Introduction
The WHO has reported that 400 million people globally lack access to one or more essential health services.1 It suggests this is largely because of workforce shortages, skills mix imbalances between training and the realities of health workforce needs, and uneven geographical and socioeconomic distribution of professionally qualified doctors, nurses and midwives.2,3 With such shortages and maldistribution of health professionals and a persistent mismatch between education and health workforce needs, it has been proposed that health professional schools are essential partners in making universal health coverage a reality.4 Recent calls have been made for health professional schools to adopt ‘socially accountable’ approaches and align their curriculum with the needs of the population they serve5,6 – in particular, for schools located in more disadvantaged regions where local health inequities are often present, and more effective quality primary healthcare systems are needed.
Socially accountable health professional education (SAHPE) institutions focus their education, research and service priorities in response to current and future health and social needs of the communities in their region.7,8 The goal of SAHPE is to produce graduates willing and able to practise in all communities within their region, both rural and urban, and provide quality health care to all patients regardless of cultural, economic or ethnic background.6,9,10
Since 2008, over a dozen SAHPE schools in predominantly underserved and rural regions across the world have joined together as a global consortium – the Training for Health Equity Network (THEnet)11. To various degrees, these schools all provide their students with clinical experiences via a community-based, service learning approach. As there are distinctly different contexts at each school, some have further developed community-based learning into ‘community-engaged’ learning.10 Community-engaged learning stresses interdependent and reciprocal relationships between the school and the community served, with students learning experientially with the community and for the community, not simply about the community. In addition, students’ learning objectives and activities are fundamentally aligned to priority community healthcare needs, with the student at the centre of the partnership between the community and the medical school, with the ultimate aim of improving the health status of local communities.
In the Philippines, two medical schools, both foundation partners of THEnet, independently developed socially accountable, community-engaged training approaches: Ateneo de Zamboanga University-School of Medicine (ADZU-SOM) in the Zamboanga Peninsula region, and the University of the Philippines Manila-School of Health Sciences (SHS-Palo) in the Eastern Visayas region. ADZU-SOM, established in 1994, has a 4-year program, with students spending 1 month per semester in community placements across years 1–3, followed by 10 months of community placement in their fourth year, involving the mandatory completion of significant community development and public health activities. SHS-Palo Leyte, with its medical school established in 1976, has a 5-year degree including a 6-month community placement in second year, a later 1-year clinical internship, and then a 1-year community internship in the final year after which graduates qualify to take the Physicians Licensure Examination.
Entry to any medical school in the Philippines requires the applicant to hold a 4-year Bachelor degree. Philippines medical schools usually have a 4-year program, except for those schools that offer an MD-MPH program (students graduate with a degree in Medicine and Public Health), in which case a fifth year internship is added. After students successfully complete their fourth year, they are conferred the degree of Doctor of Medicine, but cannot legally practice medicine; by law, they are required to do a fifth year of clinical postgraduate internship. After this fifth year, they will have qualified to take the Philippines Licensure Examination covering 12 medicine disciplines (anatomy, physiology, surgery, paediatrics, etc.). Only when medical graduates pass this exam are they licensed to practice medicine in the Philippines.
Following these requirements, admission to ADZU-SOM thus requires the applicant to have graduated from a 4-year baccalaureate (Bachelors) degree. Specifically, the ADZU-SOM recruits graduate students from the Zamboanga Peninsula region based on undergraduate grade point averages and an interview; with about 35% of accepted students subsequently availing of scholarships based on financial need, with a return-of-service requirement of 1 year per year of scholarship. ADZU-SOM is unique to other medical schools in the Philippines as it has an MD-MPH program and a problem-based learning teaching philosophy.
While SHS-Palo also admits students into its program after they have completed a baccalaureate degree, the school is unique in the Philippines in having a ‘step ladder’ curriculum, which integrates the training of midwifes, nurses and medical doctors into one continuous and sequential curriculum. The majority of the students admitted to the medical program earned their baccalaureate degree by completing the midwifery and nursing levels of the step ladder curriculum. Students are nominated and endorsed by rural and disadvantaged communities in need of health workers, and then given scholarships by the university. Scholarships are tied with a return-of-service agreement to serve the community after graduation. In addition, some students who have completed a baccalaureate degree outside of SHS-Palo are admitted through the Medical Scholarship Program of the Philippines (previously the PINOY MD program) as a response to the urgent need for medical doctors in the rural Philippines. These students likewise have return-of-service contracts with the Department of Health to serve in identified areas in need of physicians. Thus, all students accepted into the SHS-Palo medical program are recruited from rural and/or disadvantaged areas and each student provided with a scholarship requiring a rural return of service.
Both schools have obtained success in graduate retention rate and distribution in local areas of need compared with national trends from conventional medical schools. For example, ADZU-SOM has more than 80% of its graduates practising in local Philippines communities compared to the national average of only 32% of medical graduates practising in the Philippines.12 In addition, ADZU-SOM graduates often practice in areas that previously did not have a doctor, resulting in a 55% increase in the number of municipalities in Zamboanga with a medical practitioner over the past two decades.13
Similarly, graduate tracking records at the SHS-Palo in Eastern Visayas shows some 90% of the school’s medical graduates still serving in local areas of dire need. In comparison, 51% of the graduates from the University of Philippines medical school based in Manila chose to practice abroad between 1954 and 1989, and for the 49% who chose to remain, three-quarters practiced in metropolitan Manila and only a quarter practised in other provinces.14
The present study describes how the practice locations of graduates from the SAHPE medical schools of ADZU-SOM and SHS-Palo differ from the practice locations of graduates from ‘conventional’ medical schools in the respective regions. The differences investigated include the population size and the socioeconomic category of the municipality or city where each graduate is practising. Geographical Information System (GIS) software was used to calculate the overall proportional medical coverage provided by medical graduates across municipalities in the Mindanao and Visayas regions.
This study is part of a series of multi-institutional collaborative research carried out by THEnet and its institutional partners to gather evidence on the outcomes and impact of SAHPE, using THEnet Social Accountability Framework as a logic model.
Methods
Design
The practice locations of licensed medical graduates who had practised for at least 6 months were collated from two Philippines SAHPE medical schools. For the ADZU-SOM in the Zamboanga Peninsula region of Mindanao Island, there were 10 graduating cohorts from 2003–2012, with 232 graduates in total meeting the study criteria of obtaining their licence and practising for at least 6 months. For SHS-Palo on the island of Samar in the Eastern Visayas region, there were 13 graduating cohorts from 1989 to 2013, with 121 graduates in total meeting the study criteria. Practice locations were also collated for a decade of licensed graduates coming from two Philippines medical schools having more conventional curriculums (464 and 264 graduates in total) whilst also located in the same geographical regions as the SAHPE schools – conventional school A located in Mindanao, and conventional school B located in the Visayas. Graduate practice locations were linked with population size and socioeconomic income class of the respective municipality or city where the community was located, and geo-coded into GIS software.
Data sources
Current postgraduate practice location data were accessed by a variety of strategies (see description of strategies in Table 1). For any municipality or city in which graduates were found to be practising, Wikipedia was used to access 2015 Philippines census and 2008 Department of Finance data, respectively, for population size15 and income classification for provinces, cities and municipalities.16
Longitude and latitude for each Philippines municipality or city in which a graduate was found to be practising was extracted from the Philippine GIS Data Clearinghouse website. These geocodes were added to the practice location database for each graduate. The data were collated and integrated in Microsoft Excel and then transferred to GIS software QGIS v2.10 (QGIS; http://www.qgis.org), where mapping was completed. QGIS heat maps (Fig 1a,b) were then calculated to display Philippines medical graduate practice location density across the Visayas and Mindanao regions. The heat maps display the density of graduates practising in regional centres relative to the density of graduates in the region’s capital city, with darker circles representing locations with a higher density of graduates, and lighter circles representing locations with just one or a few graduates. Figure 1a displays the density of practice locations for graduates from the two socially accountable medical schools (ADZU-SOM graduates based in the Zamboanga Peninsula and SHS-Palo Leyte graduates in the Eastern Visayas), and Figure 1b displays the density of practice locations for graduates from the two conventional medical schools (in Mindanao and the Visayas).
Table 1: Strategies for collecting graduate location data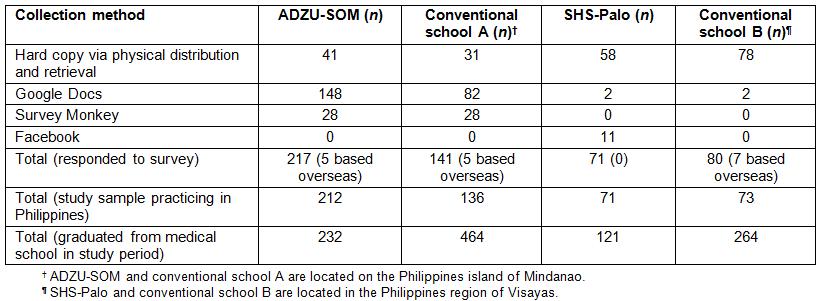
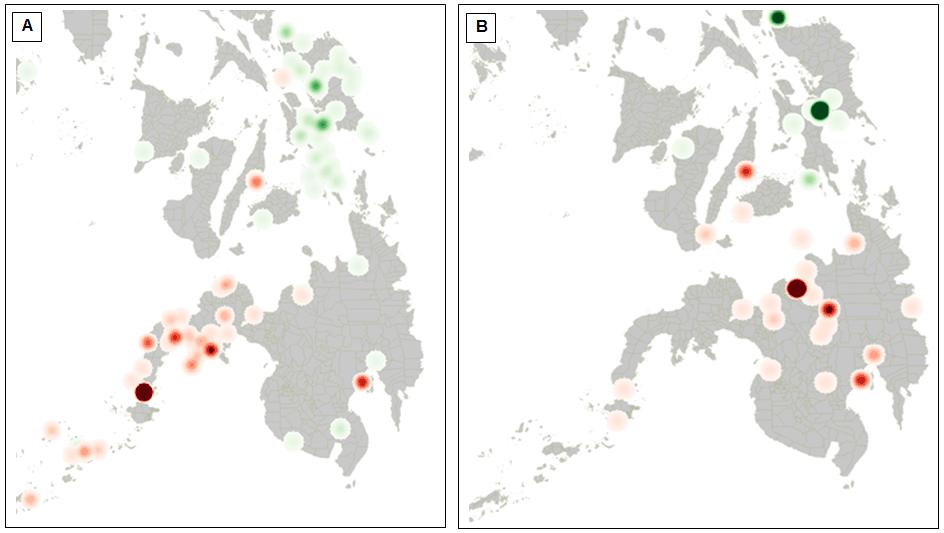 Figure 1: Heat maps of Philippines medical graduate practice location density from two socially accountable medical schools: (a) ADZU-SOM based in the Zamboanga Peninsula (red dots); and SHS-Palo Leyte in the Eastern Visayas (green dots)), and two conventional medical schools; (b) in Mindanao (red dots) and in the Visayas (green dots). The heat maps display the density of graduates practising in regional centres relative to the density of graduates in the region’s capital city, with darker circles representing locations with a higher density of graduates, and lighter circles representing locations with just one or a few graduates.
Figure 1: Heat maps of Philippines medical graduate practice location density from two socially accountable medical schools: (a) ADZU-SOM based in the Zamboanga Peninsula (red dots); and SHS-Palo Leyte in the Eastern Visayas (green dots)), and two conventional medical schools; (b) in Mindanao (red dots) and in the Visayas (green dots). The heat maps display the density of graduates practising in regional centres relative to the density of graduates in the region’s capital city, with darker circles representing locations with a higher density of graduates, and lighter circles representing locations with just one or a few graduates.
Bivariate analyses
Data for population size and socioeconomic income category were also coded numerically and entered in the computerised Statistical Package for Social Sciences v19 (SPSS; http://www.spss.com). Chi-squared tests for trend (two-sided) were used to assess bivariate relationships between the dependent variable (medical school of the graduates) with the population size (<50 000, 50 001–99 999, 100 001–999 999, >1 000 000) and income classification (1 QGISTM 6) of the municipality or city where the graduates practised. Statistical tests were considered significant, with p<0.05.
Ethics approval
Ethics approval for the study was obtained from the Ateneo de Zamboanga School of Medicine Ethics Review Committee, the University of the Philippines – Manila Research Ethics Committee (approval number RGAO-REG-2015-CM-F/C021(MED021), the Flinders University Human Research Ethics Committee (number 7042), and the respective ethics review committees of the conventional schools included in the study.
Results
Graduates’ current practice location in the Philippines was obtained for a total of 212, 71, 136 and 73 medical graduates for the medical schools of ADZU-SOM, SHS-Palo and the two conventional schools in the region, respectively, giving response rates of 91%, 59%, 29% and 28%, respectively. Thirty-one percent of ADZU-SOM graduates were practising in communities of <100 000 population versus 7% of conventional school A graduates (p<0.001), while 61% of SHS-Palo graduates were practising in communities of <100 000 population versus 12% of their conventional school B graduate peers (p<0.001) (Table 2).
Regarding the socioeconomic category of communities where the graduates were practising (Table 3), 27% of ADZU-SOM graduates were practising in lower income category municipalities or cities (categories 2–6) versus 8% of graduates from conventional school A (p<0.001). Similarly, 49% of SHS-Palo graduates were practising in lower income category municipalities or cities (categories 2–6) versus 11% of their conventional school B graduate peers (p<0.001) (Table 3).
For ADZU-SOM graduates, at least 212 (with one location not given) out of the total 232 graduates from 2003 to 2012 were currently practising in the Philippines (91%). Of these 212 ADZU-SOM graduates, 171 (81%) were practising in their home region of Zamboanga Peninsula. Overall, the 171 ADZU-SOM graduates were practising in 23 out of 67 municipalities (34%) across the Zamboanga Peninsula region. For the conventional school A graduates, at least 136 out of the total 464 graduates from the previous decade were found to be currently practising in the Philippines (29%), with 86 of the 136 (63%) practising in their home region of Mindanao across 10 of 84 municipalities (12%).
For the 71 SHS-Palo graduates who fitted the study criteria of practising in the Philippines for at least 6 months and completing the survey, 55 (78%) were practising in their home region of Eastern Visayas, with the remainder (16; 22%) returning to serve in rural and underserved communities from other regions in the Philippines where they originated.
For the 73 conventional school B graduates from the previous decade found to be practising in the Philippines, 70 out of the 73 (96%) located were practising in their home region of the Visayas. Overall, the 55 SHS-Palo graduates were practising in 26 out of 136 municipalities (19%) across non-metropolitan areas of the Visayas, while the 73 conventional school B graduates were found to be practising in 7 of 136 municipalities (5%) across non-metropolitan areas of the Visayas.
Table 2: Percentage of ADZU-SOM and SHS-Palo graduates practising in Philippines towns of different population size versus graduates of a more conventional medical school located in the same region.
Table 3: Percentage of ADZU-SOM and SHS-Palo graduates practising in Philippines towns of different income classification versus graduates of a more conventional medical school located in the same region.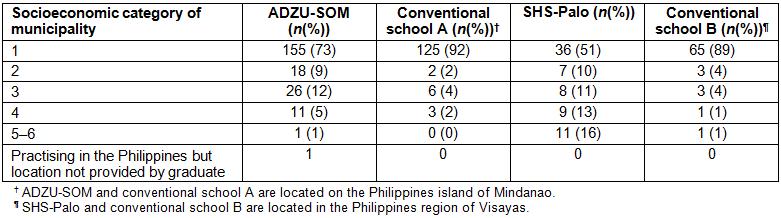
Discussion
The Philippines is an archipelago of 7107 islands, which creates great difficulty in providing adequate health workforce and access to health services in the more rural and remote areas. However, the findings of this study show that the SAHPE approach adopted by ADZU-SOM and SHS-Palo produces medical graduates who are significantly more likely to work in smaller and lower socioeconomic communities in their respective regions. In addition, ADZU-SOM and SHS-Palo graduates spread out to practise across proportionally more rural municipalities in their respective regions than the more conventionally trained graduates, who tend to practice more in larger, urban centres (clearly shown by Figs 1a,b). These findings suggest graduates trained to be socially accountable and community-engaged provide proportionally higher medical coverage across a Philippine region than a similar number of graduates from more conventional medical schools.
A number of selection and curriculum factors might explain why graduates of the two socially accountable medical schools are more likely to spread out across their respective regions regardless of geographic or socioeconomic constraints. Both schools have embraced social accountability as the guiding principle of their activities; in particular, targeted student recruitment aimed at accepting a significant proportion of students coming from lower socioeconomic strata of the local population, which may also increase later practice in underserved and/or rural areas. One study in Colorado, USA, of underserved (Hispanic) urban medical students found a similar pattern of being more likely to choose to practice in communities of similar ethnic and economic status17, while an international study of five socially accountable medical schools, each based in a different country, found having a selection process aimed at recruiting students from underserved communities produced strong intentions to work with underserved populations.9
In addition, with their focus on community-engaged medical education, SHS-Palo and ADZU-SOM schools provide students with early and extensive exposure to rural communities, and exposure to a curriculum that includes rural health issues and other rural health competencies. There is some evidence that the intensity of community-based engagement has previously been shown to be an important factor in the recruitment and retention of graduates in underserved areas18, and even simply basing students longer in the community positively contributes to rural recruitment and retention.19-22 Longer duration of community placement is shown to enhance social connectedness via the establishment of professional and community networks and community involvement,23-25 and predictably further increase this social connectedness due to the intensity of the year-long placement, where students live with community members.
It is also worthy to note that school graduate tracking records show 90% (141 out of the total 156) of the rurally bonded medical graduates from SHS-Palo are currently practising in the Philippines, many in areas that were previously doctorless and categorised as geographically isolated and disadvantaged. Those who left from earlier graduating cohorts had served for an average of 15 years. This reaffirms the policy recommendation that offering scholarships tied to return of service and aligning training of health workers with community and health system needs in settings close to their future workplace are both important factors in the retention of health workers in geographically isolated and disadvantaged locations.
Having more doctors spread across the region, in both underserved and urban centres, can only strengthen the regional health system by providing increased access to a doctor, including Filipinos living in areas of economic disadvantage. Increased access to medical services, including areas of socioeconomic disadvantage, is the foundation for achieving universal health coverage as a health system. Correlations between availability of health workers and better health outcomes have been reported across a number of cross-country ecological analyses26-30, with the 2006 WHO World health report also showing the density of health workers (doctors, nurses and midwives) was correlated with the survival probability of infants, children and mothers.31 This may at least partly explain why Philippines National Demographic and Health Survey data between 1998 and 2013 show significant improvements across infant and child mortality rates in the Eastern Visayas and Zamboanga Peninsula regions, served respectively by the SHS-Palo and ADZU-SOM medical schools. This same 15-year period saw neonatal mortality fall in Eastern Visayas and Zamboanga Peninsula by, respectively, 21 and 9 deaths per 1000 births, infant mortality by 52 and 29 deaths per 1000 births, perinatal mortality by 9 and 3 deaths per 1000 births, child mortality by 14 and 24 deaths per 1000 births, and under-5 child mortality by 54 and 40 deaths per 1000 births – far greater reductions than for any other Philippines region except for the autonomous region in Muslim Mindanao (which experienced significant unrest in the early 1990s). Many other regions showed increases in neonatal and perinatal mortality rates during this period.
The international literature shows the health status of rural populations is usually poorer than in metropolitan areas, and is associated with significantly lower life expectancy and higher rates of both mortality and morbidity.32 Two factors found to be associated with increased disease burden in rural areas as compared to urban areas are limited access to appropriate clinical services, and the lack of appropriate public health programs.20,33 Alignment with community health priorities is a critical requirement for SAHPE medical education.
Students from ADZU-SOM and SHS-Palo receive substantial training in both the priority health issues of their respective regions and in conducting priority public health and community development initiatives. Graduates competent in local health priorities and implementing public health initiatives would be best qualified to reduce the disease burdens of rural and/or underserved areas via greater strengthening of their health systems. Thus, not only are SAHPE graduates often choosing to practise in rural and/or poor communities, but they are also well-prepared for such practice, providing further evidence that SAHPE health education is an effective approach for building a fit-for-purpose health workforce across diverse geographical and socioeconomic contexts.
Limitations
The alumni tracking and networking processes of the SHS-Palo and ADZU-SOM allowed a high proportion of graduate locations (94% and 57%, respectively) to be identified for these schools; however, identification of practice locations for graduates of the conventional medical schools was much lower, at 29% and 28%. This poor response rate for conventional medical graduate practice locations thus introduces the potential for respondent bias, which may underrepresent the numbers of conventionally trained medical graduates practising in less accessible, more remote and lower socioeconomic locations. However, in line with statistics showing an average of only 32% of medical graduates choosing to practise in the Philippines,12 it is likely that a significant number of conventionally trained graduates could not be identified because they were practising internationally, rather than being unlocatable due to practising in less accessible areas of the Philippines, or because those graduates had a weaker connection to the named SHS-Palo and ADZU-SOM researchers on the project.
Cities and municipalities were also classified under the Philippines Department of Finance;16 with major regional cities classified as income level 1 (highest socioeconomic level). While major regional cities such as Zamboanga City have communities of very low as well as very high socioeconomic indicators, the practice location of graduates was only at the city/town level; thus, medical graduates of all schools could be practising in lower income classification areas than income level 1, which may bias the findings. However, given the socially accountable mandate of ADZU-SOM and SHS-Palo, it is more likely that graduates from these schools would be more prone to practice in lower income areas of major cities, and thus give an underestimation of the curriculum effects of SAHPE on recruitment to lower socioeconomic areas.
Finally, the rural background of the graduates may also be influencing the study outcomes. There is literature showing graduates who have a rural background are more likely to return to rural areas to practice.22,34-36 While ADZU-SOM practices open admission and selects applicants predominantly from the urbanised Zamboanga City based on self-reported interest in community service and academic ranking, SHS-Palo accepts a high proportion of students from rural areas via its step ladder curriculum involving rural communities personally selecting and supporting applicants, including providing them with an undergraduate scholarship with return-of-service obligation and the guarantee of a rurally based medical position post-graduation. This may at least partly explain the greater proportion of SHS-Palo practising in lower socioeconomic and/or smaller communities across their respective region than graduates from not only conventional medical schools, but also their SAHPE graduate counterparts from ADZU-SOM. However, SHS-Palo medical students who have gone through the step ladder curriculum will also have had many years of rural community immersion, significantly longer even than their counterparts from ADZU-SOM, which may also be influencing the study outcomes in addition to rural background.
Conclusions
The SAHPE training approach has contributed to increased medical coverage across the Mindanao and Visayas regions of the Philippines. It is likely that the extensive community-based student placements associated with SAHPE play a significant role in graduates choosing to practice in rural and economically disadvantaged communities – communities recognised globally as being medically underserved. Governments experiencing similar medical workforce maldistributions as the Philippines should consider SAHPE as a cost-effective strategy in recruiting and retaining health graduates to rural and/or economically disadvantaged areas.
Acknowledgements
The authors would like to acknowledge and thank graduates, colleagues and community members who participated in this study, including a specific thankyou to Helen Gumba, Rolly Borrinaga, Angie Camposano, Evangeline Pasagui, Herman Nicolas, Victor Matthew Sur, Vanessa Bolido, Eduard Remegia, Ellery Apolinario, Wilster Madamba, Jesse Serrano, Ruth Ramirez, Michael Filoteo and Mario Tumacmol. Atlantic Philanthropies have funded THEnet for this study through Resources for Health Equity.





