Introduction
As universities become more dependent on rural GPs for the delivery of significant amounts of their medical student clinical supervision, they must engage these doctors in mutually rewarding, sustainable partnerships. These partnerships need to be based on an explicit understanding of the rural GPs' motivation for precepting and perceptions of rewards, and the impacts that occur as a result of medical student attachments. In Australia there is increasing involvement of rural GPs in teaching and precepting as a result of the government's targeted programs. It is even more important to engage these practitioners in meaningful partnerships as their involvement has evolved more recently than that of their city-based colleagues. For the purposes of this article, a preceptor is defined as a GP responsible for precepting; that is the instruction, mentorship, supervision and assessment of a medical student's clinical performance within the clinical setting.
This study examines the literature of student impacts on GPs through initially summarizing the effects of student teaching on all GPs then, and more specifically, examining the effects of teaching on rural GPs and their practices.
Methods
The Medline, Ovid and ERIC e-databases were searched for original empirical and descriptive articles. Search terms included:
- medical student or undergraduate or graduate entry or medical teaching and
- doctor or practitioner or clinician or physician or preceptor or mentor and
- general practice or family medicine or primary care or ambulatory setting or community setting.
Because the nature of general practice has changed over time, only articles from 1984 to May 2004 were considered. Any articles involving the impact of medical students on doctors, which did not involve supervision in a clinical setting, were excluded. Articles voicing individual opinions of impacts on GPs, even if considered 'expert', were excluded. This resulted in the exclusion of program descriptions where authors' references to impacts on GPs were not clearly based on empirical findings using quantitative or qualitative research methods.
The search was further broadened to include all articles fitting the above criteria found either through related articles in PubMed or in the reference list of the remaining articles or in accessible non-MEDLINE listed Australian rural health publications.
Results
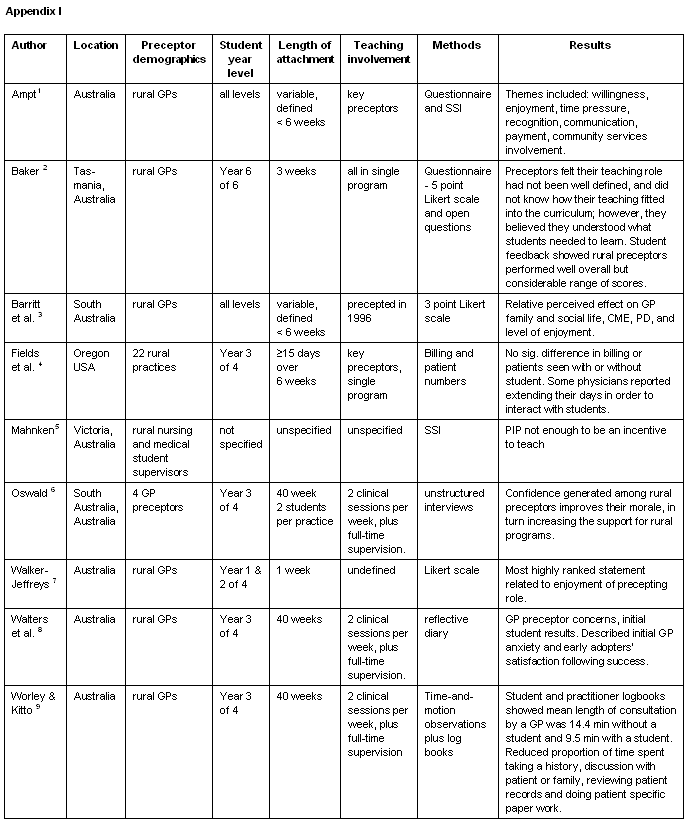
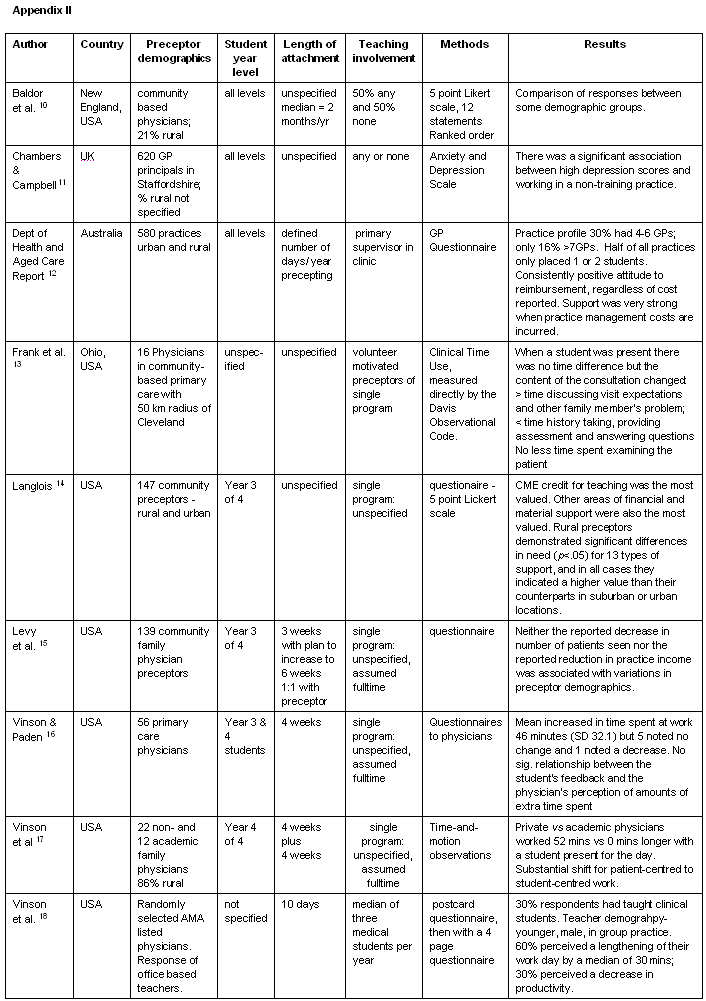
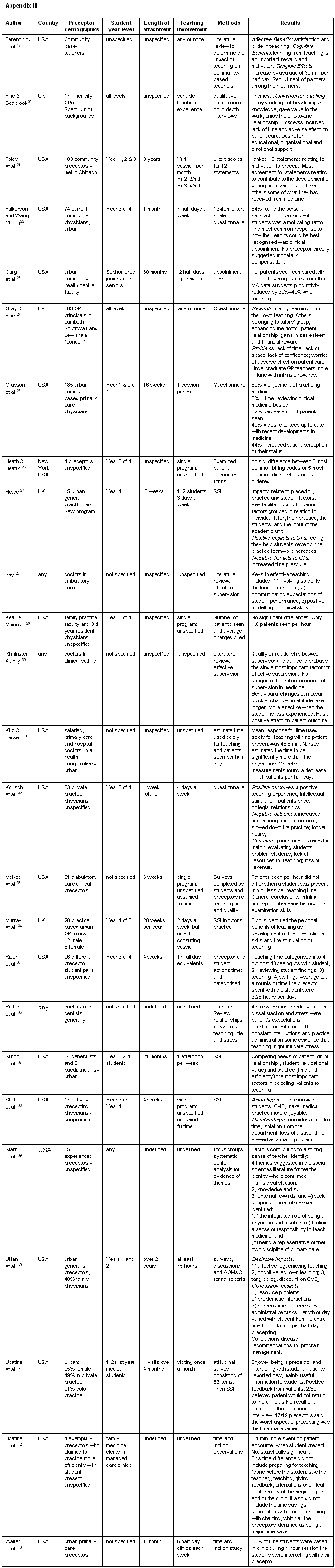
In total 43 articles studying preceptors in Australia, UK and USA were included in the final review, nine of which studied solely rural GPs (Appendix I1-9), nine studied a mix of both urban and rural preceptors (Appendix II10-18), and the remaining 25 were solely urban (Appendix III19-43). Of the articles found, four were literature reviews and 39 were original research articles or reports. Fourteen of these articles related to GP preceptors generally and 29 related to preceptors involved in specified types of student attachments or specific medical school programs. Only 16 articles clearly defined the length and nature of student clinical attachments with which GPs were involved.
Six main categories of impacts on the GPs were defined: personal; time; patient care; professional relationships and professional development; practice business and infrastructure; and recognition and remuneration. Each of these is discussed in the following section of this paper.
Personal
The proportion of doctors who reported increased enjoyment when precepting was always high6,7,44. In studies that asked doctors to think of impacts for themselves there was a reoccurring theme that enjoyment increased while supervising medical students1,6.
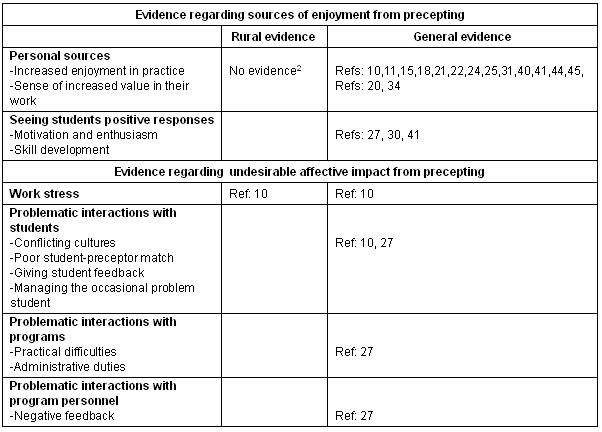
Sources of enjoyment were less explicitly defined in the rural literature2 compared with urban-based studies (Table 1). However, rural GPs were less likely to think that precepting students increased their overall stress level when compared with their urban colleagues10 (Table 1). Some components of teaching may mitigate stress36. Active preceptors saw teaching as aiding in their own learning and development and described staying current with medical literature25.
Table 1: Evidence regarding sources of enjoyment from precepting
Time
Both rural and urban GPs consistently report time pressure when supervising medical students8,38. Despite exceptionally heavy workloads more than 75% of rural GP preceptors reported spending an average of two additional hours at work on each full day of precepting12. This is somewhat greater than was found in the studies which were not specifically rural15,35. Several themes related to work time have been described across all studies. These are set out (Fig 1).

Figure 1: Work time themes defined in general literature.
Some studies have attempted to measure changes in the length of patient consultations rather than estimations of the length of GPs' days. These studies have shown wide variation in results; with a continuum from time saved to time lost17. Time and motion studies measuring changes in consulting activities show that overall the frequency ranking of physician activities did not alter with the presence of a student, however doctors spent less time examining patients13 . Similar findings are described in one Australian rural study9.
Patient care
GPs almost universally stated that patient care remained their primary responsibility, and that this was compatible with precepting students46. Rural and urban studies concluded that a majority of preceptors feel that precepting improved the quality of their clinical practice31. Themes explored in the non-rural literature are summarised (Fig 2). No rural-specific data were found.

Figure 2: Patient care themes defined in not specifically rural literature.
Professional relationships and professional development
Some GPs preceptors have described becoming more aware of the role of others in the practice team27. Key preceptors have described increased interaction with medical schools40 and increased identification with peers who also saw themselves as teachers39. This reduced professional isolation of rural practitioners6 and resulted in professional pride in relation to their role as a preceptor. Some GPs reported an increase in patients' perceptions of their status25. A small group of GPs described increased recognition in the community as an appropriate reward for teaching students27. Many preceptors described wanting to train the next generation and to be seen by the students as role models. They described a desire to pay back the profession21. No data were available regarding rural GPs specifically.
Practice business and infrastructure
Having space to accommodate students was a significant issue for many rural practices8 particularly as many practices are already reported to be overcrowded20. In an Australian study 55% of practices had a room available for students to consult on an ongoing basis and 26% on an intermittent basis12. There was also concern regarding lack of access to study facilities, important reading material, and internet access for student learning32.
Reasons given by rural GPs for teaching included the promotion of rural practice with the aim to recruit future partners to the practice. University involvement in rural practices has improved recruitment outcomes in rural South Australia47. Recruitment assistance has been valued highest after direct financial and material supports14.
The GP teachers' contact with keen students increased not only their morale, but also the morale of the whole practice. This may be due to the increase in teamwork, which is beneficial to the practice27. Most rural primary care physicians report that the presence of a medical student did not result in an increase in staff time16.
Accommodating time needed to teach diminished the number of patients seen per clinic session19. Most rural and urban GPs described a reduction of 6-10 patients per day or 1-2 patients per hour12. Further exploration of productivity is found in mainly urban-based studies (Fig 3).

Figure 3: Productivity themes defined in general literature.
There was a small but significant group of rural preceptors who described no reduction4 or an increased productivity when supervising medical students17.
Recognition and remuneration
Approximately half rural preceptors believed student attachments had a negative effect on their income3, and 40% agreed that precepting students increased practice costs. Physicians in rural private practice found this cost prohibitive and were significantly less likely to agree to precepting a student10 . This was more likely where practices were responsible for student accommodation and learning resource costs.
In an Australian study, the majority of rural GP preceptors agreed that there should be financial remuneration for precepting medical students in their private practices12. Significant numbers of GPs who have been paid have argued that they received inadequate remuneration5,24. In the past, preceptors have stated that lack of funds would not change their commitment to teaching32. However, more recently increasing pressures from clinical responsibilities have began to change this39. Other authors have found that 'dollars alone were not helpful'14and recognition by the University of the work that rural GPs were doing under difficult circumstances was just as important1.
Discussion
Where rural and urban studies focused on impacts affecting GP preceptors generally, few articles clearly defined the length and nature of student clinical attachments. In articles defining impacts to preceptors involved in specified types of student attachment or specific medical school programs there was limited discussion regarding whether findings were generalizable. Many studies have argued that the positive impacts of precepting far outweigh the negative impacts, however the risk of under-reporting of negative impacts has been described previously27.
Only nine empirical studies addressed the impact of medical students on rural GPs specifically. All but one of these studies were Australian, where the majority of studies from the total group of studies were from USA. Personal factors, including satisfaction in teaching, and increased interest in clinical medicine, are the main drivers for the majority of rural preceptors. There is some evidence that enjoyment can be secured with positive feedback from students and increased confidence in teaching and student assessment. Threats to this enjoyment jeopardise retention of rural GP preceptors and considerable program support is needed where negative experiences occur.
Rural GPs consistently report the single most significant pressure when supervising medical students is time management. It is likely that time impacts will differ, depending on how actively the learner participates in patient care, how the appointment system is adapted to manage the presence of students, whether the rotation is block or longitudinal, the point in the student attachment and how time impacts are measured. More research is needed to unravel these variables. Many authors have failed to make explicit the actual involvement of the preceptor in the medical student program, making comparisons among studies difficult.
The length of longitudinal attachment may affect the impacts on rural GPs. This confounding factor has not been evaluated in assessing differences between rural and urban contexts. One hypothetical model suggests that students became less of a time burden to their supervising doctors in prolonged attachments9: however, this model was extrapolated from two data sets only. Further studies of the effect of prolonged student attachments are required.
In considering professional impacts, further research is needed to define the characteristics of the small group of preceptors who express concerns that teaching might have an adverse effect on their patient care, and validate or challenge their concerns. Most supervisory relationships have a defacto power relationship between the supervisor and the trainee. Individual social position, particularly race, gender, social class and sexuality, also confer relative power. The possibility that demographic relationships between rural GPs and students could change the teaching context, and thereby alter the impacts on the supervisor, has not been evaluated.
If universities are expected to compensate for business impacts, including infrastructure requirements and reported decreased productivity through direct financial payments, current and future teaching may prove to be unsustainable. There are a group of rural practices where these business challenges have reportedly been overcome through adopting various consulting and teaching blends; however, it is not known if this has been at the expense of student learning. Further studies are required into different curricular structures which may minimize negative impacts and measure these against student feedback and performance. Recruitment through mentoring, although reported as an important motivator, is a primary motivator for only a minority of GPs, usually practice principals, who perhaps see student supervision from a more strategic perspective.
Conclusions
There is a paucity of literature specific to rural GPs in this field. However, from the wider literature, we have categorized the impact of precepting students into personal, professional, and business domains. Personal factors, including satisfaction in teaching, and increased interest in clinical medicine, are the main drivers for the majority of rural preceptors. Both rural and urban GPs consistently report the single most significant pressure when supervising medical students is time management. There seem to be some differences in time impacts between rural and urban studies. but country of origin of the studies and length of attachment are obvious confounding factors. Most rural GPs feel precepting does not negatively impact on professional factors, including patient care. Further studies need to evaluate the differences between these GPs and the small percentage of GPs who have concerns regarding quality of patient care. Business factors including decrease productivity; and clinic space pressures significantly impact on the capacity of some rural practices to precept students.
As universities become more dependent on GPs to deliver significant amounts of medical student clinical supervision, they must develop an explicit understanding of the impacts on rural GPs. Given the emerging acknowledgement of the differences between rural and urban practice, rural-specific studies are required. Furthermore, these studies should evaluate the relationship between the quality of teaching delivered, with the type and length of student attachments, and the likely impacts on rural GPs. As the trend towards longitudinal attachments continues, the impact of these specifically needs investigation.
References
1. Ampt A, Bloomfield L, Sutherland D. Medical School Rural Education an evaluation and development project. Project of National Significance - Commonwealth Rural Undergraduate Support and Coordination (RUSC) Program. Townsville: James Cook University, 2004.
2. Baker P, Dalton L, Walker J. Rural General Practitioner Preceptors - How can Effective Undergraduate Teaching be Supported or Improved?. Rural and Remote Health 3: 107. (Online) 2003. Available: http://rrh.org.au (Accessed 9 August 2005).
3. Barritt A, Silagy C, Worley P, Watts R, Marley J, Gill D. Attitudes of rural general practitioners towards undergraduate medical student attachments. Australian Family Physician 1997; 26: S87-S90.
4. Fields SA, Toffler Wl, Bledsoe NM. Impact of the presence of a third-year medical student on gross charges and patient volumes in 22 rural community practices. Academic Medicine 1994; 69: S87-89.
5. Mahnken J. Clinical Placements in Victoria: Issues affecting co-ordination in nursing and medical education. Rowville, Victoria: Victorian Universities Rural Health Consortium, 2002.
6. Oswald N. Parallel Rural Community Curriculum (PRCC) Final Evaluation report. Flinders University of South Australia. School of Medicine, South Australia, 2002.
7. Walker-Jeffreys M. Rural Week Preceptor Feedback Report. Whyalla Norrie, SA: Spencer Gulf Rural Health School, 2003.
8. Walters L, Worley P, Mugford B. The parallel rural community curriculum: is it a transferable model? Rural and Remote Health 3: 236. (Online) 2003. Available: http://rrh.org.au (Accessed 9 August 2005).
9. Worley P, Kitto PA. Hypothetical Model of the Financial Impact of Student Attachment on Rural General Practice. Rural and Remote Health 1: 83. (Online) 2001. Available: http://rrh.org.au (Accessed 9 August 2005).
10. Baldor R, Brooks W, Warfield M, O'Shea K. A survey of primary care physicans' perception and needs regarding the precepting of medical students in their offices. Medical Education 2001; 35: 714-715.
11. Chambers R, Campbell I. Anxiety and depression in general practitioners: associations with type of practice, fundholding, gender and other personal characteristics. Family Practice 1996; 13: 170-173.
12. Department Of Health and Aged Care. Establishment of a profile of undergraduate medical student placements and teaching practices. Final Report. Melbourne, VIC: Monash University, KPMG, Flinders University, 1999.
13. Frank S, Stange K, Langa D, Workings M. Direct observation of community-based ambulatory encounters involving medical students. JAMA 1997; 278: 712-721.
14. Langlois J. Support of Community Preceptors: What do they need? Education Research and Methods 1995; 27: 641-645.
15. Levy B, Gjerde C, Albrecht L. The effects of precepting on and the support desired by community-based preceptors in Iowa. Academic Medicine 1997: 75: 382-384.
16. Vinson D, Paden C. The effect of teaching medical students on private practitioners' workloads. Academic Medicine 1994; 69: 237-238.
17. Vinson D, Paden C, Devera-Sales A. Impact of medical student teaching on family physicians' use of time. Journal of Family Practice 1996; 42: 243-249.
18. Vinson D, Paden C, Devera-Sales A, Marshall B, Waters E. Teaching medical students in community-based practices: a national survey of generalist physicians. Journal Family Practice 1997; 45: 482-484.
19. Ferenchick GS, Chamberlain J, Alguire P. Community-based teaching: defining the added value for students and preceptors. The American Journal of Medicine 2002; 112: 512-517.
20. Fine B, Seabrook M. GPs attitudes towards increased medical education in the community. Education for General Practice 1996; 7: 42-47.
21. Foley R, Yonke A, Smith J, Roe B, Vance J. Recruiting and retaining volunteer community preceptors. Academic Medicine 1996; 71: 460-463.
22. Fulkerson P, Wang-Cheng R. Community-based faculty: motivation and rewards. Educational Research and Methods 1997; 29: 105-107.
23. Garg M, Boero J, Christiansen R, Booher C. Primary care teaching physicians' losses of productivity and revenue at three ambulatory-care centres. Academic Medicine 1991; 66: 348-353.
24. Gray J, Fine B. General Practitioner teaching in the community: a study of their teaching experience and interest in undergraduate teaching in the future. British Journal of General Practice 1997; 47: 623-626.
25. Grayson Ms, Klein M, Lugo J, Visintainer P. Benefits and costs to community-based physicians teaching primary care to medical students. Journal of Internal Medicine 1998; 13: 485-488.
26. Heath J, Beatty P. Does teaching medical students in the office affect the way physicians complete patient-encounter forms? Academic Medicine 1998; 73: 439-441.
27. Howe A. Teaching in practice: a qualitative factor analysis of community-based learning. Medical Education 2000; 34: 762-768.
28. Irby DM. Teaching and learning in ambulatory care settings: A thematic review of the literature. Academic Medicine 1995; 70: 898-931.
29. Kearl G, Mainous A. Physicians' productivity and teaching responsibilities. Academic Medicine 1993; 68: 166-167.
30. Kilminster SM, Jolly BC. Effective supervision in clinical practice settings: a literature review. Medical Education 2000; 34: 827-840.
31. Kirz H, Larsen C. Costs and benefits of medical student training to a health maintenance organization. JAMA 1986; 256: 734-739.
32. Kollisch DO, Frasier PY, Slatt L, Storaasli M. Community preceptors' views of a required third-year family medicine clerkship. Archives of Family Medicine 1997; 6: 25-28.
33. McKee MD, Steiner-Grossman P, Burton W, Mulvihill M. Quality of student learning and preceptor productivity in urban community health centres. Family Medicine 1998; 30: 108-112.
34. Murray E, Jolly B, Modell M. Can students learn clinical method in general practice? A randomised crossover trial based on objective structured clinical examinations. BMJ 1997; 315: 920-923.
35. Ricer R, Van Horne A, Filak A. Costs of preceptors' time spent teaching during a third-year family medicine outpatient rotation. Academic Medicine 1997; 72: 547-551.
36. Rutter H, Herzberg J, Paice E. Stress in doctors and dentists who teach. Medical Education 2002; 36: 543-549.
37. Simon SR, Davis D, Peters A, Skeff K, Fletcher R. How do precepting physicians select patients for teaching medical students in the ambulatory care setting? Journal of Internal Medicine 2003; 18: 730-735.
38. Slatt L, Egelhoff C, Sloane P. Why do preceptors teach? Family Medicine 1984; 16: 189-190.
39. Starr S, Ferguson W, Haley H, Quirk M. Community preceptors' views of their identities as teachers. Academic Medicine 2003; 78: 820-825.
40. Ullian J, Shore W, First L. What did we learn about the impact on community-based faculty? Recommendations for recruitment, retention and rewards. Academic Medicine 2001; 76: 78-85.
41. Usatine R, Hodgson C, Marshall E, Whitman D, Slavin S, Wilkes M. Reactions of family medicine community preceptors to teaching medical students. Family Medicine 1995; 27: 566-570.
42. Usatine R, Nguyen K, Randall J, Irby DM. Four exemplary preceptors' strategies for efficient teaching in managed care settings. Academic Medicine 1997; 72: 766-769.
43. Walter L, Zweig S, Hosokawa M. A process evaluation of a required primary care clerkship. Family Medicine 1991; 23: 547-548.
44. Shorey J, Epstein A, Moore G. The clinical-teacher in managed care settings. Managed Care 1997; 12: S98-S103.
45. Wang-Cheng R, Fulkerson P, Barnas G, Lawrence S. Effect of student and preceptor gender on clinical grades in an ambulatory care clerkship. Academic Medicine 1995; 70: 324-326.
46. Mann K, Holmes D, Hayes V, Burge F, Viscount P. Community family medicine teachers' perceptions of their teaching role. Medical Education 2001; 35: 278-285.
47. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37: 809-814.