Aboriginal children (First Nations, Inuit and Métis) are the fastest growing segment of the pediatric population in Canada1,2. The Aboriginal population in Canada was estimated at 1.4 million, or 4.3% of the Canadian population, based on the 2011 National Household Survey1. This reflects population growth of 20.1% between 2006 and 2011, compared with 5.2% growth of the non-Aboriginal population1. Within this population, 62.5% identified as First Nation, 33.1% as Métis, and 4.4% as Inuit. Approximately 36% are children aged 18 years or less1. There are unique challenges to the planning and evaluation of services for Aboriginal children. For example, in Ontario, about half of First Nation children reside on one of 133 First Nation reserves3, most of which are geographically isolated4. In 2009, these communities collectively ranked 68th on the Human Development Index, while Canada ranked third internationally2.
Aboriginal children experience serious health inequities compared to their mainstream peers2,5. A key example is the high rate of youth suicide, which is typically five to six times the mainstream average6,7 and, when combined with self-inflicted injury, is the leading cause of death among Aboriginal youth (ages 10-19 years)8. Métis and Inuit children also experience significant health inequities2. Because many Aboriginal children live in rural and/or remote communities, they rely on local health services for support.
While much of Canada now practices health care using evidence-based medicine9,10, Aboriginal health centers have not had access to culturally relevant and contextually feasible tools to gather local evidence to inform practice in a resource-constrained environment9.
The Aboriginal Children's Health and Well-being Measure (ACHWM) is a child self-report measure that assesses health and wellbeing11. It was developed to address the needs of Aboriginal health directors, to gather local data to guide the planning and evaluation of health services. Mainstream measures were not appropriate for use in their communities11. Thus, cultural relevance was of critical importance in the development process.
The ACHWM (or Aaniish Naa Gegii as it is known in Ojibway, a tribal nation of Wiikwemkoong) was developed as part of a collaborative research project co-led by a First Nation health director and an academic researcher from Laurentian University, Ontario, in 2010 and 201111, who worked in collaboration with other Aboriginal health leaders and Elders. First Nation children were actively engaged in the process throughout its development and testing. It is culturally appropriate for First Nations children and has been successfully adapted for independent completion by children (ages 8-18 years) using Android tablets. This approach to measuring Aboriginal child health is valid12,13, reliable14, and has the support of the Chiefs of Ontario (All Ontario Chiefs Conference Resolution #13/15).
While the development began in one community, the intent was always to ensure its relevance to other Aboriginal communities, including other First Nations, Inuit and Métis children11 . The purpose of this article is to document the tailoring of the ACHWM to meet the needs of other Aboriginal communities in Canada. In this article the term 'community' is broad and includes geographic communities (eg First Nations) and agencies that serve multiple communities.
Since the ACHWM is a measure of health and wellbeing, the guidelines for quality of life measures were considered most appropriate for use in this study. The literature on cross-cultural adaptation of quality-of-life measures recommends a detailed review of the question content and translation of questions into the new language, followed by an extensive interview process15-17. In 2009, a revised set of guidelines was published to adapt the process for use with rare conditions18. The adaptation process is important to ensure that the measure's interpretation and meaning is congruous across different cultures. This article follows the guidelines published by Price et al. (2009), which have previously been applied by members of this team (NLY and TAB)18-22.
During 2013 and 2014, a small research team led by a First Nation Health Director (MJW) and a university professor (NLY), engaged four new communities in this collaborative research. These communities were selected to reflect regional diversity in Ontario, and included Weechi-it-te-win Family Services (WFS), M'Chigeeng First Nation, Whitefish River First Nation, and the Ottawa Inuit Children's Centre (OICC). The Wiikwemkoong Unceded Territory completed this process as part of the initial development of the ACHWM11, previously published12. The Métis community in Sudbury has also participated in this process23. Their results are presented in a separate article as part of a graduate student project. Researchers from Laurentian University and health leaders from Wiikwemkoong combined to form the ACHWM team on this project.
Communities
The ACHWM originated in Wiikwemkoong, an unceded (non-treaty) community of First Nation people located on Manitoulin Island in north-eastern Ontario. The people of Wiikwemkoong have resided on these lands since the 17th century and come from three tribal nations: Odawa, Pottawatomi and Ojibway. Together they form the Three Fires Confederacy. Their lands comprise 42 547 ha on Manitoulin Island and 13 806 ha on the mainland. The Wiikwemkoong band membership is estimated at 7200 with approximately 45% living on-reserve in one of seven settlements: Kaboni, Buzwah, South Bay, Rabbit Island, Murray Hill, Cape Smith, and Wikwemikongsing. The community has many health-related resources including a health centre, nursing home, ambulance station and youth centre run by the health department. The community also has three schools, covering kindergarten to grade 12.
WFS is an Indigenous child welfare agency supporting 10 remote First Nations from north-western Ontario. The 10 communities are all independent First Nations within the Treaty #3 (1873) region of Ontario: Big Grassy, Big Island, Couchiching, Lac La Croix, Naicatchewenin, Nigigoonsiminikaaning, Rainy River, Ojibways of Onigaming, Seine River, and Mitaanjigamiing First Nations. WFS was founded with a vision of revitalizing an Anishinabe childcare system rooted in the customs, traditions and values of the Anishinabe people. It was granted status as a child welfare agency in 1987. The agency advocates for a system that places emphasis on family preservation, community healing and the revitalizing of traditional laws, structures, and practices in order to restore balance and meaning to the lives of their people. At the time of implementation, WFS was caring for approximately 124 children between the ages of 9 to 19 years from the 10 communities.
M'Chigeeng is a First Nation community located on Manitoulin Island, along the shores of the North Channel of Lake Huron, in north-eastern Ontario. The M'Chigeeng territory was settled in the mid-19th century and has a registered band membership of 2543 of which approximately 40% live on reserve lands of 3095 ha (Bond Head Treaty #45 (1836) and McDougal Treaty #94 (1862)). This community has a health centre and an elementary school serving kindergarten to grade 8 (Lakeview), with older children being required to leave the community for education within the mainstream educational system, a 15-minute drive away. This First Nation is a member of the Anishinabek Nation of the Union of Ontario Indians and United Chiefs and Councils of Mnidoo Mnising.
Whitefish River is a First Nation community located on the shores of Georgian Bay and the North Channel in north-eastern Ontario. It has 1200 band members and approximately 37% live on the First Nation reserve. Their land base is 5600 ha (Robinson-Huron Treaty #61, 1850). This community has an elementary school (Shawanosowe) educating children from kindergarten to grade 6, with older children being required to leave the community for education within the mainstream educational system, a 25-minute drive away.
The OICC is a not-for profit agency that supports Inuit children living in Ottawa, Ontario. This center provides cultural, educational, recreational and social support services to urban children and families. This center enabled the team to assess the relevance of the ACHWM to Inuit children. The vast majority of Inuit in Canada live in the far north, in remote communities, accessible primarily by air or sea. There is an historical link between the Inuit communities in the north and Ottawa, because Inuit who require secondary or tertiary health care have been medically evacuated to urban centres, primarily Ottawa, for many decades. As a result, the largest Inuit populations outside of the north are in Ottawa. Many of the children who are affiliated with OICC have recently arrived from the far north. Thus, the OICC provided insights into the Inuit culture, with the understanding that future studies would need to be completed in Canada's far north.
All communities volunteered to participate in this project. The research was conducted as a collaboration between the ACHWM development team (Wiikwemkoong Unceded Territory and Laurentian University), and each new partner community. Thus, there were four research agreements (one for each community) that were each signed by the collaborating teams.
Cultural adaptation process
The relevance to each of the four new communities was assessed independently, through an iterative process that had three sequential steps. A similar process had previously been used by members of this team (NLY, TAB) in other contexts18,19,24. One important alteration in the process was implemented: there was no requirement to come to consensus; rather, each community was permitted to modify the measure to fit the needs of their children. This was important to reflect the diversity of the sample and respect the autonomy of the sovereign nations. As each community completed the process, the findings were reviewed by the research team and shared with all other communities. Thus, each community started the process with the benefit of being aware of the results from previous communities, and at the end each community had access to lessons learned from preceding communities.
The first step was to determine whether the questions within the ACHWM were considered appropriate from the perspectives of health leaders, mental health workers, and Elders in the new community. If key concerns were identified, these were addressed and adaptations were made to the ACHWM.
The second step was to determine whether the questions within the ACHWM were interpreted in a consistent and accurate way by children between the ages of 8 and 18 years in that community. This was assessed through detailed cognitive debriefing, in which children and parents (or primary caregivers) completed the ACHWM as part of detailed interview. During the interview the participant read out loud and was asked to articulate examples, to ensure their understanding of the questions and selection of appropriate responses. Children were selected to represent a mix of boys and girls across the age spectrum. The primary caregiver of each child was invited to participate in a separate concurrent interview. These interviews were conducted by health workers from the community who had been trained by the ACHWM team. A member of the ACHWM team attended all interviews to take notes on the findings. Thus, there were three participants for each interview: one child or parent, one community health team member, and one ACHWM team member. Often the child and parent interviews were conducted simultaneously, in separate rooms. All interviews were conducted in a location selected by the local health team.
During the interview, the participant (child or parent) was asked to read questions out loud while the note-taker listened for words that were difficult. Participants were probed for examples to support their choice of answers as a way to ensure they understood the concept. The local health team member guided the participant through the survey and facilitated discussion of any problem areas. When concerns were identified, the participants were asked to suggest solutions (ie alternative wording of questions). The ACHWM team member recorded detailed information on the findings in a database. After each pair of interviews (child and parent) was complete, the whole team discussed the findings briefly. The ACHWM process requires a brief meeting with a local health worker immediately after the survey, when necessary to ensure support for the child.
The third step focused on revisions to improve the questions in the context of the new community. After every second or third pair of interviews was completed, there was an extensive discussion based on the findings, to determine if there were consistent problems with specific questions across multiple respondents that needed to be addressed. When consistent problems were identified, the ACHWM was revised based on solutions recommended by participants. The revised survey was presented to the next pair of participants to determine if the revision was consistently and accurately understood. This iterative process continued until a stable and well-understood version was achieved.
This process was conducted in one community at a time, beginning with Weechi-it-te-win and ending with the OICC. Weechi-it-te-win began with the original 58-question version of the ACHWM11. M'Chigeeng began with the original 58-question version showing the changes that were made in Weechi-it-te-win. This process continued, and at the end the survey with revisions made by all communities was shared with all other communities so that the learning was cumulative.
Analysis
The results from the four new communities were aggregated and reviewed by the ACHWM team. The team identified the common findings and adaptations across all communities. The collective findings were shared with all communities and each was given the opportunity to independently incorporate or disregard the changes that had been identified by others.
Ethics approval
Approvals were obtained from the Laurentian University Research Ethics Board (2014-05-10, 2014-05-14, 2014-08-11, 2014-12-01), the local Board of Directors at Weechi-it-te-win and OICC, Chief and Council in M'Chigeeng First Nation and Whitefish River First Nation, and from the Manitoulin Anishinaabek Research Review Committee.
Most communities required a minimum of three detailed preparation meetings to conduct this collaborative research. The local community leaders (SB, RB, LM and KBA) played a critical role as champions for the project within their respective communities.
The initial review of the measure by experts in three of the communities did not identify any changes that were essential to implement prior to presenting the survey to children and parents as part of the second stage of the process, with one important exception. The local team at the OICC identified five questions that required changes to reflect Inuit culture. An example of a community-specific adaptation was the concept of 'mother earth' which is a key component of Anishinabe culture, but is not recognized by the Inuit. However, through discussion with children, parents, and leaders at the OICC it was determined that 'the land' is a parallel concept among the Inuit. Changes such as these were unique to each community, but resulted in a survey that was consistently interpreted at the level of the overall concepts addressed.
The cognitive debriefing interviews were completed in June 2014 (Weechi-it-te-win), August 2014 (M'Chigeeng), October 2014 (Whitefish River) and January 2015 (OICC), involving a total of 23 children, 21 caregivers and numerous local staff. The children had a mean age of 10.9 years (standard deviation 2.7, range 8.1-18.3 years). Key lessons were learned in all communities that enabled the team to improve the ACHWM in subtle but important ways. During the collective process with four new communities a total of 23 questions (37%) underwent minor revisions: 12 questions had important changes across all communities, nine questions had community-specific adaptions and four new questions were added. (Two of the new questions underwent both changes for all communities and had a community-specific variation.) Examples are provided below. This process resulted in a stable version of the ACHWM that is now relevant across diverse communities. The collective results were shared with participating communities in March 2015. The results from all four communities are summarized in Table 1.
Table 1: Overview of changes to the Aboriginal Children's Health and Well-being Measure, by community
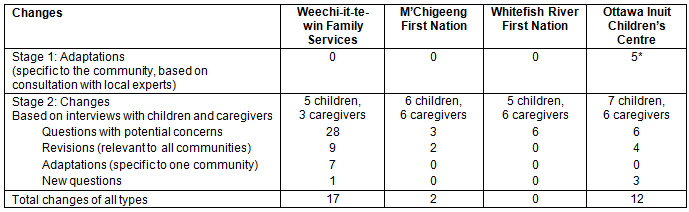
Summary of changes for each community
At Weechi-it-te win, concerns were identified on 28 questions. Within this group, eight concerns were related to reading specific words and did not require revisions because the tablet has the ability to read to children. Furthermore, 10 of the concerns were isolated to a few individuals, and were inconsistent, thus revisions were not required. Revisions were made to nine questions based on participants' comments. Five of these changes were to remove the possessive pronoun 'my' preceding 'elders'. Seven questions referred to 'family' or 'community'. Since many participants identified with one or more family and community, the wording in the WFS version was changed to be inclusive of all families and communities. In addition, one question was adapted for this community and one new question was added based on the results obtained from WFS.
In M'Chigeeng, concerns were identified on three questions. Within this group, one concern was related to reading specific words and no changes were made because the tablet's text-to-speech function can accommodate lower literacy levels. Changes were made to two questions to improve the understanding of those questions, and the new question developed in WFS was confirmed in M'Chigeeng. Thus, a total of two changes were made based on the experiences in M'Chigeeng.
In Whitefish River, concerns were identified on six questions. Within this group, two concerns were related to reading specific words and no changes were required. The remaining concerns were isolated to a few individuals and were inconsistent, thus did not require revisions. Thus, all questions were confirmed based on the experiences in Whitefish River.
At the OICC, concerns were identified on six questions. Within this group, concerns on two questions were isolated and did not require changes. Most importantly, the participants identified three new questions. For example, the children at the OICC identified the importance of food security and generated a new question, 'I worry about getting enough to eat'. A total of 11 changes were made based on the results from OICC. These three new questions were subsequently reviewed and accepted by all other communities, and have become part of the ACHWM for use in all communities.
It became clear in working with each community that the naming and logo for the survey were important because they influenced the degree to which the children viewed the survey as being relevant to them. The initial name of the survey was the Aboriginal Children's Health and Well-being Measure (ACHWM), and the project logo incorporates two children and the medicine wheel symbol. The formal name is still used as the primary identity for the measure. In January 2014 the survey was given an Ojibway name by the children in Wiikwemkoong. They call it Aaniish Naa Gegii, meaning 'how are you' in Ojibway. The Inuit perceived the medicine wheel component of the logo as a sign that this survey was not culturally relevant to their community. It was agreed that each community was free to refer to the measure with a name in their native language, as a way to ensure it was seen in a good way. Thus, the survey is known as Aaniin Ezhi-Yaayin at WFS, who use a north-western Ontario dialect of Ojibway. The ACHWM continues to be known as the Aaniish Naa Gegii in the Ojibway nations of Wiikwemkoong, M'Chigeeng and Whitefish River First Nation. It is known as Qanuippit in Inuktitut at the OICC. Additionally, the OICC have adopted a modified logo with the permission of the ACHWM developers. This enhances the relevance of the measure for each community.
Two aspects unique to the collaborative approach of this project are worthy to note. The first was the research agreement, achieved through explicit discussions between the researchers and community collaborators, in which all team members shared their goals and their expectations. This process was very valuable in the development of common goals specific to the local context of each participating community and led to research agreements that were tailored to address the needs of all partners. Second was the inclusion of children and parents throughout the study, who were engaged in interviews, designed to fine-tune the survey. Local staff were trained to conduct the interviews, with the support of an ACHWM team member, to improve the comfort level of the children. These interviews provided great value in uniting team members and building collaboration through shared experiences with the local children.
Discussion
The ACHWM is one of very few measures that have been developed intentionally for Aboriginal children. Because of the cultural diversity between Aboriginal communities, it is important to assess the relevance for other communities that are geographically distant and/or culturally distinct from these four communities. This article presents a well-tested process as a template for assessing local relevance and adapting the ACHWM, if necessary, to meet specific local needs.
This article also reports the results of detailed cognitive debriefing sessions in four Aboriginal communities. Two of the communities who participated in this collaboration were rural First Nations, and a third (Weechi-it-te-win) was a child welfare agency supporting First Nations children from 10 rural/remote First Nations. Similar findings from an Inuit population (reported in this article), as well as findings from interviews with Métis children and caregivers (reported separately) suggest that the results are robust in a region that spans 1800 km within Ontario. Consensus on the content was achieved through collaboration between academic researchers, health leaders in Aboriginal communities, and through the active participation of children and caregivers in each community. Furthermore, consultations with health and education providers in many other First Nation communities, located in more remote areas of the far north in Ontario, suggest that results are relevant to remote First Nations.
The authors encourage other Aboriginal communities across Canada and Indigenous communities internationally to consider the ACHWM and the cultural adaptation process described here as a foundation for child-health assessment to meet the needs of their communities. This is in keeping with the approach of this research program, guided in part by the recommendations from the Many Hands One Dream summit in 2005, to ensure that solutions come from within each community25 and foster empowerment26.
The revised 62-item version of the ACHWM is the main product from this research, which now incorporates important concepts from culturally diverse communities. The results provide a foundation for Aboriginal child health self-assessment that may be relevant elsewhere in Canada and with Indigenous communities internationally. The ACHWM is available for use by Aboriginal communities and agencies. More information is available on the project's website27. The ACHWM is able to provide statistical information on overall health and wellbeing and the four quadrant scores that are relevant at the level of a First Nation, agency or program. This local information can inform health directors and program managers about the health status of their population and aid in tracking change over time to evaluate the impacts of programs and services.
Research agreements are a recommended best practice. Based on this research project, the authors also encourage the active involvement of children early in the research process as a best practice. Together, these practices ensure that the voices of communities, as well as the words of the children and their caregivers and guardians, are prioritized. Furthermore, the authors recommend a collaborative approach that ensures: (1) engagement of a local champion (preferably a manager or director) who can navigate the required approvals and support the implementation at a local level; (2) access to appropriate health resources (eg mental health workers) to support implementation, (3) flexibility within the team to adapt to the local context, (4) an understanding of cultural protocols, (5) commitment by all team members to collaboration and capacity building, and (6) several face-to-face meetings with excellent ongoing communication to achieve success.
Lessons learned through the stories of ancestors are of extraordinary value, but new knowledge co-generated through respectful research partnerships is also important. Through the collective and collaborative processes in four new communities, the ACHWM has been adapted to produce one version shared by all communities. This novel assessment process is community-driven and responds to a call to 'stop talking ..., listen and hear' the voices of children28.
Acknowledgements
We are grateful for the support of Sabine Kristensen-Didur, Lauris Werenko, Ed Didur, and Mélanie Trottier who contributed to the conduct of this research. Financial support for this research was provided by the Canadian Institutes for Health Research and the Ontario Ministry of Health and Long-Term Care (Health Systems Research Fund).
References
1. Statistics Canada. Aboriginal peoples in Canada: First Nations People, Métis and Inuit. National Household Survey 2011. (Catalogue #99-011-XWE2011001). (Internet) 2011. Available: https://www12.statcan.gc.ca/nhs-enm/2011/as-sa/99-011-x/99-011-x2011001-eng.cfm (Accessed 11 January 2016).
2. Canadian UNICEF Committee (2009). Canadian supplement to the state of the world's children. Aboriginal children's health: leaving no child behind. (Internet) 2009. Available: http://www.nccah.ca/docs/child and youth/Report Summary Leaving no child behind.pdf (Accessed 12 May 2010). https://doi.org/10.18356/afc0957d-en
3. Chiefs of Ontario. About the Chiefs of Ontario. (Internet) 2015. Available: http://www.chiefs-of-ontario.org/about-us (Accessed 23 November 2015).
4. Indigenous and Northern Affairs Canada. Ontario region. (Internet) 2015. Available: https://www.aadnc-aandc.gc.ca/eng/1100100020284/1100100020288 (Accessed 23 November 2015).
5. Health Canada. First Nations and Inuit Health strategic plan: a shared path to improved health. (Internet) 2012. Available: http://www.hc-sc.gc.ca/fniah-spnia/pubs/strat-plan-2012/index-eng.php (Accessed 10 May 2013).
6. Canadian Institute for Child Health. The health of Canada's children. (3rd Edn). Ottawa: Canadian Institute for Child Health, 2000.
7. Advisory Group on Suicide Prevention (Canada). Acting on what we know: preventing youth suicide in First Nations. (Internet) 2003. Available: http://www.hc-sc.gc.ca/fniah-spnia/alt_formats/fnihb-dgspni/pdf/pubs/suicide/prev_youth-jeunes-eng.pdf (Accessed 10 December 2014).
8. Adelson N. The embodiment of inequity: health disparities in Aboriginal Canada. Canadian Journal of Public Health/Revue Canadienne de Sante Publique 2005; 96: S45-S61.
9. Rychetnik L, Hawe P, Waters E, Barratt A, Frommer M. A glossary for evidence based public health. Journal of Epidemiology and Community Health 2004; 58(7): 538-545. https://doi.org/10.1136/jech.2003.011585
10. Sackett DL, Rosenberg WMC, Gray JAM, Haynes RB, Richardson WS. Evidence based medicine: what it is and what it isn't. Clinical Orthopaedics and Related Research 1996; 455: 3-5. https://doi.org/10.1136/bmj.312.7023.71
11. Young NL, Wabano MJ, Burke TA, Ritchie SD, Mishibinijima D, Corbiere RG. A process for creating the Aboriginal Children's Health and Well-Being Measure (ACHWM). Canadian Journal of Public Health 2013; 104(2): e136-e141.
12. Young NL, Wabano MJ, Ritchie SD, Burke TA, Pangowish B, Corbiere RG. Assessing children's interpretations of the Aboriginal Children's Health and Well-Being Measure (ACHWM). Health and Quality of Life Outcomes 2015; 13(105): 1-7. https://doi.org/10.1186/s12955-015-0296-3
13. Young NL, Wabano MJ, Usuba K, Pangowish B, Trottier M, Jacko D, Burke TA, et al. Validity of the Aboriginal Children's Health and Well-Being Measure: Aaniish Naa Gegii? Health and Quality of Life Outcomes 2015; 13(148): 1-7. https://doi.org/10.1186/s12955-015-0351-0
14. Young NL, Wabano MJ, Usuba K, Mishibinijima D, Jacko D, Burke TA. Reliability of the Aboriginal Children's Health and Well-Being Measure (ACHWM). Springer Plus 2016; 5(1): 2082-2087. https://doi.org/10.1186/s40064-016-3776-y
15. Beaton DE, Bombardier C, Guillemin F, Ferraz MB. Guidelines for the process of cross-cultural adaptation of self-report measures. Spine 2000; 25(24): 3186-3191. https://doi.org/10.1097/00007632-200012150-00014
16. Bullinger M, Alonso J, Apolone G, Leplege A, Sullivan M, Wood-Dauphinee S, et al. Translating health status questionnaires and evaluating their quality: the IQOLA Project Approach. International Quality of Life Assessment. Journal of Clinical Epidemiology 1998; 51(11): 913-923. https://doi.org/10.1016/S0895-4356(98)00082-1
17. Guillemin F, Bombardier C, Beaton DE. Cross-cultural adaptation of health-related quality of life measures: literature review and proposed guidelines. Journal of Clinical Epidemiology 1993; 46(12): 1417-1432. https://doi.org/10.1016/0895-4356(93)90142-N
18. Price VE, Klaassen RJ, Bolton-Maggs PH, Grainger JD, Curtis C, Wakefield C, et al. Measuring disease-specific quality of life in rare populations: a practical approach to cross-cultural translation. Health and Quality of Life Outcomes 2009; 7(92): 1-8. https://doi.org/10.1186/1477-7525-7-92
19. Klaassen RJ, Blanchette V, Burke TA, Wakefield C, Grainger JD, Gaedicke G, et al. Quality of life in childhood immune thrombocytopenia: international validation of the kids' ITP tools. Pediatric Blood & Cancer 2013; 60(1): 95-100. https://doi.org/10.1002/pbc.24257
20. Villaça P, Carneiro J, D'Amico E, Blanchette V, Brandão L, Cassis F, et al. Process and experience of crosscultural adaptation of a quality of life measure (CHO-KLAT) for boys with haemophilia in Brazil. Haemophilia 2013; 19(6): 861-865. https://doi.org/10.1111/hae.12213
21. Wu R, Zhang J, Luke KH, Wu X, Burke T, Tang L, et al. Cross-cultural adaptation of the CHO-KLAT for boys with hemophilia in rural and urban China. Health and Quality of Life Outcomes 2012; 10(1): 112-117. https://doi.org/10.1186/1477-7525-10-112
22. Young NL, St-Louis J, Burke TA, Hershon L, Blanchette V. Cross-cultural validation of the CHO-KLAT and HAEMO-QoL-A in Canadian French. Hemophilia 2012; 18(3): 353-357. https://doi.org/10.1111/j.1365-2516.2011.02703.x
23. Paquette T, Boulard J, Roy-Charland A, Young NL. Cross-cultural adaptation of a health measure for Métis children and youth. Paper presented at the International Society for Quality of Life Research 21st Annual Conference, Berlin, Germany, 2014.
24. McCusker PJ, Fischer K, Holzhauer S, Meunier S, Altisent C, Grainger JD, et al. International cross-cultural validation study of the Canadian Haemophilia Outcomes: Kids' Life Assessment Tool. Haemophilia 2015; 21(3): 351-357. https://doi.org/10.1111/hae.12597
25. Saylor K, Blackstock C. Many Hands, One Dream: healthy aboriginal children and young people. Paediatric Child Health 2005; 10(9): 523-524.
26. Chandler MJ, Lalonde CE. Cultural continuity as a moderator of suicide risk among Canada's First Nations. In: L Kirmayer, G Valaskakis (Eds). The mental health of Canadian Aboriginal peoples: transformations, identity, and community. Vancouver, BC: University of British Columbia Press, 2008; 221-248.
27. Wiikwemkoong Unceded Territory and Laurentian University. Aboriginal Children's Health and Well-being Measure. (Internet) 2017. Available: http://www.achwm.ca/ (Accessed 14 March 2017).
28. Provincial Advocate for Children & Youth. Together we are ... feathers of hope: a First Nations youth action plan. Toronto: Office of the Provincial Advocate for Children and Youth, 2014.



