
6. WHO, UNICEF. Primary health care: report on the International Conference on Primary Health Care, Alma Ata, USSR. WHO: Geneva, 1978.
7. Maru RM. The community health volunteer scheme in India: an evaluation. Social Science and Medicine 1983; 17(19): 1477-1483.
8. Berman PA, Gwatkin DR, Burger SE. Community-based health workers: head start or false start towards health for all? Social Science and Medicine 1987; 25(5): 443-459.
9. Cherrington A, Ayala GX, Elder JP, Arredondo EM, Fouad M, Scarinci I. Recognizing the diverse roles of community health workers in the elimination of health disparities: from paid staff to volunteers. Ethnicity and Disease 2010; 20(2): 189-194.
10. Flax VL, Earp JL. Counseled women's perspectives on their interactions with lay health advisors: a feasibility study. Health Education Research 1999; 14(1): 15-24.
11. Glenton C, Lewin S, Scheel IB. Still too little qualitative research to shed light on results from reviews of effectiveness trials: a case study of a Cochrane review on the use of lay health workers. Implementation Science 2011; 6(1): 53.
12. Walt G, Perera M, Heggenhougen K. Are large-scale volunteer community health worker programmes feasible? The case of Sri Lanka. Social Science and Medicine 1989; 29(5): 599-608.
13. Menon A. Utilization of village health workers within a primary health care programme in The Gambia. American Journal of Tropical Medicine and Hygiene 1991; 94(4): 268-271.
14. Sauerborn R, Nougtara A, Diesfeld H. Low utilization of community health workers: results from a household interview survey in Burkina Faso. Social Science and Medicine 1989; 29(10): 1163-1174.
15. Kahssay HM, Taylor ME, Berman PA. Community health workers: the way forward. Geneva: World Health Organization, 1998.
16. Akintola O. What motivates people to volunteer? The case of volunteer AIDS caregivers in faith-based organizations in KwaZulu-Natal, South Africa. Health Policy and Planning 2010; 26(1): 53-62.
17. Mburu F. Whither community health workers in the age of structural adjustment? Social Science and Medicine 1994; 39(7): 883-885.
18. Rifkin SB. Lessons from community participation in health programmes: a review of the post Alma-Ata experience. International Health 2009; 1(1): 31-36.
19. Akintola O. Perceptions of rewards among volunteer caregivers of people living with AIDS working in faith-based organizations in South Africa: a qualitative study. Journal of the International AIDS Society 2010; 13(1): 22.
20. Bloom G, Standing H. Pluralism and marketization in the health sector: meeting health needs in context of social change in low and middle income countries. Working paper 136. Brighton, UK: Institute of Development Studies, 2001.
21. Maes KC, Kohrt BA, Closser S. Culture, status and context in community health worker pay: pitfalls and opportunities for policy research. A commentary on Glenton et al. (2010). Social Science and Medicine 2010; 71(8): 1375-1378.
22. Schneider H, Hlophe H, van Rensburg D. Community health workers and the response to HIV/AIDS in South Africa: tensions and prospects. Health Policy Plan 2008; 23(3): 179-187.
23. Watt P, Brikci N, Brearley L, Rawe K. No child out of reach: time to end the health worker crisis. London: Save the Children, 2011.
24. Bhutta ZA, Lassi ZS, Pariyo G, Huicho L. Global experience of community health workers for delivery of health related millennium development goals: a systematic review, country case studies, and recommendations for integration into national health systems. Geneva: Global Health Workforce Alliance, World Health Organization, 2010.
25. Liu A, Sullivan S, Khan M, Sachs S, Singh P. Community health workers in global health: scale and scalability. Mount Sinai Journal of Medicine 2011; 78(3): 419-435.
26. Davidson PL, Andersen RM, Wyn R, Brown ER. A framework for evaluating safety-net and other community-level factors on access for low-income populations. Inquiry 2004; 41(1): 21-38.
27. Lawn JE, Rohde J, Rifkin S, Were M, Paul VK, Chopra M. Alma-Ata 30 years on: revolutionary, relevant, and time to revitalise. Lancet 2008; 372(9642): 917-927.
28. Rosato M, Laverack G, Grabman LH, Tripathy P, Nair N, Mwansambo C, et al. Community participation: lessons for maternal, newborn, and child health. Lancet 2008; 372(9642): 962-971.
29. Singh P, Sachs JD. 1 million community health workers in sub-Saharan Africa by 2015. Lancet 2013; 382(9889): 363-365.
30. Gilroy K, Winch P. Management of sick children by community health workers. Intervention models and programme examples. Geneva: World Health Organization/UNICEF, 2006.
31. Nabuguzi E. Popular initiatives in service provision in Uganda. In: J Semboja (Ed). Service provision under stress in East Africa. London: Heinemann, 1995; 192-208.
32. Ministry of Finance Planning and Economic Development. Challenges and prospects for poverty reduction in northern Uganda. Discussion paper 5. Kampala: Ministry of Finance, Planning and Economic Development, 2002.
33. Sekimpi KD. Report on study of community health workers in Uganda (with focus on village health team strategy - VHT). Kampala: Ministry of Health, 2007.
34. Ministry of Health. Mid-term analytical review of performance of the Health Sector Strategic and Investment Plan 2010/11-2014/15. Kampala: Ministry of Health, 2013.
35. Ministry of Health. The annual health sector performance report for 2012/13 financial year. Kampala: Ministry of Health, 2014.
36. Lehmann U, Sanders D. Community health workers: what do we know about them? Geneva: WHO, 2007.
37. Prasad B, Muraleedharan V. Community health workers: a review of concepts, practice and policy concerns. Geneva: International Consortium for Research on Equitable Health Systems (CREHS), 2007.
38. Rifkin SB. Community participation in maternal and child health/family planning programs. An analysis based on case study material. Geneva: WHO, 1990.
39. Zakus JDL. Resource dependency and community participation in primary health care. Social Science and Medicine 1998; 46(4): 475-494.
40. Linda S. Cultural influences in community participation in health. Social Science and Medicine 1992; 35(4): 409-417.
41. Nichter M. Global health: why cultural perceptions, social representations, and biopolitics matter. Tucson, AZ: University of Arizona Press, 2008.
42. Ministry of Health. Village health teams: strategy and operational guidelines. Kampala: Ministry of Health, 2010.
43. Lehmann U, Friedman I, Sanders D. Review of the utilisation and effectiveness of community-based health workers in Africa. Joint Learning Initiative on Human Resources for Health and Development working paper. Cape Town: Global Health Trust, Joint Learning Initiative on Human Resources for Health and Development, 2004.
44. Platteau J, Somville V, Wahhaj Z. Elite capture through information distortion: a theoretical essay. Journal of Development Economics 2014; 106: 250-263.
45. Meleis AI. Community participation and involvement: theoretical and empirical issues. Health Service Management Research 1992; 5(1): 5-16.
46. Madan T. Community involvement in health policy; socio-structural and dynamic aspects of health beliefs. Social Science and Medicine 1987; 25(6): 615-620.
47. Alatas V, Banerjee A, Hanna R, Olken BA, Purnamasari R, Wai-Poi M. Does elite capture matter? Local elites and targeted welfare programs in Indonesia. National Bureau of Economic Research working paper series. Cambridge, MA: NBER, 2013.
48. Bishop C, Earp JA, Eng E, Lynch KS. Implementing a natural helper lay health advisor program: lessons learned from unplanned events. Health Promotion Practice 2002; 3(2): 233-244.
